The Need For Digital Health Solutions In Deep Brain Stimulation For Parkinson’s Disease In The Time Of Covid19 And Beyond
Copyright and License informationDisclaimerCopyrightFigure 1
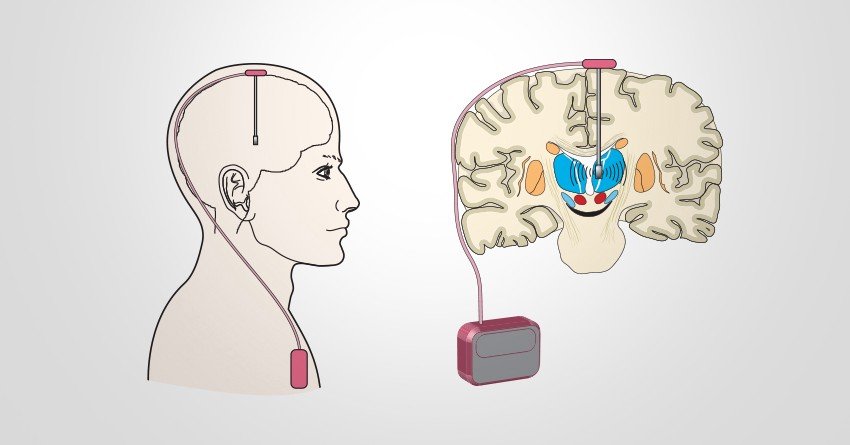
The necessary components of a distance health encounter with the medical professional on the left as it transitions to the patient on the right and vice?versa. .
The implementation of a digital health encounter between a patient and his or her neurologist in synchronous and asynchronous paradigms. .
The online version has been corrected.
We apologize for this error.
Using Computerized Spiral Analysis To Evaluate Deep Brain Stimulation Outcomes In Parkinson Disease SaraRadmarda
Spiral analysis is a computerized test that assesses DBS effects in PD subjects.
- •
-
Novel indices are generated that correspond to important clinical motor findings.
- •
-
These indices provide objective perspectives on clinical features modulated by DBS.
- •
-
All indices improved after DBS except Tightness, the correlate of micrographia.
Deep Brain Stimulation Effective Long Term In Improving Motor Function In Parkinson Disease Matthew Gavidia
In comparing the efficacy of deep brain stimulation of the subthalmic nucleus and globus pallidus, both approaches were similarly effective in improving motor function in people with Parkinson disease, with benefits maintained after 10 years.
Deep brain stimulation of the subthalmic nucleus and globus pallidus provided significant short-term and long-term improvement in motor function for people with Parkinson disease , with DBS of the STN shown to be slightly more effective, according to an abstract presented at the American Academy of Neurology’s 73rd Annual Meeting being held virtually April 17-22, 2021.
In prior research, DBS has been associated with a myriad of benefits for patients with PD, ranging from improvements in social, occupational, and psychosocial function to decreasing risk of disease progression. However, it has been cited to lose efficacy over time.
Examining the 2 main types of DBS studied in PD, surgery within the STN and GPi, the researchers of the present study sought to examine the long-term outcomes of both approaches for patients with the condition.
“There are no published studies from prospective randomized trials examining outcomes beyond 3 years comparing STN to GPi DBS,” said the study authors.
Compared with baseline, at which the score was 43.2, motor function was significantly improved and maintained at each completed visit for both the GPi-DBS group and STN-DBS group , respectively.
Reference
How Long Will It Take For Me To Feel The Benefits Of Deep Brain Stimulation
The stimulator is not activated immediately after the surgery.
During the appointment with your specialized neurologist within two weeks of the operation, your stimulator will be activated. The medical team will then try different electrical current adjustments to maximize symptom control and minimize side effects.
In the next two months, your medical team will gradually increase the intensity of the electrical current and decrease your doses of levodopa. This adjustment period may take several months before you get the most out of this procedure.
Some devices allow patients to change the current intensity themselves according to their daily activities. In the near future, these DBS systems will be able to automatically adjust their intensity according to your needs.
Will I Have To Limit My Activity Following Deep Brain Stimulation Surgery
- You should not engage in light activities for 2 weeks after surgery. This includes housework and sexual activity.
- You should not engage in heavy activities for 4 to 6 weeks after surgery. This includes jogging, swimming, or any physical education classes. Anything strenuous should be avoided to allow your surgical wound to heal properly. If you have any questions about activities, call your doctor before performing them.
- You should not lift more than 5 lbs. for at least 2 weeks.
- You should not raise your arms above your shoulders or over bend or stretch your neck.
- Depending on the type of work you do, you may return to work within 4 to 6 weeks.
How Does The Neurosurgeon Know Where To Place The Electrodes In My Brain
Positioning the electrodes in the brain is the most critical step. The electrodes have to be placed in an exact location in the brain to improve symptoms. Computed tomography or magnetic resonance imaging scans are taken before and/or during the procedure to pinpoint the exact areas to target and guide the lead and electrode placement. Many times an electrode may be used to record brain cell activity at the target site to improve lead placement.
Which Parts Of The Brain Are Targeted Using Dbs For Movement Disorders
Before the procedure, a neurosurgeon uses noninvasive diagnostic imaging—either magnetic resonance imaging or computed tomography scanning—to identify and locate the exact target in the brain for the surgery. Most surgeons use microelectrode recording—which involves insertion of a tiny wire that monitors the activity of nerve cells—to more specifically identify the precise brain area that will be stimulated.
