Cause Signs And Symptoms Treatment And Management Age Of Onset Of Parkinsons And Huntingtons Disease:
Cause:
Parkinson’s Disease: PD is caused by the degeneration of the neurons in Substantia nigra of the midbrain.
Huntington’s Disease: HD is caused by the mutations in the HTT gene.
Age of Onset:
Parkinson’s Disease: PD usually occurs after the age of 50.
Huntington’s Disease: HD usually occurs in the thirties or forties.
Symptoms:
Parkinson’s Disease: PD causes tremors, rigidity, slowing of movements and gait disturbances.
Huntington’s Disease: HD causes higher function abnormalities such as problems in thinking and reasoning together with characteristic chorea.
Treatment:
Parkinson’s Disease: PD is treated with dopamine-enhancing drugs such as levodopa, dopamine agonists, etc.
Huntington’s Disease: HD has no curative treatment and main the treatment is supportive.
Life expediency:
Parkinson’s Disease: PD doesn’t have an effect on life expectancy. However, it reduces the quality of life.
Huntington’s Disease: HD patients live 15-20 years after the appearance of the first symptom.
Multiple Sclerosis Vs Parkinsons Disease Differences In Symptoms Causes And Treatment
Multiple sclerosis is an autoimmune condition that affects the nervous system, while Parkinson’s disease is a progressive neurological disorder affecting movement. Symptoms of multiple sclerosis and Parkinson’s disease are quite similar at times, but there are distinct differences setting the two conditions apart.
Causes of multiple sclerosis and Parkinson’s disease are not well known, although there is some speculation to their roots. We will outline those speculated causes and highlight the symptoms, risk factors, complications, treatment, and therapies for both multiple sclerosis and Parkinson’s disease to raise your awareness on each disorder.
Benefits Of Aquatic Therapy For Alzheimers Patients In Senior Living Facilities
Stay active
Many physicians believe that the key to longevity with Alzheimer’s is activity. Thus, if a patient with Alzheimer’s can enjoy working out in a therapy pool, whether with a clinician or as part of a larger class, that patient has a better chance of remaining in good health for as long as possible. Even if he or she fears falling when walking on land , that fear is highly negated by the natural buoyancy of the water.
Become accustomed to a routine
Alzheimer’s patients who have a scheduled plan for pool therapy and/or exercise may become accustomed to the routine. This, in turn, can be a boost to their mental abilities. Routine for Alzheimer’s patients may even promote slower memory loss, although this is debatable. If nothing else, it provides them with a very positive outlet.
Psychological Effect
The therapy pool has a psychological effect on those with Alzheimer’s by the warmth of the water. Not only is it soothing to the body, but it can be soothing to the mind. Many Alzheimer’s patients live with a high degree of uncertainty and stress because they know something is wrong, but aren’t sure what that is. If pool therapy can alleviate those tensions, the patients will be under far less emotional turmoil throughout the day.
Request a Free Info Kit View Our Products Find a Pool Near You
Multiple Sclerosis Vs Parkinsons Disease: Us Prevalence And Economic Impact
Anyone can develop multiple sclerosis, but it mostly affects 20- to 40-year-olds. Prevalence of multiple sclerosis in the U.S. is estimated at over 400,000 cases, and nearly 200 new cases are diagnosed each week. Rates of multiple sclerosis are highest in areas furthest away from the equator, so the rates are higher in the Northern U.S.
Direct and indirect costs resulting from multiple sclerosis can range from $8,528 to $54,244.
One million Americans live with Parkinson’s disease. The average cost of Parkinson’s disease including treatment, lost work wages, and social security payments is $25 billion annually in the U.S.
Multiple Sclerosis Vs Parkinsons Disease: Risk Factors And Complications
Risk factors for multiple sclerosis include being female, having a family history of multiple sclerosis, having certain infections, being white of European descent, living furthest from the equator, living in temperate climate regions, already having an autoimmune disease, and smoking.
Complications resulting from multiple sclerosis include muscle stiffness and spasms, paralysis, problems with bladder, bowel, and sexual function, as well as forgetfulness, mood changes, depression, and epilepsy.
Risk factors for Parkinson’s disease include being over the age of 50, being male, having a family history of Parkinson’s disease, carrying gene variations, experiencing a head injury, being exposed to environmental toxins, and taking certain medications such as anti-anxiety medications or sleeping pills.
