The Effects Of Parkinson’s Disease Can Creep Up On Us Exercise Has Been Shown To Fend Off Parkinson’s Disease Symptomsit’s

Make exercise part of your daily routine. For those at risk for Parkinson’s disease, consistent physical activity can delay the symptoms.
About 60,000 people are diagnosed with Parkinson’s disease each year; most are over age 60, and men are twice as likely to have it as women. Early Parkinson’s disease symptoms are subtle, occur gradually, and may go unnoticed for some time. As the disease progresses, however, the shaking, or tremor, that affects the majority of people with PD, may begin to interfere with daily activities.
Patients may also experience other symptoms, such as sleep issues, depression, and cognitive decline. To combat those symptoms, neurologists–specialists in treating Parkinson’s disease–are increasingly prescribing exercise as part of their recommended treatment plan.
“Exercise is like medicine and is used along with medications,” says neurologist Indira Subramanian, MD, UCLA Department of Neurology. “It’s part of our counseling from day one because it helps patients overall and may slow down the progression of the disease.”
If Someone Did Not Have Parkinsons Before Is It Likely That They Will Develop It After Recovering From Covid
Dr. Okun: We do not have the numbers on how common it is to receive a Parkinson’s diagnosis after recovering from COVID-19. There are several intriguing papers on how COVID-19 may affect the brain and how it may possibly contribute to Parkinson’s risk. At this point, we caution the public and researchers not to speculate until we have more data.
Weedkiller Paraquat Linked To Parkinsons And Deadly Diseases & Keystone Xl Pipeline Officially Ends
Via America’s Lawyer: Roundup is far from the only herbicide that’s caused concern among medical professionals. Paraquat has been around since the 90’s and has been called the deadliest weedkiller on the planet after being directly linked to Parkinson’s disease and a litany of other deadly ailments. Attorney Alex Taylor joins Mike Papantonio to describe how regulators have whitewashed the dangers of Paraquat over the course of decades. Plus, Environmentalists cheer the official end of the Keystone XL Pipeline as TransCanada finally pulls the plug on the hotly-debated project. Mike Papantonio and discuss more.
Transcript:
*This transcript was generated by a third-party transcription software company, so please excuse any typos.
Mike Papantonio: Roundup is far from the only weed killer that’s caused a stir among medical professionals, another popular herbicide called Paraquat has been called the deadliest weed killer on the planet. Yet, it’s still being sold on the shelves. I have Alex Taylor who’s after these folks to try to hold them responsible for what they’ve done, Alex, I mean the headline, three drops of Paraquat will kill you. Okay. Inhalation will cause Parkinson’s disease. Talk about it.
Alex Taylor: Absolutely. And that’s, that’s no joke. If you were to take just a couple of drops, put them in your mouth and then spit them right back out.
Mike Papantonio: You’re dead.
Alex Taylor: That would be enough exposure to kill you.
Mike Papantonio: Yeah.
I Have Parkinsons And Blood Pressure Issues Should I Be Worried About Getting The Vaccine
Dr. Okun: No. You will most likely be sitting when you get the vaccine, so if you get faint or have a change in your blood pressure you should be okay. Stay hydrated; it will help with changes in blood pressure. Take a water bottle and a snack with you. You will likely be asked to sit in a waiting area for 15-20 minutes after each shot to make sure you do not have a reaction. If you can drink a small bottle of water either immediately before or immediately after the shot, we believe this is a good idea, especially if prone to fainting.
What Do People With Parkinsons Need To Bring With Them For Their Vaccine Appointment
Dr. Okun: Take your personal information and medication list. If you are prone to fainting, let the nurse know. For the second shot, bring the card issued to you on the first shot, so that the vaccine administration can be documented. Take a picture of the card once you have both shots so that you always have a copy.
What Other Conditions Have Similar Symptoms And Signs Of Parkinsons Disease
Other neurological diseases may cause symptoms similar to Parkinson’s disease. The term Parkinsonism refers to a patient that has symptoms similar to Parkinson’s.
Early in the disease process, it can be tough to make an assertive diagnosis and difference between Parkinson’s and Parkinson-like diseases.
Often the correct diagnosis is made after further symptoms develop, and the physician can monitor the course of the disease.
