What Causes Parkinsons Disease
The most prominent signs and symptoms of Parkinsons disease occur when nerve cells in the basal ganglia, an area of the brain that controls movement, become impaired and/or die. Normally, these nerve cells, or neurons, produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems associated with the disease. Scientists still do not know what causes the neurons to die.
People with Parkinsons disease also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying position.
Many brain cells of people with Parkinsons disease contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons andLewy body dementia.
Who Is Affected By Parkinsons Disease
Parkinsons disease affects both men and women. Statistically, however, men have a slightly higher chance of developing the disease. The risk of developing Parkinsons disease also increases with age, with the average age of onset being 65 years old. Five to ten per cent of people develop the condition before the age of 40 years old. When symptoms appear in people aged 21-40, this is known as young-onset Parkinsons disease. Juvenile Parkinsons disease is the term used when symptoms appear before the age of 18 years old, although this is extremely rare.
To-date, no one knows exactly why people get Parkinsons disease, but viral infection or environmental toxins may play a role. People with a parent, sibling or child with Parkinsons disease, are twice as likely to get it as people in the general population.
General Comments On Methodology
This analysis identified many potentially important differences in the incidence of PD, which could possibly be attributed to environmental or genetic factors. However, as this meta-analysis contains studies with a range of methodological strategies, the differences between age- and gender-specific incidence may also be due to methodological differences or potential population confounders. Ideally, only studies using the same methods of case ascertainment would be combined in the meta-analysis. However, only 27 studies of PD incidence were found, with only 14 providing data that could be combined in the meta-analysis. There were only a few studies that used identical methodologies for case ascertainment. As all methods of case ascertainment have drawbacks, including attrition, misclassification, and nonresponse, the quality of individual studies may be equally as important as the method of case ascertainment in determining PD incidence. Therefore, we chose to combine studies using different methodologies and examine closely for heterogeneity using the I2 statistic calculated from the Cochrane Q chi-square test for heterogeneity. I2 values showed low to moderate heterogeneity in the female age groups from 40 to 70, with considerable heterogeneity in those 70-79 and 80+. Similarly, heterogeneity increased with age in males, though considerable heterogeneity was found in all age groups over 50.
You May Like: What Foods Should Be Avoided If You Have Parkinson’s Disease
Incidence Of Parkinsons Disease
Its estimated that approximately four people per 1,000 in Australia have Parkinsons disease, with the incidence increasing to one in 100 over the age of 60. In Australia, there are approximately 80,000 people living with Parkinsons disease, with one in five of these people being diagnosed before the age of 50. In Victoria, more than 2,225 people are newly diagnosed with Parkinsons every year.
Symptoms Of Parkinsons Disease
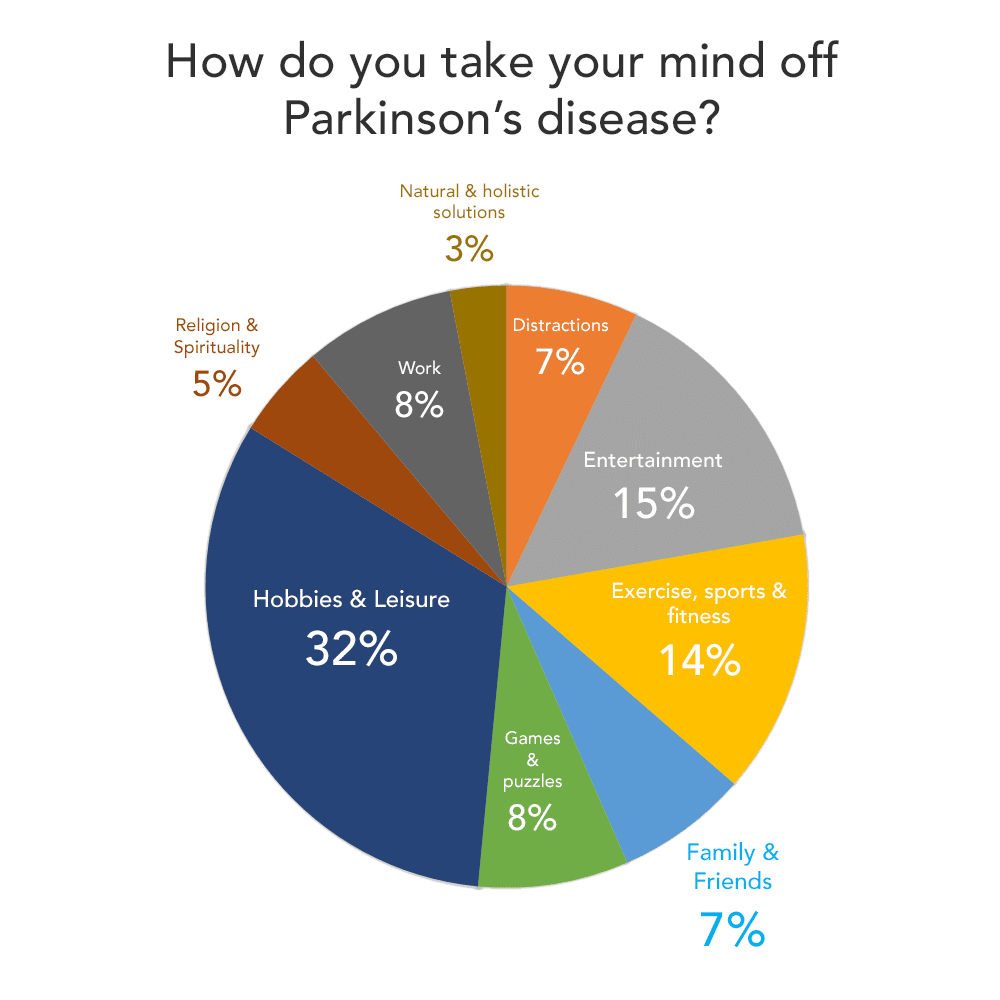
Parkinsons has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Muscle stiffness, where muscle remains contracted for a long time
- Slowness of movement
- Impaired balance and coordination, sometimes leading to falls
Other symptoms may include:
