How Is Constipation An Early Warning Sign Of Parkinson’s It’s Such A Common Problem
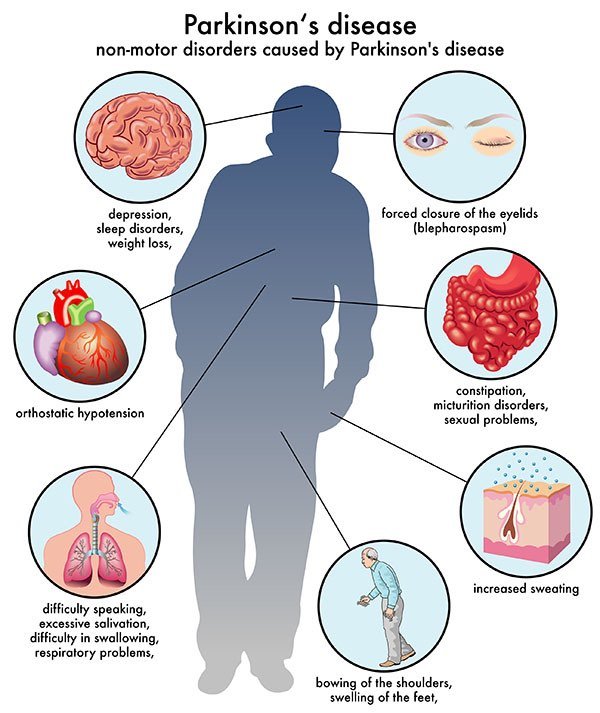
A: It’s not as specific as other prodromal symptoms, like anosmia. The rate at which people with chronic and unexplained problems with constipation develop Parkinson’s disease is not as easy to pin down. But if someone has unexplained, persistent constipation, it should at least be noted, as it could be considered prodromal.
Australian Researchers Hope Brain Gel Can Reverse Parkinsons Disease Symptoms
SYDNEY – Australian researchers say they have developed a new type of gel that could radically transform the treatment of Parkinson’s disease and could also help stroke patients.
The hydrogel is made from natural amino acids, the building blocks of proteins, and has been shown to safely deliver replacement cells into damaged parts of the brain.
The gel acts as a vehicle to safely transfer stem cells into the brain. Scientists believe the process can restore damaged tissue and replace lost neurons, which affect patients with Parkinson’s disease, a nervous system disorder. About 100,000 Australians are estimated to suffer from the disease, which currently has no cure.
“If you imagine a stroke, you have a whole bunch of dead cells where you are no longer getting blood flow, said professor David Nisbet, one of the lead researchers from the Australian National University’s College of Health and Medicine. “In terms of Parkinson’s disease, you lost population of neurons, that’s what results in the symptoms we are familiar with seeing. Basically, what we are doing we are introducing replacement cells into the brain to replace those ones that we can see some repair and regeneration. But they also have the added advantage that we have also shown they can actually protect some of the existing cells in the surrounding tissue once they are implanted.”
Nisbet said the early results are encouraging.
It has been published in the journal Advanced Functional Materials.
Study Says Dancing Helps Slow Progression Of Symptoms Of Parkinsons Disease Christine Sismondotimer
Over the past decade or so, it’s become increasingly clear that brain health and physical health go hand in hand.
As such, on the advice of neuroscientists, people who weren’t necessarily that keen on athleticism have redoubled their efforts. Almost anything that’s good for your heart and circulation system, it seems, is also good for your brain.
Some experts, however, have stressed that certain activities are more promising when it comes to brain health than others. Like walking, which has been referred to as a human superpower, since our brains are always mapping out routes and distances as we make our way through the city. Other forms of exercise, such as swimming and cycling, are said to help us develop the protein needed to repair and create new brain cells.
As exciting as all these discoveries are, it’s beginning to look as if learning to dance might be the greatest superpower of all. And the reason for this might be that it’s an activity that forces us to do several different things at once.
“Walking is very good for you compared to, say, sitting,” says Joseph DeSouza, a professor in York University’s department of psychology. “But imagine walking a little faster and then start counting backwards from a hundred. That’s pushing your brain more. Then imagine you’re doing choreographed steps. And then imagine you have to step in time with someone else, all the while listening to music and, now, an instructor telling you which way to move.”
Depression And Anxiety Are Also Early Warning Signs Of Parkinson’s How So
A: Like the other symptoms discussed here, late-onset depression and anxiety are nonmotor prodromal manifestations of the condition. It’s not that everyone who is depressed will get Parkinson’s, and the numbers are lower than they are for symptoms like anosmia and REM behavior disorder. But the link is important to explore, and we are doing more research on it all the time.