For treatment of Parkinson’s disease, DBS targets parts of the brain that play a role in the control of movement—the thalamus , subthalamic nucleus , or globus pallidus . DBS for dystonia specifically targets the globus pallidus interna , while DBS for essential tremor targets the thalamus. Different areas of the brain may be targeted for individuals with epilepsy who don’t respond well to other therapies.
Up To Five Additional Hours Of Good Movement Without Dyskinesia
Good movement control means no troubling symptoms like shaking, stiffness, and difficulty moving. DBS therapy can provide up to five additional hours of good movement control without dyskinesia per day, compared with medication alone.*2,3,4 What would you do with five additional hours every day?
*Measured by the UPDRS IV
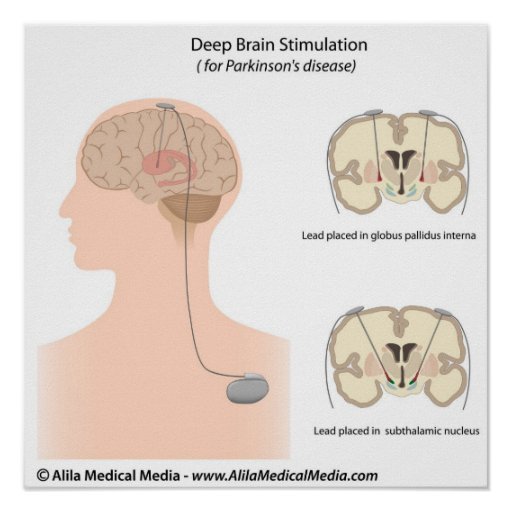
How Is Deep Brain Stimulation Used To Treat Parkinsons Disease
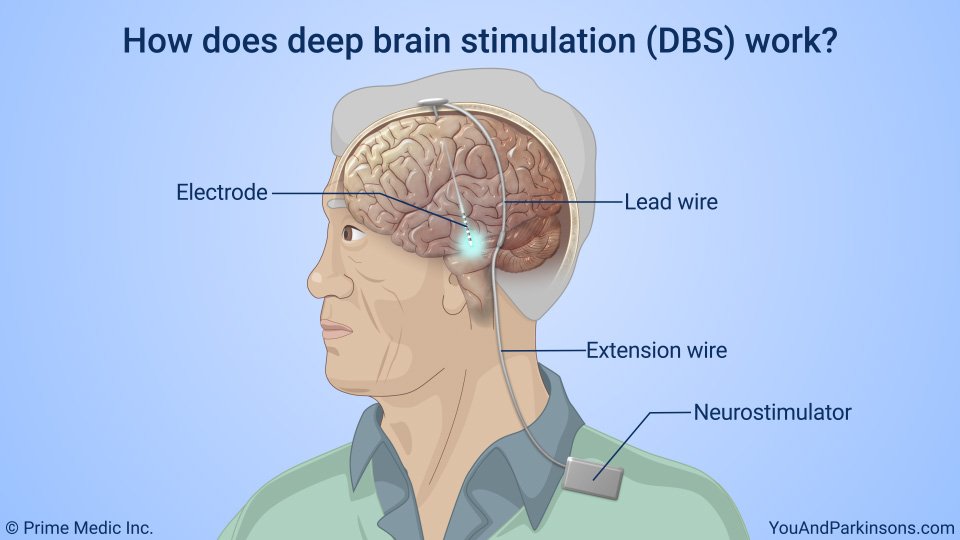
Deep brain stimulation delivers electrical impulses to a targeted area of the brain that is responsible for the movement symptoms caused by Parkinson’s disease. The electrical impulses disrupt the abnormal activity that occurs in the brain’s circuitry, which is causing the symptoms.
There are three areas in the brain that can be targets for deep brain stimulation in patients with Parkinson’s disease. They are the subthalamic nucleus, the globus pallidus internus, and the ventral intermediate nucleus of the thalamus. Each of these areas plays a role in the brain’s circuitry that is responsible for the control of movement.
The specific area in the brain to target in an individual with Parkinson’s disease depends on symptoms that need to be treated. For example, deep brain stimulation of subthalamic nucleus is effective for all major movement symptoms of Parkinson’s disease, such as tremor, slowness of movement , stiffness , and problems with walking and balance. Deep brain stimulation of globus pallidus is another effective target for a wide range of Parkinson’s symptoms. The thalamic target is sometimes selected for patients with tremor symptoms. The recommended target for each patient is made collaboratively with the neurologist, neurosurgeon and other caregivers involved in the decision making process.
What Are The Risks And Complications Of Deep Brain Stimulation
As with any surgical procedure, there are risks and complications. Complications of DBS fall into three categories: surgery complications, hardware complications, and stimulation-related complications.
- Surgical complications include brain hemorrhage, brain infection, wrong location of the DBS leads, and less than the best location of the leads.
- Hardware complications include movement of the leads, lead failure, failure of any part of the DBS system, pain over the pulse generator device, battery failure, infection around the device and the device breaking through the skin as the thickness of skin and fat layer change as one ages.
- Stimulation-related complications occur in all patients during the device programming stage. Common side effects are unintended movements , freezing , worsening of balance and gait, speech disturbance, involuntary muscle contractions, numbness and tingling , and double vision . These side effects are reversible when the device is adjusted.