Complications associated with Parkinson’s disease include difficulty thinking, depression, emotional changes, swallowing problems, sleep problems and disorders, bladder issues, constipation, changes in blood pressure, smell dysfunction, fatigue, pain, and sexual dysfunction.
Parkinson’s Disease And Multiple Sclerosis: Conditions And Differences
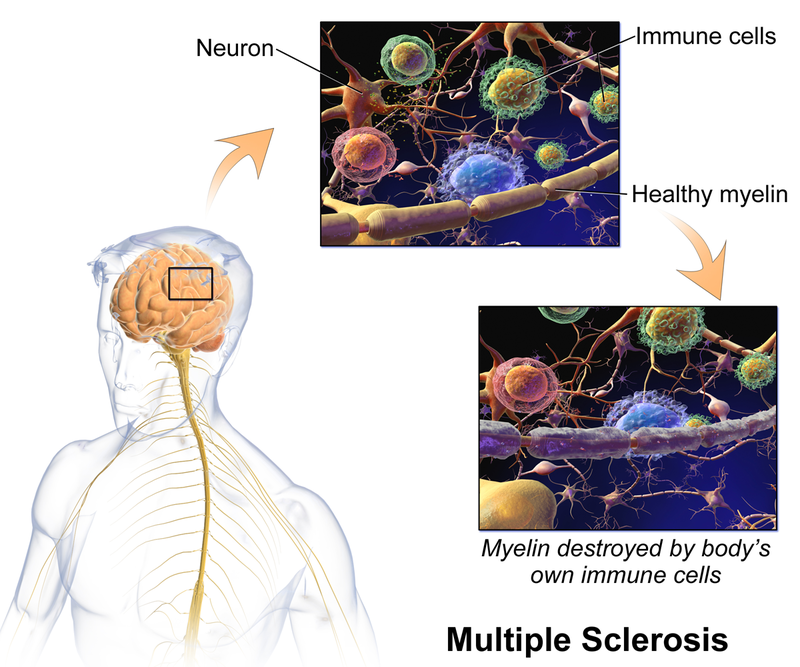
It’s important to note that, while both Parkinson’s and multiple sclerosis are diseases of the CNS, they don’t originate in the same way. MS is an autoimmune disease, brought on by the immune system attacking myelin, the protective coating over the nerves in the CNS that also speeds up signals. This affects mainly the brain and spinal cord, though it can also affect the optic nerve as well. In Parkinson’s disease, the neurons in the brain die off without any known attack, with the lack of dopamine they produce leading to the onset of the disease. This doesn’t affect nerves in the spinal cord.
Other notable differences include:
Know The Difference Between Parkinson’s Disease And Multiple Sclerosis
Multiple Sclerosis and Parkinson’s Disease are two medical conditions, which are often mistaken for each other, as both are progressive and have similar symptoms. And although patients can have both conditions simultaneously, there are a few striking differences between the two.
Check out this quick guide about the similarities and differences between the two conditions to help patients avail the best Parkinson’s Disease and Multiple Sclerosis treatment on time.
Understanding Parkinson’s Disease and Multiple Sclerosis
Parkinson’s Disease is one of the most common neurodegenerative conditions in the world. It primarily damages the dopamine-producing neurons in a specific area of the brain called substantia nigra.
Multiple Sclerosis is a chronic inflammatory condition of the central nervous system. It is an autoimmune demyelinating disease, which means the immune system mistakenly attacks normal tissues — in this case, the myelin or protective covering around nerve fibers. This leaves scarred tissues or lesions in multiple areas, disrupting electrical impulses throughout the body. When the myelin sheath is damaged, nerve impulses slow or even stop, causing neurological problems.
Similarities between the two conditions
Both Multiple Sclerosis and Parkinson’s Disease affect the brain and the central nervous system, which leads to changes in the way you move, talk, and interact with the world. The two conditions have several common symptoms, including
What Natural Interventions May Be Beneficial For Restless Leg Syndrome
- Iron. Iron deficiency or altered brain iron metabolism have been linked to RLS; supplementation is often recommended for RLS patients who have been tested and shown to be deficient. Iron supplementation has been shown to significantly improve symptoms in iron-deficient RLS patients.
- Folate. Low levels of folate may play a role in RLS, especially in pregnant women. Pregnant women with lower folate levels were more likely to develop RLS than women who took vitamins during pregnancy.
