Treatment For Genitourinary Dysfunctions
Unlike the motor symptoms of PD, genitourinary dysfunctions do not respond to levodopa therapy, and other treatments must be used. There are several medications that can help manage urinary difficulties, including Detrol® , Ditropan® , Enablex® , and Vesicare® . These medications work to block or reduce overactivity in the bladder. Treatments for sexual dysfunction include counseling or talk therapy, treating erectile dysfunction with Viagra® or Cialis® , and the use of lubricants in women.1,3-5
Urinary Issues In Advanced Parkinsons Disease
Urinary dysfunction and symptoms in PD are most commonly caused by overactivity of the detrusor muscle, or the muscle of the bladder, which contracts excessively despite the fact that it is not filled with urine. This causes an increased urge to urinate and/or an increased frequency of urination, which can be especially prominent at night. In advanced PD, this could culminate in urinary incontinence, or involuntary release of urine. Mobility issues which make getting to the bathroom slower and more cumbersome, compound the problem.
Always remember that people with advanced PD may have other medical problems that affect their urination such as an enlarged prostate. Make sure to have a complete evaluation before assuming that the problem is only related to PD. It is also essential to keep in mind that if changes in urination occur suddenly, there could be a urinary tract infection present.
Once other medical issues and urinary tract infection are ruled out, there are a number of approaches to the issue of urinary incontinence in a person with advanced PD:
Unfortunately, for some, the above available options may not be sufficient to effectively treat urinary incontinence in advanced PD. If this is the reality, it becomes extremely important to keep the skin dry with frequent changes of incontinence products to prevent skin breakdown and the potential development of skin infection.
Treating And Managing Bowel Problems
The first step in dealing with bowel disorders is to talk to your doctor. He or she will probably review your medication to see if this is a contributory factor. Whilst it is usually possible to control any difficulties with diet, fluid intake and exercise, your doctor, or Parkinsons nurse specialist if you have one, will be able to advise further, and may, for example, prescribe laxatives in severe cases of constipation. If you have any alarm features such as unintentional weight loss or rectal bleeding, then you may need to be referred for specialist assessment.
