Cause Signs And Symptoms Treatment And Management Age Of Onset Of Parkinsons And Huntingtons Disease:
Cause:
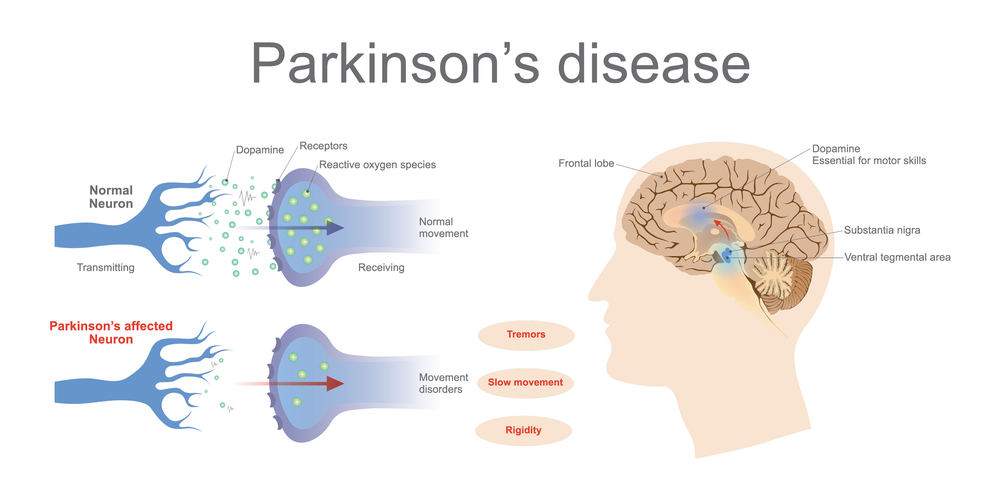
Parkinson’s Disease: PD is caused by the degeneration of the neurons in Substantia nigra of the midbrain.
Huntington’s Disease: HD is caused by the mutations in the HTT gene.
Age of Onset:
Parkinson’s Disease: PD usually occurs after the age of 50.
Huntington’s Disease: HD usually occurs in the thirties or forties.
Symptoms:
Parkinson’s Disease: PD causes tremors, rigidity, slowing of movements and gait disturbances.
Huntington’s Disease: HD causes higher function abnormalities such as problems in thinking and reasoning together with characteristic chorea.
Treatment:
Parkinson’s Disease: PD is treated with dopamine-enhancing drugs such as levodopa, dopamine agonists, etc.
Huntington’s Disease: HD has no curative treatment and main the treatment is supportive.
Life expediency:
Parkinson’s Disease: PD doesn’t have an effect on life expectancy. However, it reduces the quality of life.
Huntington’s Disease: HD patients live 15-20 years after the appearance of the first symptom.
Multiple Sclerosis Vs Parkinsons Disease Differences In Symptoms Causes And Treatment
Multiple sclerosis is an autoimmune condition that affects the nervous system, while Parkinson’s disease is a progressive neurological disorder affecting movement. Symptoms of multiple sclerosis and Parkinson’s disease are quite similar at times, but there are distinct differences setting the two conditions apart.
Causes of multiple sclerosis and Parkinson’s disease are not well known, although there is some speculation to their roots. We will outline those speculated causes and highlight the symptoms, risk factors, complications, treatment, and therapies for both multiple sclerosis and Parkinson’s disease to raise your awareness on each disorder.
Benefits Of Aquatic Therapy For Alzheimers Patients In Senior Living Facilities
Stay active
Many physicians believe that the key to longevity with Alzheimer’s is activity. Thus, if a patient with Alzheimer’s can enjoy working out in a therapy pool, whether with a clinician or as part of a larger class, that patient has a better chance of remaining in good health for as long as possible. Even if he or she fears falling when walking on land , that fear is highly negated by the natural buoyancy of the water.
Become accustomed to a routine
Alzheimer’s patients who have a scheduled plan for pool therapy and/or exercise may become accustomed to the routine. This, in turn, can be a boost to their mental abilities. Routine for Alzheimer’s patients may even promote slower memory loss, although this is debatable. If nothing else, it provides them with a very positive outlet.
Psychological Effect
The therapy pool has a psychological effect on those with Alzheimer’s by the warmth of the water. Not only is it soothing to the body, but it can be soothing to the mind. Many Alzheimer’s patients live with a high degree of uncertainty and stress because they know something is wrong, but aren’t sure what that is. If pool therapy can alleviate those tensions, the patients will be under far less emotional turmoil throughout the day.
