Symptoms Of Parkinsons Disease
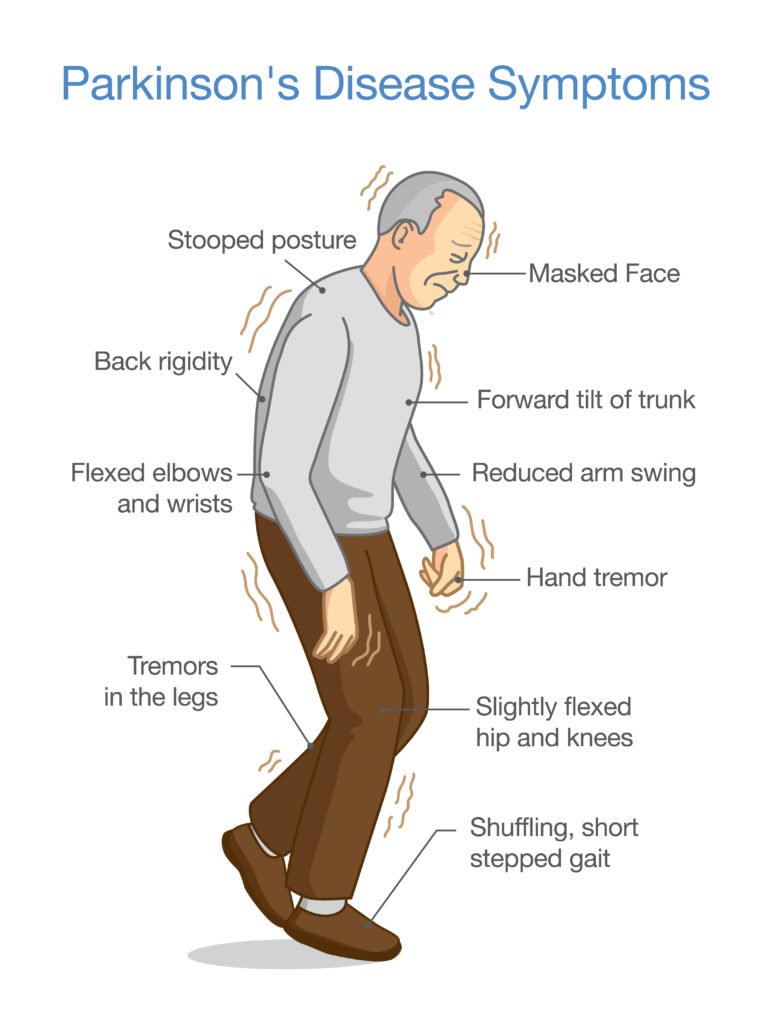
Parkinson’s disease has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Stiffness of the limbs and trunk
- Slowness of movement
- Impaired balance and coordination, sometimes leading to falls
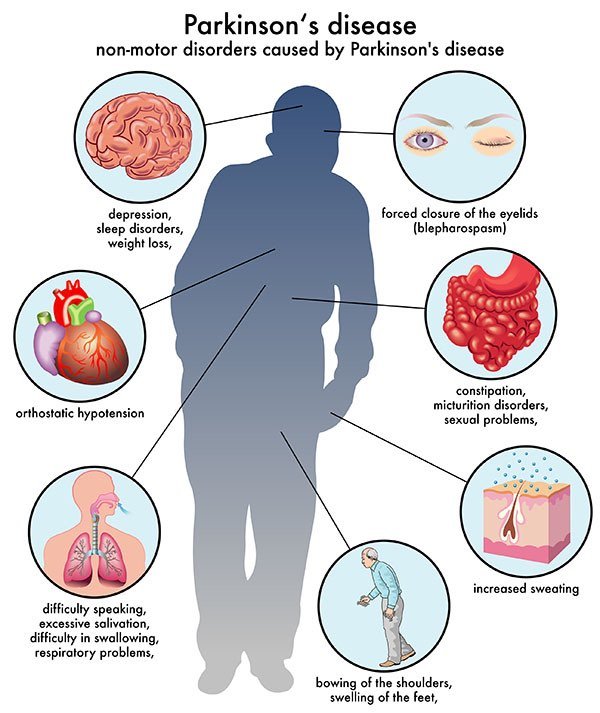
Other symptoms may include depression and other emotional changes; difficulty swallowing, chewing, and speaking; urinary problems or constipation; skin problems; and sleep disruptions.
