How Do Doctors Diagnose Parkinsonism
No single test exists for doctors to diagnose Parkinsonism.
A doctor will start by taking a persons health history and review their current symptoms. They will ask for a medication list to determine if any medicines could be causing the symptoms.
A doctor will likely also order blood testing to check for underlying potential causes, such as thyroid or liver problems. A doctor will also order imaging scans to examine the brain and body for other causes, such as a brain tumor.
Doctors can perform a test that tracks the movement of dopamine in the brain. This is known as the DaT-SPECT test.
The test uses radioactive markers designed to track dopamine in the brain. This allows a doctor to watch the release of dopamine in a persons brain and identify the areas of the brain that do or do not receive it.
Because Parkinsonism does not respond to typical treatments and can have a variety of symptoms, doctors can have difficulty coming to a quick diagnosis. It may take time for doctors to rule out other conditions and begin to make treatment recommendations.
Other Reasons For Cognitive Symptoms
Besides PD, there are other important causes of cognitive dysfunction to keep in mind. Medical illnesses such as thyroid disease or vitamin B12 deficiency can cause cognitive symptoms. Urinary tract infections or pneumonia can acutely cause confusion or hallucinations. In these settings, the cognitive symptoms are generally reversible after the infection or medical condition is treated. One should be aware that some medications for pain or bladder problems may cause sedation/sleepiness or confusion, and, thereby, impair cognitive function.
The Connection Between Pd And Drug
In addition to potentially causing parkinsonism in the general population, these medications should definitely be avoided in people who have parkinsonism from other causes, such as PD. APDA has created a list of Medications to be Avoided or Used With Caution in Parkinsons Disease. It is important to note that there are anti-psychotics and anti-nausea medications which do;not;cause parkinsonism and can be used safely by people with PD.
Sometimes, a person without a diagnosis of PD is prescribed a medication which leads to a side effect of drug-induced parkinsonism. The prescribing physician may stop the new medication, but the parkinsonism does not resolve. The patient remains off the medication with continuing symptoms, and eventually is given a diagnosis of PD. In this scenario, that person most likely had dopamine depletion in the brain which had not yet manifested as a clinical symptom. The prescription medication that blocked the dopamine receptor, was the proverbial straw that broke the camels back, inducing the full-fledged symptoms of dopamine depletion and revealing that the person did in fact have PD.
The differences of PD vs drug-induced parkinsonism
There are key differences to note between parkinsonism from PD and parkinsonism as a side effect of medication.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Antipsychotics Are Dopamine Blocking Drugs
A few people develop Parkinsons disease like symptoms after they undergo treatment with specific type of medicines. This type of medicine refers to drug-induced Parkinsonism or DIP i.e. secondary type of Parkinsonism. Specific medicines, including antipsychotics may make the symptoms worse in patients, who already suffer from Parkinsons disease.
Almost every medicine responsible to create blockage of dopamine in humans may create symptoms related to Parkinsons disease. Dopamine refers to a brain chemical that mainly controls body movements. Antipsychotics are common types of dopamine blocking drugs, which are useful in the treatment of specific mental illnesses or nausea in its severe form. In less common cases, calcium channel blockers medicines may result in drug induced Parkinsonism. These drugs are helpful in the treatment of high blood pressure, chest pain as well as irregular heart beat rate.
Diagnosis Of Dip And The Role Of Dat Imaging
The clinical diagnostic criteria for DIP are defined as 1) the presence of parkinsonism, 2) no history of parkinsonism before the use of the offending drug, and 3) onset of parkinsonian symptoms during use of the offending drug. Since asymmetrical rest tremors are common in many DIP patients and symptoms persist or progress after cessation of the offending drug, patients clinically diagnosed with DIP may include individuals in the preclinical stage of PD whose symptoms were unmasked by the drug.,,,
DATs are presynaptic proteins in the membrane on terminals of dopaminergic neurons. They take up dopamine from the synaptic cleft projections that extend from the substantia nigra to the striatum. These transporters control dopaminergic transmission by spatial and temporal buffering, rendering the molecule an imaging target in diseases affecting the dopaminergic nigrostriatal pathway. Single-photon-emission computed tomography and positron-emission tomography scans are available using several DAT ligands., SPECT radioligands include 123I-N-3-fluoropropyl-2-carbomethoxy-3-nortropane , 123I-ioflupane, DaTSCAN, and 123I-2-carbomethoxy-3-tropane . PET scans may be superior to SPECT for imaging DATs, in that the lower energy of positrons provides higher resolution, resulting in better image quality with widespread clinical applications. However, most DAT imaging studies, including those in patients with DIP, have utilized SPECT.,-
Recommended Reading: Parkinson’s Ribbon Color
Myth : Deep Brain Stimulation Is Experimental Therapy
Fact: Deep brain stimulation, or DBS, is a procedure in which doctors place electrodes in the brain at the point when medications are less effective in masking motor symptoms, such as tremor, stiffness and slowness of movement.
