First Signs Of Impaired Righting Reflexes This Is Evident As The Patient Turns Or Is Demonstrated When He Or She Is Pushed From Standing Equilibrium With The Feet Together And Eyes Closed

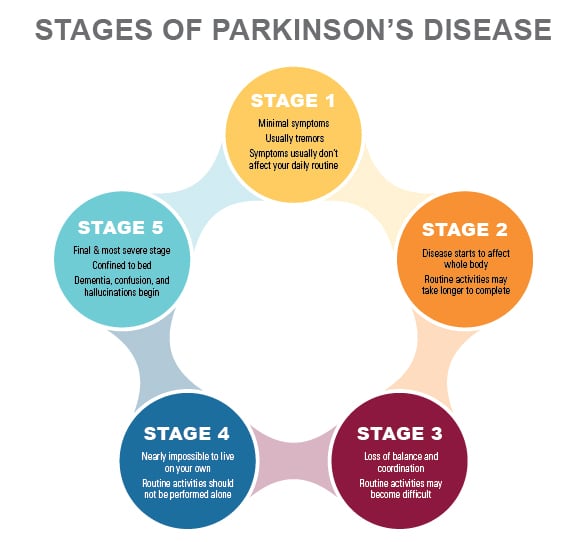
Loss of balance, with the inability to make the rapid, automatic and involuntary movements necessary to protect against falling, is one of the most troubling and dangerous aspects of Parkinsonism and one of the least easily treated. Even when manifested by only slight unsteadiness, it is the criterion separating Stage II and Stage III. All other aspects of Parkinsonism are evident and usually diagnosis is not in doubt.
However, the most important factor identifying Stage III is that the patient is still fully independent in all activities of daily living Although somewhat restricted, has work potential depending upon the type of employment. A normal life can be.
If You Live In South Jersey And Have Questions About The Final Stages Of Parkinsons Disease Or Hospice Care For Your Loved One Please Call Samaritan At 229
Samaritan is a member of the National Partnership for Healthcare and Hospice Innovation, a network of not-for-profit hospice and palliative providers across the country. If you know someone outside of our service area who is living with advanced illness and can benefit from hospice or palliative care, please call 1 -GET-NPHI for a referral to a not-for-profit provider in your area.
Fully Developed Severely Disabling Disease; The Patient Is Still Able To Walk And Stand Unassisted But Is Markedly Incapacitated
The patient is unable to lead an independent life because of the need for help with some activities of daily living. It is this inability to live alone which marks the transition from Stage III to Stage IV. No matter how difficult it is for him/her, if the patient still is able to live alone, his/her disease is at Stage III not Stage IV. The patient at Stage IV however, does remain able to stand and walk unassisted.
Want To Learn More About The Latest Research In Parkinsons Disease Ask Your Questions In Our Research Forum
Stage 3As motor symptoms become worse, patients may begin to experience loss of balance leading to falls and movement can become very slow. Although many patients can still live independently they may have difficulty in everyday activities such as eating or dressing.
MORE: How does Parkinson’s disease affect the brain?
Stage 4In this later stage, symptoms are now extremely limiting. Many patients can still stand without assistance but movement is greatly impaired. Most will need help with everyday activities and will not be able to look after themselves.
Stage 5This is the most advanced stage of the disease and most patients will experience difficulty in walking and standing, often requiring a wheelchair. Assistance will be needed in all areas of daily life as motor skills are seriously impaired. In addition, people with advanced Parkinson’s disease may also begin to suffer hallucinations.
MORE: How Parkinson’s disease affects your body.
Parkinson’s News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Can A Patients Ability To Make Decisions In The Last Days Of Life Be Impaired And How Is This Managed
In a North American study of 47 carers of idiopathic PD patients in the last months of life most described the goal of care as comfort, and almost half “of the patients were described as unable to make any decisions in the last month of life.” 10
When presenting, the patient may already be unable to communicate their symptoms and care preferences due to cognitive impairment and confusion. Also, there might be a physical difficulty in communication from severe rigidity. Care should be taken in considering the presence and consequent treatment of an intercurrent illness, and whether dopaminergic medication is exacerbating confusion due to hallucinations and/or psychosis.27
Continued attempts at verbal and non-verbal communication should be made throughout given the often fluctuating symptoms associated with PD and possible improvement in the intercurrent illness. In the absence of a next of kin or other person who is able to inform the clinical team, decisions should be made on a best interest basis as recommended in end of life care guidance.30
Stage Four: Symptoms Are Severe And Disabling And You Often Need Assistance To Walk Stand And Move
Stage Four Parkinson’s disease is often called advanced Parkinson’s disease. People in this stage experience severe and debilitating symptoms. Motor symptoms, such as rigidity and bradykinesia, are visible and difficult to overcome. Most people in Stage Four aren’t able to live alone. They need the assistance of a caregiver or home health aide to perform normal tasks.