What Is Rem Behavior Disorder And How Is It Connected To Parkinson’s
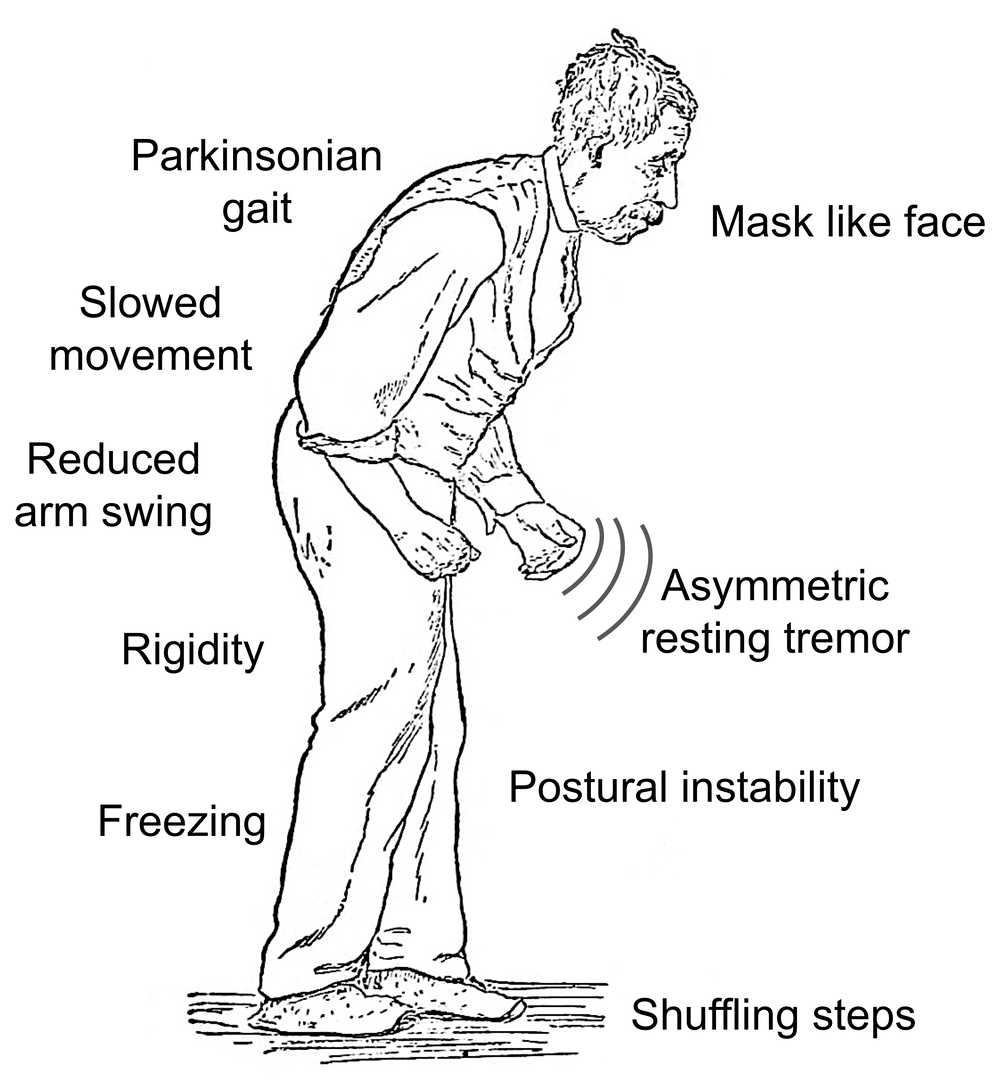
A: REM behavior disorder is different than other sleep problems, like insomnia. People who have it may jerk or kick — it’s as though they are acting out their dreams. In a similar pattern to anosmia, people with idiopathic REM sleep behavior disorder have at least a 50 percent chance of eventually developing Parkinson’s disease.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Parkinsons Disease 101: Signs Symptoms And Options For Treatment Jennifer Palisoc
Parkinson’s disease can affect individuals in different ways. With the early signs of the disease, some individuals may find they’re moving more slowly and experience stiffness, have trouble with their balance, or might encounter problems with sleeping.
For Walter Gretzky, the Great One’s dad, it was a tremor in his left hand that led to a diagnosis of Parkinson’s disease in 2012. Canadian hockey legend Wayne Gretzky recently shared news of his dad’s passing in a tweet saying, “He bravely battled Parkinson’s and other health issues these last few years, but he never let it get him down.”