Request a Free Info Kit View Our Products Find a Pool Near You
Sidebar: Morris K Udall Centers Of Excellence For Parkinson’s Disease Research
The Morris K. Udall Parkinson’s Disease Research Act of 1997 authorized the NIH to greatly accelerate and expand PD research efforts by launching the NINDS Udall Centers of Excellence, a network of research centers that provide a collaborative, interdisciplinary framework for PD research. Udall Center investigators, along with many other researchers funded by the NIH, have made substantial progress in understanding PD, including identifying disease-associated genes; investigating the neurobiological mechanisms that contribute to PD, developing and improving PD research models, and discovering and testing potential therapeutic targets for developing novel treatment strategies.
The Udall Centers continue to conduct critical basic, translational, and clinical research on PD including: 1) identifying and characterizing candidate and disease-associated genes, 2) examining neurobiological mechanisms underlying the disease, and 3) developing and testing potential therapies. As part of the program, Udall Center investigators work with local communities of patients and caregivers to identify the challenges of living with PD and to translate scientific discoveries into patient care. The Centers also train the next generation of physicians and scientists who will advance our knowledge of and treatments for PD. See the full list of Udall Centers.
Multiple Sclerosis Vs Parkinsons Disease: Us Prevalence And Economic Impact
Anyone can develop multiple sclerosis, but it mostly affects 20- to 40-year-olds. Prevalence of multiple sclerosis in the U.S. is estimated at over 400,000 cases, and nearly 200 new cases are diagnosed each week. Rates of multiple sclerosis are highest in areas furthest away from the equator, so the rates are higher in the Northern U.S.
Direct and indirect costs resulting from multiple sclerosis can range from $8,528 to $54,244.
One million Americans live with Parkinson’s disease. The average cost of Parkinson’s disease including treatment, lost work wages, and social security payments is $25 billion annually in the U.S.
Multiple Sclerosis Vs Parkinsons Disease: Risk Factors And Complications
Risk factors for multiple sclerosis include being female, having a family history of multiple sclerosis, having certain infections, being white of European descent, living furthest from the equator, living in temperate climate regions, already having an autoimmune disease, and smoking.
Complications resulting from multiple sclerosis include muscle stiffness and spasms, paralysis, problems with bladder, bowel, and sexual function, as well as forgetfulness, mood changes, depression, and epilepsy.
Risk factors for Parkinson’s disease include being over the age of 50, being male, having a family history of Parkinson’s disease, carrying gene variations, experiencing a head injury, being exposed to environmental toxins, and taking certain medications such as anti-anxiety medications or sleeping pills.
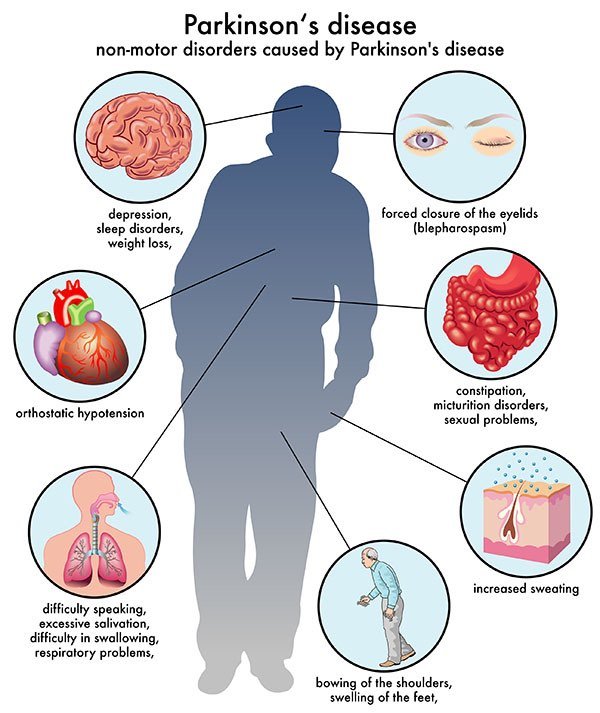
Complications associated with Parkinson’s disease include difficulty thinking, depression, emotional changes, swallowing problems, sleep problems and disorders, bladder issues, constipation, changes in blood pressure, smell dysfunction, fatigue, pain, and sexual dysfunction.
What Natural Interventions May Be Beneficial For Restless Leg Syndrome
- Iron. Iron deficiency or altered brain iron metabolism have been linked to RLS; supplementation is often recommended for RLS patients who have been tested and shown to be deficient. Iron supplementation has been shown to significantly improve symptoms in iron-deficient RLS patients.