Stage Three: Symptoms Are More Pronounced But You Can Still Function Without Assistance
The third stage is considered moderate Parkinson’s disease. In this stage, you’ll experience obvious difficulty with walking, standing, and other physical movements. The symptoms can interfere with daily life. You’re more likely to fall, and your physical movements become much more difficult. However, most patients at this stage are still able to maintain independence and need little outside assistance.
What Are The Considerations For Pain Management In The Last Days Of Life In Pd
It is important to consider that pain can be a risk factor for, and associated with, many other symptoms which might be the presenting features in a patient with complex or advanced PD. These include a new or worsened confusion, hallucinations, agitation and symptoms of depression or apathy.
As well as being an underlying cause of another symptom, pain can also be the symptom of other features of PD, such as rigidity, dyskinesia, but also non-motor features, for example, depression and fatigue.
Identifying whether pain is at the root of the presenting complaint and what might be causing the pain is therefore the most important part of the initial history from the patient and the carer. Then using the clinical examination to confirm findings from the history and identify any features not already elicited such as abnormal posturing, or dystonia.
A recent review into the pathophysiology and treatment of pain in PD suggests simple analgesia with paracetamol and non-steroidal anti-inflammatory drugs but advises caution with opiate analgesia as constipation is a recognised problem in PD patients.25 The review mentions, however, the lack of evidence for many widely used analgesics specifically in PD.26
How Can I Support Someone With Parkinson’s At The Advanced Or Palliative Stage

In the advanced stages of Parkinson’s, your patient’s care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the ‘whole person’ to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinson’s may be supported by a number of professionals, including a Parkinson’s nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinson’s also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinson’s should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the person’s wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesn’t want to have in the future – this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
How Can Hospice Help Your Loved One In The Final Stages Of Parkinsons Disease
Hospice care is an extra layer of support to help you care for your loved one with end-stage Parkinson’s disease. It is a special kind of care that provides comfort, support, and dignity at the end of life.
The comprehensive program focuses on physical, emotional, and spiritual quality of life through the help of a team of experts. The team includes a board-certified physician, nurse, social worker, certified home health aide , spiritual support counselor, and volunteer.
The nurse will explain the prognosis and what to expect in the upcoming days or weeks. They will also monitor pain and other symptoms. The CHHA helps with personal care needs like bathing and changing bed linens. The social worker helps address social, emotional and practical challenges including complex and inter-related needs. The spiritual support counselor helps explore spiritual concerns.
Most importantly, the hospice team will be there for you during this difficult time, bringing you peace of mind. The team is on call 24 hours a day – even at 2:00 am.
Hospice is about making your final months and weeks as good as possible. This means focusing on what really matters to you.
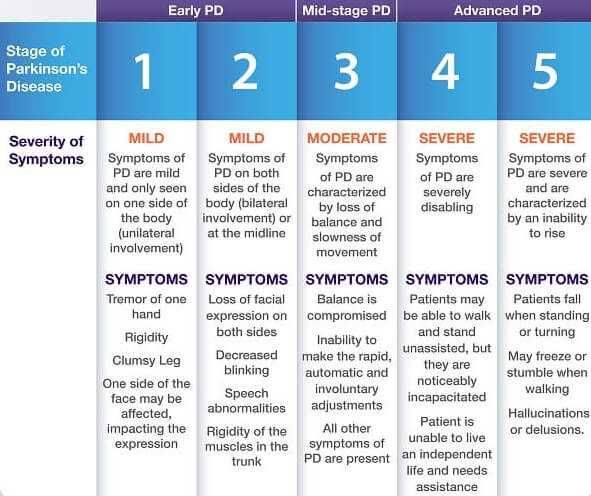
Unilateral Involvement Only Usually With Minimal Or No Functional Impairment
The patient has tremor, rigidity, slowness and paucity of movement, or poor condition in the arm and/or legs on one side of the body. Occasionally one side of the face is involved, producing an asymmetry of expression that may look very like the effects of a mild stroke or Bell’s palsy. This stage of Parkinson’s is often missed entirely. For example when the diagnosis is made at a more advanced Stage, the patient may remember having noticed an intermittent tremor of one hand many years before. Old home movies may show that the patient didn’t swing one arm as much as the other did while walking. One hand or foot may have been clumsier than the other may have. Often these symptoms are so mild that no formal medical attention is sought. If sought it is not uncommon that the physician is unable to make a diagnosis, either by the most assiduous and astute physical examination or by the most advanced technology. Sometimes the disease must evolve over many years before a diagnosis can be made with certainty.