Deep Brain Stimulation Surgery For Parkinson’s Disease At Ucla
If you’ve been diagnosed with Parkinson’s, your doctor will first prescribe medication. There are many drugs available that improve symptoms, but they have many side effects, including nausea, hallucinations and impulsive behavior. Some patients respond well to medications for years before seeing side effects. In these patients, the drugs may start to wear off quickly, or they may become extremely sensitive to the drugs and experience too much movement
Deep brain stimulation is a surgical option available to patients who are intolerant of medications or who experience serious side effects. This procedure involves implanting electrodes, or wires, deep inside the brain to change irregular brain activity. As a result, it improves motor function in patients with Parkinson’s disease. It is used more often to treat Parkinson’s disease than any other movement disorder.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
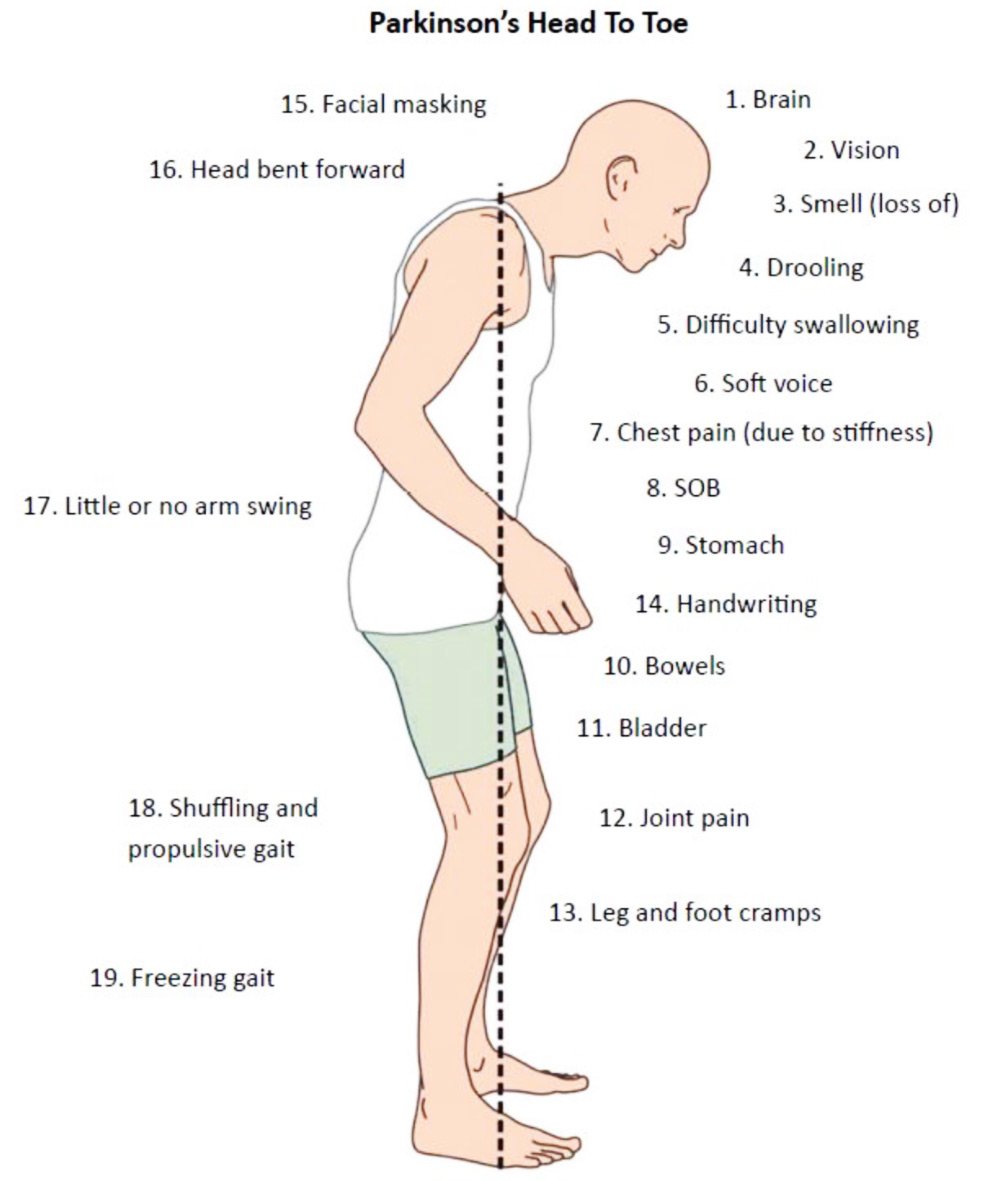
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
Do People Actually Lose Their Sense Of Smell With Parkinson’s
A: Yes. It’s a condition called anosmia, and if you have it with no other disease , you have at least a 50 percent chance of developing Parkinson’s disease in the next five to 10 years. What happens is that alpha-synuclein, the protein that clumps in the part of the brain that regulates dopamine and leads to Parkinson’s disease, also aggregates in the olfactory bulb, the part of the brain responsible for your sense of smell. This happens well before the protein accumulations cause motor symptoms.
What Are The Primary Motor Symptoms Of Parkinsons Disease
There are four primary motor symptoms of Parkinson’s disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinson’s.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinson’s disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinson’s disease has a tremor, nor is a tremor proof of Parkinson’s. If you suspect Parkinson’s, see a neurologist or movement disorders specialist.
Tremors
Read more about Parkinson’s tremors
Rigidity
Bradykinesia
mask-like expression of the face
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
A Balancing Act: The Struggle To Maintain Balance With Pd
With this tool, doctors and researchers might “better manage and treat the disease, as well as use the best candidates for more targeted and effective clinical trials,” the company added.