- Magnesium. Low magnesium levels can cause excitability of neurons; magnesium supplements are often used to prevent abnormal activity in the nervous system. A case study indicated magnesium may improve symptoms and sleep problems associated with RLS.
- Diosmin. Diosmin is a natural flavone derivative often used for supporting venous function. Since venous disorders have been linked with RLS, diosmin is a promising possible treatment.
- Green coffee extract. Diabetes and pre-diabetes are known risk factors for RLS. Green coffee extract may help maintain healthy glucose levels.
- Valerian root. Valerian, an herbal sedative, is often used as a sleep aid. In a clinical trial, supplementation with valerian resulted in improvements in RLS symptoms and less daytime sleepiness.
- Other natural interventions that may help relieve RLS symptoms include D-ribose and vitaminsC and E.
Is There A Link Between Restless Leg Syndrome And Parkinson’s Disease
Parkinsons & Restless Leg Syndrome: Using Dopaminergic Medication
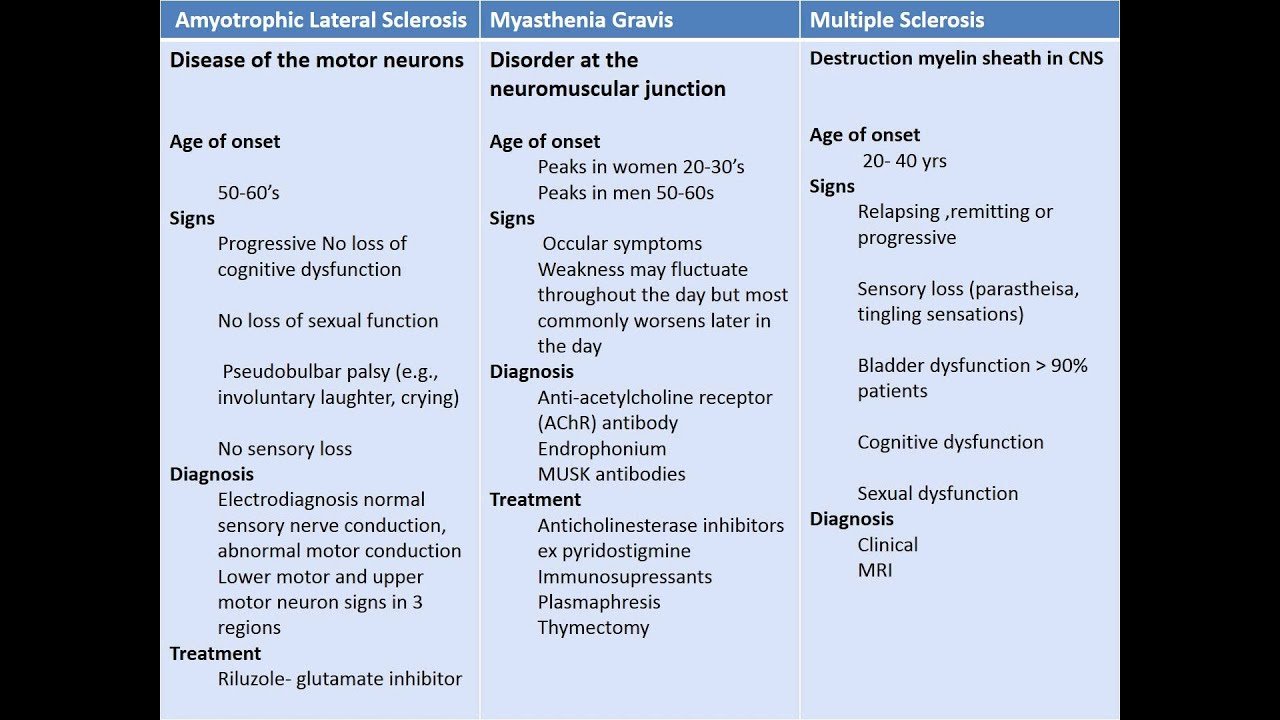
Myasthenia Gravis And Multiple Sclerosis: Differences And Similarities

Nervous System Disorders and Diseases
Multiple sclerosis presents patients with a number of symptoms that can disrupt everyday life. During an episode for those with relapsing-remitting MS, or those with one of the progressive MS forms with constant symptoms, obtaining a diagnosis that allows the patient to work with doctors and therapists to create a treatment and management regimen is crucial to living a full and healthy life.