The development of additional symptoms and the course of the illness generally points towards the correct diagnosis. These are the most common neurological diseases that can produce Parkinson-like symptoms.
- Progressive Supranuclear Palsy
- Lewy Body disease or Dementia with Lewy bodies
- Corticobasal degeneration or corticobasal ganglionic degeneration
Nonetheless, doctors should think of other causes rather than Parkinson’s disease when events like this happen.
- Poor response to dopamine
- Early loss of balance or vision problems
- Prominent intellectual decline – dementia
- Rapid onset or progression of the disease
Actually, though it is a disease that is not clearly understood, there are specific organizations like Parkinson’s UK that dedicate themselves to doing research.
These organizations look forward to following the natural course of the disease and developing clinical trials for patients in an attempt to find a cure.
Combating Parkinsons Disease Symptoms: Start Sooner Rather Than Later
Researchers from the National Parkinson’s Foundation looked at data on more than 1,300 of the study participants who reported little regular exercise at the beginning of the study. Five hundred of those individuals began exercising more than 2.5 hours per week within the next two years.
The researchers compared participants who exercised regularly for the entire two years to people who didn’t exercise at the beginning of the study, but then started to exercise regularly. Over the two-year study period, quality of life scores worsened 1.4 points in the early starters and 3.2 points in the late starters.“This design is the standard approach to show that an intervention slows the disease: If it just improved symptoms, people who start late would get the same benefit as those who start early,” explains Peter Schmidt, PhD, NPF’s Senior Vice President and an author of the study. “We found that people who start exercise early get more benefit than those who start late.”
The study didn’t separate types of exercises, just the total exercise reported.
“There is some controversy about exercise intensity, and whether it should be one-on-one or in a group,” says Dr. Subramanian. “What matters is getting the heart rate up and staying challenged. It’s also important not to water it down just because someone has been diagnosed with the disease.”
Rock Steady Boxing is a program designed for those who are battling Parkinson’s disease; see sidebar below.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
What Is The Main Cause Of Death In Parkinsons Disease Patients

Parkinson’s is often referred to as a “bespoke” disease because it affects each patient differently. Another factor worth considering is that Parkinson’s disease generally affects people in their 60s, most of whom die of unrelated conditions such as cancer, heart disease or stroke. However, the most common cause of death in those with Parkinson’s disease is pneumonia. This is because the disease can impair your ability to swallow in the later stages, putting you at risk for aspirating food or liquid into the lungs.
Know The Causes Symptoms And Treatment Of This Nerve Disorder
Parkinson’s disease, a chronic and progressive nerve disorder, affects as many as one million Americans, with 60,000 people diagnosed each year. You might have questions like: What is Parkinson’s disease? Who gets it, what are the symptoms, and is there a cure? Here’s what you need to know.
Who Is At Risk?
Age is one of the biggest risk factors for Parkinson’s. The disease develops most often after age 60 and occurs more often in men than in women. Early-onset Parkinson’s can strike people under age 50. In very rare cases, symptoms may even appear at age 20 or younger.
Causes
The underlying . Roughly 15% of people with Parkinson’s have a family history of the disease. Some research suggests that certain pesticides can increase the risk of developing the disease. And mounting evidence connects head injuries and concussions—especially knockout blows—to Parkinson’s, with one study showing that they can more than double the risk.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
Is Parkinsons Disease Fatal Life Expectancy For Parkinsons Emma-Marie Smith
Worried about your Parkinson’s disease life expectancy? A Parkinson’s disease diagnosis comes with many worries and anxieties. One worry concerns the progression of the disease and whether Parkinson’s disease can be fatal. The issue is rarely straightforward, but there is no reason to think your condition is a death sentence. Many people live for years or decades with their Parkinson’s disease symptoms under control, while the illness progresses more quickly for others. It’s important that you know what to expect when you’re diagnosed with Parkinson’s disease, so don’t be afraid to ask questions and air your concerns to your doctor. For now, let’s explore the issue of life expectancy of patients with Parkinson’s disease and address some common concerns.
Do People With Parkinsons Get Priority Access To The Covid

Each state has its own process for rolling out the vaccine to different population groups. If you would like to advocate for people with Parkinson’s to be part of a priority group, we encourage you to contact your elected officials. We have created a letter that you can personalize and send them either by mail or electronically.