Symptoms of Parkinsons and the rate of progression differ among individuals. Sometimes people dismiss early symptoms of Parkinson’s as the effects of normal aging. In most cases, there are no medical tests to definitively detect the disease, so it can be difficult to diagnose accurately.
Early symptoms of Parkinson’s disease are subtle and occur gradually. For example, affected people may feel mild tremors or have difficulty getting out of a chair. They may notice that they speak too softly, or that their handwriting is slow and looks cramped or small. Friends or family members may be the first to notice changes in someone with early Parkinson’s. They may see that the person’s face lacks expression and animation, or that the person does not move an arm or leg normally.
People with Parkinson’s often develop a parkinsonian gait that includes a tendency to lean forward, small quick steps as if hurrying forward, and reduced swinging of the arms. They also may have trouble initiating or continuing movement.
Parkinson’s Disease Symptoms Everyone Should Know
Parkinsons disease symptoms can include tremor and trouble with movement, along with emotional and cognitive changes.
Parkinson’s disease symptoms can vary significantly from person to person. Some people may have range of motor symptoms, like tremor, stiffness, and slow movements. Others may also experience the non-motor symptoms of Parkinson’s disease, such as anxiety, cognitive changes, and loss of smell.
It has to do with a chemical messenger known as dopamine, which plays a role in the brain’s ability to control movement, coordination, and emotional responses. In Parkinson’s disease, the brain cells that produce dopamine either stop doing their job or they die out, resulting in both motor and non-motor symptoms. ; It’s not always easy to tell if someone you care about has Parkinson’s disease. Let’s take a closer look at the symptoms of the disease and signs that someone should make an appointment with their doctor.
Extended Data Fig 1 Epec Infection Results In The Selective Degradation Of Mitochondrial Proteins
RAW 264.7 macrophages were either infected with EPEC at a multiplicity of infection of 1 for 1, 2, 4 or 6;h or treated with 20;µM CCCP for 8 or 24;h alongside control cells. Total cell lysates were collected for all conditions, quantified, separated via SDSPAGE, and probed for mitochondrial markers;and LC3 via western blot. Data are representative of two independent experiments.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Contact Our Information And Referral Helpline
The Parkinson Canada Information and Referral Helpline is a toll-free Canada-wide number for people living with Parkinsons, their caregivers and health care professionals. We provide free and confidential non-medical information and referral services. When you have questions or need assistance, our information and referral staff help connect you with resources and community programs and services that can help you. We provide help by phone or email, Monday to Friday, 9:00 a.m. 5:00 p.m. ET.
What Are Atypical Parkinsonian Disorders
Atypical Parkinsonian disorders are progressive diseases that present with some of the signs and symptoms of Parkinsons disease, but that generally do not respond well to drug treatment with levodopa. They are associated with abnormal protein buildup within brain cells.
The term refers to several conditions, each affecting particular parts of the brain and showing a characteristic course:
- Dementia with Lewy bodies, characterized by an abnormal accumulation of alpha-synuclein protein in brain cells
- Progressive supranuclear palsy,; involving tau protein buildup affecting the frontal lobes, brainstem, cerebellum and substantia nigra
- Multiple system atrophy, another synucleinopathy that affects the autonomic nervous system , substantia nigra and at times the cerebellum
- Corticobasal syndrome, a rare tauopathy that typically affects one side of the body more than the other and makes it difficult for patients to see and navigate through space
Also Check: Can Parkinson’s Run In The Family
What Are The Symptoms Of Parkinsons Disease
According to the Public Health Agency of Canada, an estimated 84,000 Canadians aged 40 or older have been diagnosed with Parkinsons disease, a disorder that most often occurs after age 50, and is more likely to affect men than women.