Of course, MS is not the only chronic disease that causes such issues or requires direct attention. Another condition, called Myasthenia gravis, can also cause significant impairment when trying to complete daily activities. In fact, Myasthenia gravis actually seems quite similar to some aspects of multiple sclerosis and distinguishing one from the other is essential to prescribing the right treatment plan.
Myasthenia Gravis And Multiple Sclerosis: Conditions And Differences
One of the biggest differences between multiple sclerosis and Myasthenia gravis is that the latter is far less common than MS. While multiple sclerosis is believed to affect about one in four hundred people, Myasthenia gravis is estimated to develop in only about one in five thousand. Other differences include:
In addition, while both diseases involve weakness in the limbs, this is typically one of the first signs of multiple sclerosis. In Myasthenia gravis, it usually only follows weakness in the neck, facial muscles, and eyes.
Differentiating Multiple Sclerosis Symptoms With Parkinsons Disease
Signs and symptoms of multiple sclerosis include numbness or weakness in one or more limbs, partial or complete vision loss, prolonged double vision, tingling or pain, electric-shock sensations, tremors and lack of coordination, fatigue, dizziness, slurred speech, and problems with bowel and bladder function.
Parkinson’s disease symptoms typically begin with tremors followed by muscle stiffness, difficulty standing or walking, changes in speech, slow movements, impaired posture and balance, loss of automatic movements, and writing changes.
As you can see, Parkinson’s disease and multiple sclerosis do have some symptoms in common, which can make early diagnosis difficult.
The First Sign Of Parkinson’s And Multiple Sclerosis: A Dodgy Tummy
- Study suggests that brain disease can be caused by an unhealthy gut
- ‘Butterflies in the stomach’ could be linked to Parkinson’s and MS
17:07 EDT, 21 June 2014 | Updated:
Gut feeling: Brain disease can be caused by an unhealthy stomach
Anxiety or anticipation can often lead to a feeling of ‘butterflies in the stomach’ – which usually dissipates along with the source of the consternation.
But scientists have discovered that the nerve pathways between the gut and the brain that cause this phenomenon may also be linked to degenerative illnesses such as Parkinson’s disease and multiple sclerosis , as well as some mental health problems.
Dr Anton Emmanuel, consultant neuro-gastroenterologist at University College London and the National Hospital for Neurology, explained: ‘The gut and brain share the same nerve chemistry and have a dialogue.
‘That’s why when you feel stress and other strong emotions, such as fear, it leads to gastrointestinal symptoms, like rushing to the loo.’
A new study suggests that brain disease can be caused by an unhealthy gut because these signals also travel in the opposite direction.
The study, which was published in the journal Movement Disorders, found that sufferers of Parkinson’s disease had a higher prevalence of a condition called small intestinal bacterial overgrowth, or SIBO.
In SIBO, normally harmless bacteria proliferate in large numbers in the small intestine.
Myasthenia Gravis And Multiple Sclerosis: Symptoms And Similarities
As a condition of the nervous system, there are obviously going to be similarities in the presentation of Myasthenia gravis and multiple sclerosis. Some of these include:
- Both diseases are chronicautoimmune diseases that lead to improper or lack of communication between the brain and muscles, which makes mobility more difficult.
- Both conditions cause weakness in the limbs, as well as potential issues with vision .
- Though the reason behind the deficiency is different, either disease can lead to problems speaking, chewing, and swallowing .
- Both diseases are most common in adult women under the age of forty.
- Having another autoimmune disease, such as rheumatoid arthritis or type 1 diabetes, puts a person at greater risk for developing either disease.
- Both diseases may “come and go”, with relief from symptoms over a period of time before they return.
- A relapse or episode in either disease can be triggered by factors such as stress, fatigue, illness or injury, and certain medications .
- Neither disease has a cure, but both can be treated to reduce relapses and symptoms. Some common treatments for both include immunosuppressants, corticosteroids, and DMTs like treatment with monoclonal antibodies.
Multiple Sclerosis Vs Parkinsons Disease: Treatment And Therapies
Treatment for multiple sclerosis is lifelong, and although it cannot cure the condition, it aims to minimize symptoms and allow the patients to live as normal of a life as possible. Some treatment methods include corticosteroids and plasma exchange, beta interferons, Glatiramer acetate, Dimethyl fumarate, Fingolimod, Teriflunomide, Natalizumab, Alemtuzumab, and Mitoxantrone, which all help to reduce the likelihood of relapses.
