Apomorphine Subcutaneous Injections And Infusion
Apomorphine is an alternative therapy for patients with disabling motor and non-motor fluctuations poorly controlled with conventional treatment. It is a potent dopamine agonist with a short-acting effect that makes it effective in complicated situations such as off dystonia episodes or unpredictable disabling off. Subcutaneous injections are used as a rescue therapy when a rapid on is needed. The effect is quick and lasts 4590min. Patients needing more than three to six injections per day are best treated with a continuous infusion therapy.
Overall, studies report improvement of off time of 50%80%. Its effect on dyskinesias is more controversial. Reductions may occur after a few weeks or months of continuous therapy and mostly if large reduction in levodopa dose can be achieved.
Both apomorphine subcutaneous injections and infusion are safe in terms of procedure but can cause adverse events related to the drug itself. These include nausea, hypotension, excessive somnolence and neuropsychiatric problems, such as confusional state, impulse control disorder and dopamine dysregulation syndrome. Subcutaneous nodules develop in 37% of cases treated with infusions although these are usually not severe and can be managed with non-pharmacological measures, the treatment may need to be stopped.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
What Are The Symptoms Of Parkinson’s Disease How Is Parkinson’s Disease Diagnosed
People with Parkinsons disease suffer from motor symptoms as well as non-motor symptoms.
Motor symptoms include intermittent tremors, slow and rigid movements. Non-motor symptoms include loss of smell, pain and even dementia.
In the initial stages of Parkinsons disease a person may experience symptoms such as:
- Slight rigidity in the arms and legs
- unable to change facial expressions according to emotions spontaneously
- Slight back pain due to which the posture of the person may be slightly stooped
- Sudden stiffness in the body at times
- Tremor on one arm on one side of the body
- The symptoms may be experienced only on one side of the body
- Handwriting may get messier and smaller
In the intermediate stage of Parkinsons disease a person may experience symptoms such as:
- Slower movements and therefore takes longer to do the daily work such as combing, dressing etc
- Loss of balance
- Sudden falls due to frequent loss of balance
- Slurring of speech
- Inability to speak loudly and clearly
- Erratic footwork, as the person is unable to start walking immediately after getting up as if the feet are stuck to the ground, or change direction quickly while walking
- Taking smaller steps than normal while walking
- Trouble swallowing food
- May require aids while walking such as a walker
In the advanced stage of Parkinsons disease the symptoms include:
Read Also: Is Parkinson’s Disease Fatal
Balance And Coordination Issues
Issues with stability and balance usually happen later on in the course of Parkinsons as the disease advances, but its quite common, explains Dr. Pan. You may lose balance if you try to turn too quickly, for example. You may also experience whats called freezing of gait, where your feet struggle to catch up with your brain while youre walking, which can throw you off balance, she says. This may happen when starting to walk, turning, or going through doorways, you can get stuck, so its very impairing.
Parkinsons Disease And Preparing For Surgery

People with Parkinsons disease sometimes face procedures or surgeries due to other medical conditions not related to PD. These could be relatively simple procedures such as a colonoscopy or endoscopy, common surgeries such as cataract removal, gall bladder removal or hernia repair, or more complex surgeries such as open-heart surgery or transplant surgery. I am frequently asked about specific concerns that arise when contemplating surgery for someone with PD.
People with PD, as well as people with other brain disorders, are more prone to side effects from anesthesia as well as negative effects from the stress of the surgery itself. Its important to remember that not everyone is affected in the same way, and this doesnt mean people with PD cannot have the surgeries and procedures they need. It is however important to be educated about what potential problems may arise so that you are as prepared as you can be.
Also Check: Is Parkinson’s Disease Hereditary
Common Complications And Side
As Parkinsons disease progresses , symptoms have a knock-on effect. Deterioration and impairments in the body can lead to a variety of other health concerns that cause a person great difficulty.
As much as these potential concerns cause discomfort for a person, all are treatable with appropriate medication or therapies.
Associated complications which can arise include:
How to manage some of the more common side-effects of Parkinsons disease
The nature of Parkinsons disease progression means that the condition manifests in a variety of ways, not just in areas of mobility. Non-motor symptoms can sometimes be of more distress to a sufferer, troubling their day-to-day lives even more so than their physical ailments.
Once certain non-motor symptoms are recognised, it is easier to understand why and how they are adversely affecting quality of life, as well as gain control through appropriate treatment.
Other problems which can also be effectively managed include:
What Is Parkinsons Disease Symptoms Causes Diagnosis Treatment And Prevention
The causes and symptoms of Parkinsons disease can vary from person to person. While there is no cure, there are medications and treatments to help manage the condition.
Parkinsons disease is a movement disorder that happens when nerve cells in a certain part of the brain are no longer making the chemical dopamine.
The condition is also sometimes known as paralysis agitans or shaking palsy.
The Parkinsons Foundation estimates that 60,000 Americans are diagnosed with Parkinsons every year. However, the true number of people who develop the disease may be much higher.