The symptoms of Parkinsons and the rate of progression differ among individuals. Early symptoms of this disease are subtle and occur gradually. For example, people may feel mild tremors or have difficulty getting out of a chair. They may notice that they speak too softly, or that their handwriting is slow and looks cramped or small. Friends or family members may be the first to notice changes in someone with early Parkinsons. They may see that the persons face lacks expression and animation, or that the person does not move an arm or leg normally.
People with Parkinson’s disease often develop a parkinsonian gait that includes a tendency to lean forward take small, quick steps and reduce swinging their arms. They also may have trouble initiating or continuing movement.
Symptoms often begin on one side of the body or even in one limb on one side of the body. As the disease progresses, it eventually affects both sides. However, the symptoms may still be more severe on one side than on the other.
Also Check: What Are The Early Symptoms For Parkinson Disease
What Is Parkinsons Disease
Parkinson’s disease belongs to a group of conditions called motor system disorders, which are the result of the loss of dopamine-producing brain cells. Parkinson’s disease is a brain disorder that leads to shaking, stiffness, and difficulty with walking, balance, and coordination. Symptoms generally develop slowly over years. Parkinson’s symptoms usually begin gradually and get worse over time.
This Technology Listens To Your Breath To Diagnose Early
No uncomfortable wearables required.
In 1817, Jacob Parkinson, an English surgeon and polymath, published a brief, 66-page booklet on a condition that was little known to the medical community. In An Essay on the Shaking Palsy, Parkinson described, in excruciating detail, his observations of six individuals demonstrating varying degrees of the same symptoms: involuntary tremors, difficulty walking, muscle weakness, and slurred speech.
As you may have guessed, Parkinson was describing the disease now bearing his name, a neurodegenerative condition that affects nearly a million U.S. adults. Over the last two hundred years, weve since discovered the why behind the disease destruction of neurons producing the neurotransmitter dopamine and how to treat it through a variety of innovative means.
But doctors still struggle to diagnose Parkinsons in the first place, particularly in its early stages. Scientists are aiming to change that with a new AI-powered device that can help diagnose Parkinsons from breathing patterns, according to a paper published last month in the journal Nature Medicine.
Heres the background The Parkinsons-detecting device relies on a technology called wireless sensor networks , says Dina Katabi, a senior study author and professor in MITs Department of Electrical Engineering and Computer Science.
Don’t Miss: What Is A Good Diet For Parkinson’s Disease
Sidebar: Ninds Steps Up Pursuit Of Pd Biomarkers
In 2012, the NINDS dramatically accelerated efforts to identify biomarkers by establishing the Parkinsons Disease Biomarkers Program . This unprecedented program unites a range of stakeholders from basic and clinical researchers to healthcare professionals, the NINDS staff, information technology experts, and people living with PD and their families.
PDBP supports research and builds resources aimed at accelerating the discovery of biomarkers to ultimately slow the progression of PD. For example, the program has established a repository of biological specimens and a Data Management Resource system maintained by the NIH Center for Information Technology. The DMR allows researchers to access clinical, imaging, genetic, and biologic data, while a complementary PDBP-supported project develops statistical tools to analyze vast quantities of data so that patterns can be identified across these diverse sources of information.
Parkinson’s Disease By Age And Gender
Parkinsons disease generally affects people who are over 60 years old. Early-onset Parkinsons disease is defined as beginning before age 50. The prevalence of Parkinsons disease increases with increasing age, and it is estimated to affect 1 in 40 people who are 85 to 89 years old.