How Effective Is Deep Brain Stimulation For Parkinsons Disease
Deep brain stimulation provides excellent relief for most patients’ symptoms including tremor, stiffness , slowed movement , freezing of gait and dyskinesias. Long-term studies have shown continued improvement in tremor, bradykinesia, and dyskinesia. Many patients are able to reduce their medications and maintain their level of function including independent participation in activities of daily living required to care for oneself. One of the distinct advantages, is that after DBS, patients on average improve their daily ‘on time’—when they are at their best, without troublesome dyskinesia—by half a day.
How Long Does The Battery In The Impulse Generator Device Last
Batteries can last 3 to 5 years in non-rechargeable devices and up to 15 years or even longer in rechargeable battery devices. However, these times may vary significantly. A simple outpatient procedure is needed to replace the battery. Rechargeable battery devices can be charged daily or every 10 to 14 days . Your doctor will discuss how often you should recharge your battery based on your therapy settings.
If The Mechanism Of Dbs Is Not Known Why Should I Consider It
Because it works.
Because it is quite safe.
There are many things for which we don’t understand the exact reason. For example, we are still finding out more about the myriad benefits of exercise.
For example – How does exercise improve Mood? We don’t understand that too well. But it is easy to grasp that exercise is good for you.
This what-you-see-is-true evidence is called “Empiric Evidence”.
How Do I Know If Im A Candidate For Deep Brain Stimulation
Before being considered a candidate for deep brain stimulation , patients with Parkinson’s disease must undergo an extensive evaluation process. Ideally, a multidisciplinary team of specialists in the area of movement disorders will assess the patient. This clinical team typically includes a neurologist, neurosurgeon, neuropsychologist and psychiatrist.
If patients are well managed on medications, DBS is not considered. Candidates for DBS are patients who meet one or more of the following criteria:
- Symptoms are not well controlled despite receiving the appropriate dose of levodopa and other medications.
- Symptoms are significantly reducing patients’ quality of life.
- Abnormal or uncontrolled involuntary movements or motor fluctuations are not improving despite adjustments in medications.
- Four or more doses of levodopa are required a day.
- Tremors that have not been able to be controlled by medications.
Levodopa response test
Patient’s response to a single dose of levodopa is another test physicians use to identify which patients are likely to benefit from DBS. In this test, patients stop taking levodopa for 8 to 12 hours and then receive a single dose. Patients are likely to benefit from DBS if they have a clear positive response after receiving the single dose of levodopa.
Deep Brain Stimulation For Parkinson’s May Help Long Term HealthDay Reporter
THURSDAY, June 3, 2021 — Parkinson’s disease patients can get symptom relief with deep brain stimulation therapy that lasts over the long term, a new study shows.
Over 15 years, patients who received DBS, which requires surgical implantation, had significant improvement in motor symptoms and less need for medication, researchers found.
“Our study, for the first time, supports the efficacy of deep brain stimulation in the very long term — 15 years after surgery and 25 years since Parkinson’s diagnosis,” said senior researcher Dr. Elena Moro, director of the Movement Disorders Unit at Grenoble Alpes University in France.
“Indeed, after an average of 15 years after surgery, patients could experience improvement, compared to before surgery,” she said. “Moreover, we could still observe a marked reduction of anti-Parkinson’s medication and improvement of quality of life, compared with before the intervention.”
Patients with Parkinson’s disease no longer make dopamine, which affects their speech, walking and balance. Symptoms can be partially relieved by the drug levodopa, which temporarily restores dopamine.
But as levels of dopamine fluctuate during the day, patients can suffer from dyskinesia, a side effect of levodopa that can cause twisting, swaying or head bobbing.
For the study, Moro’s team collected data on 51 patients being treated with DBS. On average, they had the device for 17 years.
More information
What Risks Come Along With Doing Deep Brain Stimulation
DBS is a surgical procedure. As with any surgery there are some risks associated with it. Some of the risks of DBS include infection and bleeding. Your neurosurgeon may discuss some additional risks with you. Studies have shown that any risks are relatively small, but they should be kept in mind when considering DBS.
How Should I Care For The Surgical Area Once I Am Home
- Your stitches or staples will be removed 10 to 14 days after surgery.
- Each of the four pin sites should be kept covered with band aids until they are dry. You will be able to wash your head with a damp cloth, avoiding the surgical area.
- You may only shampoo your hair the day after your stitches or staples are removed, but only very gently.
- You should not scratch or irritate the wound areas.
What Is Deep Brain Stimulation For Parkinsons Disease
DBS is electrical stimulation of the brain by using a small machine. DBS can stimulate many brain areas.
DBS is actually approved for many diseases. It is not just a “Parkinson’s surgery”. It can be used for epilepsy and other movement disorders as well.
The basic setup is the same.