- Folate. Low levels of folate may play a role in RLS, especially in pregnant women. Pregnant women with lower folate levels were more likely to develop RLS than women who took vitamins during pregnancy.
- Magnesium. Low magnesium levels can cause excitability of neurons; magnesium supplements are often used to prevent abnormal activity in the nervous system. A case study indicated magnesium may improve symptoms and sleep problems associated with RLS.
- Diosmin. Diosmin is a natural flavone derivative often used for supporting venous function. Since venous disorders have been linked with RLS, diosmin is a promising possible treatment.
- Green coffee extract. Diabetes and pre-diabetes are known risk factors for RLS. Green coffee extract may help maintain healthy glucose levels.
- Valerian root. Valerian, an herbal sedative, is often used as a sleep aid. In a clinical trial, supplementation with valerian resulted in improvements in RLS symptoms and less daytime sleepiness.
- Other natural interventions that may help relieve RLS symptoms include D-ribose and vitaminsC and E.
Is There A Link Between Restless Leg Syndrome And Parkinson’s Disease
Parkinsons & Restless Leg Syndrome: Using Dopaminergic Medication
Myasthenia Gravis And Multiple Sclerosis: Differences And Similarities
Nervous System Disorders and Diseases
Multiple sclerosis presents patients with a number of symptoms that can disrupt everyday life. During an episode for those with relapsing-remitting MS, or those with one of the progressive MS forms with constant symptoms, obtaining a diagnosis that allows the patient to work with doctors and therapists to create a treatment and management regimen is crucial to living a full and healthy life.
Of course, MS is not the only chronic disease that causes such issues or requires direct attention. Another condition, called Myasthenia gravis, can also cause significant impairment when trying to complete daily activities. In fact, Myasthenia gravis actually seems quite similar to some aspects of multiple sclerosis and distinguishing one from the other is essential to prescribing the right treatment plan.
Parkinsons Disease And Multiple Sclerosis: Conditions And Differences
It’s important to note that, while both Parkinson’s and multiple sclerosis are diseases of the CNS, they don’t originate in the same way. MS is an autoimmune disease, brought on by the immune system attacking myelin, the protective coating over the nerves in the CNS that also speeds up signals. This affects mainly the brain and spinal cord, though it can also affect the optic nerve as well. In Parkinson’s disease, the neurons in the brain die off without any known attack, with the lack of dopamine they produce leading to the onset of the disease. This doesn’t affect nerves in the spinal cord.
Other notable differences include:
Know The Difference Between Parkinsons Disease And Multiple Sclerosis
Multiple Sclerosis and Parkinson’s Disease are two medical conditions, which are often mistaken for each other, as both are progressive and have similar symptoms. And although patients can have both conditions simultaneously, there are a few striking differences between the two.
Check out this quick guide about the similarities and differences between the two conditions to help patients avail the best Parkinson’s Disease and Multiple Sclerosis treatment on time.
Understanding Parkinson’s Disease and Multiple Sclerosis
Parkinson’s Disease is one of the most common neurodegenerative conditions in the world. It primarily damages the dopamine-producing neurons in a specific area of the brain called substantia nigra.
Multiple Sclerosis is a chronic inflammatory condition of the central nervous system. It is an autoimmune demyelinating disease, which means the immune system mistakenly attacks normal tissues — in this case, the myelin or protective covering around nerve fibers. This leaves scarred tissues or lesions in multiple areas, disrupting electrical impulses throughout the body. When the myelin sheath is damaged, nerve impulses slow or even stop, causing neurological problems.
Similarities between the two conditions
Both Multiple Sclerosis and Parkinson’s Disease affect the brain and the central nervous system, which leads to changes in the way you move, talk, and interact with the world. The two conditions have several common symptoms, including
Myasthenia Gravis And Multiple Sclerosis: Conditions And Differences
One of the biggest differences between multiple sclerosis and Myasthenia gravis is that the latter is far less common than MS. While multiple sclerosis is believed to affect about one in four hundred people, Myasthenia gravis is estimated to develop in only about one in five thousand. Other differences include:
In addition, while both diseases involve weakness in the limbs, this is typically one of the first signs of multiple sclerosis. In Myasthenia gravis, it usually only follows weakness in the neck, facial muscles, and eyes.
Are There Differences In Parkinsons Treatment Between Men And Women
All current treatment options address PD symptoms, but they do not slow down or stop the progression of PD. Levodopa, often prescribed as Sinemet, is considered the gold standard therapy for Parkinson’s movement symptoms. However, many people with PD experience changes in the effectiveness of the drug as the disease progresses. And some studies suggest that women are more likely than men to report these fluctuations earlier in the disease course and more frequently overall.