Other treatment methods include physical therapy to improve mobility, muscle relaxants, medications to reduce fatigue, and other medications like antidepressants, medications to control the bowels and bladder, and medications to improve sexual function.
Exercise, meditation, yoga, and acupuncture are also recommended as a means to reduce stress and improve overall mental and physical well-being.
There is no cure for Parkinson’s disease as well, but treatments are available to manage the symptoms and slow down the disease progression as much as possible. Alongside traditional treatments, supportive therapies are also used to improve different aspects of a person’s health.
Common medications prescribed in Parkinson’s disease include dopamine replacement therapy, dopamine agonists, anticholinergics, amantadine, monomine oxidase type B inhibitors, and catechol-o-methyl transferase inhibitors.
You can work closely with your doctor to create a specific treatment plan for you.
Restless Legs Syndrome: Detection And Management In Primary Care
NATIONAL HEART, LUNG, AND BLOOD INSTITUTE WORKING GROUP ON RESTLESS LEGS SYNDROME, National Institutes of Health, Bethesda, Maryland
Am Fam Physician. 2000 Jul 1;62:108-114.
Restless legs syndrome is a neurologic movement disorder that is often associated with a sleep complaint. Patients with RLS have an irresistible urge to move their legs, which is usually due to disagreeable sensations that are worse during periods of inactivity and often interfere with sleep. It is estimated that between 2 and 15 percent of the population may experience symptoms of RLS. Primary RLS likely has a genetic origin. Secondary causes of RLS include iron deficiency, neurologic lesions, pregnancy and uremia. RLS also may occur secondarily to the use of certain medications. The diagnosis of RLS is based primarily on the patient’s history. A list of questions that may be used as a basis to assess the likelihood of RLS is included in this article. Pharmacologic treatment of RLS includes dopaminergic agents, opioids, benzodiazepines and anticonvulsants. The primary care physician plays a central role in the diagnosis and management of RLS.
Chronic Dopaminergic Therapy Can Cause Augmentation Of Symptoms
Refer patients experiencing augmentation to a specialist. Most cases can be reversed with a change in dosing frequency, by lowering the dose, by switching drugs or by stopping dopaminergic therapy.3
Can Restless Legs Syndrome Develop Into Something More Serious
What Is The Pooled Prevalence Of Rls/wed And Its Mimics In Pd
In view of these contrasting results, what is the overall prevalence of the sum of true, secondary and mimics of RLS/WED in PD? A recently-published meta-analysis4343. Yang X, Liu B, Shen H, Li S, Zhao Q, An R et al. Prevalence of restless legs syndrome in Parkinson’s disease: a systematic review and metaanalysis of observational studies. Sleep Med. 2018 Mar;43:40-6. https://doi.org/10.1016/j.sleep.2017.11.1146https://doi.org/10.1016/j.sleep.2017.11…. tried to answer this question comparing 28 clinical studies. The pooled prevalence among diverse populations was 14%, being higher among those who had previously received dopaminergic treatment than among drug-naïve patients . Differences were also marginal for gender prevalence, favoring women . In their discussion, the authors were careful enough to acknowledge the intrinsic limitations of these studies, including a variety of biases.
Pramipexole Is Not Recommended In Pregnancy Or Breastfeeding
There is a lack of clinical data in pregnancy, along with evidence that pramipexole impairs implantation and disrupts early pregnancy in rats .6 Pramipexole is expected to inhibit lactation because of its effects on prolactin. It may be excreted into breast milk and should not be used during breastfeeding.6
Pathological Evidence Of Dopamine Dysfunction In Pd And Rls
Pramipexole May Be Useful For Severe Restless Legs Syndrome
Treatment Of Depression In The Setting Of Parkinsons Disease
The evidence base for the treatment of depression in PD is extremely slim. A recent Cochrane library review of treatments for depression in PD reported three randomised controlled trials fulfilling the criteria for inclusion.1 These trials included a total of 106 patients and indicated that nortryptilline was superior to placebo but that citalopram was not. The review concluded that there were “insufficient data on the effectiveness and safety of any antidepressant therapy in Parkinson’s disease”. There is an urgent need for larger scale clinical trials in this area.