How Can Falls Resulting From Parkinsons Disease Be Fatal
Patients with Parkinson’s disease are seen to be at an increased risk of bad falls which can lead to death. Generally it is seen that death results from hip fractures that require hospitalization because surgery would be required. Hip surgery is a major operation which carries the risk of infection, heart failure and blood clots. Such clots become dangerous if they reach the lungs. Sometimes fall may even lead to fatal brain injuries if not taken care properly.
Janet Reno’s Death: How Does A Person Die Of Parkinson’s
Former U.S. Attorney General Janet Reno has died at age 78 from complications of Parkinson’s disease, her family announced today. But how do people die from this disease?
In patients with Parkinson’s disease, the brain cells that produce a chemical called dopamine start to die off. It’s not clear what triggers the death of these cells, but researchers do know that dopamine is important for the control of muscle movement. Parkinson’s patients experience symptoms such as tremors, slowed movements, muscle stiffness and impaired balance.
Parkinson’s itself is usually not considered a deadly disease, and many people with the disease have a life expectancy that’s close to the average life expectancy in the general population, according to the Parkinson’s Disease Foundation.
“You die with Parkinson’s disease, not from it,” according to the Michael J. Fox Foundation for Parkinson’s Research. Reno’s family did not release any further details about her death.
But in some cases, advanced symptoms of Parkinson’s disease can lead to complications that result in death, the Michael J. Fox Foundation says. For example, patients can have problems swallowing because they have a loss of control over the muscles in their throat.
Patients also may have impaired balance, which can result in falls that lead to serious or even fatal injuries, the Michael J. Fox Foundation says.
Myth 4: Aside From Medication There Isnt Much You Can Do
Fact: This “it is what it is; there’s nothing I can do to help myself” myth is counterproductive. There is a lot you can do — chiefly, keeping as active as you can. A recent study found that patients with Parkinson’s who took part in weekly, hourlong exercise sessions were able to do more in their daily lives than those who did not.
Complications Related To Parkinson’s Can Affect Survival

Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology.
Parkinson’s is a common neurodegenerative disease, and although it is not fatal, research suggests it may influence life expectancy.
A 2012 study in Archives of Neurology examined the six-year survival of nearly 140,000 Medicare beneficiaries with Parkinson’s disease in the United States. During the six-year period, 64% of the participants with Parkinson’s disease passed away.
The risk of death of those with Parkinson’s was then compared to Medicare beneficiaries who did not have Parkinson’s or any other common diseases, including:
When controlling for variables like age, race, and gender, the six-year risk of death among people with Parkinson’s was found to be nearly four times greater than those Medicare beneficiaries without the disease or other common diseases.
At the same time, the rate of death among those with Parkinson’s disease was similar to those with hip fracture, Alzheimer’s dementia, or a recent heart attack—although it was higher than those who had been newly diagnosed with either colorectal cancer, stroke, ischemic heart disease, or chronic obstructive pulmonary disease.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Parkinsons Disease Late Stages: What Will Happen To Me
With advanced Parkinson’s disease, stage 5 life expectancy can be months or years depending on how your condition presents. You are likely to need round-the-clock care at this stage, and you may not be able to move around independently. Patients with late-stage Parkinson’s disease are more susceptible to pneumonia, sepsis, pyelonephritis and decubitus ulcers. Late-stage Parkinson’s also leads to Parkinson’s disease dementia in 50% of cases. For all of these reasons, many late-stage Parkinson’s patients are cared for by loved ones or in a hospice.
Myth 6: Deep Brain Stimulation Is Experimental Therapy

Fact: Deep brain stimulation, or DBS, is a procedure in which doctors place electrodes in the brain at the point when medications are less effective in masking motor symptoms, such as tremor, stiffness and slowness of movement.
While it may sound frightening and futuristic, it’s been around and successfully used for decades. DBS works very similarly to a pacemaker, except the wire is in the brain, not in the heart. It’s been a standard procedure for the past two decades.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinson’s disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinson’s disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinson’s disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinson’s disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinson’s disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
How To Take Care Of Patients With Parkinsons Disease
The condition of Parkinson’s disease progress with time and demands care from a care giver. The disease affects the motor abilities of the patient and the gradual loss of independence can be disheartening. Care givers should-
Emotional Support: Try maintaining the quality of life of the patient with proper mental support.