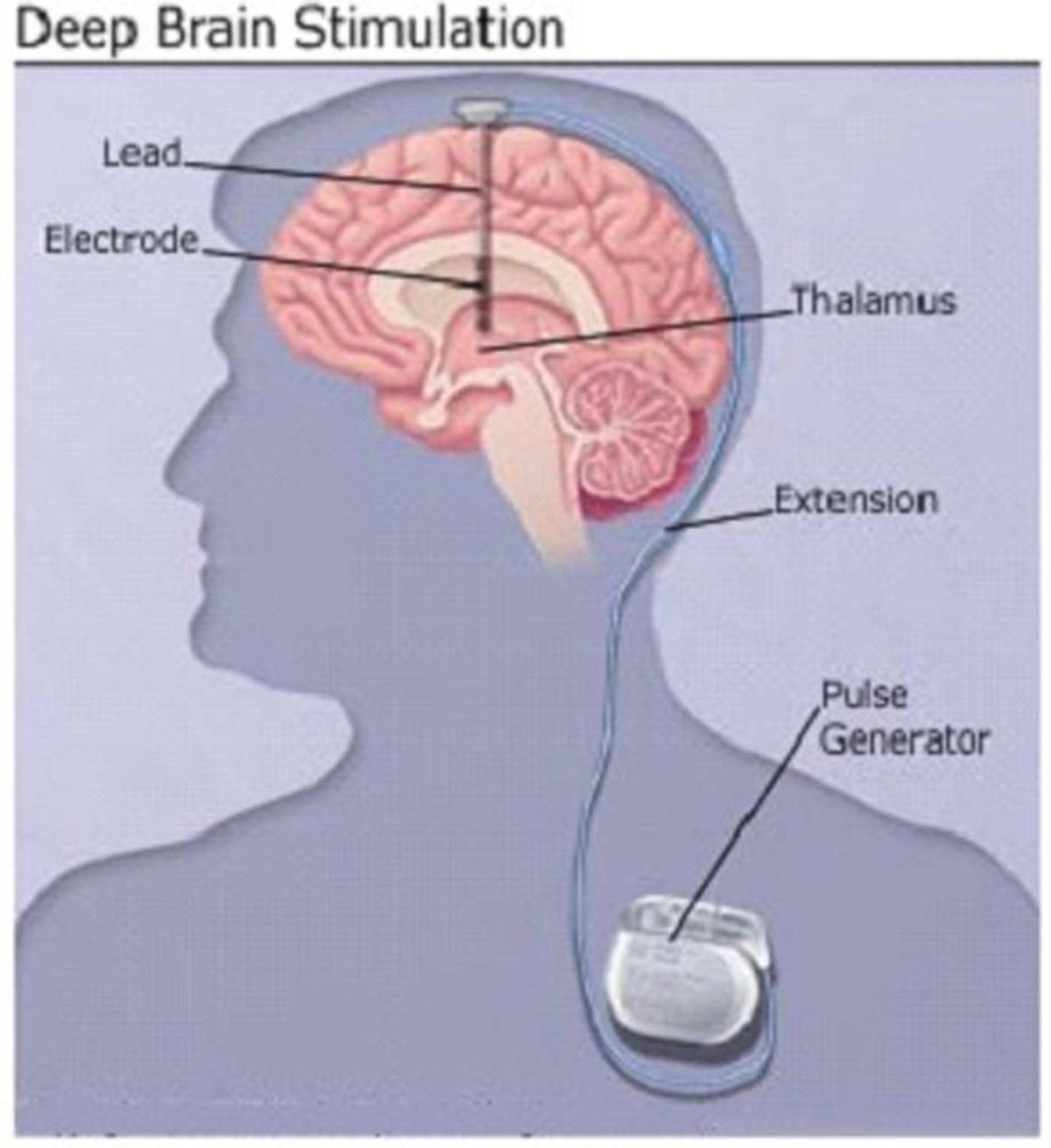
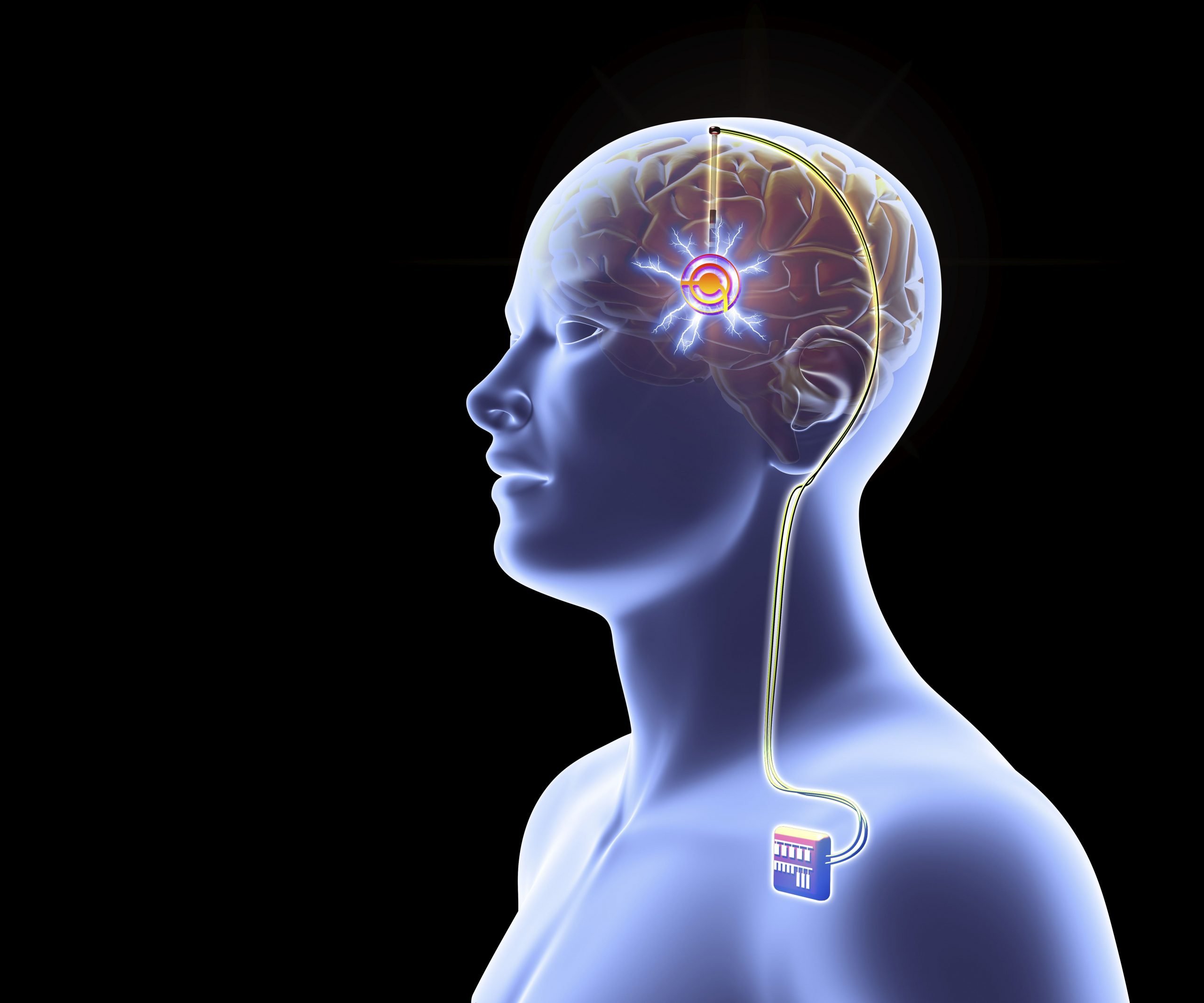
The DBS battery is inserted below the chest skin. Two small wires from the battery go up to the head. The wires go through the skull. They are inserted into the desired area of the brain.