Nevertheless, depression is common in PD and decisions have to be made about treatment. The last 10 years have seen a shift in prescribing practice away from tricyclic antidepressants and towards selective serotonin reuptake inhibitors as a first line treatment of depression in PD. The main reason for this is the more favourable side effect profile of SSRIs.
Tricyclic antidepressants
Selective serotonin reuptake inhibitors
Withdrawal syndromes can occur in people who stop SSRIs suddenly and can include flu-like symptoms, insomnia, nausea, imbalance, sensory disturbance, and hyperarousal . Therefore SSRIs should be reduced slowly.
?SSRI withdrawal symptoms
Other treatments for depression
Comparing Multiple Sclerosis And Parkinsons Disease Causes
Multiple sclerosis is an autoimmune disease in which the immune system attacks the myelin, causing damage and thus exposing nerve fibers. Like many autoimmune diseases, the exact cause is unknown, but environmental, immunologic, infectious, and genetic factors have all been found to play a role in the onset of multiple sclerosis.
When certain nerve cells in the brain begin to die or break down that is what causes Parkinson’s disease, but why this occurs is unclear. Some factors that contribute to nerve cell death include genetics as specific gene mutations have been identified to contribute to Parkinson’s disease, environmental factors such as exposure to certain toxins, the presence of Lewy bodies in the brain as well as alpha-synuclein found in Lewy bodies.
Restless Legs Syndrome And Periodic Limb Movement Disorder
Most people who have RLS also have a condition called periodic limb movement disorder . PLMD involves repetitive flexing or twitching of the limbs while asleep at night. It is different from RLS in that these movements are not accompanied by uncomfortable sensations and because they occur during sleep, patients are often not aware of them. However, PLMD-associated movements can cause a person to wake up and therefore can compound sleep issues in patients who also have RLS.
Although most people with RLS have PLMD, many with PLMD do not have RLS.
Your Dreams Could Be An Early Clue To Parkinson’s Disease
Breaking down Parkinson’s disease05:25
Actor Alan Alda revealed that he has Parkinson’s disease — and in an interview Tuesday on “CBS This Morning,” the award-winning actor said an unusual dream helped lead to his diagnosis.
Alda, best known for his portrayal of Army Capt. “Hawkeye” Pierce in the TV series “M*A*S*H, was diagnosed three and a half years ago after experiencing a lesser-known early sign of Parkinson’s. He said he asked his doctor to test him for the disease after reading an article about how physically acting out your dreams can be one of the earliest precursors of the neurological disorder.
“By acting out your dreams, I mean I was having a dream where someone was attacking me and I threw a sack of potatoes at them, and what I was really doing was throwing a pillow at my wife,” Alda explained.
Restless Legs Syndrome: A Common Underdiagnosed Disorder
US Pharm.
Scales Used To Measure Depression In Parkinsons Disease
As mentioned above, symptoms of idiopathic PD have considerable overlap with those of depression. This means that standard rating scales for depression may not be valid in this situation. Rating scales for depression may be loaded with “somatic” or “vegetative” symptoms, which reduce their validity.
Three rating scales have been tested using a clinical interview with operationalised diagnosis as a gold standard. Using receiver operating curves, the sensitivity and specificity at a given “cut off” point can be calculated. From this methodology, it is clear that the Beck depression inventory is not a useful rating scale in PD. The Montgomery and Asberg depression rating scale and the Hamilton depression scale have performed better. In summary, diagnosis of depression should be made clinically, using appropriate diagnostic criteria, with severity or response to treatment being measured using MADRS or HAM-D.
Restless Leg Syndrome And Multiple Sclerosis Connection

Cases of restless leg syndrome in multiple sclerosis patients greatly vary from 13.3 percent to 65.1 percent. These numbers are still larger than rates of restless leg syndrome in the general population. Multiple sclerosis patients with RLS rate higher on the Expanded Disability Status Scale compared to MS patients without RLS. RLS can negatively impact a person’s sleep and cause further complications such as worsened fatigue and greater inflammation, which can contribute to pain. Further research will be conducted to better understand the connection between RLS and MS and provide more effective treatment.
