How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Depression May Be An Early Symptom Of Parkinsons
Depression is one of the most common, and most disabling, non-motor symptoms of Parkinsons disease. As many as 50 per cent of people with Parkinsons experience the symptoms of clinical depression at some stage of the disease. Some people experience depression up to a decade or more before experiencing any motor symptoms of Parkinsons.
Clinical depression and anxiety are underdiagnosed symptoms of Parkinsons. Researchers believe that depression and anxiety in Parkinsons disease may be due to chemical and physical changes in the area of the brain that affect mood as well as movement. These changes are caused by the disease itself.
Here are some suggestions to help identify depression in Parkinsons:
- Mention changes in mood to your physician if they do not ask you about these conditions.
- Complete our Geriatric Depression Scale-15 to record your feelings so you can discuss symptoms with your doctor. Download the answer key and compare your responses.
- delusions and impulse control disorders
New Techniques For Mri
In recent years, deep brain stimulation has become increasingly employed in carefully selected patients with medically intractable essential tremor and dystonia. Many patients are poor surgical candidates or averse to an invasive procedure or chronically implanted device. Moreover, fully awake microelectrode recordings can be difficult to virtually impossible in some subjects with severe generalized dystonia. Therefore, new tools and approaches are needed in neurologists’ and neurosurgeons’ armamentaria.
Gamma knife radiosurgery has been used to treat essential tremor for over 15 years. However, gamma knife radiosurgery has Level U recommendation from the American Academy of Neurology for essential tremor due to lack of randomized multicenter trials with long-term follow-up. The effects of gamma knife radiosurgery are often modest, and, even in experienced hands, can be associated with temporary or permanent neurologic side effects in over 5% of patients. Alternatives to gamma knife radiosurgery and deep brain stimulation for essential tremor such as magnetic resonanceguided focused ultrasound are in development. In comparison to gamma knife radiosurgery, ultrasound may create more discrete lesions and may be associated with a significantly lower risk of delayed sequelae.
You May Like: What Is The Life Expectancy For Someone With Parkinson Disease
Clinical History And Testing
Diagnostic tests can be used to establish some features of the condition and distinguish them from symptoms of other conditions. Diagnosis may include taking the person’s , a physical exam, assessment of neurological function, testing to rule out conditions that may cause similar symptoms, brain imaging, to assess cognitive function,, or myocardial scintigraphy. Laboratory testing can rule out other conditions that can cause similar symptoms, such as abnormal , , , or vitamin deficiencies that may cause symptoms similar to dementia.
Dementia screening tests are the and the . For tests of attention, , , and can be used for simple screening, and the Revised Digit Symbol Subtest of the may show defects in attention that are characteristic of DLB. The , and are used for evaluation of executive function, and there are many other screening instruments available.
If DLB is suspected when parkinsonism and dementia are the only presenting features, PET or SPECT imaging may show reduced dopamine transporter activity. A DLB diagnosis may be warranted if other conditions with reduced dopamine transporter uptake can be ruled out.
Since 2001, – has been used diagnostically in East Asia , but not in the United States. MIBG is taken up by nerve endings, such as those that innervate the heart, and is for scintigraphy with radioactive 123iodine. Autonomic dysfunction resulting from damage to nerves in the heart in patients with DLB is associated with lower cardiac uptake of 123I-MIBG.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Read Also: Is Parkinsons Disease Fatal
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Contact Our Information And Referral Helpline
The Parkinson Canada Information and Referral Helpline is a toll-free Canada-wide number for people living with Parkinsons, their caregivers and health care professionals. We provide free and confidential non-medical information and referral services. When you have questions or need assistance, our information and referral staff help connect you with resources and community programs and services that can help you. We provide help by phone or email, Monday to Friday, 9:00 a.m. 5:00 p.m. ET.
Don’t Miss: How Does Parkinson’s Progress
Research And Clinical Trials
OHSU scientists have long been at the forefront of research into Parkinsons disease. Over the years, we have played a role in every major development in Parkinsons care. Our work includes:
Clinical trials: The OHSU Brain Institute offers clinical trials for patients with varying stages of Parkinsons disease. We have research happening across many sites, so if you qualify, you may not need to travel to Portland to take part.
Parkinsons disease: We are conducting research on psychological and physical aspects of Parkinsons, including:
- How stress affects the progression of the disease.
- Ways to slow the breakdown of dopamine, a brain chemical that plays a central role in Parkinsons.
- The role of protein buildup, with the goal of developing and testing a new medication.
Balance Disorders Laboratory: Researchers in our Balance Disorders Laboratory are exploring the connection between motor signals and balance to develop rehabilitation approaches.
Improving deep brain stimulation devices: DBS uses open-loop devices, which deliver constant stimulation even if symptoms are absent. Were exploring a closed-loop device to provide stimulation only as needed.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Also Check: What Are The Four Cardinal Signs Of Parkinson’s Disease
May 19 201: Move4u 5k
The Parkinson’s and Movement Disorder Foundation and the National Spasmodic Torticollis Association held our 8th annual MOVE4U 5k Walk/Run Fundraiser at Mile Square Park at Group Shelter 17 in Fountain Valley, CA on May 19th supporting the mission of each organization in our fight against movement disorders. We had over 200 people attending our event, successfully raising over $30,000!