For Parkinson’s disease: This target area of the brain is usually the “Subthalamic Nucleus .
In some patients, another area is chosen as the target. This other area is the Globus Pallidus interna .
How is the target chosen? Read this article
DBS can dramatically improve Parkinson’s symptoms. There are many before-after videos available on the internet.
For example, here is a video posted on youtube by the Neuromedical Center in USA.
What Kind Of Results Can You Expect After Having Dbs
A few weeks after the surgery, a specialist will program the DBS settings to your symptoms.
DBS won’t eliminate symptoms, but more than 70 percent of people with Parkinson’s experience a significant improvement.
You’ll likely be able to cut back on medication. DBS settings can be adjusted without surgery. It may take a few months to find the best combination of medications and DBS settings.
Surgery To Implant The Deep Brain Stimulation Device
Deep brain stimulation requires the surgical implantation of an electrical device into the brain. A neurosurgeon uses imaging scans to pinpoint the right spot in the brain for implanting the electrode.
When surgeons have determined the correct location, they create a small opening in the skull and insert a thin, insulated wire, through which they insert the electrode. Surgery to implant the electrode takes about four hours and requires general anesthesia. You may then stay overnight in the hospital for observation.
The next day, doctors perform the second part of the surgery, which involves connecting the insulated wire to a battery-operated pulse generator that is implanted under the skin near the collarbone. Most people can return home after this procedure.
Several days after the surgery, you meet with your neurologist, who programs the pulse generator. Pushing a button on an external remote control sends electrical impulses from the pulse generator to the electrode in the brain.
People who use deep brain stimulation work closely with their neurologist to find the combination of settings that best controls their symptoms. After several visits, they are able to control the strength of the electrical impulses on their own. Following this adjustment period, most people require only occasional maintenance visits.
What Results Can I Expect After Parkinson’s Surgery
Deep brain stimulation does not cure Parkinson’s disease or stop the degeneration of dopaminergic neurons.
However, deep brain stimulation reduces the severity of some motor symptoms such as severe tremors and slow movements.
Think of your best ON episode, i.e. when levodopa is most effective. This response is a good indicator of the best possible effect of deep brain stimulation on the extent and intensity of your symptoms.
Deep brain stimulation should significantly increase your ON time during the day and reduce your motor fluctuations. Your daily dose of levodopa should then decrease by half and therefore your dyskinesias caused by levodopa overdoses should partially disappear.
Deep brain stimulation substantially improves the quality of life of most patients who undergo surgery and usually gives them more autonomy in the performance of daily tasks.
However, this surgical procedure does not improve or only slightly improves Parkinson’s disease non-motor symptoms. Your symptoms that are unaffected by levodopa will most likely not improve after surgery.
Symptoms such as speech disorders, balance problems and cognitive disorders are generally unaffected by deep brain stimulation. These symptoms may even intensify after surgery.
Pallidal Stimulation Versus Subthalamic Stimulation
As mentioned, there are two main anatomic targets for using DBS to treat PD – the STN and the GPi. There have been several large randomized studies comparing STN and GPi DBS in PD. It is suggested that both STN DBS and GPi DBS overall equally and successfully improve motor symptom, and are similar in cost-effectiveness. However, although no differences were observed in the on phase between STN DBS and GPi DBS, significant differences were seen in the off phase; STN DBS was more effective in terms of motor function improvement in the off phase. There are different opinions in terms of effects of STN DBS and GPi DBS on quality of life. Some authors have found no significant difference between the STN and GPi targets. However, others agree with that greater improvements in quality-of-life measures are achieved in patients with GPi DBS.
GPi DBS can be used for patients with more axial symptoms, gait issues, dyskinesias, depression, and word fluency problems. STN DBS is often favored in reducing medication post surgery, and for patients with greater tremor. STN-DBS has also demonstrated an improvement in the quality of sleep for patients.