“Usually” was inserted into the original definition to modify “minimal” or no functional impairment: because, very rarely, a patient presents with very severe and disabling unilateral symptoms: extreme and violent tremor or rigidity and akinesia in one limb so severe that the limb is virtually paralyzed. Most doctors worry about a stroke or tumor – which they should. When all necessary tests show nothing, one must wait and observe. Eventually Stage II may emerge.
What Are The Important Points Regarding Apomorphine At The End Of Life
Apomorphine is a dopamine agonist, which is given as a subcutaneous infusion either continuously or intermittently and also as single subcutaneous injections. An overview of studies into apomorphine use shows improvement in motor off periods and in dyskinesias.39
Apomorphine has side-effects similar to other dopaminergic medication but also notably nausea and vomiting. Ondansetron is not recommended for nausea in patients using apomorphine due to adverse effects.21
Subcutaneous apomorphine has been used at the end of life in a patient with advanced PD although with the recommendation that this is by a healthcare professional experienced in its use.40
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage
Parkinson’s progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinson’s about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinson’s may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more ‘off’ periods – when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinson’s symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinson’s most often die because of an infection or another condition, usually caused by Parkinson’s.
What Are The Important Points Regarding Duodopa At The End Of Life
Duodopa is a continuous infusion of dopaminergic medication administered as a gel into the gut, pumped via a percutaneously inserted gastrostomy tube . There is a requirement for care of the stoma and PEG tube together with functioning of the pump by the patient or carer.41 It reduces the time in motor off periods in advanced PD and quality of life.42 There is evidence of effective treatment up until death from within a case series.43
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
What Are The Risks Of Not Receiving Any Dopaminergic Medication
There is the possibility of neuroleptic malignant-like syndrome , a life-threatening and distressing condition resulting in rigidity and fever, from withdrawal of therapy.31 This can also occur with sudden cessation of Deep Brain Stimulation .32,33,34 To reduce the risk of this, dopaminergic therapy at the end of life should be continued.27 It should also be noted that in a patient dying of another condition, whose PD is still responsive to dopaminergic medication, the cessation of this also risks aspiration pneumonia.35 Transdermal rotigotine can be used in patients in whom a NG tube may cause excessive distress or is not possible. The dose should be calculated with an accepted converter.36
Bilateral Or Midline Involvement Without Impairment Of Balance
![Neural Stem Cell Therapy for Parkinson’s Disease [PD]](https://www.parkinsonsinfoclub.com/wp-content/uploads/neural-stem-cell-therapy-for-parkinsons-disease-pd.jpeg)
Months or years later similar symptoms and signs are noticed on the opposite side of the body, or other signs appear in “midline” what physicians call “Axial” signs. These may include: bilateral loss of facial expression ; decreased blinking; speech abnormalities; soft voice, monotony, fading volume after starting to speak loudly, slurring, stiffness of truncal muscles making the patient appear awkward and stiff or resulting in neck and back pain; postural abnormalities causing stooping, generalized slowness in, but still capable of, carrying out all activities of daily living, sometimes an aggravation to those waiting for the patient to complete tasks.
Usually the diagnosis is easy at this Stage if it has been preceded by a clear cut tremor or other symptom on one side. But not all Parkinson’s patients have tremor or other definite signs of Stage I unilateral Parkinsonism. If Stage I was missed and the predominant symptoms at Stage II are only slowness and a lack of spontaneous movement, the diagnosis may still be in doubt. For example, even in Stage II, Parkinsonism may be interpreted as only advancing age.
Which Medications Can Make Confusion And Hallucinations Worse
As PD progresses, non-motor symptoms including psychosis and hallucinations become more prominent both for the patient and caregivers.9 Dopaminergic medication can exacerbate these symptoms and this can be reduced through a “last in, first out approach.” 27,28 Medications that have an anticholinergic effect also may cause or worsen acute confusion and the anticholinergic burden in the patient’s medication history should be considered.29
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
What To Expect In The The Final Stages Of Parkinsons Disease Blog
- Blog Archive
When your older family member’s doctor told them that they have Parkinson’s disease, they probably explained that the disease gets worse over time. However, as a family caregiver, you may be uncertain just what that means for their future. In fact, you might be wondering just how bad the disease will get. Knowing what to expect can assist you with making plans for their care when the disease reaches its final stages.
What Are the Late Stages of Parkinson’s Like?