While it may sound frightening and futuristic, its been around and successfully used for decades. DBS works very similarly to a pacemaker, except the wire is in the brain, not in the heart. Its been a standard procedure for the past two decades.
What Are Home Remedies For Parkinson’s Disease
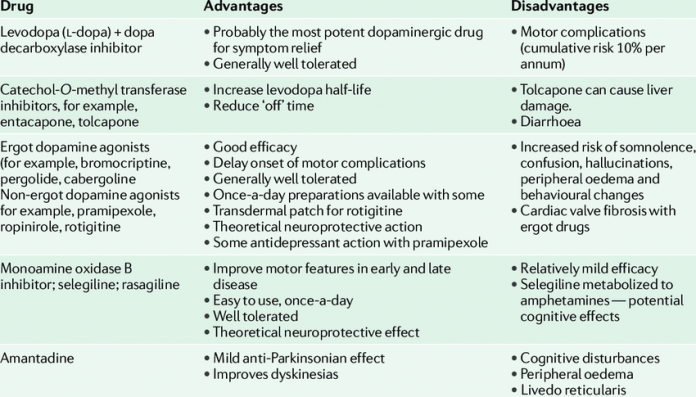
Treatment for Parkinson’s disease may include medications, surgery, gene therapy, other therapies, or a combination of these.
The decision to care for a family member with Parkinson’s disease is very complex.
Some patients’ treatment will include or begin with medications to “protect” the neurons that make dopamine. Although “neuroprotective agents” protect cells in tissue cultures, it is not clear if they have the same effect on patients’ neurons. These medications are monoamine oxidase B inhibitors .
Occasionally, some doctors may prescribe amantadine for short-term treatment of early Parkinson’s disease symptoms or use the medication in conjunction with carbidopa-levodopa treatment.
Patients usually will be given medications at the lowest effective dose. Over time, the various medication effects often diminish. To minimize medication side effects, the doctor may slowly increase dosages. Side effects involving problems with thinking are relatively common in older patients.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Side Effects And Problems With Levodopa
In the early days of taking levodopa, you may feel sickness or nausea. In most people this will pass as your body adjusts to the medication.
Overtime as Parkinsons progresses the levodopa dose will need to be adjusted. Many people will become more aware that symptoms sometimes return between doses of medication. This is called wearing off and is a sign your dose needs to be adjusted.
As levodopa is absorbed through the gut, constipation or other stomach problems may impact on uptake of the medication. In some people who have had Parkinsons for sometime extra involuntary movements can occur. Your neurologist will be able to help adjust medications to minimise dyskinesia.
Other side effects may include:
- Confusion
- Psychological changes
- Sleepiness, fainting or dizziness
Side effects of levodopa can sometimes be improved by changing your dose, the form of the drug or how often you take it. If this doesnt work, other types of drug may be combined with levodopa.
Speak to your GP or specialist about the right treatment for you.
Anesthetic Drugs May Interact With Medications Used For Parkinsons Disease
Lorri A. Lee, MD; Tricia A. Meyer, PharmD, MS, FASHP
An estimated one million people in the United States have been diagnosed with Parkinsons Disease making it one of the most common neurological disorders in patients. This number is estimated to double in the next 30 years as PD is associated with increasing age. PD patients have a deficiency of dopamine in their brain and many of their medications are used to increase this neurotransmitter. They are frequently very sensitive to missing even one dose of their Parkinson medications and may exhibit increased rigidity, loss of balance, agitation, and confusion if their dosing schedule is delayed. Neuroleptic malignant syndrome or parkinsonism-hyperpyrexia syndrome can develop if their medications are held too long or as a result of serious infection.1 Many drugs used in the perioperative period, such as metoclopramide, butyrophenones , and phenothiazines have anti-dopaminergic activity that can worsen the symptoms of PD.
