Overall 2020 Std Ranking
Using population figures, the most recent gonorrhea, chlamydia, and syphilis rates per 100K population, and Census.gov data on high school graduates percentage and percentage of household that have married couples, we gave all 50 states a score based on the prevalence of STDs and STD risk factors.
A higher STD index score indicates a higher likelihood of contracting an STD in a particular state.
States with the highest STD index score:
States with the lowest STD index score:
The Ghosts Of Pesticides Past
Over the past half century, we have begun to identify the worst risks and address them. The insecticide DDT was once considered a miracle compound. In the 1930s, the Swiss chemist Paul Hermann Müller was looking for a chemical that could kill insects that were destroying crops and spreading diseasewithout harming the plants. Müller, a nature lover, tested hundreds of chemicals before coating the inside of a glass box with DDT, a colorless, tasteless, and almost odorless nerve toxin. He placed houseflies into the container, and they bit the dust. Müller had found his answer.
In the 1940s DDT was considered harmless to humans and regularly sprayed on neighborhoods; here children play in the sprays at the beach in New York. Even though DDT was banned half a century ago, it persists in the environmentand in our food supply. It becomes more concentrated as it makes its way up the chain to human consumption. The pesticide is then stored in fatty tissues, including the brain. DDT has been linked to Parkinsons disease. Because of the widespread use of the pesticide, DDT and its breakdown products are detectable in nearly everyone in the United States. It has also been found in the breast milk of women living in Spain, Nicaragua, Taiwan, and the Spanish Canary Islands as recently as 2014.
Pictorial Press Ltd/Alamy Stock Photo
We eat fruits, vegetables, nuts, and grains every day that have been doused in pesticides. What kind of risk are we all exposed to? We do not know.
Parkinson Disease And Rurality
To test the hypothesis that Parkinson disease is associated with rural living, we used the United States Department of Agriculture’s rural-urban continuum classification system to classify residence for Medicare beneficiaries from the year 2003 and determined the mean prevalence and incidence per rural category. There was a significant difference in age- and race-standardized Parkinson disease prevalence and incidence between the rural classification categories .4). Post hoc analysis revealed that Parkinson disease prevalence for the most urban counties was significantly greater than that for the most rural counties . Similarly, Parkinson disease incidence for the most urban counties was significantly greater than that for the most rural counties .
Race/sex Demographics Of Parkinson Disease
The mean age-standardized prevalence of Parkinson disease from 1995, and 20002005 was highest among White men and lowest among Asian women .3). The mean age-standardized prevalence of Parkinson disease in Blacks and Asians was approximately 50% lower than the prevalence in Whites, with crude prevalence ratios of 0.58 and 0.62 , respectively, as compared to Whites. Parkinson disease incidence also varied by race, but not as markedly in Blacks, who had a crude incidence ratio of 0.74 .3). The incidence ratio for Asians was similar to the prevalence ratio . The age-standardized prevalence and incidence were greater in men than in women for all races, with a mean prevalence sex ratio of 155 males per 100 females and a mean incidence sex ratio of 146 males per 100 females.
Geographic Distribution Of Parkinson Disease In The Us
The incidence and prevalence of Parkinson disease varied significantly across the United States. Disease rates were highest in the Midwest and Northeast regions, where the incidence and prevalence of Parkinson disease were 210 times greater than the rates of many Western and Southern US counties. The median relative risk and interquartile relative risk indicated that the spatial variations of the incidence and prevalence were considerable .
County level age- and race-standardized incidence of Parkinson disease among Medicare beneficiaries in the United States .
How Is Parkinsons Diagnosed
Doctors use your medical history and physical examination to diagnose Parkinson’s disease . No blood test, brain scan or other test can be used to make a definitive diagnosis of PD.
Researchers believe that in most people, Parkinson’s is caused by a combination of environmental and genetic factors. Certain environmental exposures, such as pesticides and head injury, are associated with an increased risk of PD. Still, most people have no clear exposure that doctors can point to as a straightforward cause. The same goes for genetics. Certain genetic mutations are linked to an increased risk of PD. But in the vast majority of people, Parkinsons is not directly related to a single genetic mutation. Learning more about the genetics of Parkinsons is one of our best chances to understand more about the disease and discover how to slow or stop its progression.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
Men are diagnosed with Parkinsons at a higher rate than women and whites more than other races. Researchers are studying these disparities to understand more about the disease and health care access and to improve inclusivity across care and research.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
The Michael J. Fox Foundation has made finding a test for Parkinsons disease one of our top priorities.