In particular, it seems that women are more likely to have involuntary movements called dyskinesias that occur when levodopa levels are highest in the blood. There are several factors that could be contributing to dyskinesia, including dosage, body weight and age of onset. Lower body weight can affect how medications build up in someone’s system. Lighter people sometimes need a smaller dose of medication to feel its effect. On average, women weigh less than men. If women and men are receiving similar doses, this may explain how levodopa levels are causing dyskinesias.
Physicians have also suggested that they find it harder to fine-tune Parkinson’s medications for women than for men. Women more often experience large swings in symptoms from even small changes in medications or schedules.
Differentiating Multiple Sclerosis Symptoms With Parkinsons Disease
Signs and symptoms of multiple sclerosis include numbness or weakness in one or more limbs, partial or complete vision loss, prolonged double vision, tingling or pain, electric-shock sensations, tremors and lack of coordination, fatigue, dizziness, slurred speech, and problems with bowel and bladder function.
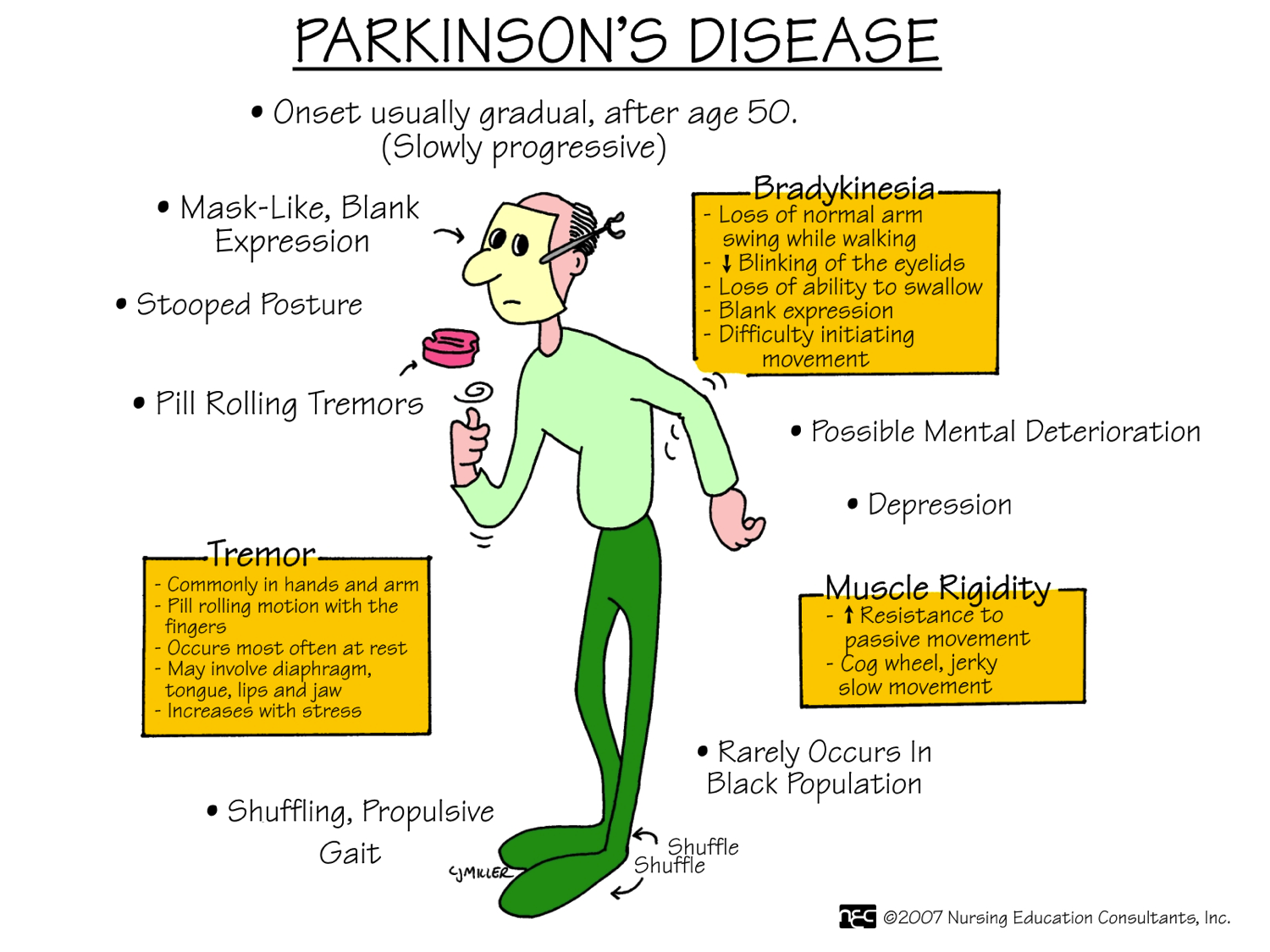
Parkinson’s disease symptoms typically begin with tremors followed by muscle stiffness, difficulty standing or walking, changes in speech, slow movements, impaired posture and balance, loss of automatic movements, and writing changes.