The following healthcare professionals can also advise on aspects of bowel care:
- A dietician will be able to advise on diet and fluid.
- A physiotherapist may be able to help with advice and abdominal exercises which will help in passing stools.
- A speech and language therapist can help with swallowing problems. They may be able to advise on ways of relaxing your throat, and give guidance on posture and exercises to help overcome any difficulties you have.
- An occupational therapist may also be able to suggest practical ways to overcome any difficulties you have with eating and drinking.
Read Also: How Many Kinds Of Parkinson Disease Are There
Parkinsons Disease And Parkinsonian Syndromes
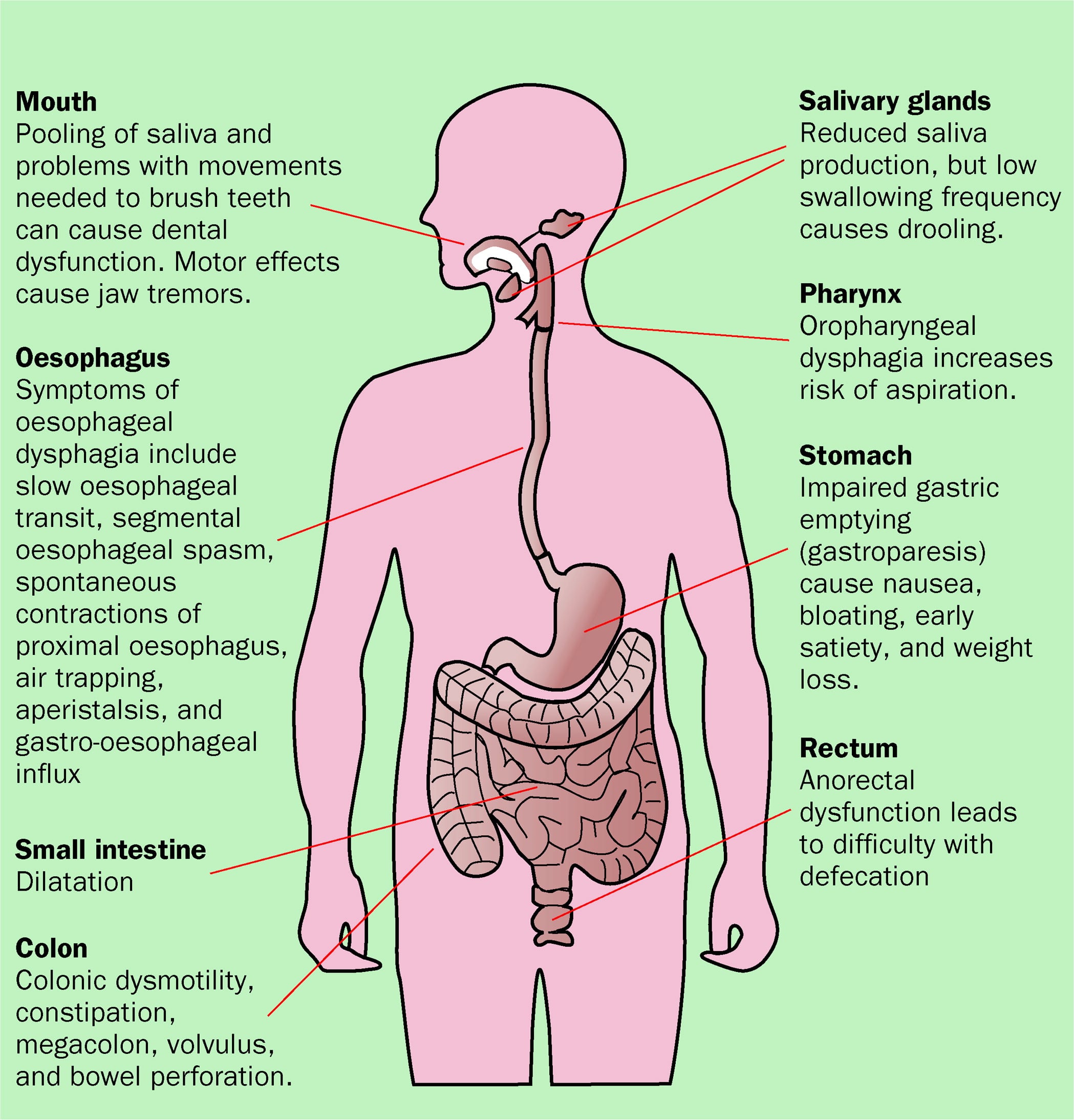
The majority of patients with PD or parkinsonian syndromes-in particular, multiple system atrophy -complains of gastrointestinal and pelvic organ dysfunction. Stocchi et al reported a similar occurrence of altered bowel frequency and defecation in PD and MSA patients. Gastrointestinal symptoms in PD include gastroparesis and constipation as a result of decreased bowel movement frequency and defecation difficulty. In all patients, these disorders became manifest or worsened after the onset of neurologic symptoms. The most striking features of bowel dysfunction in PD patients were constipation and difficulty in expulsion . The prevalence of constipation in PD patients is high: more than 50% suffer from moderate to severe constipation . PD patients are reported to have prolonged colorectal transit time and paradoxical contraction of the PR muscle on defecation . Difficulty in defecation is a very common symptom in PD, occurring in 67-94% of patients constipation is present in 29-77% of patients compared with 13% of age-matched controls . Singaram et al. reported a reduction of dopamine-containing neurons in immunostaining of biopsied submucosa and colonic musculature and the presence of Levy bodies in the myenteric plexus of the colon. These findings suggest that prolonged transit time and constipation in PD patients may depend not only on central but also on peripheral dopamine reduction in the colon.