This neurodegenerative disease can start with small signs, and then get progressively worse, eventually causing trouble with movement, rigidity, stiffness, and other symptoms.;One of the most well-known signs and symptoms of Parkinsons disease are tremors or shaking.
About 70 per cent of people with the disease experience a resting tremor, and it can become more noticeable during stress or excitement.;A resting tremor occurs even when a person isnt moving; it might be a slight shake in your finger, thumb, hand, chin, lip, or lips when your body is at rest and your muscles are relaxed.
These tremors are one of the most common symptoms and often tip people off to the disease, but when Parkinsons patients think back, they sometimes realize they experienced other symptoms of the disease before the tremors began. Here are the ones you should know.
Managing Depression In Parkinsons Disease
People with Parkinsons, family members and caregivers may not always recognize the signs of depression and anxiety. If you are experiencing depression as a symptom of Parkinsons, it is important to know it can be treated.
Here are some suggestions:
- For information and support on living well with Parkinsons disease, contact our Information and Referral line.
- As much as possible, remain socially engaged and physically active. Resist the urge to isolate yourself.
- You may want to consult a psychologist and there are medications that help relieve depression in people with Parkinsons, including nortriptyline and citalopram .
Read Also: Can Parkinson’s Run In The Family
Movement Disorders Similar To Parkinsons
Conditions causing excess movement or decreased movement that are sometimes associated with Parkinson’s disease-like symptoms include:
What Movement Disorder Could I Have?
When making a Parkinson’s diagnosis, your doctor will review your medical history and symptoms, perform a careful neurological exam, and, if necessary, carry out further tests to rule out other movement disorders.
Your symptoms may be caused by a movement disorder other than Parkinson’s disease if:
- You display Parkinson’s disease symptoms and features that are characteristic of an additional movement disorder.
- The results of a brain imaging study or laboratory test, such as a blood test, confirm the presence of another movement disorder.
- Your symptoms do not respond to Parkinson’s disease medication.
Because movement disorders are not all treated the same way, it is important to get a proper diagnosis as early as possible so you can formulate the right treatment plan with your doctor.
What Are The Primary Motor Symptoms Of Parkinsons Disease
There are four primary motor symptoms of Parkinsons disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinsons.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinsons disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinsons disease has a tremor, nor is a tremor proof of Parkinsons. If you suspect Parkinsons, see a neurologist or movement disorders specialist.
Tremors
Rigidity
Bradykinesia
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
Read Also: Parkinson Risk Factors
Extended Data Fig 8 C
Brain and spinal cord tissue were assessed for haematopoietic cells in both control and infected wild-type and Pink1/;mice. a, b, Absolute number of monocytes or T cells at 13 and 28;d.p.i. were calculated using true count beads. Data pooled from two independent experiments. Data are mean;±;s.e.m.
Is There A Link
Some people have MS and Parkinsonâs, but it could be a coincidence.
Research suggests that the damage that MS causes to your brain can lead some people to develop Parkinsonâs later on.
If you have MS, your immune system triggers ongoing inflammation. This can create lesions in your brain that cause Parkinsonâs disease. If lesions form in certain spots in your brain, they can affect how it makes dopamine.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How Is A Diagnosis Made
Because other conditions and medications mimic the symptoms of PD, getting an accurate diagnosis from a physician is important. No single test can confirm a diagnosis of PD, because the symptoms vary from person to person. A thorough history and physical exam should be enough for a diagnosis to be made. Other conditions that have Parkinsons-like symptoms include Parkinsons plus, essential tremor, progressive supranuclear palsy, multi-system atrophy, dystonia, and normal pressure hydrocephalus.
Environmental Factors And Exposures
Exposure to pesticides and a history of head injury have each been linked with PD, but the risks are modest. Never having smoked cigarettes, and never drinking caffeinated beverages, are also associated with small increases in risk of developing PD.
Low concentrations of urate in the blood is associated with an increased risk of PD.
Drug-induced parkinsonism
Different medical drugs have been implicated in cases of parkinsonism. Drug-induced parkinsonism is normally reversible by stopping the offending agent. Drugs include:
Don’t Miss: Does Parkinson’s Cause Memory Issues
Realities Of Living With Parkinsons
Parkinsons disease is unpredictable, so it can be difficult to make any plansbig or smallwithout worrying you have to cancel at the last minute. Living with the painful symptoms, both physical and mental, can be draining.