As you can see, Parkinson’s disease and multiple sclerosis do have some symptoms in common, which can make early diagnosis difficult.
Myasthenia Gravis And Multiple Sclerosis: Symptoms And Similarities
As a condition of the nervous system, there are obviously going to be similarities in the presentation of Myasthenia gravis and multiple sclerosis. Some of these include:
- Both diseases are chronicautoimmune diseases that lead to improper or lack of communication between the brain and muscles, which makes mobility more difficult.
- Both conditions cause weakness in the limbs, as well as potential issues with vision .
- Though the reason behind the deficiency is different, either disease can lead to problems speaking, chewing, and swallowing .
- Both diseases are most common in adult women under the age of forty.
- Having another autoimmune disease, such as rheumatoid arthritis or type 1 diabetes, puts a person at greater risk for developing either disease.
- Both diseases may “come and go”, with relief from symptoms over a period of time before they return.
- A relapse or episode in either disease can be triggered by factors such as stress, fatigue, illness or injury, and certain medications .
- Neither disease has a cure, but both can be treated to reduce relapses and symptoms. Some common treatments for both include immunosuppressants, corticosteroids, and DMTs like treatment with monoclonal antibodies.
The First Sign Of Parkinsons And Multiple Sclerosis: A Dodgy Tummy
- Study suggests that brain disease can be caused by an unhealthy gut
- ‘Butterflies in the stomach’ could be linked to Parkinson’s and MS
17:07 EDT, 21 June 2014 | Updated:
Gut feeling: Brain disease can be caused by an unhealthy stomach
Anxiety or anticipation can often lead to a feeling of ‘butterflies in the stomach’ – which usually dissipates along with the source of the consternation.
But scientists have discovered that the nerve pathways between the gut and the brain that cause this phenomenon may also be linked to degenerative illnesses such as Parkinson’s disease and multiple sclerosis , as well as some mental health problems.
Dr Anton Emmanuel, consultant neuro-gastroenterologist at University College London and the National Hospital for Neurology, explained: ‘The gut and brain share the same nerve chemistry and have a dialogue.
‘That’s why when you feel stress and other strong emotions, such as fear, it leads to gastrointestinal symptoms, like rushing to the loo.’
A new study suggests that brain disease can be caused by an unhealthy gut because these signals also travel in the opposite direction.
The study, which was published in the journal Movement Disorders, found that sufferers of Parkinson’s disease had a higher prevalence of a condition called small intestinal bacterial overgrowth, or SIBO.
In SIBO, normally harmless bacteria proliferate in large numbers in the small intestine.
Multiple Sclerosis Vs Parkinsons Disease: Treatment And Therapies
Treatment for multiple sclerosis is lifelong, and although it cannot cure the condition, it aims to minimize symptoms and allow the patients to live as normal of a life as possible. Some treatment methods include corticosteroids and plasma exchange, beta interferons, Glatiramer acetate, Dimethyl fumarate, Fingolimod, Teriflunomide, Natalizumab, Alemtuzumab, and Mitoxantrone, which all help to reduce the likelihood of relapses.
Other treatment methods include physical therapy to improve mobility, muscle relaxants, medications to reduce fatigue, and other medications like antidepressants, medications to control the bowels and bladder, and medications to improve sexual function.
Exercise, meditation, yoga, and acupuncture are also recommended as a means to reduce stress and improve overall mental and physical well-being.
There is no cure for Parkinson’s disease as well, but treatments are available to manage the symptoms and slow down the disease progression as much as possible. Alongside traditional treatments, supportive therapies are also used to improve different aspects of a person’s health.
Common medications prescribed in Parkinson’s disease include dopamine replacement therapy, dopamine agonists, anticholinergics, amantadine, monomine oxidase type B inhibitors, and catechol-o-methyl transferase inhibitors.
You can work closely with your doctor to create a specific treatment plan for you.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Restless Legs Syndrome: Detection And Management In Primary Care
NATIONAL HEART, LUNG, AND BLOOD INSTITUTE WORKING GROUP ON RESTLESS LEGS SYNDROME, National Institutes of Health, Bethesda, Maryland
Am Fam Physician. 2000 Jul 1;62:108-114.