Scientists analyzed medical records of people registered with the Parkinson’s Progression Markers Initiative , an observational study designed to collect and catalogue as much information on Parkinson’s and its various features over an individual’s life as possible.
Up to seven years’ worth of medical records per person were gathered, covering 423 Parkinson’s patients and 196 healthy people serving as controls.
“Having access to a large dataset is crucial for success in machine learning models,” the company stated, “which is why the troves of data in the PPMI were key to our model’s viability.”
Importantly, the eight states identified by the algorithm largely agreed with clinical observations assigned to each corresponding individual.
The eight states are mainly defined by functional impairment, tremor, a stillness known as bradykinesia, and neuropsychiatric measures. States five and eight, for instance, associated with more postural instability or gait difficulty.
People in the eighth state were more likely than others to develop dementia, or motor symptoms that limited their daily ability to function.
Individual states appeared to influence disease progression. In other words, the state in which a person found themselves was likely to determine their future states.
Deep Brain Stimulation For Parkinson’s: Am I A Candidate
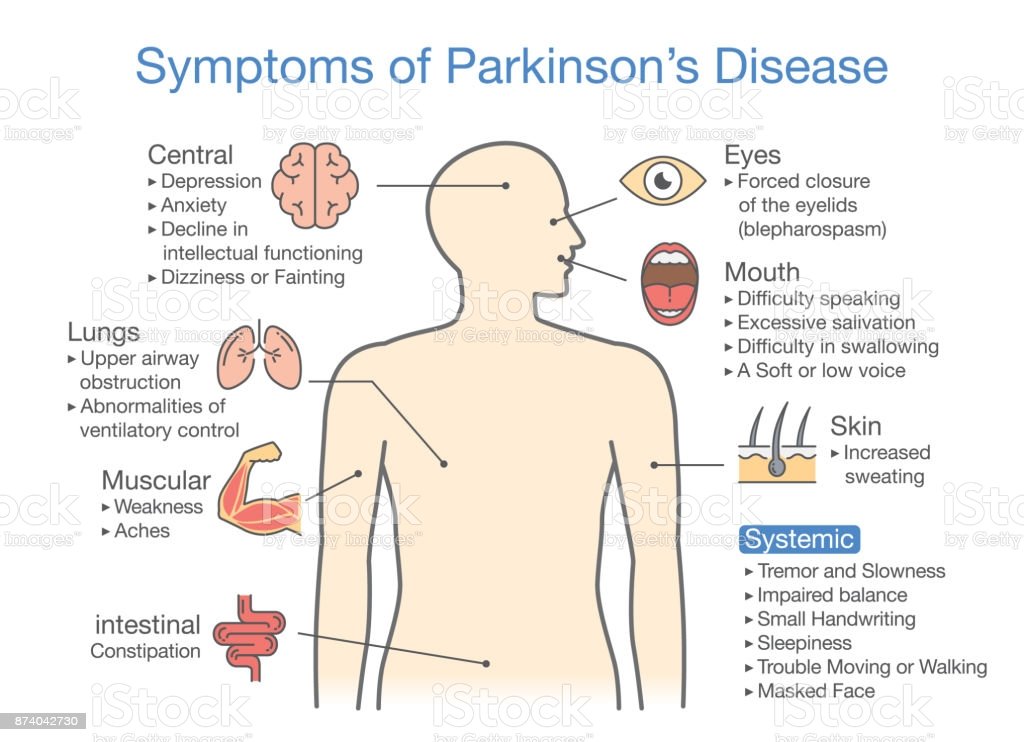
Deep brain stimulation is not a cure, but it can relieve your symptoms from Parkinson’s disease when medications are not an option. Only you and your doctor can decide if this surgical procedure is right for you. You may be a candidate for deep brain stimulation if:
- You have idiopathic Parkinson’s disease. Patients with atypical parkinsonism are not candidates.
- You have good motor function and independence during your best “on” state when taking the drug Sinemet.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinson’s disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinson’s disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinson’s disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinson’s disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinson’s disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Drugs And Medication Used To Treat Parkinsons Disease
A number of different drugs can be used to treat Parkinson’s.
Levodopa
Levodopa is the most common treatment for Parkinson’s. It helps to replenish dopamine.
About 75 percent of cases respond to levodopa, but not all symptoms are improved. Levodopa is generally given with carbidopa.
Carbidopa delays the breakdown of levodopa which in turn increases the availability of levodopa at the blood-brain barrier.
Dopamine agonists
Dopamine agonists can imitate the action of dopamine in the brain. They’re less effective than levodopa, but they can be useful as bridge medications when levodopa is less effective.
Drugs in this class include bromocriptine, pramipexole, and ropinirole.
Anticholinergics
Anticholinergics are used to block the parasympathetic nervous system. They can help with rigidity.
Benztropine and trihexyphenidyl are anticholinergics used to treat Parkinson’s.