Study Reveals Ibs Risk
BERLIN — Irritable bowel syndrome may be a more frequent symptom in Parkinson’s disease than constipation, researchers reported here.
In a case-control study, about a quarter of Parkinson’s patients had IBS compared with only 5% of healthy controls , according to Tuomas Mertsalmi, MD, of the University of Helsinki, and colleagues.
On the other hand, the prevalence of constipation was higher among Parkinson’s patients, but the difference from healthy controls wasn’t significant, they reported at the Movement Disorders Society meeting here.
“Gastrointestinal symptoms in Parkinson’s disease are more complex than just constipation,” Mertsalmi told MedPage Today. “Usually constipation is just seen as decrease bowel frequency, but it is also about straining during defecation, hard and lumpy stools, and diarrhea in these patients.”
Previous work has shown that the majority of patients with Parkinson’s suffer from gastrointestinal symptoms. About 70% have been estimated to have constipation, which is considered to be a premotor symptom of the disease and is one of the strongest risk factors for Parkinson’s, Mertsalmi said.
IBS is among the most common functional gastrointestinal disorders, and is characterized by symptoms of abdominal pain or discomfort, and alteration of bowel habits.
All patient with a pre-existing diagnosis of IBS were excluded, he added.
Disclosures
Also Check: Does Parkinson’s Lead To Dementia
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Causes Of Constipation In Parkinsons Disease
The ways in which Parkinsons disease can increase the risk of constipation include:
- lack of dopamine in the brain impairs control of muscle movement throughout the body. Bowel muscles can become slow and rigid
- uncoordinated bowel motions the bowel muscles may be weak and unable to contract, or they may clench instead of relaxing when trying to pass a motion
- eating problems dietary fibre containing insoluble fibre adds bulk to your bowel motions and can help prevent constipation. However, if a person with Parkinsons disease finds it difficult to chew or swallow, they may avoid eating fibrous foods
- drinking problems you need water to plump up the dietary fibre in your bowel motions. Swallowing difficulties may discourage a person with Parkinsons disease from drinking enough fluids
- sedentary lifestyle lack of exercise slows the passage of food through your intestines. Parkinsons disease reduces muscle control, so lack of exercise is common
- medications many different medications can cause constipation. Medications used in the treatment of Parkinsons disease may slow bowel movements or cause a decrease in appetite.
Recommended Reading: Finger Foods For Parkinsons
Read Also: Parkinson’s Disease And Spinal Stenosis
How Does Parkinson’s Affect The Bowel
Two out of three people with Parkinson’s disease suffer from constipation, and the symptom can occur long before the diagnosis is made. Constipation is one of the most common non-motor symptoms of this condition.
Many patients find it embarrassing to talk about their bowel problems, but it is important to seek help in managing constipation. Left untreated, constipation can lead to other problems. You may feelunwell and nauseous, exacerbating the constipation as you dont feel like eating or drinking.Constipation can also cause overactive bladder and urinary incontinence due to mechanical pressure on the bladder. Sometimes constipation makes it difficult to empty your bladder, and when urineremains in the bladder there is a risk of urinary tract infections.
We spoke to Ethan and Susan about their symptoms and how they manage it – here’s an excerpt from our free guides: “Bladder and Bowel dysfunction when you have Parkinson’s Disease”
Ethan’s story
Susan’s story
Female and male anatomy are different, and the effects of Parkinson’s disease may have different effects when it comes to bladder and bowel dysfunction.
The bladder and bowel also interact and effect the functioning of these processes. In these free guides, we look at the symptoms, effects and therapies available to manage this condition.