Follow-Up: It is the responsibility of the caregiver to take the patient for proper follow-ups to the doctor.
Diet: The care giver should keep an eye on the diet of the patient. He should have a balanced and nutritious diet. He should also be motivated to exercise regularly.
Learn More About the Disease:The care giver should make attempts to learn about the symptoms of Parkinson’s disease in order to provide sufficient empowerment to the patient.
Im Allergic To Other Vaccines Should I Get The Covid
Dr. Okun: In many cases, people with allergies to vaccines may possibly receive the Moderna or Pfizer vaccines. Side effects including allergies to vaccines are usually caused by the fluid surrounding the vaccine itself. Do not assume you cannot get this vaccine; talk to your doctor. Old fashioned vaccines are manufactured in a completely different fashion as compared to the current COVID-19 vaccinations. It will be rare for someone to not be able to receive the vaccines; we believe most people are eligible.
What Are The Differences Between Available Vaccines

Dr. Okun: Moderna and Pfizer vaccines are distributed in the U.S. and in other countries, with 94 and 95 percent effectiveness. Both require two dosages and need to be stored at incredibly low temperatures — the Pfizer vaccine requiring an even lower storage temperature than the Moderna vaccine — making distribution and storage a challenge. These two vaccines belong to a new treatment approach called messenger RNA vaccines, which create a COVID-19 defense system.
Other vaccines are in development around the world and most work more like a traditional vaccine . They send instructions through DNA, teaching the immune system how to respond to COVID-19. There are several vaccines in early development, but these have the most available information:
- Oxford–AstraZeneca: distributed in the U.K. with ~70 percent effectiveness. It works in two dosages. The major benefit to this vaccine is that it can be stored at refrigerator temperatures. The vaccine may be more effective if a weakened first shot is followed a few weeks later by a standard dose.
- Sinovac and Sinopharm: created in China with ~78-80 percent effectiveness using two dosages. There is limited data on these vaccines. Sinovac is currently in late-stage trials in other countries.
- Sputnik V: distributed in Russia and works using two dosages. Early reports are of ~92 percent effectiveness. However, there is limited data on this vaccine.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinson’s disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinson’s disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinson’s disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
How Does The Parkinsons Disease Progress Over Time
Although slow, Parkinson’s disease is progressive in nature where the condition keeps worsening at every stage.
In the initial stage, the symptoms are seen to be mild in nature. The symptoms do not really interfere with the daily tasks and the lifestyle of the patient. The tremors and problems with balance, movement starts from one side of the body.
The next phase is characterized by moderate form of the symptoms which are distinctively noticed by people. The muscles become stiff and posture is likely to be irregular. Exercise may be recommended by the doctor to ease out the stiffness. However, balance of the patient is not much impaired.
The next stage is considered to be the turning point of the symptoms because the patient may start to lose control over his balance of the posture. He may also experience decreased reflex and is more prone to fall down while his movements become slower. In this stage, occupational therapy is required to help the patient with the stiffness and fine motor abilities.
In the second last stage the patient may not even be able to stand without help. The patient should not live alone because daily activities cannot be done independently. It is extremely important to have the assistance if a care giver at this stage.
Also Read:
Psoriasis Trigger Lurking In Your Medicine Cabinet
Dear?Turapür?Today?Reader, If you’ve ever been diagnosed with psoriasis, you know first-hand just how uncomfortable it can be. Whether it’s the itchy, flaky skin that causes you to cover up every square inch of your body… to the pain and inflammation it can cause in your joints… psoriasis goes way beyond your run-of-the-mill ‘skin condition.’ To…
We Have Choices About How This Condition Plays Out

In fact, medical scientists have proved that many people with a genetic disposition to this never get it.
While others with no genetic disposition at all still get full-on Parkinson’s that ravages their mental health quickly and remorselessly.
It’s not genetics. It’s a basic illness with recognized causes.