Medication Changes And Mortality
Within the cohort of PD patients with COVID-19, 8 underwent reductions in their PD medications. Of these patients, 75% died, which was statistically significant when compared to those who died without PD medication changes 31% . These patients did not receive their PD medications for different reasons: due to mental status being impaired to the point that they could not safely take any oral medications; patients being made comfort care, and therefore no oral medications were administered; and all medications being held not related to the current COVID-19 illness. Since the reasons for medication changes differed, or was prompted by already aggravated prognosis, and was not limited to the PD medications, it is difficult to infer that the change in the PD medications was the cause of the increased mortality rate.
Us Parkinson’s Rates Highest In Whites Hispanics And Midwest Northeast
- Date:
- Washington University School of Medicine
- Summary:
- The largest epidemiological study of Parkinson’s disease in the United States has found that the disease is more common in the Midwest and the Northeast and is twice as likely to strike whites and Hispanics as blacks and Asians. The study is based on data from 36 million Medicare recipients.
The largest epidemiological study of Parkinson’s disease in the United States has found that the disease is more common in the Midwest and the Northeast and is twice as likely to strike whites and Hispanics as blacks and Asians.
The study, based on data from 36 million Medicare recipients, is both the first to produce any significant information on patterns of Parkinson’s disease in minorities and to show geographic clusters for the condition.
“Finding clusters in the Midwest and the Northeast is particularly exciting,” says lead author Allison Wright Willis, M.D., assistant professor of neurology at Washington University School of Medicine in St. Louis. “These are the two regions of the country most involved in metal processing and agriculture, and chemicals used in these fields are the strongest potential environmental risk factors for Parkinson’s disease that we’ve identified so far.”
The results appear online in the journal Neuroepidemiology.
Willis found Asians and blacks developed Parkinson’s disease at half the rate of whites and Hispanics.
Story Source:
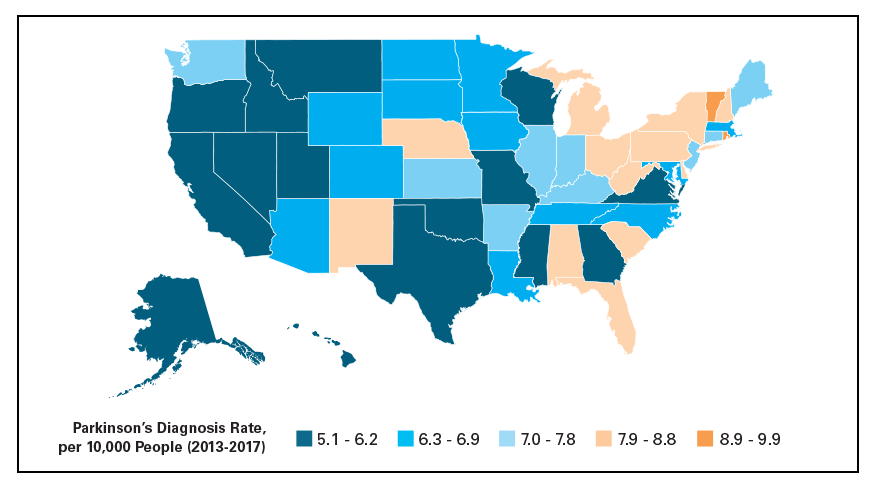
Prevalence Of Parkinsons State
Western and Southern states appear to have lower rates of Parkinsons disease, while Northeastern and many Midwestern states have higher rates . Mississippi and Montana have the lowest rates of Parkinsons, at 5.1 per 10,000. Vermont has the highest rate of Parkinsons at 9.9 per 10,000.
Exhibit 2: Prevalence of Parkinsons Disease, by geography
What Causes Parkinsons Disease
Parkinsons disease develops when there is a loss of nerve cells in the brain which produce a chemical called dopamine. Dopamine is a chemical messenger that transmits impulses between nerve cells in the brain to control body movements. Without enough dopamine, nerves in the brain which control muscle action do not work properly. When the loss of nerve cells reaches 80%, Parkinsons disease symptoms begin to appear. The disease progresses over time as dopamine levels in the brain gradually fall.