What Is Deep Brain Stimulation And How Does It Help
Deep Brain Stimulation or DBS as it is commonly called is a surgical treatment for people with certain types of Parkinson’s. It greatly helps in significantly improving the movement ability.
Deep brain stimulation helps control movement symptoms of Parkinson’s – tremor , slowed movement , and stiffness . When medications aren’t as effective as they used to be and your symptoms make everyday life a challenge, DBS may help.
Deep brain stimulation uses a small, pacemaker-like device, placed under the skin of the chest, to send electronic signals to an area in the brain that controls movement. To give you relief, these signals block some of the brain messages that cause the movement symptoms of Parkinson’s.
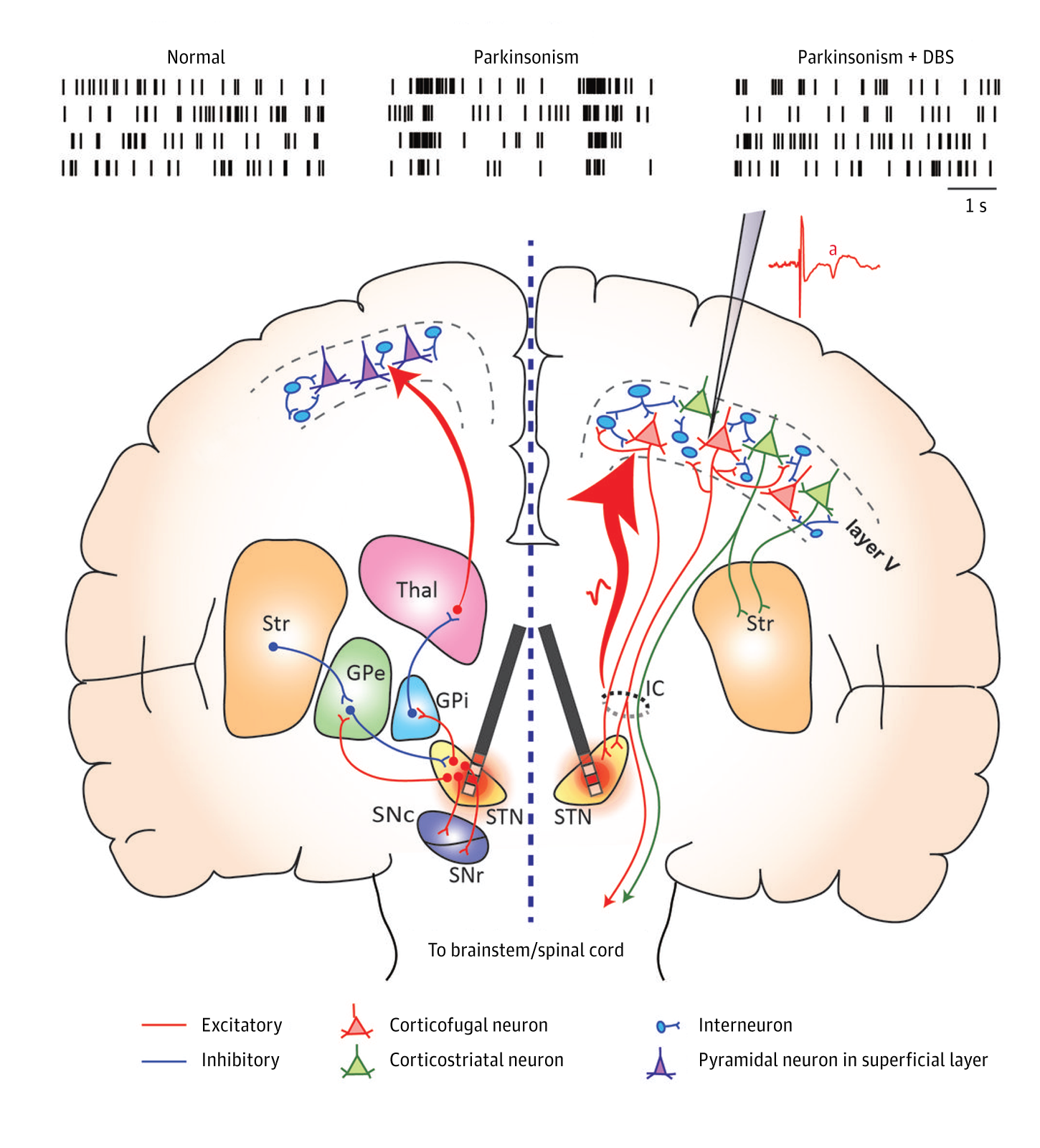
Findings On Medication Use And Motor Complications
The results showed that deep brain stimulation was effective at reducing motor complications from Parkinson’s disease for more than 15 years.
The researchers also found that the therapy reduced the amount of time a person experienced dyskinesia by a whopping 75%. Dyskinesia is a side effect of a common Parkinson’s medication called levodopa that results in rapid, involuntary body movements, like twisting, squirming, and head bobbing.
What’s more, participants spent about 59% less time in an “off state,” when medication stopped being as effective, and reduced their use of medications to manage dopamine levels by 51%.
Strength And Limitations Of Deep Brain Stimulation
Even though participants still experienced progression of Parkinson’s disease over the course of the study, their quality of life continued to climb by an average of 14% from the time of their surgery to their follow-up around 15 years later. That finding illustrates both the strengths and the limitations of deep brain stimulation for Parkinson’s disease, experts say.