Recommended Reading: Essential Oils And Parkinson’s
Urinary Incontinence And Constipation Issues
Both constipation and urinary problems are common with Parkinsons. Again, this is because the disease affects the muscles. Weak muscles in the digestive system slow down digestion, which leads to .
Likewise, you may have trouble completely emptying your bladder, or have frequent urges to use the bathroom.
Let your doctor know if you have bladder or . There are medicines as well as changes you can make to your daily routine that will help with these complications. For example, dietary changes can often help with constipation.
Causes Of Parkinson’s Disease
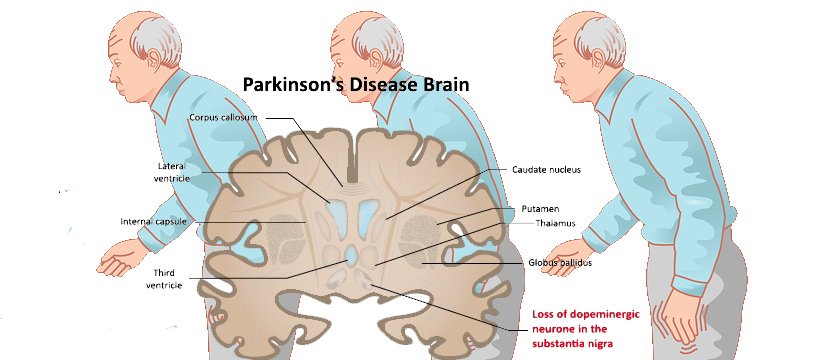
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Don’t Miss: Is Parkinson’s Disease Terminal
Do People Die From Parkinson’s
PD does not directly kill patients people with PD die from other causes, not from PD itself. Two major causes of death for those with PD are falls and pneumonia.
People with PD are at higher risk of falling, and serious falls that require surgery carry the risk of infection, adverse events with medication and anesthesia, heart failure, and blood clots from immobility.3
Pneumonia is a common cause of death, and those with PD are at risk for aspiration pneumonia.3 People with PD often have problems with swallowing, so the risk of aspirating food or drink, or having food or drink going down the wrong pipe is higher. In PD, the person may not be able to cough up the food or drink they aspirated, and it can remain in the lungs, eventually causing an infection.3 Even with general pneumonia, when coughing is weakened, as in PD, the mucus and other material that needs to be coughed up isnt able to be expelled, and this makes effective treatment of pneumonia more difficult in those with PD.
Complications Of Parkinsons Disease
Cognitive problems can occur in the later stages of Parkinsons disease, such as thinking difficulties and impaired reasoning. Emotional changes are also common, namely depression and anxiety. In fact, nearly half of sufferers experience clinical depression at some point in their lives, and its quite common for people living with chronic conditions to feel anxious. Dementia is another complication of Parkinsons disease, due to abnormal protein deposits in the brain known as Lewy bodies. This causes memory loss, trouble concentrating, poor judgement, hallucinations, delusions, irritability, sleep disturbances, and anxiety. Some of these symptoms can be treated with the same medications that treat Alzheimers disease and other forms of dementia.
Sleep problems and disorders are a common complication of Parkinsons disease. These issues range from trouble falling asleep and confusion at night, to acting out dreams and restless legs syndrome, to sleep apnea and frequent need to urinate. Additional bladder and bowel problems include stool leakage, diarrhea and constipation, constant urge to urinate, weak urine stream, and leaking with laughter, exercise, or sneezing. Most of these bladder and bowel issues can be resolved through lifestyle changes, like taking stool softeners, increasing intake of fiber and fluid, and going to the bathroom at regular times throughout the day.
Resources:
Recommended Reading: Parkinson Disease Genetic Link
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
How To Manage The Motor Complications Related To Parkinsons Disease
Go to Doctor: The most important and the initial methods of managing such complications of Parkinsons disease are to inform the doctor. The patient in case of any form of uneasiness should inform the doctor immediately. The doctor will go through the doses and change the schedule according to the requirements. One must not stop the medications abruptly without informing the doctor.
Caregiver: The role of a caregiver for managing motor complications is of extreme importance when it comes to neurological disease like Parkinsons disease. In case the patient encounters freezing, the caregiver should be with him for support and motivation.
Physical Assistance: Falls can be quite dangerous and may lead to fatal accidents too. One popular way to manage falls is using of wheel chair for the patient to move around. This way the patient does not have to walk on legs in order to move. Even while using wheelchair one must be aware of risky places like staircases.
Safe Home: Grab bars may be installed in the potentially dangerous places so that the patient may get quick support in case of accidents.
Lowering the Dosage- When it comes to dyskinesia, the doctor usually lowers the dose of levodopa in use. It has been seen that the lowest dose of the drug may increase the time for the starting of the symptoms of dyskinesia in the patient.
Also Read:
Recommended Reading: Propranolol Increased Total Peripheral Resistance
Apda In Your Community
APDAUncategorizedDeath in Parkinsons Disease
This article was written at the request of a Parkinsons patient who wanted to know how patients die from PD.