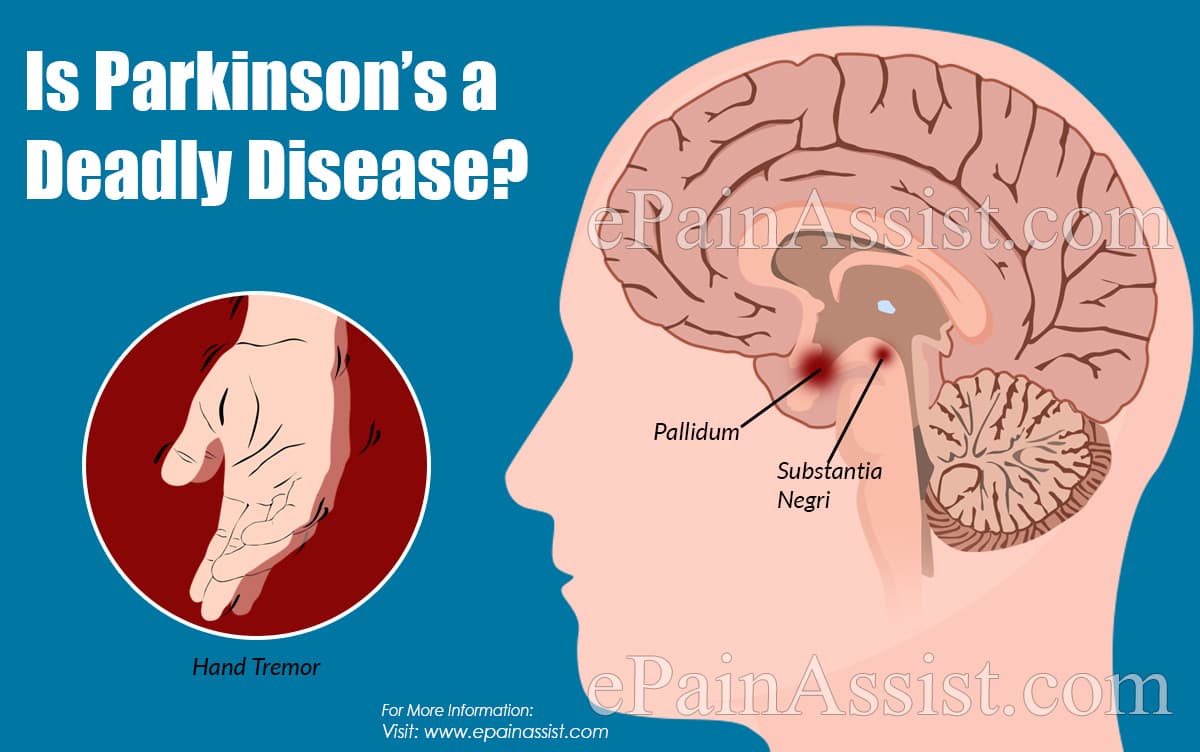
Remember: the substantia nigra produces dopamine. It’s the loss of substantia nigra nerve cells that leads to the loss of dopamine.
And that loss of dopamine leads to Parkinson’s Disease.
So the big question is:
Why on earth is the substantia nigra losing those dopamine-producing cells in the first place?
I was shocked to discover that we already know why we’re losing those priceless, life-giving substantia nigra cells.
Yet still do almost nothing about it…
Prevalence And Risk Of Attempted And Fatal Suicide
Twenty-one articles discussed prevalence and risk of attempted or fatal suicide in PwP. All of these studies were observational and all were rated as low or moderate quality. The first paper to report on suicide in PD was the 1967 article by Hoehn and Yahr, which described causes of mortality in parkinsonism. Among 340 patients with Parkinson’s disease who died during the study period, three died by suicide.s1 Importantly, there was little distinction between idiopathic and atypical parkinsonian syndromes at that time, and the extent to which this contributed to the suicide rate is unclear.