People who begin to have symptoms at an older age generally have more severe symptoms and also have more comorbid conditions , such as heart disease, lung disease, or diabetes.
Parkinsons disease is more common among males than females, affecting approximately twice as many males.
You May Like: How Long Does Parkinson’s Disease Last
Is There Treatment For Parkinsons Disease
At present, there is no cure for PD, but a variety of medications provide dramatic relief from the symptoms. Usually, affected individuals are given levodopa combined with carbidopa. Carbidopa delays the conversion of levodopa into dopamine until it reaches the brain. Nerve cells can use levodopa to make dopamine and replenish the brain’s dwindling supply. Although levodopa helps at least three-quarters of parkinsonian cases, not all symptoms respond equally to the drug. Bradykinesia and rigidity respond best, while tremor may be only marginally reduced. Problems with balance and other symptoms may not be alleviated at all. Anticholinergics may help control tremor and rigidity. Other drugs, such as bromocriptine, pramipexole, and ropinirole, mimic the role of dopamine in the brain, causing the neurons to react as they would to dopamine. An antiviral drug, amantadine, also appears to reduce symptoms. In May 2006, the FDA approved rasagiline to be used along with levodopa for patients with advanced PD or as a single-drug treatment for early PD. In March 2017, the FDA approved safinamide tablets as an add-on treatment for individuals with PD how are currently taking levodopa/carbidopa and experiencing “off” episodes .
Support For People Living With Parkinsons Disease
While the progression of Parkinsons is usually slow, eventually a persons daily routines may be affected. Activities such as working, taking care of a home, and participating in social activities with friends may become challenging. Experiencing these changes can be difficult, but support groups can help people cope. These groups can provide information, advice, and connections to resources for those living with Parkinsons disease, their families, and caregivers. The organizations listed below can help people find local support groups and other resources in their communities.
Also Check: What Is Deep Brain Stimulation For Parkinson’s Disease
Causes Of Parkinson’s Disease
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Improving Diagnosis With Composite Scores
A diagnostic challenge, particularly outside of expert centers, there are long delays in diagnosing LBD leading to significant burden. Although consensus criteria have excellent specificity, there is no standardized way to assess symptoms, reducing sensitivity. We developed the LB Composite Risk Score 21 from autopsy-verified cases to improve the ability to detect LBD in clinic and research populations .
Figure. Diagnostic Tools for Dementia With Lewy Bodies. The Lewy Body Composite Risk Score is a 10-item questionnaire to capture signs and symptoms associated with Lewy body pathology. A score of 3 or greater represents a high probability that Lewy bodies are contributing to cognitive decline . Comparison of MRI in Alzheimers disease and dementia with Lewy bodies demonstrates less cortical and hippocampal atrophy in DLB . Comparison of dopamine transporter single photon emission tomography in AD and DLB shows decreased dopamine uptake in the basal ganglia in DLB vs normal uptake in AD.
You May Like: How Close Is A Cure For Parkinson’s Disease
Neuropsychological And Behavioral Assessment
All the enrolled patients, at baseline and follow-up, underwent a comprehensive neuropsychological assessment when in on state. Neuropsychological evaluations were performed by neurologists with a specific expertise in neuropsychology and dementia, and the same rater performed both baseline and follow-up assessments.
Patients underwent a Level I MDS criteria evaluation of global cognition using the following tests: the Mini Mental State Examination , the Montreal Cognitive Assessment , and the Frontal Assessment Battery .
According to MDS Level II criteria , two tests for cognitive domains have been performed. The memory domain has been assessed with the Reys Auditory Verbal Learning Test and the Prose recall test with a delayed recall condition the attention domain with the Stroop color-word test and the Trail Making Test part A the executive function domain with the Verbal fluency letter test and the Colored Ravens Progressive Matrices the visuo-spatial function domain with the Clock drawing test and the Copy of figures lastly, the language domain has been assessed with the Aachener Aphasie Test-Naming item and the short version of the Token test .
For each test, details regarding administration procedures and Italian normative data for score adjustment were used. Neuropsychological performances were considered as impaired when the subject scored 2 standard deviation below normality cut-off values.