Daily tasks may require a lot of energy for someone with Parkinson’s disease to complete or are taken away altogether. For example, a person without a chronic disease can drive to the grocery store, come home and do laundry, cook dinner for their family, and still have time to relax at the end of the day. However, a person with Parkinson’s will have to put much more effort and time into each task and may not be able to drive at all.
As the disease progresses to its later stages, many people are forced to give up their independence and autonomy when it comes to taking care of themselves. This makes coping with a diagnosis and the disease incredibly difficult.
However, with the right treatments, you can slow disease progression and remain independent for as long as possible.
Tips For Living With Parkinsons Disease
The challenges of living with Parkinson’s disease often go misunderstood. Therefore, if you’re living with Parkinson’s disease, it’s important to educate yourself about the condition, so you know what to expect and when to ask for help. Here are some tips to help you live better with Parkinsons disease:
- Stick to your medication schedule write it down or keep a diary if you have to
- Establish a daily routine to keep your medications, mealtimes and sleep cycles on track
- Relieve stress practice yoga, meditation or mindfulness to keep stress at bay
- Get regular exercise to improve your balance, flexibility and mental health
- Maintain a healthy, balanced diet thats high in fiber and low in processed foods
- Follow your bodys signals take a break or rest if you feel low on energy
- Establish a rapport with a specialist and attend regular medical appointments
- Make sure you have a support system whether thats your family, a group of friends or neighbors or a Parkinsons support group
- Dont be afraid to ask for help from your loved ones or carers
- Take up a hobby that takes your mind off your symptoms, such as painting, journaling or gardening
Living with Parkinsons disease comes with many challenges. If you have just been diagnosed with PD or you know someone who has, its important to educate yourself about Parkinsons so you know what to expect. If you have any questions, you can consult your doctor or call the National Parkinsons Foundation helpline at 1-800-4PD-INFO .
Also Check: Severe Hip Pain Parkinson’s
Extended Data Fig 2 C Rodentium Induces Mild Colonic Pathology And Inflammation In Both Wild
a, The distal colon was collected at 13;d.p.i. and assessed for colon-associated C. rodentium in infected wild-type and Pink1/ mice via serial dilution and plating on MacConkey agar. Data representative of two independent experiments. b, Analysis of colonic epithelial hyperplasia via measurement of crypt heights from haematoxylin and eosin -stained colon sections. Data represents individual crypt measurements from five wild-type mice and six Pink1/ mice. Data representative of two independent experiments. c, Tissue pathology scores from H&E-stained distal colon sections from infected wild-type and Pink1/ mice. d, e, Protein quantification of faecal S100A8/A9 and lipocalin-2; from control and infected wild-type and Pink1/ mice. Data pooled from two independent experiments. P values were determined by two-tailed MannWhitney unpaired t-test at a 95% confidence interval , two-way ANOVA at a 95% confidence interval , or two-way ANOVA at a 95% confidence interval with Tukeys multiple comparisons test. Data are mean;±;s.e.m.
Stiffness And Slowed Movements
Watch for an abnormal stiffness in your joints along with muscle weakness that doesnt go away and makes everyday tasks like walking, teeth brushing, buttoning shirts, or cutting food difficult. If you no longer swing your arms when walking, your feet feel stuck to the floor , or people comment that you look stiff when you havent been injured, the National Parkinson Foundation suggests seeing a doctor.
Learn more about these types of leg pain.
Don’t Miss: Is Parkinson’s Genetically Inherited
Living With Parkinsons Disease: What You Should Know
Living with Parkinson’s disease can be unpredictable and difficult for others to understand. Someone with PD may look normal from the outside but be suffering pain, fatigue, and depression on the inside.
Whether youve recently been diagnosed with PD or you know someone who has, heres what to expect from life with Parkinsons disease:
Pain is often unpredictable
People with PD say that it is hard to make plans because the pain can be so unpredictable. The physical symptoms of Parkinson’s disease can also be exhausting, so someone with PD may be able to socialize and live fairly normally on one day and not another.