Parkinsons Disease Surgery: Deep Brain Stimulation
Like all existing therapies for Parkinson’s disease, deep brain stimulation has no effect on the progression of the disease. However, it can help you better manage your tremors, slow movements, OFF periods and dyskinesias.
Surgery for Parkinson’s disease is limited to certain patients. If you are considering deep brain stimulation surgery, you should have realistic expectations about the results. This technique does not result in a complete cure and results vary from person to person
A multidisciplinary team consisting of a specialized neurologist, neurosurgeon, psychiatrist and other health care professionals can assess your eligibility and explain the benefits and risks of this procedure.
What Are The Advantages Of Deep Brain Stimulation
Deep brain stimulation has many advantages:
- DBS does not cause permanent damage in any part of the brain, unlike thalamotomy and pallidotomy, which surgically destroy tiny areas of the brain and therefore is permanent and not reversible.
- The electrical stimulation is adjustable and reversible as the person’s disease changes or his or her response to medications change.
- Because DBS is reversible and causes no permanent brain damage, use of innovative not-yet-available treatment options may be possible. Thalamotomy and pallidotomy result in small, but permanent changes in brain tissue. A person’s potential to benefit from future therapies may be reduced if undergoing these procedures.
- The stimulator can also be turned off at any time if DBS is causing excessive side effects without any long-term consequences.
How Is Dbs Being Used To Treat Movement Disorders
Parkinson’s Disease
DBS is used to treat the most commonly debilitating motor symptoms of Parkinson’s disease such as rigidity, slowed movement, stiffness, tremor, and problems walking. It is used only for individuals whose symptoms cannot be adequately controlled with medication. However, only people who improve to some degree after taking medication for Parkinson’s benefit from DBS. A variety of conditions may mimic PD but do not respond to medication or DBS.
Most people with PD still need to take medicine after undergoing DBS, but many people experience considerable reduction of their motor symptoms and may be able to reduce their medications. The degree of reduction varies by individual but can lead to a significant improvement in side effects such as dyskinesia . In some cases, the stimulation itself can suppress dyskinesia without a reduction in medication. DBS does not improve cognitive symptoms in PD and may worsen them. Therefore, it is not generally used if there are signs of dementia. DBS does not slow the progression of the neurodegeneration.
Dystonia
For individuals with dystonia, DBS may reduce the disorder’s characteristic involuntary muscle contractions that cause such symptoms as abnormal posture, repetitive movements, or twisting. DBS has been shown to reduce both the severity of symptoms caused by dystonia and the level of disability they may cause.
Essential Tremor
Epilepsy
What Is Deep Brain Stimulation How Does Dbs Work
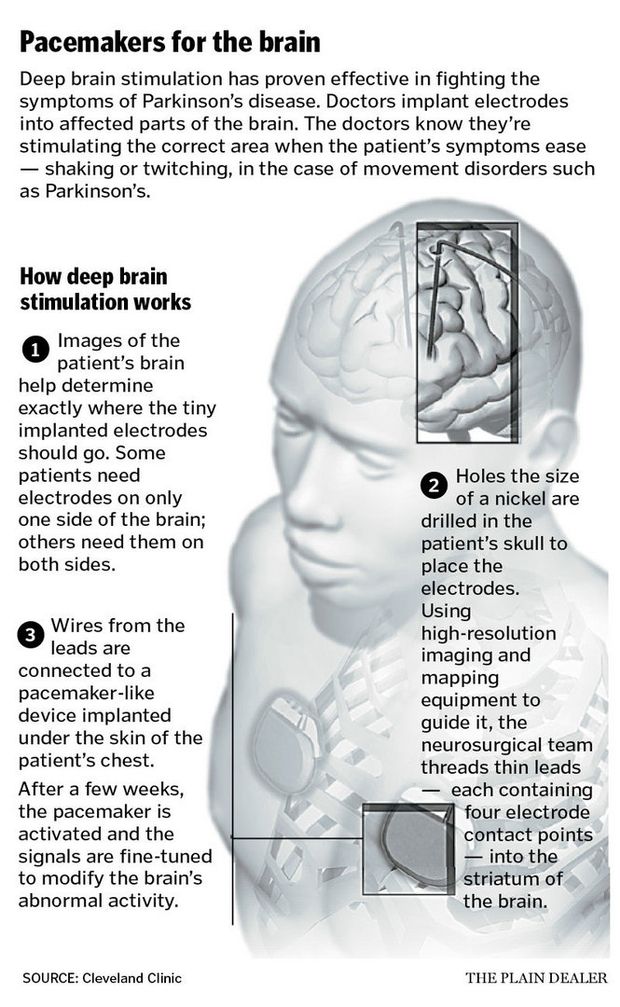
DBS is the short form of “Deep Brain Stimulation”. DBS is one type of Parkinson’s Surgery.
DBS works by passing a small current into the brain. This current is passed into only to a small part of the brain.
The doctor selects one out of two brain parts .
DBS works by changing the electrical currents in these areas. At present, we cannot mathematically calculate these changes.
But, empirically – DBS improves Parkinson’s symptoms.
Let us learn more about these topics:
Deep Brain Stimulation Surgery And Implantation
DBS consists of two surgeries, spaced approximately three to six weeks apart to ensure the patient has adequate time to recover. Throughout your experience, you will be attended to by a top team of physicians and other medical experts including a neurosurgeon, an electrophysiologist, and an anesthesiologist.