Amantadine
Amantadine can be used along with carbidopa-levodopa. It’s a glutamate-blocking drug . It offers short-term relief for the involuntary movements that can be a side effect of levodopa.
COMT inhibitors
Catechol O-methyltransferase inhibitors prolong the effect of levodopa. Entacapone and tolcapone are examples of COMT inhibitors.
Tolcapone can cause liver damage. It’s usually saved for people who do not respond to other therapies.
Ectacapone does not cause liver damage.
Stalevo is a drug that combines ectacapone and carbidopa-levodopa in one pill.
MAO-B inhibitors
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinson’s disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinson’s disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinson’s disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
How To Cope With The Symptoms Of Parkinsons Disease
The only predictable thing about this disease is that it is unpredictable.— Richard, diagnosed at 36
Tremors are the first sign noted in about half of all people with Parkinson’s disease. But maybe, like 15 percent of people with the illness, you have never experienced this symptom. That is because Parkinson’s disease affects everyone somewhat differently.
As you will discover, your symptoms will continue to change, often from day to day, and throughout the course of your life. But even though there is no cure for Parkinson’s, the sooner you can take steps to manage symptoms when they arise, the better chance you will have at maintaining a good quality of life.That is why the first step in coping with the changes that accompany a Parkinson’s diagnosis is to simply increase awareness, to notice new symptoms as well as how your body responds to certain activities, stresses and therapies. A helpful way to do this is by logging your symptom patterns in a daily journal. It is just a matter of jotting down small changes you notice in your physical and emotional health each day. That way you can discuss these issues promptly with your doctor and receive treatment.
Depression May Be An Early Symptom Of Parkinsons
Depression is one of the most common, and most disabling, non-motor symptoms of Parkinson’s disease. As many as 50 per cent of people with Parkinson’s experience the symptoms of clinical depression at some stage of the disease. Some people experience depression up to a decade or more before experiencing any motor symptoms of Parkinson’s.
Clinical depression and anxiety are underdiagnosed symptoms of Parkinson’s. Researchers believe that depression and anxiety in Parkinson’s disease may be due to chemical and physical changes in the area of the brain that affect mood as well as movement. These changes are caused by the disease itself.
Here are some suggestions to help identify depression in Parkinson’s:
- Mention changes in mood to your physician if they do not ask you about these conditions.
- Complete our Geriatric Depression Scale-15 to record your feelings so you can discuss symptoms with your doctor. Download the answer key and compare your responses.
- delusions and impulse control disorders
What Doctors Look For When Diagnosing Parkinsons
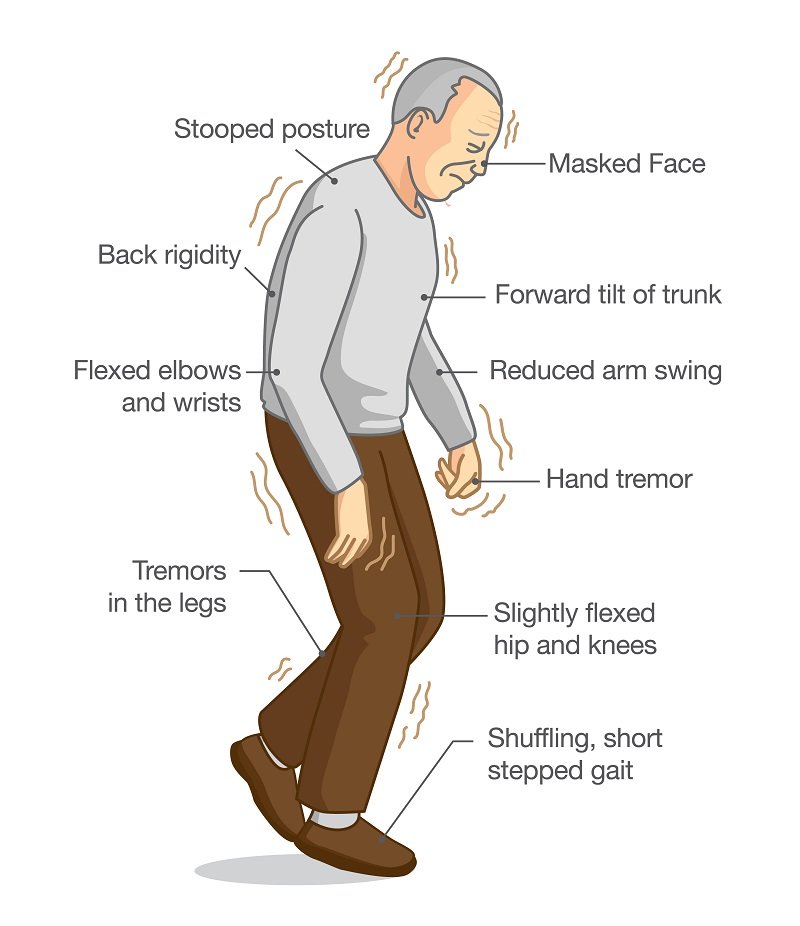
Certain physical signs and symptoms — noticed by the patient or his or her loved ones — are usually what prompt a person to see the doctor. These are the symptoms most often noticed by patients or their families:
-
Shaking or tremor: Called resting tremor, a trembling of a hand or foot that happens when the patient is at rest and typically stops when he or she is active or moving
-
Bradykinesia: Slowness of movement in the limbs, face, walking or overall body
-
Rigidity: Stiffness in the arms, legs or trunk
-
Posture instability: Trouble with balance and possible falls
Once the patient is at the doctor’s office, the physician:
-
Takes a medical history and does a physical examination.