Other Conditions Associated With Restless Legs Syndrome
The following medical conditions are also associated with RLS, although the relationships are not clear. In some cases, these conditions may contribute to RLS. Others may have a common cause, or they may coexist due to other risk factors:
The Link Between Rls And Parkinsons: Dopamine Agonists
Lastly, RLS does not progress to cause other major symptoms such as tremor, gait disorder, or loss of taste or smell, and does not progress to PD. In fact, one of the leading possibilities as the cause of RLS and for which there is good scientific evidence and much research is a form of iron-transport abnormality in the brain. In effect, RLS patients may have low levels of iron in brain nerve cells—just the opposite of some portions of the brain in PD.
Is Restless Leg Syndrome A Precursor To Other Ailments
Parkinsons And Multiple Sclerosis Case Study: Virginia
One recent case illustrating the power of water to combat problems related to major conditions involves a 67-year-old patient diagnosed with both Multiple Sclerosis and Parkinson’s who sought treatment at a senior living campus. The woman, Virginia, has been wheelchair bound due to her illnesses, but was particularly concerned because her body had begun to lean to the left to the point where she could not easily read the newspaper, play the piano or easily put on her slacks.
Virginia was determined not to allow her conditions to stop her from having a good quality of life. Therefore, she turned to water therapy twice a week. When she began her rehabilitation, it was very difficult for her to bear any weight until she was significantly submerged and the buoyancy could prevent her from falling. After three months, she improved her core strength to the point where she could sit and stand upright, and could exercise in water depths that were lower than before.
As Virginia’s physical therapist now notes, she has improved to the point where she can stand against currents created by resistance jets. Additionally, her posture is much better. Most exciting of all from Virginia’s perspective was when she had a check-up with her neurologist who was amazed at the results. Now, Virginia plays the piano for up to 45 minutes at a time without leaning to the left, and can feel the positive effects of being stronger and more stable.
Link Between Multiple Sclerosis Vs Parkinsons Disease
Researchers have found that nerve pathways in the gut and the brain may be linked to multiple sclerosis and Parkinson’s disease. Dr. Anton Emmanuel explained, “The gut and brain share the same nerve chemistry and have a dialogue. That’s why when you feel stress and other strong emotions, such as fear, it leads to gastrointestinal symptoms, like rushing to the .”
The study suggests that an unhealthy gut can trigger the onset of brain disease as the signals from brain to gut can also travel in the opposite direction – from gut to brain. The findings of the study were published in the journal Movement Disorders where researchers found that Parkinson’s disease sufferers have a higher prevalence of small intestinal bacterial overgrowth .
The researchers suggest the bacteria produce toxic chemicals affecting the nerves in the gut and this way causing damage to the brain. This can bring about the onset of multiple sclerosis or Parkinson’s disease.
Dr. Emmanuel said, “We now think that neurological diseases such as MS and Parkinson’s are linked to the gut being more leaky, permitting pathogens into the bloodstream and causing an antibody response. Either the pathogens, directly, or the immune response, indirectly, may damage nerve tissue.”
Researchers are now exploring bacterial genomes that can help identify the bacteria so that doctors can specifically treat it as a means of preventing Parkinson’s disease and multiple sclerosis.
How Effective Is Early Treatment Of Ms And Parkinsons
Though not a cure, nipping neurologic disorders in the bud may help slow their progression. But proper diagnosis is necessary—and that’s not easy.
Arlie Barber knew something was wrong when, in the spring of 2008, she found herself running to the bathroom all the time. Her gynecologist diagnosed her with overactive bladder. But Barber, then 35, was an avid runner who had never had children. The diagnosis didn’t seem to fit.
ILLUSTRATION BY BRIAN STAUFFER
A few months later, she woke up with half her face numb. Her doctor blamed it on the Botox injection Barber had received a few days earlier, but the numbness spread over the next few weeks to her hands and feet. Along with balance problems and a sense of just not “feeling right,” Barber knew something was amiss. But it wasn’t until she described her symptoms to a second doctor in October 2008 that she started to get answers that made sense. “When a woman your age describes symptoms like these,” the doctor told her, “the medical community thinks multiple sclerosis .”
Given Barber’s symptoms and lesions, the doctor strongly suspected Barber would eventually be diagnosed with MS, so he offered to start her on treatment. But many of the drugs used to treat the condition require injections and can have significant side effects. “He told me that it was really serious stuff and to be really sure that’s what I wanted to do,” she says.