Dont Miss: Does Vitamin B12 Help Parkinsons
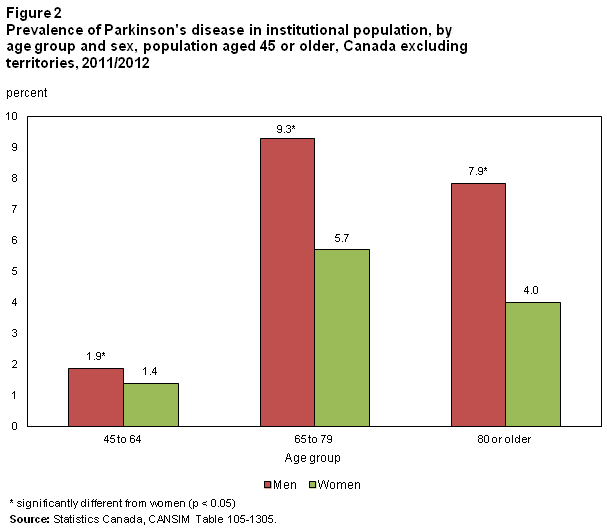
Prevalence Of Parkinsons Disease
An estimated 55,000 Canadians aged 18 or older living in private households reported that they had been diagnosed with Parkinsons disease. This represented 0.2% of the household population, unchanged from the 2000/2001 CCHS prevalence estimate.Note 6 As well, 12,500 residents of long-term residential care facilities4.9% reported a Parkinsons diagnosis. Among the household population, 79% with Parkinsons were 65 or older in institutions, almost everyone with the condition was 65 or older.
Overall, men were more likely than women to have Parkinsons disease: 0.3% versus 0.2% for those in private households, and 6.6% versus 4.0% for residents of institutions.
In general, the prevalence of Parkinsons disease increased with age, although in the institutionalized population, prevalence decreased in the oldest age group . This may reflect greater disease severity and higher mortality among older people in institutions compared with those in private households.Note 7 As well, being male and the presence of symptoms such as severe motor impairment, psychosis and dementia have been associated with earlier death among people with Parkinsons.Note 8
You May Like: How Does A Doctor Diagnose Parkinson’s Disease
Pd Is Different For Everyone
It is important to note that PD is different for everyone. Though it is a progressive disorder, not every case of PD progresses the same. Some may progress faster or slower than others.
Different people also experience different symptoms. One person may experience only tremor and stiffness. Another may have difficulty with balance, mood changes, and slowness of movement or gradual loss of spontaneous movement .4
It is difficult to predict how PD may affect someone and how symptoms may progress or change over time.4
If you have more questions about PD or would like to understand if you are at risk for developing PD, talk to your doctor.
Trends In Ylds Caused By Pd
In 2019, the number of YLDs caused by PD was 1210.09 × 103 globally, with an increase of 154.73% since 1990. The overall ASR of YLDs reported an increasing trend from 1990 to 2019, with the EAPC of 0.53 . Male patients had a higher burden, and undertook a larger increasing trend than female patients . Among the age groups, the highest YLD number was seen in the age group of over 80 years , and the percentage increased pronouncedly among the patients aged 45 years old .
Table 2. The changes in YLDs of Parkinson’s disease worldwide, and in sexes, SDI areas, and regions, 19902019.
The upward trend in the ASR of YLDs occurred in all SDI areas from 1990 to 2019, particularly the middle one . In terms of geographic regions, the largest number of YLDs was seen in East Asia , while the lowest one was in Oceania . The percentage of YLDs number increased from 27.97% in Eastern Europe to 256.90% in Central Latin America during 19902019. The ASR of YLDs ranged from 8.01/100,000 in Eastern SubSaharan Africa to 20.84/100,000 in East Asia. Increasing trends in the ASR of YLDs occurred in most regions, particularly East Asia . However, a minor decreasing trend was found in Oceania . The ASRs of YLDs were positively associated with SDI among the regions in 2019 .
Also Check: What Are The Early Stages Of Parkinson’s Disease
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinsons disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinsons. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinsons disease. Electrical impulses are introduced to the brain, which has the effect of normalising the brains electrical activity reducing the symptoms of Parkinsons disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
Having Parkinsons Is Not A Death Sentence
Parkinsons disease is not fatal, and your life expectancy depends highly on the type of Parkinson’s you have. If the type of disease isn’t causing issues with brain function, you can potentially live as long as people without the disease.
However, if someone has an atypical case of the condition that occurs at the same time as other conditions such as dementia, this can negatively affect their life expectancy.
Also Check: Which Is Worse Ms Or Parkinson’s
Other Studies Of Interest
Three high-quality papers were found but not included in the meta-analysis as they did not report age- and gender-specific incidence rates or proportions. These studies provided information on Asian and Eastern European populations that were not well represented in the meta-analysis.
Das et al. was the only study that examined PD in a south Asian Indian population, reporting average annual incidence rates for males and females in different age categories. AAIRs peaked earlier for males, than females. Male AAIRs peaked at 60-69 years female AAIRs continued to rise in 70-79 years before dropping off in the 80+ age group. Hristova et al. and Kyrozis et al. both provided incidence rates not stratified by gender and age and therefore could not be included in the meta-analysis. Both represented unique European populations and found peak incidence between 70 and 80 years.