Restless legs syndrome is a neurologic movement disorder that is often associated with a sleep complaint. Patients with RLS have an irresistible urge to move their legs, which is usually due to disagreeable sensations that are worse during periods of inactivity and often interfere with sleep. It is estimated that between 2 and 15 percent of the population may experience symptoms of RLS. Primary RLS likely has a genetic origin. Secondary causes of RLS include iron deficiency, neurologic lesions, pregnancy and uremia. RLS also may occur secondarily to the use of certain medications. The diagnosis of RLS is based primarily on the patient’s history. A list of questions that may be used as a basis to assess the likelihood of RLS is included in this article. Pharmacologic treatment of RLS includes dopaminergic agents, opioids, benzodiazepines and anticonvulsants. The primary care physician plays a central role in the diagnosis and management of RLS.
Chronic Dopaminergic Therapy Can Cause Augmentation Of Symptoms
Refer patients experiencing augmentation to a specialist. Most cases can be reversed with a change in dosing frequency, by lowering the dose, by switching drugs or by stopping dopaminergic therapy.3
Can Restless Legs Syndrome Develop Into Something More Serious
Projected Estimates Of Parkinsons Disease With Aging Population
As the life expectancy has increased worldwide, it is expected that the burden of chronic diseases, like PD, will continue to grow. It is estimated that the number of people with PD in 2005 totaled between 4.1 million and 4.6 million and that number will more than double by 2030 to between 8.7 million and 9.3 million.7
Are There Differences In Parkinsons Care Between Men And Women
Women with PD may face more barriers to quality healthcare and social support than men. Women are less likely than men to be cared for by a Parkinson’s specialist, such as a neurologist or movement disorder specialist, and are also less likely to have a care partner. On the other hand, women with Parkinson’s are more likely to do the following:
- Go to doctor’s appointments alone
- Use home healthcare
- Live in a skilled nursing facility
All these factors mean that women may not have access to adequate Parkinson’s care.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
What Is The Pooled Prevalence Of Rls/wed And Its Mimics In Pd
In view of these contrasting results, what is the overall prevalence of the sum of true, secondary and mimics of RLS/WED in PD? A recently-published meta-analysis4343. Yang X, Liu B, Shen H, Li S, Zhao Q, An R et al. Prevalence of restless legs syndrome in Parkinson’s disease: a systematic review and metaanalysis of observational studies. Sleep Med. 2018 Mar;43:40-6. https://doi.org/10.1016/j.sleep.2017.11.1146https://doi.org/10.1016/j.sleep.2017.11…. tried to answer this question comparing 28 clinical studies. The pooled prevalence among diverse populations was 14%, being higher among those who had previously received dopaminergic treatment than among drug-naïve patients . Differences were also marginal for gender prevalence, favoring women . In their discussion, the authors were careful enough to acknowledge the intrinsic limitations of these studies, including a variety of biases.
Pramipexole Is Not Recommended In Pregnancy Or Breastfeeding
There is a lack of clinical data in pregnancy, along with evidence that pramipexole impairs implantation and disrupts early pregnancy in rats .6 Pramipexole is expected to inhibit lactation because of its effects on prolactin. It may be excreted into breast milk and should not be used during breastfeeding.6
Pathological Evidence Of Dopamine Dysfunction In Pd And Rls
Pramipexole May Be Useful For Severe Restless Legs Syndrome
The Importance Of Establishing Parkinsons Prevalence Numbers
Parkinson’s Prevalence estimates will help the Parkinson’s Foundation attract the attention of federal and state government as well as the pharmaceutical industry to the growing need and urgency in addressing PD. This is an important first step to better understanding who develops PD and why.
The next phase of this study will be to determine the rate of PD diagnosis or incidence, how that has changed over time and what is the rate of mortality among those affected by PD. Determining the prevalence and incidence will allow the PD community to effectively advocate for additional money and resources necessary to support Parkinson’s research.
Parkinson’s Foundation Prevalence Project numbers highlight the growing importance of optimizing expert Parkinson’s care and treatment for people with Parkinson’s, which would help future caregivers and ease the strain on health and elder care systems.
Loading…
Treatment Of Depression In The Setting Of Parkinsons Disease
The evidence base for the treatment of depression in PD is extremely slim. A recent Cochrane library review of treatments for depression in PD reported three randomised controlled trials fulfilling the criteria for inclusion.1 These trials included a total of 106 patients and indicated that nortryptilline was superior to placebo but that citalopram was not. The review concluded that there were “insufficient data on the effectiveness and safety of any antidepressant therapy in Parkinson’s disease”. There is an urgent need for larger scale clinical trials in this area.