Most of the research reviewed suggested an elevated suicide risk in PwP.s2–s6 Risk varies by population; for example, a group in South Korea found a standardised mortality ratio for suicide in PwP of 1.99 .s4 In the Netherlands, the OR for PD was 2.9 in those who attempted suicide via poisoning.s6 Studies of Serbian and British populations have demonstrated a suicide risk over five times that of the general population matched for age and sex.s5,s7 In British Columbia, suicide is the second most common cause of injury-related mortality in PwP.s8
Unlike deaths, SAs are difficult to accurately measure in large retrospective studies. Several researchers have noted no SAs in their study population.s15,s16 Others have found that PwP have a lifetime rate of SAs similar to the general population .s17-s19,24
Parkinson Disease: An Evolving Clinical Phenotype
As previously described, approximately 90 % of PD is sporadic, but the discovery that specific genes underlie the development of PD has kindled new approaches to understanding both the clinical and neuropathological characteristics of the disorder, as well as approaches to understanding pathogenesis and treatment. For instance the discovery that familial PD is linked to missense mutations in the synuclein gene led to the development of immunocytochemical methods that revealed ?-synuclein to be the major constituent of the ‘Lewy body’ in both sporadic and genetic variants of PD. ?-Synuclein contributes to the cytoplasmic and nuclear accumulations in neurons and glia in a range of disorders: MSA, DLBD, LBD, NBIA1 and amyotrophic lateral sclerosis . It is apparent that synuclein pathology underlies a range of neurodegenerative disorders and the term ‘synucleinopathies’ was coined . Thus, PD is no longer a single nosological entity and along with the aforementioned diseases, is now considered a multisystem ?-synucleinopathy.
Why Does Modern Medicine Know This But Ignore It
Why don’t we tackle the inflammation and toxins causes of those nerve cells continually dying in the substantia nigra?
My doctor told me: it’s cultural.
Most patients – especially in western countries – want a drug or a procedure for a problem.
Something that’s a one-off fix – like an operation.
Or an easy, regular thing – like a course of tablets.
What they don’t want to have to make an effort to heal themselves. So pills it is.
But most inflammatory diseases can be tackled more effectively by lifestyle changes than by drugs.
Whole classes of deadly modern illnesses can be changed by a small number of simple, targeted lifestyle tweaks.
But our medics push meds because they know that, mostly, their patients won’t make lifestyle changes.
So they give their patients drugs – knowing that they’ll at least take them.
Frustratingly, the best solution – addressing lifestyle factors – isn’t at all difficult. It’s just that popping a pill is easier.
What Is The Cause Of Death In Parkinsons Disease
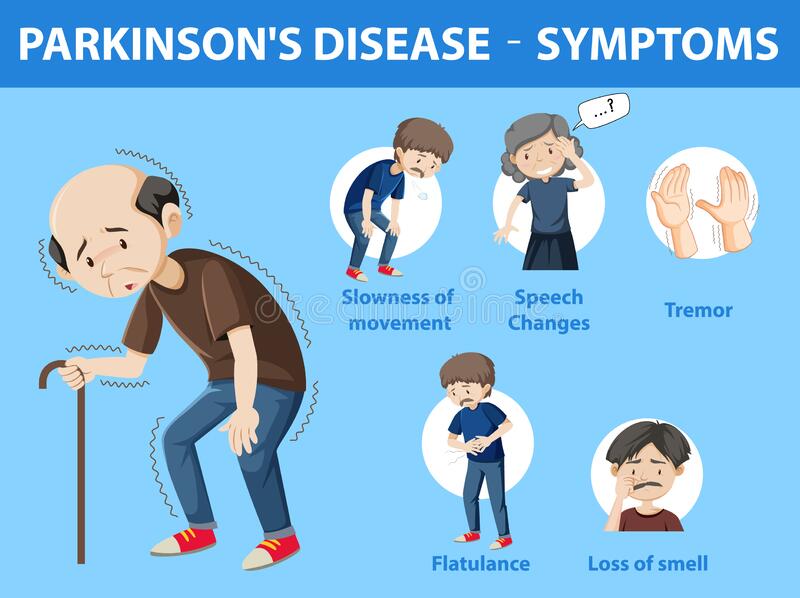
Parkinson’s disease itself is not fatal. Nevertheless, the symptoms associated with it can be quite dangerous because they affect the motor abilities of the patient. If motor abilities are affected, the patient may lose balance and fall. Falls can be pretty dangerous in unsafe environment which may eventually lead to death. Other complications with swallowing and dementia may also be fatal if proper care is not taken.