Congratulations to our top 3 runners with 1st place being 2 Roundtrip Southwest E-tickets, 2nd place being 4 Knott’s Berry Farm tickets, and 3rd place being 2 Six Flags Magic Mountain tickets. Participants of the fundraiser who attended were also eligible to win one of our raffle prizes, ranging in gift cards from Amazon, Target, Starbucks, Katella Deli, Origin Massage & Bodyworks, Emerald Isle Golf Course, and Masana Portrait Artwork NYC.
Sidebar: Morris K Udall Centers Of Excellence For Parkinson’s Disease Research
The Morris K. Udall Parkinsons Disease Research Act of 1997 authorized the NIH to greatly accelerate and expand PD research efforts by launching the NINDS Udall Centers of Excellence, a network of research centers that provide a collaborative, interdisciplinary framework for PD research. Udall Center investigators, along with many other researchers funded by the NIH, have made substantial progress in understanding PD, including identifying disease-associated genes investigating the neurobiological mechanisms that contribute to PD, developing and improving PD research models, and discovering and testing potential therapeutic targets for developing novel treatment strategies.
The Udall Centers continue to conduct critical basic, translational, and clinical research on PD including: 1) identifying and characterizing candidate and disease-associated genes, 2) examining neurobiological mechanisms underlying the disease, and 3) developing and testing potential therapies. As part of the program, Udall Center investigators work with local communities of patients and caregivers to identify the challenges of living with PD and to translate scientific discoveries into patient care. The Centers also train the next generation of physicians and scientists who will advance our knowledge of and treatments for PD. See the full list of Udall Centers.
Recommended Reading: What Are Neurological Soft Signs
What Is Parkinsons Disease
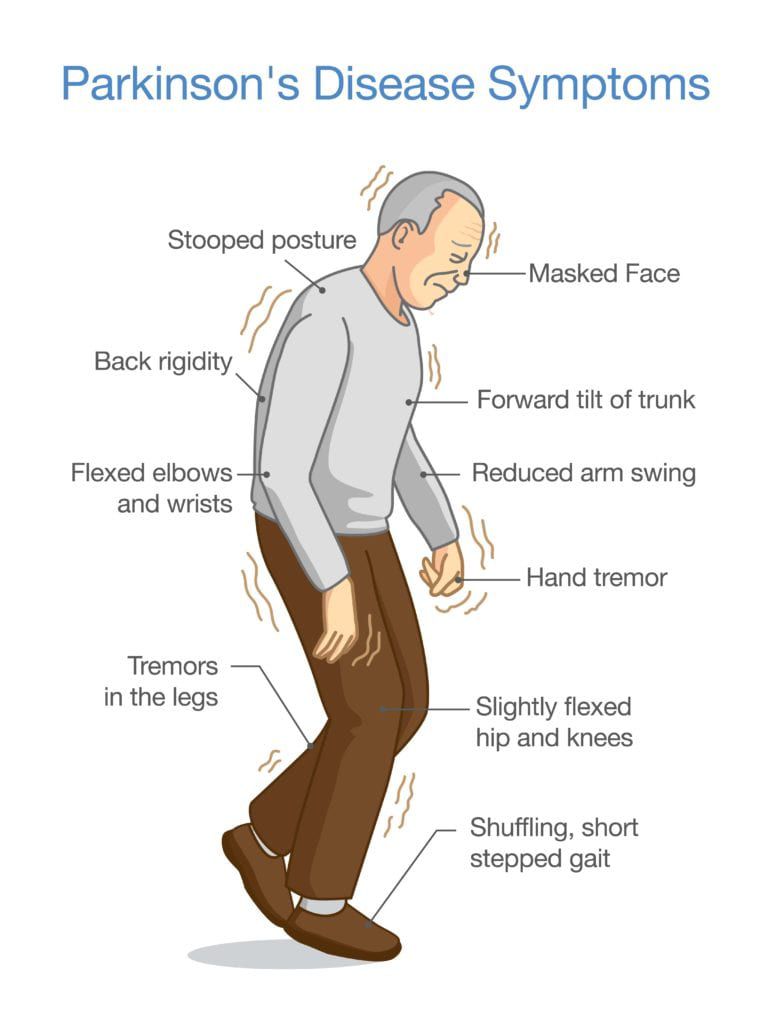
Parkinsons disease is a nervous system disease that affects your ability to control movement. The disease usually starts out slowly and worsens over time. If you have Parkinsons disease, you may shake, have muscle stiffness, and have trouble walking and maintaining your balance and coordination. As the disease worsens, you may have trouble talking, sleeping, have mental and memory problems, experience behavioral changes and have other symptoms.
Range Of Personalized Movement Disorder Treatment Options
At UH, we work closely with you to identify your quality-of-life goals and then partner with our colleagues throughout the UH system to provide treatment options that address both your specific condition and your unique goals. These may include medication therapies, surgery, physical and occupational therapy or other treatments.