The reason for the nerve damage is currently unknown, although two areas currently being researched as possible causes are genetics and environmental factors.
Teaming Up To Find Treatments
It takes a wide variety of experts to understand how complex environmental and genetic factors can intertwine to affect human health. For that reason, the Parkinsons registry project reaches across disciplines and beyond the walls of the university to perform more comprehensive research.
One of the many researchers working alongside Church is Deborah Swackhamer, Ph.D., a professor of science, technology and public policy with the Us Humphrey School of Public Affairs who will study how environmental policy decisions have influenced the degree of exposure Minnesotans have had to pesticides. Another, Jerrold Vitek, Ph.D., of the Department of Neurology, will collaborate with a research team to develop a biological model that will help determine what factors contribute to Parkinsons disease.
Meanwhile, staff at the University of Minnesota Medical Center and the Struthers Parkinson Center will help identify and recruit research volunteers from within their patient networks to populate the registry. At Mayo Clinic, Dr. James Bower, an associate professor of neurology with Mayo, is examining ways to partner with Churchs efforts at the U of M to build and support the registry.
I am excited and energized by this project, he said. The support from medical, industrial, governmental and Parkinsons communities has been overwhelming.
The Impact Of Parkinsons Disease On Overall Health
Based on the Blue Cross Blue Shield Health Index, the overall health of those affected by Parkinsons is significantly lower than the general population. In 2017, the average BCBS Health Index for someone aged 30-64 with Parkinsons was 57, compared to 88 for the entire commercially insured population in this age range. This translates to an average of 10.7 years of healthy life lost for those with the condition compared to 3.4 years for the 30-64 population as a whole.
Caring for someone with Parkinsons Disease
The majority of Parkinsons patients are cared for by informal caregivers, such as a family member. The physical, mental and emotional work this requires can be significant. The Impact of Caregiving on Mental and Physical Health found that caregivers have 26% poorer health compared to a benchmark population, as measured by the BCBS Health Index. In addition, a national survey conducted by the Blue Cross Blue Shield Association found that 1 in 4 unpaid caregivers are feeling more stress trying to balance work and family due to COVID-19.
What Are The Symptoms Of Parkinsons Disease
The symptoms of Parkinsons disease develop gradually, as levels of dopamine fall. Early Parkinsons disease symptoms usually affect one side of the body. The main symptoms of Parkinsons disease include:
- Tremors: uncontrollable shaking, the symptom most associated with the disease, often beginning in the hands.
- Rigidity: stiffness or tensing of the muscles.
- Bradykinesia: slowness of movement, and loss of spontaneous movement.
- Postural instability: lack of balance and coordination which may lead to falling.
People with Parkinsons disease may also experience other problems, including tiredness, depression, sleep problems, cognitive impairment and difficulties with handwriting. They can also find their speech and facial expression change and some people have difficulties eating and swallowing.
The Danger Of Paraquat Today
The United States banned DDT, Agent Orange, and heptachlor in the 1970s and 1980s. However, the United States has not banned all pesticides linked to Parkinsons. The one with perhaps the strongest link to the disease is still in widespread use: paraquat.
The United States has not banned all pesticides linked to Parkinsons. The one with perhaps the strongest link to the disease is still in widespread use: paraquat.
Paraquat has been used as a pesticide since the 1950s and is marketed as an alternative to the worlds most popular weed killer, glyphosate, more commonly known as Roundup. Paraquat takes care of weeds that not even Roundup can kill. Today, it is used on farm fields across the United States, and its use continues to increase. The pesticides primary uses are for corn, soybeans, wheat, cotton, and grapes.
Portraits of several Parkinsons patients show the many faces of people with the diagnosis. It affects people from all walks of life.
Robert Dein
In the laboratory, paraquat reproduces the features of Parkinsons disease. In a 1999 study in Brain Research, A. I. Brooks of the University of Rochester and colleagues gave paraquat to mice, and their activity decreased. Paraquat also killed dopamine-producing nerve cells in the rodents substantia nigras. The greater the amount of paraquat administered, the greater the number of nerve cells lost.