It should be noted that DBS offers many benefits. The generator can be programmed by a neurologist, and customized to each individual patient. The procedure is also reversible. Most patients experience a significant improvement of symptoms. However, as with any brain surgery, there are risks. With DBS, the risk of stroke is 1 in 100 and infection is 1 in 50.
Today, many more patients could be helped by DBS than are currently benefiting from the procedure. Statistics show only 7 percent of Parkinson’s disease and 1 percent of tremor patients in Michigan who would benefit from the procedure have undergone DBS. At U-M, we are proud to have one of the superior DBS programs in the country. We have developed a wide array of ways to improve DBS, including special imaging tools that help doctors more accurately place the electrodes, and lead intraoperative motor and speech testing that result in fewer side effects for the patient.
U-M is also home to an active research program, where our team of experts is always working on ways to make DBS faster and more accurate. We also regularly have clinical trials available for patients interested in participating.
Why A Doctor May Choose Deep Brain Stimulation
According to the National Parkinson Foundation, the ideal Parkinson’s disease candidate for DBS surgery has:
-
PD symptoms that interfere with activities of daily living.
-
Fluctuations in mobility due to PD medications with or without dyskinesia .
-
Continued good response to PD medications, even if the medication effects may wear off sooner than they have in the past.
-
A history of several different combinations of PD medications while under the supervision of a neurologist specializing in movement disorders.
These factors* may make a person a less than ideal candidate for DBS surgery:
-
Difficulty with balance, walking, or “freezing” as the main disabling symptom.
-
A primary symptom of speech difficulty.
-
Continuous confusion and problems with memory and thinking.
-
A psychiatric condition such as depression or anxiety that has not improved or stabilized with other treatment.
-
Another condition that increases the risk for surgery complications.
*Some of these factors may be treatable. Having one or more does not disqualify a person for future DBS surgery, but the doctor may recommend more aggressive therapy focused on these issues before surgery takes place.
Deep Brain Stimulation For Parkinsons Disease
For people with severe motor symptoms of Parkinson’s disease that are not adequately controlled by medication, a treatment called deep brain stimulation may offer some relief.
Deep brain stimulation requires the surgical placement of a small conductor called an electrode in the brain. The electrode delivers electrical stimulation that blocks the nerve signals that cause tremors.
Specialists at NYU Langone’s Center for Neuromodulation perform more than 100 deep brain stimulation procedures each year. Our neurologists, neurosurgeons, and psychiatrists provide a thorough evaluation to ensure you’re a good candidate for the procedure.
Who Is A Candidate For Deep Brain Stimulation
DBS is more than just a surgical procedure. It involves a series of evaluations, procedures, and consultations before and after the actual operation, so people interested in being treated with DBS should be prepared to commit time to the process.
For example, those who do not live close to a medical center that offers DBS surgery may need to spend significant time traveling back and forth to appointments.
The procedure, as well as the pre-operative evaluation and post-operative follow-up, can be expensive depending on the person’s insurance coverage. DBS surgery is an FDA-approved treatment for Parkinson’s disease, and Medicare and most private insurers cover the procedure, but the extent of coverage will depend on each person’s individual policy.
Prospective patients should have realistic expectations about DBS results. Although DBS can improve movement symptoms of Parkinson’s disease and greatly improve quality of life in properly selected patients, it is not likely to return anyone to perfect health.
Will I Be Asleep During The Entire Procedure
You will be sedated or receive local anesthesia for part of the procedure, may or may not be awake for lead and electrode placement, and will be asleep when the impulse generator is implanted. To provide more details:
- A local anesthetic is applied to areas of the head where pins or screws are used to secure the head frame and sedation is given.
- You will be sedated during the beginning of the procedure, while the surgical team is opening the skin and drilling the opening in the skull for placement of the lead.
- Most patients will be awake for lead and electrode placement. This part of the procedure is not painful, as the brain does not feel pain. Being awake allows the surgical team to interact with you when testing the effects of the stimulation. However, some patients who cannot tolerate the procedure while awake can have the electrode and lead placed under general anesthesia. The lead placement is guided in real time by magnetic resonance imaging. The procedure is performed in a special MR-equipped operation room.
- Implantation of the pulse generator in the chest and connection of the leads from the device to the lead in the brain is usually done under general anesthesia.
Treating The Movement Symptoms Of Parkinsons
Deep brain stimulation helps control your movement symptoms when your medications aren’t working as well as they used to. For many people with Parkinson’s, DBS makes a difference when even small tasks have become challenging. DBS has helped some people stay as independent as possible and keep doing the activities they love.
Deep Brain Stimulation In Parkinsons Disease Raja Mehanna
1University of Texas Health Science Center, Houston, TX, USA
2Center for Neurological Restoration, Cleveland Clinic, Cleveland, OH, USA
3University of Florida, Gainesville, FL, USA
4Parkinson’s, Movement Disorders and Neurorestoration Program, National Neuroscience Institute, King Fahad Medical City, Riyadh, Saudi Arabia
Deep brain stimulation of the subthalamic nucleus and globus pallidus interna is considered an essential therapy in the management paradigm of Parkinson’s disease . Its success stems essentially from its remarkable efficacy and, compared to the lesions created with thalamotomy and pallidotomy, its flexibility through programming that allows modification of the stimulation delivered to the precise brain targets, thereby obtaining maximal benefit with minimal side effects. In light of the impressive pace of advances in DBS technology, relentless exploration of new targets, development of programming paradigms, and continued controversy on patient selection and timing of DBS surgery, a special issue on this fascinating topic is pertinent and timely.
Raja Mehanna