Parkinson’s is more than a movement disorder.
Because tremor is the hallmark symptom of Parkinson’s disease, people may not understand the effects it can have on a person’s life. Patients often report that the non-motor symptoms of Parkinson’s such as depression, sleep disorders, fatigue and problems with memory are more debilitating than the movement-related symptoms.
Depression is common
Over 50% of people living with Parkinson’s disease will experience depression. This is thought to be due to the chemical changes that take place in the brain, as well as the physical and emotional impact of living with PD. ;Certain lifestyle changes, alternative therapies, and antidepressant medications can help relieve symptoms of depression.
Parkinsons disease is a progressive illness
Parkinson’s often leads to dementia.
Conditions Misdiagnosed As Parkinson’s Disease
Parkinsons disease, especially in its early stages when symptoms are mild, is not an easy disease to diagnose. The non-specific, and easily overlooked nature of the signs of Parkinsons make it difficult to spot, and unlike many illnesses, there is no one laboratory test or radiological exam that will provide a definitive diagnosis of Parkinsons disease.
Patients exhibiting Parkinsons-like symptoms may undergo blood and urine tests, or CT or MRI scans to exclude other conditions, but none of these will provide a diagnosis of Parkinsons disease. The best way to test for Parkinsons disease is to conduct a systemic neurological examination that includes tests to gauge a patients reflexes, muscle strength, coordination, balance, gait, and overall movement. Even so, according to information presented on The Michael J. Fox Foundation for Parkinsons Research, up to 25 percent of Parkinsons disease diagnoses are incorrect.
So, why is there confusion about diagnosing Parkinsons disease? The simple answer is that symptoms of Parkinsons disease are not clear cut, and therefore, it is easy to mistake them for other conditions, or to classify them as parkinsonian when they are not.
Here is a brief overview of the top ten conditions mistaken for Parkinsons disease:
Beyond those top three, there are other conditions that are often confused with Parkinsons disease, including:
Recommended Reading: What Color Represents Parkinson’s Disease
The Right Diagnosis Can Save Time
Because the symptoms of Parkinsons vary and often overlap other conditions, it is misdiagnosed up to 30% of the time, Dr. Fernandez says. Misdiagnosis is even more common in the early stages.
Patients;who dont know where to turn may make appointments with a rheumatologist, or an orthopaedic or heart specialist, and undergo MRIs, EMGs and other expensive tests.
But only a neurologist can distinguish Parkinsons from essential tremor, drug-induced Parkinsons and Parkinsons plus syndromes, he says.
If patients come to us with typical signs of Parkinsons, we dont need to order expensive tests, he says.
Instead, neurologists base their diagnosis on a detailed patient exam and medical history, along with other information from the patient, family members or caregivers.
Thats all stirred into the pot, he says. Sometimes we can diagnose Parkinsons with one visit. Other times, several follow-up visits are necessary.
What Are The Symptoms Of Atypical Parkinsonian Disorders
Like classic Parkinsons disease, atypical Parkinsonian disorders cause muscle stiffness, tremor, and problems with walking/balance and fine motor coordination.
Patients with atypical Parkinsonism often have some degree of difficulty speaking or swallowing, and drooling can be a problem. Psychiatric disturbances such as agitation, anxiety or depression may also be part of the clinical picture.
Dementia with Lewy bodies can cause changes in attention or alertness over hours or days, often with long periods of sleep during the day. Visual hallucinations typically of small animals or children, or moving shadows in the periphery of the visual field are common in DLB. DLB is second only to Alzheimers disease as a cause of dementia in the elderly, and it most commonly affects patients in their 60s.
Patients with progressive supranuclear palsy may have difficulties with eye movements, particularly when looking downward, and with balance when descending stairs, for instance. Backward falls are common and may occur during the early course of the disease. PSP is not usually associated with tremor, unlike Parkinsons disease.
Parkinson’s Disease and Movement Disorders Center
Also Check: Parkinson’s Ribbon