-
Asks about current and past medications. Some medications may cause symptoms that mimic Parkinson’s disease.
-
Performs a neurological examination, testing agility, muscle tone, gait and balance.
The First Motor Symptoms Of Parkinsons Disease
When people ask “what are the early signs and symptoms of PD?” the answer they are typically expecting is one that involves motor symptoms. Early motor symptoms of PD can be a subtle rest tremor of one of the arms or hands . A rest tremor is one that occurs when the limb is completely at rest. If the tremor occurs when the limb is suspended against gravity or actively moving, this may still be a sign of PD, but may also be a sign of essential tremor.
The initial motor symptom of PD may be a sense of stiffness in one limb, sometimes interpreted as an orthopedic problem . This sense of stiffness may be noted when a person is trying to get on his/her coat for example. A person may also experience a sense of slowness of one hand or a subtle decrease in dexterity of one hand. For example, it may be hard to manipulate a credit card out of a wallet or perform a fast, repetitive motor task such as whisking an egg. A person may notice that one arm does not swing when he/she walks or that one arm is noticeably less active than the other when performing tasks. Another motor sign may be a stoop with walking or a slowing down of walking. A family member may notice that the person blinks infrequently or has less expression in his/her face and voice.
These motor symptoms may be very subtle. Bottom line – if you are concerned that you may have an early motor or non-motor symptom of Parkinson’s disease, make an appointment with a neurologist for a neurologic exam to discuss your concerns.
How Early Can Parkinson’s Disease Be Diagnosed
A: A true determination of Parkinson’s disease is a clinical diagnosis, which means certain motor symptoms have to be present, but we now know more about some early signs of Parkinson’s disease that, while they don’t always lead to the condition, are connected.
In terms of how early we can detect, we can detect a mutation that is associated with an increased risk of Parkinson’s as early as birth. In the minority of patients who may have a known Parkinson’s-related genetic mutation , that gene could be tested for at any time in life. At the same time, that’s not diagnosing Parkinson’s; it’s just identifying the risk.
Early warning signs are what we call prodromal, or preclinical, symptoms. Prodromal symptoms are an early warning sign that someone might get Parkinson’s disease. Though some of these symptoms have a very high probability of signaling future Parkinson’s, having one or more of them is still not a 100 percent probability. Some prodromal symptoms are loss of sense of smell, REM behavior disorder, anxiety or depression, and constipation.
Diagnosis And Management Of Parkinsons Disease
There are no diagnostic tests for Parkinson’s. X-rays, scans and blood tests may be used to rule out other conditions. For this reason, getting a diagnosis of Parkinson’s may take some time.
No two people with Parkinson’s disease will have exactly the same symptoms or treatment. Your doctor or neurologist can help you decide which treatments to use.
People can manage their Parkinson’s disease symptoms through:
- seeing a Doctor who specialises in Parkinson’s
- medication
- multidisciplinary therapy provided for example, by nurses, allied health professionals and counsellors
- deep brain stimulation surgery .