Most patients die with Parkinsons Disease and not from it. The illnesses that kill most people are the same as those that kill people with PD. These are heart conditions, stroke and cancer. As we age we become increasingly aware that more than one bad thing can happen to our bodies.
Motor Complications In Parkinson Disease: Clinical Manifestations And Management
- Chulalongkorn Comprehensive Movement Disorders Center, Division of Neurology, Chulalongkorn University Hospital, Bangkok 10330, ThailandDepartment of Neurology, David Geffen School of Medicine at UCLA, Los Angeles, CA 90095, USAThe Parkinson’s and Movement Disorder Institute, Fountain Valley, CA 92708, USA
You May Like: What Is The Difference Between Huntington’s Disease And Parkinson’s Disease
Parkinsons Disease And Covid
At this time, people living with Parkinsons disease do not seem to be at a higher risk of contracting COVID-19. However, there may be an increased risk of developing more severe disease from a COVID-19 infection, particularly respiratory complications, especially for those in later stages of Parkinsons disease.
Hospitalization rates for those who get COVID-19 may be higher, and those with Parkinsons disease may also have a higher instance of death from COVID-19 than the general population. The increased risk of severe disease and death were consistent with the known risk factors shared by the general public which include:
- Older than 60 years of age
- Other health conditions such as obesity, heart disease, diabetes, or kidney disease
These statistics will continue to evolve as more data is found as studies on the impact of COVID-19 and Parkinsons disease continue.
Drastic Changes In Blood Pressure
PD can cause drastic changes in blood pressure because it affects the autonomic nervous system, which controls blood flow and blood pressure. Unlike other parts of the body, we do not have control over our nervous system. When PD occurs, it takes over the nervous system creating changes in blood pressure throughout the day, says Medical News Today.
These drastic changes in blood pressure can lead to orthostatic hypertension, a drop in blood pressure that causes a person to feel dizzy or faint when they stand up, writes the source. It can also lead to falls and fainting. Another common problem is low blood pressure, also known as hypotension. High blood pressure can also be a problem for some people. Any type of wild fluctuation between the two can lead to heart problems. To help treat this complication and avoid any drastic changes, doctors can sometimes prescribe medications that will help stabilize blood pressure. Patients can also invest in a pair of compression stockings which may also be helpful.
You May Like: Parkinson’s Disease Genetics
Research And Statistics: Who Has Parkinsons Disease
According to the Parkinsons Foundation, nearly 1 million people in the United States are living with the disease. More than 10 million people worldwide have Parkinsons.
About 4 percent of people with Parkinsons are diagnosed before age 50.
Men are 1.5 times more likely to develop the disease than women.
What Are Lewy Bodies
The affected neurons of people with Parkinsons disease have been found to contain clumped proteins called Lewy bodies, but researchers arent yet sure why Lewy bodies form or what role they play in the disease.
Lewy bodies are clumps of a protein called alpha-synuclein . Neurons cant break down these protein clumps, which may lead to the death of these cells.
Some other theories about what causes the death of brain cells in people with Parkinsons disease include free radical damage, inflammation, or toxins.
You May Like: Parkinson’s Disease Awareness Ribbon Color
Reduced Sense Of Smell
According to research published in the Parkinsons Disease journal, over 95-percent of people with this chronic condition will lose their sense of smell to some degree. Part of this loss of smell may be an inability to identify certain odors or differentiate between odors. This is due to Parkinsons impact on the nervous system, says Medical News Today.
This reduced sense of smell can be interpreted as a warning sign of PD because it can begin to happen years before any other symptoms appear. Oftentimes its overlooked. The source notes that doctors can sometimes use a reduced sense of smell as a predictor for PD. Its also considered one of the top five most common symptoms.
How Is Parkinson’s Disease Diagnosed

Diagnosis is difficult at every stage of the disease, but particularly in the early stages. No single test can provide a diagnosis. A diagnosis will likely involve physical and neurological examinations, conducted over time to assess changes in reflexes, coordination, muscle strength, and mental function. Your doctor might also see how you respond to medicine.
You may need to have brain imaging tests to rule out other conditions that might be causing your symptoms. Such tests could include MRI and CT scans and possibly some other types of scans. Blood tests may also be done to exclude other illnesses.
Read Also: Life Expectancy Of Parkinson’s Disease
Living With Parkinsons Disease
Patients living with PD can take steps to ensure they get quality care from their healthcare team, as well as take good care of themselves.
Staying as active as possible with help from an occupational therapist who can show you how to modify daily activities, eating a healthy and well-balanced diet, and taking medications as prescribed can all help optimize your health and promote well-being. Talking with the doctor about any challenges or concerns can also help you brainstorm solutions to problems or help create a plan to address issues.
Don’t neglect emotional health, as well. Depression and anxiety affect up to half of those living with PD.5
Mood disorders and changes like these can actually worsen symptoms and affect overall health, so proper treatment is crucial. Tell the doctor if youre noticing changes in mood at all, so this can be addressed with treatment, whether its medication, counseling, or both. Spending time with other people friends, family members, activity groups can also help decrease feelings of isolation or loneliness.