Through a continuous focus on research and discovery, our movement disorder specialists keep up-to-date on evolving movement disorder therapies as new medications and treatments are tested and approved. One increasingly promising treatment for Parkinsons disease is deep brain stimulation. For patients, this specialized treatment can dramatically improve independence and quality of life.
Mike DeRubertis, who was diagnosed with tremor predominant Parkinson’s disease in 2008, had deep brain stimulation at UH Cleveland Medical Center and got his life back.
Don’t Miss: Mortality Rate Of Parkinson’s Disease
Our Team And Clinic Vision
The Cole Center employs a multidisciplinary team to treat the complex issues associated with Parkinsons disease and other movement disorders. Our team is comprised of three neurologists fellowship trained in movement disorders, an advanced registered nurse practitioner with more than a decade experience in movement disorders, a registered nurse and a social worker.
We also have physical therapists at our clinic several times each month to help with complicated cases, and refer actively to ancillary care such as physical therapy, speech therapy and occupational therapy. Our movement disorder specialists are experts in the diagnosis and treatment of Parkinsons disease, essential tremor, dystonia, chorea and a variety of other movement disorders. The Cole Center is further considered a Huntingtons Center of Excellence as an associate site of Vanderbilts Level I HDSA Huntingtons Center of Excellence given our medical expertise and patient services.
Our comprehensive team strives to incorporate patients into the treatment process. We provide the patient and family with educational materials of clinical issues and treatment recommendations. The team works with the patient and family to help them understand the situation and encourages them to participate in the development of a management plan.
Helping You Understand Your Movement Disorder
Managing movement disorders can be challenging since your capabilities are always changing. Tasks you could do recently without issuelike swallowing or walkingmay gradually cause issues or difficulties. At UH, we work hard to make sure you understand what to expect from your disease. Our annual Parkinsons Disease Boot Camp, you and your loved ones will learn exercise techniques, mind and body wellness practices, and invigorating skills to manage Parkinsons.
As your condition progresses, our movement disorder neurologists will support you along the way and modify treatment as necessary.
Parkinsons patients need more guidance from their neurological team if hospitalized for another reason since their disease and treatment therapies are often complex and our neurology team is ready to assist. At UH, we have processes in place to make sure our Parkinsons patients get very focused attention from a multidisciplinary team while in the hospital to make sure your care and outcomes are optimal. Visit our patient resources page to learn more about support programs for managing your Parkinsons disease.
Read Also: What Are Early Warning Signs Of Parkinson’s Disease
People With Parkinson’s Guiding Research And Moving Towards A Cure
Parkinsons Movement is an initiative of The Cure Parkinsons Trust . Created people with Parkinsons for people with Parkinsons, we aim to inform and encourage all to get involved in any way they wish to. From clinical trials, TV appearances, or just completing one of our surveys, you can provide invaluable insights to those working on a cure. Click on the boxes below to read about, participate in or contribute toParkinsons research:
Principal Medical Conditions Treated At The Cole Center
- Parkinsons disease
- Parkinsonism/atypical parkinsons/parkinsons plus
- Multiple System Atrophy
- Dementia with Lewy Bodies
- Drug-Induced parkinsonism
- Tardive Dyskinesia and drug-induced Movement Disorders
- Involuntary Movements/Movement Disorder Not Otherwise Specified
- Tremor
- Myoclonus
- Dystonia
- Hemifacial spasm
- Ataxia
- Friedreichs ataxia
- Gait Impairment
- Normal Pressure Hydrocephalus
- Clinical trials
Recommended Reading: Parkinson’s And Alzheimer’s Life Expectancy
Managing Depression In Parkinsons Disease
People with Parkinsons, family members and caregivers may not always recognize the signs of depression and anxiety. If you are experiencing depression as a symptom of Parkinsons, it is important to know it can be treated.
Here are some suggestions:
- For information and support on living well with Parkinsons disease, contact our Information and Referral line.
- As much as possible, remain socially engaged and physically active. Resist the urge to isolate yourself.
- You may want to consult a psychologist and there are medications that help relieve depression in people with Parkinsons, including nortriptyline and citalopram .
Sidebar: Ninds Steps Up Pursuit Of Pd Biomarkers
In 2012, the NINDS dramatically accelerated efforts to identify biomarkers by establishing the Parkinsons Disease Biomarkers Program . This unprecedented program unites a range of stakeholders from basic and clinical researchers to healthcare professionals, the NINDS staff, information technology experts, and people living with PD and their families.
PDBP supports research and builds resources aimed at accelerating the discovery of biomarkers to ultimately slow the progression of PD. For example, the program has established a repository of biological specimens and a Data Management Resource system maintained by the NIH Center for Information Technology. The DMR allows researchers to access clinical, imaging, genetic, and biologic data, while a complementary PDBP-supported project develops statistical tools to analyze vast quantities of data so that patterns can be identified across these diverse sources of information.
Don’t Miss: Parkinson Disease Dementia Mortality