PD patients may be prescribed selective MAOI-B medications such as selegiline and rasagiline that inhibit metabolism of dopamine. Though caution is still advised, several studies have demonstrated that the risk of serotonin syndrome with these selective MAOI-B drugs is extremely low, even in combination with serotonergic antidepressants.
The authors have no conflicts of interest to declare for this article.
Patients With Parkinsons Disease Are At Risk For Carpal Tunnel Syndrome
Recommended Reading: Does Parkinson’s Disease Cause Death
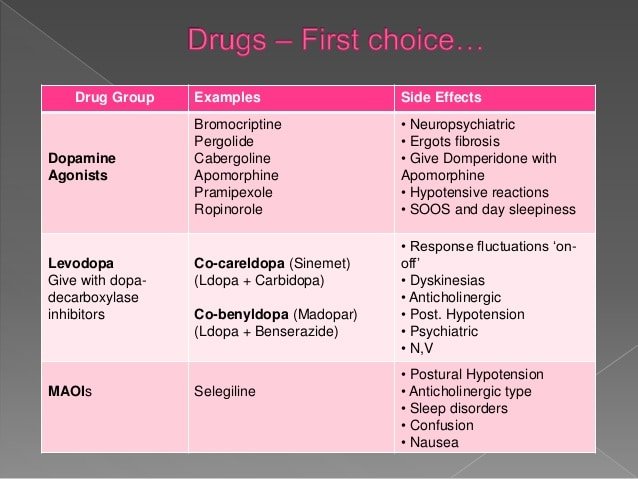
Treatments For Parkinsons And Parkinsonism
Parkinsons disease is a movement disorder that causes motor symptoms such as stiffness, bradykinesia , resting tremor, and postural instability that can lead to falls. In people who have symptoms of Parkinsons, but the cause is unknown, the condition may be referred to as parkinsonism. There is at present no cure for Parkinsons, and no treatments have been proven to change the course of the disease. However, many people with Parkinsons can improve their symptoms and quality of life with effective treatment options.
Symptoms and severity can vary widely between individuals with parkinsonism. There is no standard treatment for Parkinsons. Guidelines for Parkinsons treatments are based on what symptoms a person has, the severity of the symptoms, how long they have had Parkinsons, which type and stage of Parkinsons they have, tolerance of side effects, the age of the person, and any other health conditions they have or medications they use. Some treatments are highly effective for one type of Parkinsons, but ineffective for others. In most people, medications gradually lose their effectiveness as the disease progresses.
Can Drug Induced Parkinsonism Be Prevented
Although there is no surety in the prevention of drug-induced parkinsons disease, but efforts may be made to check the dosage of drugs so prescribed-
Be Cautious with Antipsychotics: The patient or in some cases the caregiver should make sure that antipsychotic drugs are given at their least effective dosage.
Inform the Doctor: The doctor should be informed well before in case the patient already has symptoms of Parkinsons disease so that they do not appear to get worse with the starting of some prescribed drugs.
Abrupt Stoppage of Medicine: It is never a wise decision to stop taking a medicine by oneself. It is important to talk to the doctor in case of any concerns.
Also Check: Parkinsons Double Vision
Impulse Control Disorders Up Close And Personal
Michael J. Fox and people from his foundation answer questions about Parkinsons in a Google Hangout
Interestingly, Daniel Weintraub, MD, associate professor of psychiatry and Neurology at the Perelman School of Medicine at the University of Pennsylvania, says that ICDs are most likely to manifest in men as gambling and hyper sexuality, whereas in women it expresses as shopping and overeating.
Needless to say, these compulsive behaviors can have serious repercussions.
Ive seen marriages break up and lives ruined as a result of dopamine agonists, says Howard Weiss, director of the Parkinsons Disease and Movement Disorder Programs at the LifeBridge Health Brain & Spine Institute in Baltimore. Ive had at least three patients who have lost their homes because of bankruptcy after taking the drugs. It sounds like a joke, but its not.
Whats more, ICDs are shockingly common. Weintraub cites a study that demonstrated about 14% of people with PD experience 1of 4 of the typical ICD behaviors. He says his own guess is more like 17% to 20%, perhaps even 25%.
The reason that ICD might be even more prevalent than statistics show lies in the fact that they can easily slip under a doctors radar. Many patients arent forthcoming about the symptoms, and doctors may not take the time to ask the right questions.