Nevertheless, depression is common in PD and decisions have to be made about treatment. The last 10 years have seen a shift in prescribing practice away from tricyclic antidepressants and towards selective serotonin reuptake inhibitors as a first line treatment of depression in PD. The main reason for this is the more favourable side effect profile of SSRIs.
Tricyclic antidepressants
Selective serotonin reuptake inhibitors
Withdrawal syndromes can occur in people who stop SSRIs suddenly and can include flu-like symptoms, insomnia, nausea, imbalance, sensory disturbance, and hyperarousal . Therefore SSRIs should be reduced slowly.
?SSRI withdrawal symptoms
Other treatments for depression
Two Areas In Which Parkinsons Disease May Bring About Death
I. Falls
PD patients are at an increased risk of falling and bad falls can lead to death. This usually occurs as a complication of a fall that requires hospitalization, particularly if it involves surgery. While most people do not fracture their hips when they fall, some do, and hip surgery, while routine, is still major surgery. It carries the risk of infection, delirium related to pain medications and anesthesia, heart failure, pneumonia, blood clots in the legs that then go to the lungs, and general weakness from immobility. Hip fractures are probably the main cause for death for those who fall, but people can fracture other bones and require surgery. They may fracture their ribs, which leads to reduced coughing, because of the pain, and an increased risk of lung infections . It is surprisingly uncommon for Parkinson’s Disease patients to die from brain injuries related to falls, but it still may occur.
II. Pneumonia
PD patients also may develop pneumonias completely unrelated to difficulties with swallowing, just like their non-PD friends and relatives.
Misperception #3: The Tremor Of Et Is Bilateral & Symmetric
Action tremor in patients with ET is usually, though not always, bilateral, and it is typically asymmetric . In a community-based study of 54 patients with ET, the use of clinical rating scales revealed on average a 1.32-fold side–side difference, and quantitative computerized tremor analysis revealed on average a 1.71-fold side–side difference in arm tremor severity . Unilateral arm tremor is less common, reportedly occurring in 2, 4.4 and 10% of ET cases, with values varying depending on the criteria used . One study evaluated unilateral arm tremor in 412 ET cases from 133 kindreds with presumed autosomal dominant ET . Inclusion criteria required unilateral kinetic or postural tremor for at least 5 years, without dystonic posturing or bradykinesia/rigidity . Only subjects with a first-degree relative with definite ET were included . Eighteen patients were identified as having isolated unilateral arm tremor without tremor affecting other body segments . Out of the 18 patients, 13 had a combination of postural and kinetic tremor and 5/18 had only unilateral postural tremor . Isolated unilateral postural tremor should raise the suspicion of PD, and the patient should be followed closely for the development of additional signs suggestive of PD.
Clinical pearl #3: Action tremor in ET is often but not necessarily bilateral. Small to moderate side–side differences are the rule rather than the exception.
Differences Between Essential Tremor And Parkinsons Disease
- 559-770-2002
Comparing Multiple Sclerosis And Parkinsons Disease Causes
Multiple sclerosis is an autoimmune disease in which the immune system attacks the myelin, causing damage and thus exposing nerve fibers. Like many autoimmune diseases, the exact cause is unknown, but environmental, immunologic, infectious, and genetic factors have all been found to play a role in the onset of multiple sclerosis.
When certain nerve cells in the brain begin to die or break down that is what causes Parkinson’s disease, but why this occurs is unclear. Some factors that contribute to nerve cell death include genetics as specific gene mutations have been identified to contribute to Parkinson’s disease, environmental factors such as exposure to certain toxins, the presence of Lewy bodies in the brain as well as alpha-synuclein found in Lewy bodies.
Restless Legs Syndrome And Periodic Limb Movement Disorder
Most people who have RLS also have a condition called periodic limb movement disorder . PLMD involves repetitive flexing or twitching of the limbs while asleep at night. It is different from RLS in that these movements are not accompanied by uncomfortable sensations and because they occur during sleep, patients are often not aware of them. However, PLMD-associated movements can cause a person to wake up and therefore can compound sleep issues in patients who also have RLS.
Although most people with RLS have PLMD, many with PLMD do not have RLS.
Your Dreams Could Be An Early Clue To Parkinson’s Disease
Breaking down Parkinson’s disease05:25
Actor Alan Alda revealed that he has Parkinson’s disease — and in an interview Tuesday on “CBS This Morning,” the award-winning actor said an unusual dream helped lead to his diagnosis.