There are five stages of Parkinson’s disease. When doctors talk about the “late stages” of Parkinson’s disease, they are usually referring to stages four and five. By the time the senior reaches stage four, they are disabled and need help to do many things. They might still be able to stand up on their own but will probably need to use a mobility aid like a walker to move around safely. Because they need help with many daily activities, the senior will not be able to live alone.
In stage five, your aging relative will no longer be able to stand up or get out of bed without help. They are likely to fall when they are standing or turning. Because of the high probability of falling, the person must have constant care to keep them safe. In addition to motor symptoms, the senior may also experience delusions or hallucinations.
Late Stage Care
If you or an aging loved-one are considering senior care in Forest Acres, SC, please talk to our caring staff. Call today 223-6173.
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38 and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patient’s handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
Parkinson’s Progression Palliative And End Of Life Issues
This 38-minute webinar provides an overview of Parkinson’s symptoms, and treatment challenges due to disease progression. 18-minutes in the topic turns to planning a good death, the euphemisms even doctors use to avoid discussing death, the most common cause of death in those with PD, putting your end-of-life preferences in writing. Palliative care can help families face these end-of-life issues.
What To Expect In The Late Stages Of Parkinsons Disease
The late stages of PD are medically classified as stage four and stage five by the Hoehn and Yahr scale:
- Stage Four of Parkinson’s Disease – In stage four, PD has progressed to a severely disabling disease. Patients with stage four PD may be able to walk and stand unassisted, but they are noticeably incapacitated. Many use a walker to help them. At this stage, the patient is unable to live an independent life and needs assistance with some activities of daily living. The necessity for help with daily living defines this stage. If the patient is still able to live alone, it is still defined as Stage Three.
- Stage Five of Parkinson’s Disease – Stage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking. Around-the-clock assistance is required at this stage to reduce the risk of falling and help the patient with all daily activities. At stage five, the patient may also experience hallucinations or delusions.1,2
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Stage One: Symptoms Affect Only One Side Of Your Body
The initial phase of Parkinson’s disease typically presents with mild symptoms. Some patients will not even detect their symptoms in the earliest phases of this stage. Typical motor symptoms experienced in Stage One include tremors and shaking limbs. Family members and friends may begin to notice other symptoms including tremor, poor posture, and mask face or loss of facial expression.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinson’s disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinson’s disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinson’s disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinson’s disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinson’s disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Caring For A Person With Advanced Parkinsons Disease
In this 47-minute webinar Anne Wallis, Associate Director of Education at the Parkinson’s Foundation, talks with doctor of physical therapy, Sarah King, about when to look for outside help, how to lasso the power of your friends and family , and how to build an allied healthcare team that decreases your stress and improves your loved ones care.
Caregiving In The Late Stages Of Parkinsons Disease

In late-stage PD, patients have significant mobility challenges. Caregivers likely need to provide more hands-on assistance to help them get around the house. It’s important that caregivers learn safe and effective methods to provide help without injuring themselves. Physical therapists can be a great resource to assess an individual situation and teach effective ways of giving assistance.3
Freezing, a sudden but temporary inability to move, can become more common in late-stage PD. Freezing often happens when initiating movement or navigating around obstacles, and freezing episodes contribute to falls. Caregivers can help their loved one overcome freezing by providing a visual cue to step over, like a laser pointer, or using music or rhythm for the person with PD to walk to.3
Late stage PD can make daily activities, such as getting dressed, much more challenging. Caregivers can make getting dressed easier by ensuring adequate time to account for slow movement, choosing a time when medications are “on” and working well, and assembling all necessary items close to the person. Allowing the person with PD to do as much as they can gives them a sense of participation in the process.3
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinson’s disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinson’s disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinson’s disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
How Long Can A Person Live With Stage 5 Parkinson
When patients reach stage five – the final stage of Parkinson’s disease – they will have severe posture issues in their back, neck, and hips. In end–stage of Parkinson’s disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
Additionally, what do Parkinson’s patients usually die from? But the most common cause of death in those with Parkinson’s is pneumonia, because the disease impairs patients‘ ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
Also asked, what happens in stage 5 Parkinson’s?
Stage Five of Parkinson’s Disease –Stage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
How quickly can Parkinson’s progress?
While symptoms and disease progression are unique to each person, knowing the typical stages of Parkinson’s can help you cope with changes as they occur. Some people experience the changes over 20 years or more. Others find the disease progresses more quickly.
Care Of Patients With Advanced Parkinsons Disease
Presenting at the UCSF 9th Annual Conference of Parkinson’s Disease for Patients and Caregivers, Dr. Maya Katz spoke for 38-minutes about caring for those with advanced Parkinson’s disease, including a definition of advanced PD, medication considerations, non-motor symptoms, wellness and exercise, goals of care and taking a supportive care approach.