Early Treatment in Multiple Sclerosis
Early Treatment for Parkinson’s Disease
Drugs And Medication Used To Treat Parkinsons Disease

A number of different drugs can be used to treat Parkinson’s.
Levodopa
Levodopa is the most common treatment for Parkinson’s. It helps to replenish dopamine.
About 75 percent of cases respond to levodopa, but not all symptoms are improved. Levodopa is generally given with carbidopa.
Carbidopa delays the breakdown of levodopa which in turn increases the availability of levodopa at the blood-brain barrier.
Dopamine agonists
Dopamine agonists can imitate the action of dopamine in the brain. They’re less effective than levodopa, but they can be useful as bridge medications when levodopa is less effective.
Drugs in this class include bromocriptine, pramipexole, and ropinirole.
Anticholinergics
Anticholinergics are used to block the parasympathetic nervous system. They can help with rigidity.
Benztropine and trihexyphenidyl are anticholinergics used to treat Parkinson’s.
Amantadine
Amantadine can be used along with carbidopa-levodopa. It’s a glutamate-blocking drug . It offers short-term relief for the involuntary movements that can be a side effect of levodopa.
COMT inhibitors
Catechol O-methyltransferase inhibitors prolong the effect of levodopa. Entacapone and tolcapone are examples of COMT inhibitors.
Tolcapone can cause liver damage. It’s usually saved for people who do not respond to other therapies.
Ectacapone does not cause liver damage.
Stalevo is a drug that combines ectacapone and carbidopa-levodopa in one pill.
MAO-B inhibitors
Restless Leg Syndrome As A Symptom For Other Diseases
Aside from multiple sclerosis, restless leg syndrome can be a symptom of other diseases as well. A recent study revealed that restless leg syndrome can be a symptom of heart problems, kidney problems and stroke.
For the study 3,700 veterans with RLS were observed along with 3,700 healthy participants as controls. Both groups were followed for eight years. Researchers were specifically looking for outcomes of stroke and heart and kidney problems.
Related Reading:
Restless leg syndrome is symptom for stroke, heart and kidney disease: Study
Restless leg syndrome has been found to increase the risk of stroke, heart disease and kidney disease. Restless leg syndrome is a condition that causes a person to feel an overwhelming urge to move their legs when in an inclined position . Tingling, aching and itching sensations may occur as well. Continue reading…
New research from the University of Vermont suggests that in mice models, salt intake may increase the risk of developing multiple sclerosis . With the use of three genetically different groups of mice, researchers conducted their study. Continue reading…
Key Difference Parkinsons Vs Huntingtons Disease
The key difference between Parkinson’s and Huntington’s disease is that Parkinson disease is a disorder with rigidity, tremors, slowing of movements, postural instability and gait disturbances usually occurring in old age due to degeneration of the substantia nigra of the midbrain while Huntington’s disease is a familial neurodegenerative disorder usually occurring in a younger population, characterized by emotional problems, loss of thinking ability and abnormal choreiform movements .
Simple Skin Test Can Confirm Parkinsons Diagnosis
This post is available in: Spanish
Patients suspected of having Parkinson’s disease can now have their diagnosis confirmed with a simple skin test available at Marcus Neuroscience Institute in Boca Raton. The test identifies abnormal alpha-synuclein proteins in nerve fibers of the skin, which experts say are linked to Parkinson’s and a variety of other movement disorders.
Sameea Husain Wilson, D.O., director of Movement Disorder Neurology for Marcus Neuroscience Institute at Boca Raton Regional Hospital, says the Syn-One Test gives movement disorder specialists like herself the ability to confirm a clinical diagnosis with up to 99 percent accuracy.
“Diagnosing a neurodegenerative disease such as Parkinson’s disease, dementia with Lewy bodies, or multiple system atrophy can be challenging,” says Dr. Husain. “While patients with advanced disease have symptoms that are fairly obvious, that’s not always the case for those with early-stage disease.”
Studies show that a misdiagnosis can occur 30 to 50 percent of the time in earlier stages of a neurodegenerative disease. This, Dr. Husain says, is why you want to see a fellowship-trained neurologist who is specially trained to spot the differences between Parkinson’s disease and other movement disorders. It’s also why you want to go to a specialized center such as Marcus Neuroscience Institute that offers the Syn-One test.
- Tremor, mainly at rest
- Limb rigidity
- Gait and balance problems