Most doctors have no idea how to diagnose ICDs, says Weiss, and most patients are in the dark.
Sleep Attacks
Gambling
DAWS Risks
Who Are At Risk Of Developing Drug Included Parkinsonism

Some patients may be at a higher risk of developing medication-induced Parkinson
ism than others. Some of the risks include-
Women: Women are seen to be two times as much at risk of having drug inducing Parkinsons disease than men.
AIDS Patients: People with AIDS are at a higher risk.
Family History: Patients having a family history Parkinsons disease are at a higher risk of having drug induced Parkinsonism.
Elderly: Since elder people are usually on multiple medicines, they are at risk of having drug induced Parkinsonism.
You May Like: Turapã¼r Reviews
Pros & Cons To Treating Mit
Your doctor can help you determine if the medication regimen is right for you. The doctor is able to evaluate if there are alternative drugs, formulations, or dose adjustments that can help to better manage your medical condition without the presence of tremor.
Some people can eliminate drugs that are inducing tremor. Yet there can be trade-offs between having side effects and benefitting from what could be life-saving treatment with immunosuppressant drugs to prevent transplant rejection.
Make sure to let your doctor know if you are experiencing tremor or other side effects from the medications you take, whether for Parkinsons or other conditions. Do not stop taking any medications without first discussing what you are experiencing with your medical team.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Also Check: What Does Parkinson’s Smell Like
Myth : Aside From Medication There Isnt Much You Can Do
Fact: This it is what it is; theres nothing I can do to help myself myth is counterproductive. There is a lot you can do chiefly, keeping as active as you can. A recent study found that patients with Parkinsons who took part in weekly, hourlong exercise sessions were able to do more in their daily lives than those who did not.
Parkinsonism Falls And Fracture Risk
All forms of parkinsonism, both PD and DIP, have implications for bone health. A 2014 meta-analysis on PD and fracture risk concludes that PD increases the risk of fracture.4
Given that the symptoms of parkinsonism affect balance, motor skills, gait, and the bodys ability to control movement, it is no surprise that people with PD are more likely to experience a fall than people without PD. Here is an excerpt from a 2016 study comparing the incidence of falls and fracture in PD patients:
It is estimated that 60.5% of patients with PD experience at least one fall and 39% have recurrent falls. The high frequency of falls consequently contributes to the increased risk for fractures in PD patients, which has been estimated to be approximately two times the risk in healthy controls. It has been estimated that 76% of falls in PD patients require health care services and 33% result in fractures. Falls and fractures may result in a series of unfavorable outcomes, such as disabilities and death. Furthermore, among PD patients with fractures, the mortality rate is approximately 10.6%.5
All too often, doctors prescribe these drugs without appropriate consideration of this risk. This excerpt from a study on DIP clarifies the danger of accepting a prescription of an unnecessary or inappropriate prescription drug:
Shockingly, the drugs that cause DIP are still being prescribed. This yet one more example further proving that the FDAs drug approval process is useless.
Synopsis
Read Also: When Was Muhammad Ali Diagnosed With Parkinson’s Disease
For Your Good Health: Can Lyme Disease Lead To Parkinsons
DEAR DOCTOR. ROACH: Can Lyme Disease Put A Person Into Parkinsons Disease? I tested positive for Lyme I had the rash, a fever, and a terrible headache. After a month on doxycycline, my left arm started shaking and my neurologist diagnosed me with Parkinsons. The doctor said it had nothing to do with Lyme disease. What is your opinion? SM
ANSWER: I can absolutely understand why you suspect that the neurologist might be wrong. Chance seems too much to believe. However, I think your neurologist is probably right. The different types of neurological complications of Lyme disease are many.
The most common are any combination of meningitis symptoms ; Disorders of the cranial nerves ; and damage to peripheral nerves causing pain and weakness or numbness, often similar to sciatica .
A detailed neurological exam by a neurologist would look for signs of Parkinsons disease not just the tremors you described, but muscle stiffness and gait changes. These would be very unusual in Lyme disease. I found cases that resembled some aspects of Parkinsons disease, but they improved with treatment.
Its possible that the stress of Lyme disease hastened the onset of Parkinsons disease you were meant to be. I say your neurologist is probably right because what Ive found the lack of data to show a correlation doesnt mean there isnt a correlation, and it is possible that time can prove the Lyme -Borreliosis related to Parkinsons. However, I think it is unlikely.