Table adapted from: .
Figure adapted from R. Dorsey et al., 2020.
Parkinsons Disease In African Americans: A Review Of The Current Literature
Article type: Review Article
Affiliations: Rush University Medical Center Department of Neurological Sciences, Chicago, IL, USA
Correspondence: Correspondence to: Meagan Bailey, MD, MS, Department of Neurological Sciences, Rush University Medical Center, 1725 West Harrison, Suite 755, Chicago, IL 60612, USA. Tel.: +1 312 563 2900; Fax: +1 312 563 2024; E-mail: .
Keywords: Parkinsons disease, African Americans, healthcare disparities, epidemiology
DOI: 10.3233/JPD-191823
Journal: Journal of Parkinson’s Disease, vol. 10, no. 3, pp. 831-841, 2020
Abstract
Table 1
Research in African Americans with Parkinsons disease
Std Statistics 2020: States With The Highest Rates
Sexually transmitted disease infection rates continue to rise in the United States, with combined cases of chlamydia, gonorrhea, and syphilis hitting a new all-time high in 2018.
Additionally, each of the three most commonly reported STDs witnessed an increase in cases between 2017 and 2018, with reported gonorrhea cases increasing by 5 percent, chlamydia cases increasing by 3 percent, and primary and secondary syphilis cases increasing by a remarkable 15 percent to reach the highest number reported since 1991 .
In order to find out which states had the highest STD rates, we pulled the latest data from all 50 states on reported cases of the three most commonly reported sexually transmitted diseases, chlamydia, gonorrhea, and syphilis, from the the Centers for Disease Control and Preventions 2018 STD Surveillance Report. Then, we used this data and other variables to rank all 50 states based on overall STD infection rates.
A quick note on prevention: Theres no equivalent of a security system to help you identify carriers before having intercourse. Always make sure to use appropriate protection and choose your partners wisely.
What Is Parkinson’s Disease
Parkinsons disease occurs when brain cells that make dopamine, a chemical that coordinates movement, stop working or die. Because PD can cause tremor, slowness, stiffness, and walking and balance problems, it is called a movement disorder. But constipation, depression, memory problems and other non-movement symptoms also can be part of Parkinsons. PD is a lifelong and progressive disease, which means that symptoms slowly worsen over time.
The experience of living with Parkinson’s over the course of a lifetime is unique to each person. As symptoms and progression vary from person to person, neither you nor your doctor can predict which symptoms you will get, when you will get them or how severe they will be. Even though broad paths of similarity are observed among individuals with PD as the disease progresses, there is no guarantee you will experience what you see in others.
Parkinsons affects nearly 1 million people in the United States and more than 6 million people worldwide.
For an in-depth guide to navigating Parkinsons disease and living well as the disease progresses, check out our Parkinsons 360 toolkit.
What Is Parkinson’s Disease?
Dr. Rachel Dolhun, a movement disorder specialist and vice president of medical communications at The Michael J. Fox Foundation, breaks down the basics of Parkinson’s.
Prevalence/incidence Of Parkinson Disease In The Us
The mean prevalence of Parkinson disease per 100,000 Medicare beneficiaries over age 65 from 1995, and 20002005 was 1,588.43 or approximately 1.6% of the elderly population. The mean annual incidence from 2002 to 2005 was 445.79 . The mean prevalence of Parkinson disease steadily increased with age, with no apparent plateau, from 553.52 between ages 6569, to 2,948.93 per 100,000 at ages 85 and above. Similarly, mean Parkinson disease incidence also appears to increase with age, from 124.22 between ages 6569 to 970.19 among those greater than 85 years of age. The incidence and prevalence of Parkinson disease have remained stable over the 10-year period from 1995 to 2005 .
Estimated Healthcare Costs Related To Pd In The Us
The combined direct and indirect cost of Parkinsons, including treatment, social security payments and lost income, is estimated to be nearly $52 billion per year in the United States alone.
Medications alone cost an average of $2,500 a year and therapeutic surgery can cost up to $100,000 per person.