Medications For People With Parkinsons Disease
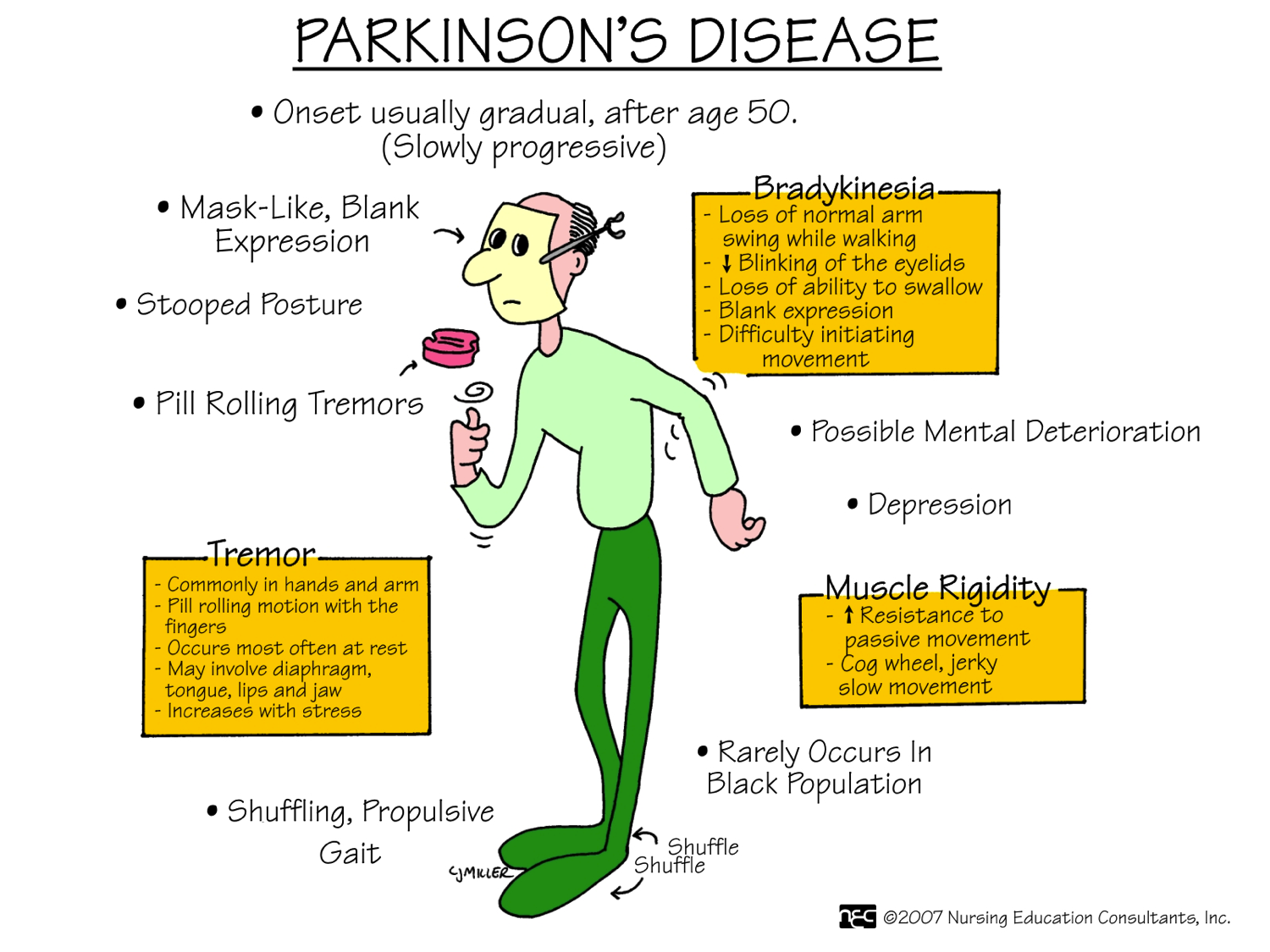
Symptoms of Parkinson’s disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinson’s medications fit into one of the following broad categories:
- levodopa – dopamine replacement therapy
- dopamine agonists – mimic the action of dopamine
- COMT inhibitors – used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics – block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine – has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors – prevent the metabolism of dopamine within the brain.
What Is The Treatment For Parkinson’s Disease
There is currently no treatment to cure Parkinson’s disease. Several therapies are available to delay the onset of motor symptoms and to ameliorate motor symptoms. All of these therapies are designed to increase the amount of dopamine in the brain either by replacing dopamine, mimicking dopamine, or prolonging the effect of dopamine by inhibiting its breakdown. Studies have shown that early therapy in the non-motor stage can delay the onset of motor symptoms, thereby extending quality of life.
The most effective therapy for Parkinson’s disease is levodopa , which is converted to dopamine in the brain. However, because long-term treatment with levodopa can lead to unpleasant side effects , its use is often delayed until motor impairment is more severe. Levodopa is frequently prescribed together with carbidopa , which prevents levodopa from being broken down before it reaches the brain. Co-treatment with carbidopa allows for a lower levodopa dose, thereby reducing side effects.
In earlier stages of Parkinson’s disease, substances that mimic the action of dopamine , and substances that reduce the breakdown of dopamine inhibitors) can be very efficacious in relieving motor symptoms. Unpleasant side effects of these preparations are quite common, including swelling caused by fluid accumulation in body tissues, drowsiness, constipation, dizziness, hallucinations, and nausea.
Slice Title3 Things We Know About Parkinson’s
Parkinson’s develops when cells in the brain stop working properly and are lost over time. These brain cells produce a chemical called dopamine.
Symptoms start to appear when the brain can’t make enough dopamine to control movement properly.
There are 3 main symptoms – tremor , slowness of movement and rigidity – but there are many other symptoms too.