Alda, best known for his portrayal of Army Capt. “Hawkeye” Pierce in the TV series “M*A*S*H, was diagnosed three and a half years ago after experiencing a lesser-known early sign of Parkinson’s. He said he asked his doctor to test him for the disease after reading an article about how physically acting out your dreams can be one of the earliest precursors of the neurological disorder.
“By acting out your dreams, I mean I was having a dream where someone was attacking me and I threw a sack of potatoes at them, and what I was really doing was throwing a pillow at my wife,” Alda explained.
Restless Legs Syndrome: A Common Underdiagnosed Disorder
US Pharm.
What Are The Primary Motor Symptoms Of Parkinsons Disease
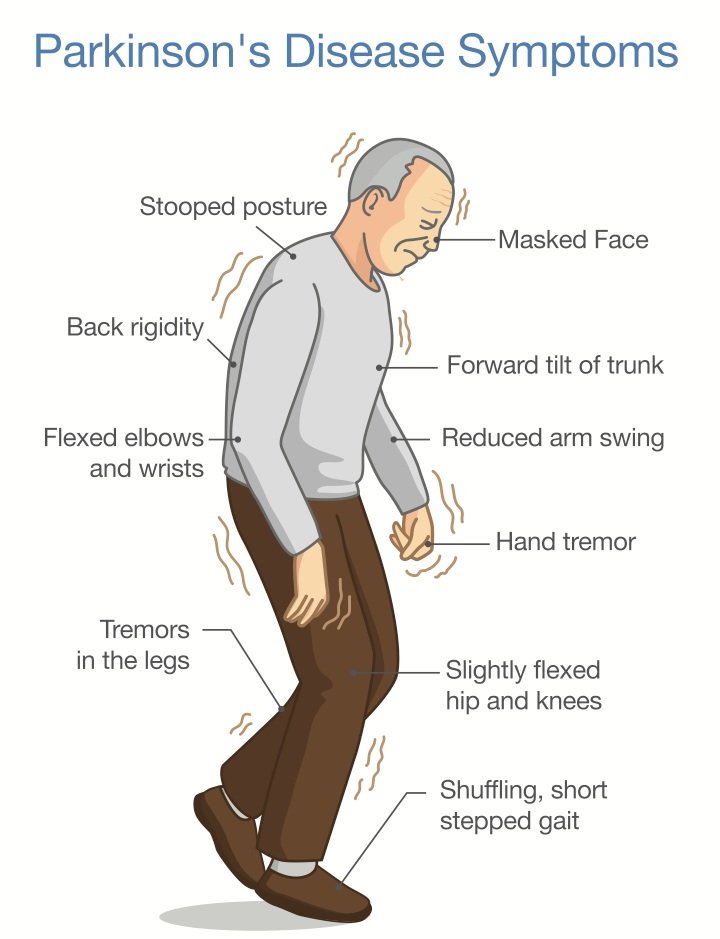
There are four primary motor symptoms of Parkinson’s disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinson’s.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinson’s disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinson’s disease has a tremor, nor is a tremor proof of Parkinson’s. If you suspect Parkinson’s, see a neurologist or movement disorders specialist.
Tremors
Read more about Parkinson’s tremors
Rigidity
Bradykinesia
mask-like expression of the face
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
Clinical Impression 1: Proximal Vs Distal Postural Tremor
On arm extension, a higher proportion of ET than PD patients had isolated proximal tremor whereas a higher proportion of PD than ET patients had isolated distal tremor . There were similar differences when isolated proximal and distal tremors were defined liberally . Even when tremor was present in multiple joints, it was more prominent in the proximal joints in ET patients compared to PD patients . Furthermore, relative to PD, tremor in ET involved the wrist more than distal hand joints . When we excluded 28 PD patients who had taken carbidopa/levodopa within 4 h of the clinical examination, the results were similar. Even when we excluded 39 PD patients who had taken carbidopa/levodopa within 12 h of the examination, the results were similar . We did not perform similar analyses that excluded ET patients who had taken their medications on the day of testing, as there is less of a clear acute timed effect of these medications on motor state.
Table 3. ET vs. PD – Main measures with patients removed who took carbidopa/levodopa within 12 h of exam.
Misperception #4: Head Tremor Occurs In Et But Not In Pd
Clinical pearl #4: Head tremor often occurs in patients with ET but can on occasion also be seen in patients with PD. The head tremor of ET is typically one that resolves at rest , in contrast to what has been reported in PD.
What Are The Different Categories Or Types Of Tremor
Essential tremor
Dystonic tremor
Cerebellar tremor
Ancillary Tests For Tremor Differential Diagnoses