Worldwide Parkinsons Disease Statistics
Worldwide Parkinsons Disease Statistics
WORLD PREVALENCE
There are up to 10 million or more people in the world who have Parkinson’s Disease. There may be many more than this due to the incompleteness and inconsistencies of prevalence studies, no precise definition of Parkinson’s Disease, and so many people with Parkinson’s Disease not being diagnosed. The actual number of people in the world with Parkinson’s Disease is not known.
WORLD’S HIGHEST PREVALENCE
China is the country with the world’s greatest number of people with Parkinson’s Disease. In China there are probably more than 1.7 million people who have Parkinson’s Disease.
The world’s highest prevalence of Parkinson’s Disease is along the River Nile in Egypt, south of Cairo, amongst illiterate Egyptians in rural areas. They have a prevalence rate of 1,103 per 100,000. The high prevalence of Parkinson’s Disease is probably related to poverty rather than illiteracy. In some of the villages south of Cairo there are only mud roads and open sewers. Egypt is the country with the third highest prevalence of Parkinson’s Disease in the world.
The world’s next highest prevalence of Parkinson’s Disease is in the vicinities of ferromanganese plants near Brescia in Italy, with 407 people per 100,000 population. Manganese concentrations in settled dust were found to be significantly higher in the surroundings and downwind from the ferromanganese plants. In high concentrations, manganese is a known cause of Parkinson’s Disease.
Mortality From Parkinsons Disease
With treatment, the life expectancy of people with PD is similar to that of the general population. However, dementia seems to largely impact life expectancy among people with PD, and about 50 percent to 80 percent of people with PD develop dementia in their lifetime. Risk factors for mortality include later age of onset, male sex, severity of motor impairment, presence of psychotic symptoms, and dementia. Early detection of disease, prevention of motor symptom progression, and treatment of dementia can increase life expectancy.8,9
Engage with the community by asking a , telling your , or participating in a .
Patient Education And Education Of Pd In General
Like other chronic diseases such as diabetes, hypertension and cerebral vascular disease, it is important to educate physicians and patients for PD management. Health education is an effective way for local physician and patients to acquire knowledge of PD, which could improve the early diagnosis and management of PD . Tan et al. performed a study on awareness status of PD among elderly veterans in Beijing. In this study, 80.3% subjects heard the name of PD. As for the prevention knowledge, the awareness rate was 62.1%. In those veterans with prevention knowledge of PD, 52.7% of them learned from media, 72.1% of them learned from word of mouth, and only 11.8% learned from health care professionals . Thanks to communication tools through smartphone, such as Weibo and WeChat, it is much easier to perform patient education. Personal health education and health education to caregivers are effective and need more attention .
Who Is Affected By Parkinsons Disease
Several studies have found that the incidence of PD is much more common in than .2,4 One estimate found that PD affects about 50 percent more men than women.2 The reasons for the differences in men and women with PD are unclear, although some suggested explanations are the protective effect of estrogen in women, the higher rate of minor head trauma and exposure to occupational toxins in men, and genetic susceptibility genes on the sex chromosomes.4