What Are The Symptoms Of Parkinson’s Disease
Parkinson’s disease is a movement disorder that progresses slowly. Some people will first notice a sense of weakness, difficulty walking, and stiff muscles. Others may notice a tremor of the head or hands. Parkinson’s is a progressive disorder and the symptoms gradually worsen. The general symptoms of Parkinson’s disease include:
- Slowness of voluntary movements, especially in the initiation of such movements as walking or rolling over in bed
- Decreased facial expression, monotonous speech, and decreased eye blinking
- A shuffling gait with poor arm swing and stooped posture
- Unsteady balance; difficulty rising from a sitting position
- Continuous “pill-rolling” motion of the thumb and forefinger
- Abnormal tone or stiffness in the trunk and extremities
- Swallowing problems in later stages
- Lightheadedness or fainting when standing
The Clinical Symptoms Of Parkinson’s Disease
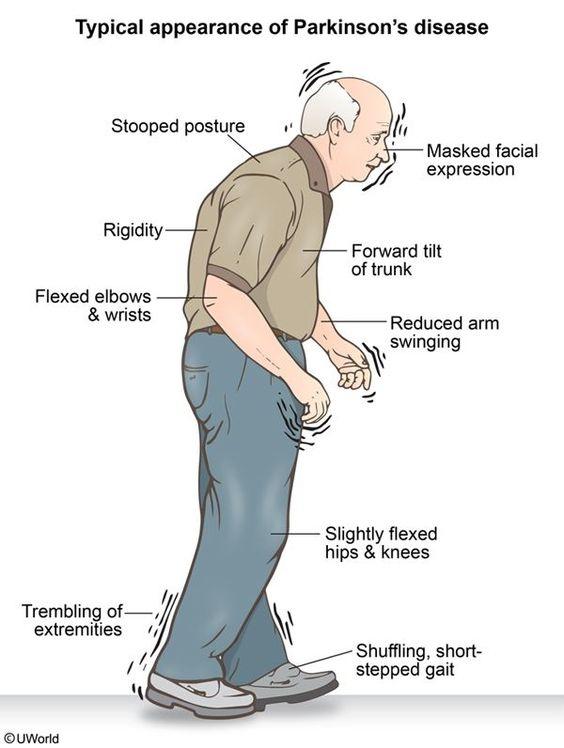
Department of Neurology, Broomfield Hospital, Chelmsford, Essex, CM1 7ET UK
Queen Mary School of Medicine and Dentistry, University of London, London, UK
Department of Neurology, Broomfield Hospital, Chelmsford, Essex, CM1 7ET UK
Queen Mary School of Medicine and Dentistry, University of London, London, UK
sigurlaug.sveinbjornsdottir@meht.nhs.ukSearch for more papers by this author
What Are The Symptoms Of Parkinsons Disease
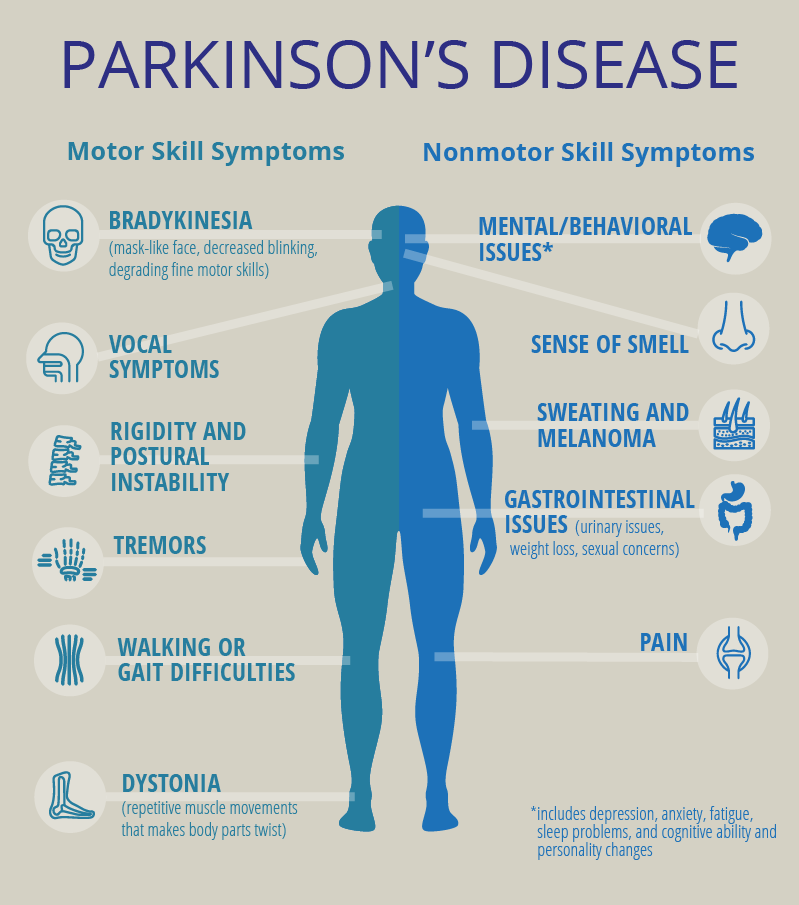
Symptoms of Parkinson’s disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Decreased facial expressions: You may not smile or blink as often as the disease worsens; your face lacks expression.
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinson’s disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinson’s. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinson’s disease. Electrical impulses are introduced to the brain, which has the effect of ‘normalising’ the brain’s electrical activity reducing the symptoms of Parkinson’s disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