Bladder and Bowel dysfunction when you have Parkinson’s Disease
Urinary Tract Infection In Parkinsons Disease
Article type: Review Article
Authors: Hogg, Elliota | Frank, Samuela | Oft, Jillianb | Benway, Brianc | Rashid, Mohammad Haruna | Lahiri, Shourid*
Affiliations: Department of Neurology, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Department of Infectious Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Department of Urology, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Departments of Neurology, Neurosurgery, and Biomedical Sciences, Cedars-Sinai Medical Center, Los Angeles, CA, USA
Correspondence: Correspondence to: Shouri Lahiri, MD, Departments of Neurology, Neurosurgery, and Biomedical Sciences, Cedars-Sinai Medical Center, 8700 Beverly Blvd., Los Angeles, CA 90048, USA. E-mail: .
Keywords: Parkinsons disease, urinary tract infection, delirium, falls, exacerbation
DOI: 10.3233/JPD-213103
Journal: Journal of Parkinsons Disease, vol. Pre-press, no. Pre-press, pp. 1-15, 2022
Abstract
Recommended Reading: Azithromycin Urinary Tract Infection Dose
You May Like: Difference Between Tardive Dyskinesia And Parkinson’s
Problems Caused By Limited Mobility
Some people with Parkinsons might soil their underwear. This is because mobility problems can make it difficult to wipe after using the toilet. If this is the case, it might help to use wet wipes, a bidet, or an adapted bottom wiper. An occupational therapist or the Disabled Living Foundation can offer further advice.
Bowel problems are common. But you should tell your GP if there are any changes in your bowel habits, particularly if you see blood in your stool. Some problems are difficult to avoid, but there are things you can do to make them less likely to happen.
Parkinsons Disease And Incontinence: Why It Happens And How To Cope
Constipation is a common side effect of Parkinson’s disease, but about 30-40% of patients also experience urinary difficulties, according to the Parkinson’s Foundation. A sudden or immediate urge to urinate is more than annoying. Without diagnosis and treatment, accidents may prevent you from running errands, visiting friends, or doing other activities you enjoy.
Fortunately, there are things you can do to reduce accidents, strengthen your pelvic floor, and improve your quality of life. In this article, we highlight symptoms to watch out for, discuss healthy lifestyle changes that you can make, and feature some of our best-selling products.
Also Check: Does Parkinson Disease Affect Walking
Tips For Living With Faecal Incontinence
If you have faecal incontinence, its important to use the toilet properly. Sit with your knees higher than your hips, lean forward and put your elbows on your knees. Push your tummy out, straighten your back and dont strain.
To prevent the problem getting worse:
- Dont go to the toilet just in case only go when you have a strong urge.
- Dont go to the toilet too often.
- Exercise your pelvic muscles.
You May Like: Can Parkinsons Cause Congestive Heart Failure
Other Symptoms Of Parkinsons Affecting Continence
Urinary incontinence can be a common symptom of Parkinsons, but you are also likely to see symptoms that affect your loved ones muscles and movements.
One of those will often be a tremor in someones arm or hand when theyre sitting down or relaxing, while it is also likely that someone with Parkinsons will not be able to move around particularly freely. Walking can become more challenging while your muscles can become stiff.
So its particularly important that you make the route to the toilet as clear and easy as possible. That way, your loved one will have a better chance of getting to the loo when the urge to urinate arises.
Dont Miss: Neck Brace For Parkinsons
Read Also: Can You Test For Parkinson’s Gene
How Might Parkinson’s Affect The Bowels
Bowel problems can occur in anyone, but some problems, especially reduced bowel movement or constipation, are particularly common in Parkinsons. This tends to be as a result of slowness of movement and muscle rigidity, both of which are visible symptoms of the condition. But Parkinson’s also muscles we cannot see including the bowel muscles – which in turn causes a reduction or slowness of bowel movements.
Poor bowel function may be exacerbated if chewing and swallowing food is difficult, which is quite common in Parkinsons. This may make it harder to eat a diet that is rich in fibre – for example fruit, vegetables and whole grains which helps form soft, bulky stools and aids bowel function.
Exercise is also thought to play a role in efficient bowel function, but if Parkinson’s makes activities more difficult, the bowel may be less stimulated and the intestines can become sluggish.