People with a close family member with Parkinsons have a small increased risk of developing the disease. About 15 percent to 25 percent of people with PD have a known relative with the disease.2
It is estimated that about 10 million people worldwide are living with PD. The incidence of the disease is higher in industrialized countries.3,4
The incidence of PD increases with age: while PD affects 1 percent of the population over the age of 60, this increases to 5 percent of the population over the age of 85.1
Approximately 5 percent of people with PD are diagnosed before the age of 60.1
Urban areas have a higher prevalence and incidence of PD.5
New Parkinsons Disease Prevalence Study
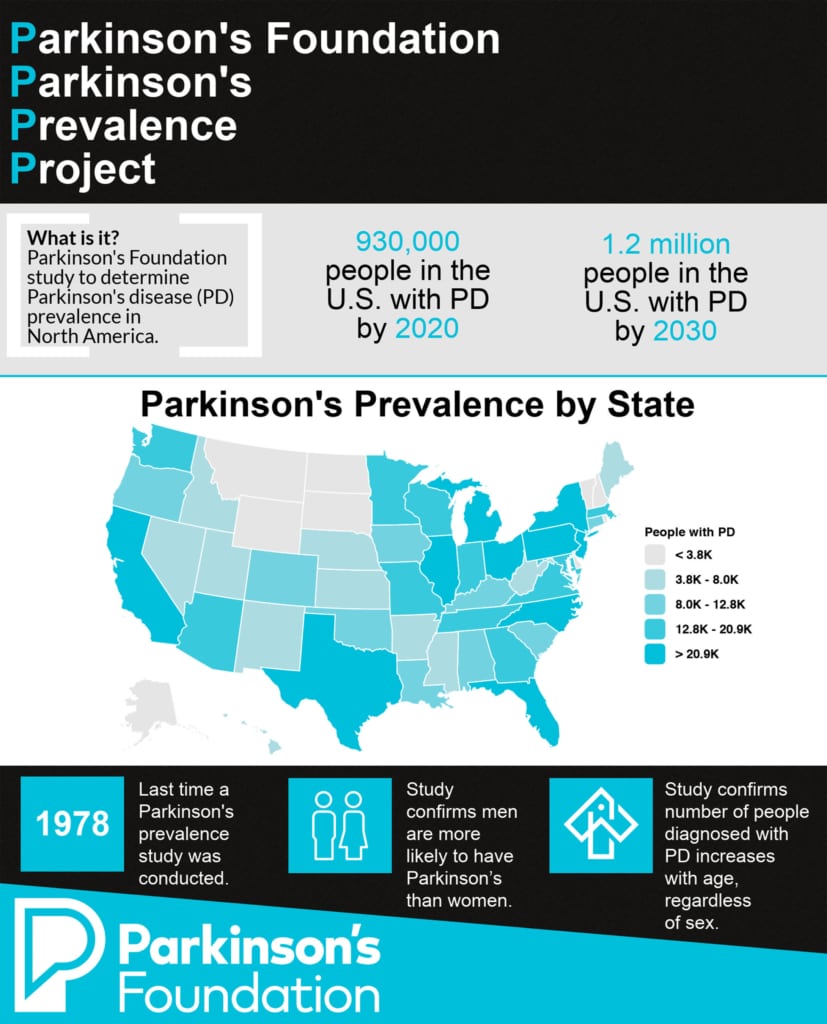
Trying to estimate the number of people living with Parkinsons disease in North America is extremely important but notoriously difficult. It is critical to know the prevalence of PD because it informs lawmakers who make decisions concerning allocation of research funds about the true impact of the disease, and it also informs public health officials who need to plan for the growing PD population. The difficulties in ascertaining this number however, lie in trying to capture every case of a highly varied disease, on a continent without a centralized medical system and without uniformity in medical care.
A newly published study on the prevalence of PD is the most comprehensive study yet to tackle this question. The study was conducted with the support of Parkinsons Foundation and consisted of five separate studies to determine the local prevalence one each in Minnesota, Hawaii, and Ontario, Canada, and two in California. The data from each study was then analyzed together and compared to US Medicare data. According to this strategy, the estimated prevalence of PD in people 45 and older is 572 per 100,000. Using the last available US Census Bureau data from 2010, the overall prevalence of PD across North America in 2010 was calculated to be 680,000. Population projections were then used to extrapolate the prevalence for the year 2020, calculated to be 930,000, and for the year 2030, calculated to be 1,238,000.
The State Of Parkinsons Disease In Finland
PARKINSONS Disease is not a new disease, nor a new challenge. In spite of the diseases many unknowns, the Finnish health system and its stakeholders are becoming more effective in supporting individuals living with Parkinsons as well as leading innovative research to find a cure.
More than 15,000 people in Finland live with the disease, which has symptoms ranging from a slight tremor to loss of voice to depression and physical incapacitation. The composition and intensity of symptoms are as individual as the patients are, making treatment and research challenging.
Supporting Parkinsons patients
One of the greatest challenges faced today by the Parkinsons community is awareness. Much remains to be done to better educate and inform the public and medical practitioners about the process of diagnosing Parkinsons as well as the options for treatment and care. In the same vein, educating doctors about the importance of referring patients to neurologists and movement disorder specialists is crucial to providing effective care for each individual patient.
…
Matthew MitchellLEHTIKUVA / HEIKKI SAUKKOMAA
|
Only a fraction of the articles are available to public, please subscribe to be able to read whole article on the digital paper. |