Constipation is thought to affect up to 65% of people with Parkinson’s the bowel symptoms may predate the neurological ones . Tremor and a fear of spilling drinks can mean some people unintentionally reduce their fluid intake which can make stools hard and more difficult to pass. When stools remain unpassed for a long time, they become harder as the body absorbs more water from them. If stools build up in the rectum they can become impacted and block the rectum. They may also overflow as lumps of stool or watery mucus.
Bowel Incontinence: Another Embarrassing Casualty Of Pd
Fecal Incontinence is where you lose control of your bowels. This blog post explains the primary cause of this in Parkinsons disease. Problems reaching the toilet in time because of mobility, abdominal bloating or cramping compound the problem. Dr. De León has included a check list of things to help minimize occurrences and embarrassment, even to the point of surgery, if necessary.
Recommended Reading: How Fast Does Parkinson’s Dementia Progress
What You Can Do To Help
- Discuss bladder problems with your family doctor or neurologist, who may perform some tests to rule out urinary tract infection or other problems.
- Speak with your family doctor or neurologist about a referral to a urologist . The urologist will be able to look into any bladder symptoms and provide treatment plans.
- Be aware that bladder difficulties can be a sign of wearing off. Wearing off is where some of the symptoms of Parkinsons occur or worsen between doses of medication and are related to the level of medication becoming too low. Taking your medication on time every time helps reduce fluctuations and that will help reduce bladder difficulties.
- Managing constipation and making sure that you have regular bowel movements will also assist in minimising bladder problems.
What Specialist Help Is Available For Bladder Problems
Depending on the problems you are experiencing it may be helpful to seek advice from an Occupational Therapist , Physiotherapist, PDNS, Public Health Nurse or Continence Nurse. Some of the HSE areas and large hospitals offer continence advisory services run by continence nurses with special knowledge and expertise in continence problems and their management. This service can be contacted directly through the local HSE office or via a referral from a GP or PHN. The services are for people who have all types of incontinence. Where appropriate, the continence nurse may refer you to a consultant for specialist advice.
You May Like: L Tyrosine Parkinson’s Disease
How Can I Help Myself
It is easy to become obsessed with bowel activity, but it is not necessary to have a bowel movement every day it can be quite normal for some people to empty their bowels only three or four times a week. What is important is that passing stools does not cause pain or unnecessary strain. Focus on what is normal and healthy for you and remember that bowel activity is affected by food and exercise, so will vary according to what you are eating and doing.
Remember that learning to manage your bowels will take time and patience, so dont expect to solve problems overnight. It may take a few weeks to adjust diet etc, so be patient. There are also plenty of ways you can help yourself.
Parkinsons And Urinary Incontinence
Parkinsons causes problems with automatic bodily functions, such as breathing, heart rate, and urinary function. Urinary incontinence is much different than fecal incontinence and usually doesnt start to occur until the later stages of the disease. Urinary incontinence due to Parkinsons is a two-fold problem. The bladder has trouble holding urine in, but, at the same time, its difficult to control the release of urine, leading to some serious discomfort and emergency bathroom visits.
Urinary incontinence problems can come in many forms:
A person with Parkinsons may have to urinate very frequently, complicated by an increasingly difficult time with movement. Once they sit down, they may find it difficult to let go of the urine and void their bladder. While nearly 40% of Parkinsons patients may experience some level of urinary incontinence, only 15% of patients should develop a serious urinary condition.
Also Check: Parkinsons Disease Symptoms And Treatment
Also Check: Can Lead Poisoning Cause Parkinson’s
Why Do Some People With Parkinsons Disease Experience Urinary Incontinence
Parkinsons is best known for its effects on balance and movement, but it impacts the autonomic nervous system as well. The autonomic nervous system controls specific bodily functions, like heart rate, blood pressure, libido, and urine production.
Over time, changes to the autonomic nervous system affect your bladders ability to store and release urine. That means you might have trouble making it to the bathroom on time or need to urinate more frequently.
