What Is The Mortality Rate For Parkinsons
Parkinsons disease is the most common movement disorder. It represents the second most common degenerative disease of the central nervous system.
Studies show that this disease affects around 1-2 people out of 1000. 1% of the population over 60 years old suffers from this disease. Nonetheless, Parkinsons is very rare before 50 years old.
The diseases appearance varies considerably on different reports, probably due to discrepancies in methodological concerns or diagnostic criteria. There is an appearance of approximately 5 to 21 new cases every year per 100.000 people. Also, statistics show that there are from 18 to 328 people with this condition per 100,000 population. Still, most of the studies estimate 120 cases per 100,000 people. Parkinsons disease is about 1.5 times more common in men than in women.
Before introducing Levodopa, Parkinsons disease caused severe disability or death in 25% of patients within five years of onset, 65% within ten years, and 90% within 15 years. After introducing levodopa, the mortality rate drops approximately 50%, and longevity extends by many years.
Nonetheless, statistics from 1999 to 2017 reveal there is an increase in deaths from this cause. In adults over 65 years, old death rates increased from 42 to 65 per 100,000 population from 1999 to 2017.
Medications For People With Parkinsons Disease
Symptoms of Parkinsons disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements.;Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinsons medications fit into one of the following broad categories:;
- levodopa dopamine replacement therapy
- dopamine agonists mimic the action of dopamine
- COMT inhibitors used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors prevent the metabolism of dopamine within the brain.
Diagnosis Of Parkinsons Disease
A number of disorders can cause symptoms similar to those of Parkinson’s disease. People with Parkinson’s-like symptoms that result from other causes are sometimes said to have parkinsonism. While these disorders initially may be misdiagnosed as Parkinson’s, certain medical tests, as well as response to drug treatment, may help to distinguish them from Parkinson’s. Since many other diseases have similar features but require different treatments, it is important to make an exact diagnosis as soon as possible.
There are currently no blood or laboratory tests to diagnose nongenetic cases of Parkinson’s disease. Diagnosis is based on a person’s medical history and a neurological examination. Improvement after initiating medication is another important hallmark of Parkinson’s disease.
Also Check: Does Susan Collins Have Parkinsons
What Treatments Are Available
Many Parkinson’s patients enjoy an active lifestyle and a normal life expectancy. Maintaining a healthy lifestyle by eating a balanced diet and staying physically active contributes to overall health and well-being. Parkinson’s disease can be managed with self-care, medication, and surgery.
Self careExercise is as important as medication in the treatment of PD. It helps maintain flexibility and improves balance and range of motion. Patients may want to join a support group and continue enjoyable activities to improve their quality of life. Equally important is the health and well being of the family and caregivers who are also coping with PD. For additional pointers, see Coping With Parkinsons Disease.
These are some practical tips patients can use:
Medications There are several types of medications used to manage Parkinson’s. These medications may be used alone or in combination with each other, depending if your symptoms are mild or advanced.
After a time on medication, patients may notice that each dose wears off before the next dose can be taken or erratic fluctuations in dose effect . Anti-Parkinsons drugs can cause dyskinesia, which are involuntary jerking or swaying movements that typically occur at peak dosage and are caused by an overload of dopamine medication. Sometimes dyskinesia can be more troublesome than the Parkinsons symptoms.
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Is The Best Test For My Doctor To Order To Diagnose Parkinsons Disease
There is no reliable blood test to diagnose Parkinsons disease.; The best way to make a diagnosis is to have a neurological examination by someone experienced in the care of Parkinsons disease patients.; There are diagnostic criteria for the diagnosis of Parkinsons disease , which usually include:
;I: Is Bradykinesia (slowness of movement present?
;II: Are two of the below present?
___ Rigidity
___ 4-6 Hertz resting tremor
___ Postural instability not caused by primary visual, vestibular, cerebellar,
proprioceptive dysfunction
III: Are at least 3 of the below present?
___ Unilateral onset
___ Persistent asymmetry affecting side of onset most
___ Excellent response to levodopa
___ Severe levodopa induced dyskinesia
___ Levodopa response for 5 years or more
___ Clinical course of 5 years or more
Very rarely, there exists confusion about the diagnosis, and in these cases other tests such as Positron Emission Tomography, and Beta SPECT scanning may be useful . ;
Learn more about Parkinson Disease and its treatment by watching videos from our educational Parkinson Symposiums
Read more about Parkinsons Disease in Dr. Michael S. Okuns Book, Ask the Doctor about Parkinsons Disease. ;Dr. Okun works at the University of Florida Gainesville, and also serves as the National Medical Director for the Parkinsons Foundation.
Parkinson’s Foundation
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Role Of Pet Scans In Diagnosis
Scanning for loss of dopamine, the major chemical responsible for some symptoms of Parkinsons, permits comparison against scans of people who have no dopamine deficiency. By itself, a scan does not make the diagnosis of Parkinson’s but identifies the decline in dopaminergic neurones. It is used by experienced neurologists in cases where the diagnosis of Parkinsons is uncertain.Scans include radionuclide positron emission tomography or by injecting radiopharmaceutical agent in the brain) into a patients veins in a procedure referred to single photon emission computed tomography imaging.
PET scans typically focus on glucose metabolism, and DaT/SPECT scans focus on the activity of the dopamine transporter. Unfortunately, this decline is seen in conditions other than Parkinsons such as Multiple Systems Atrophy and Progressive supranuclear palsy .
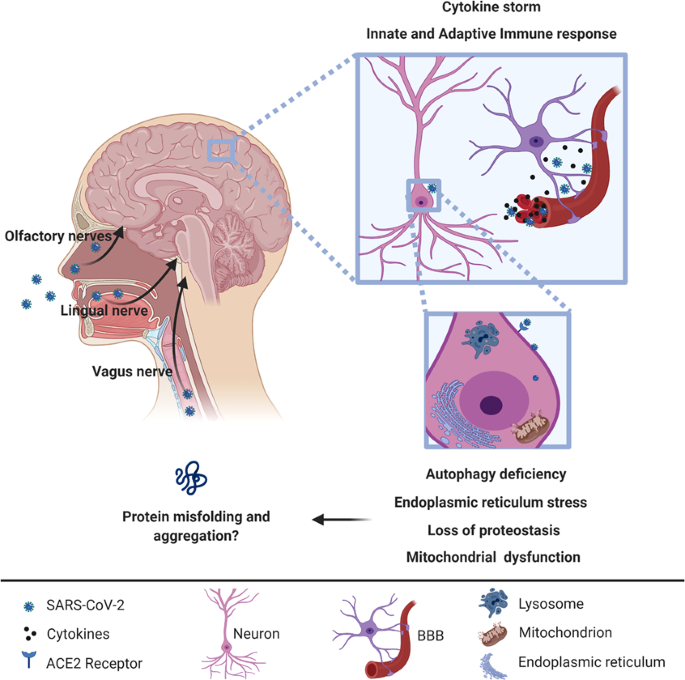
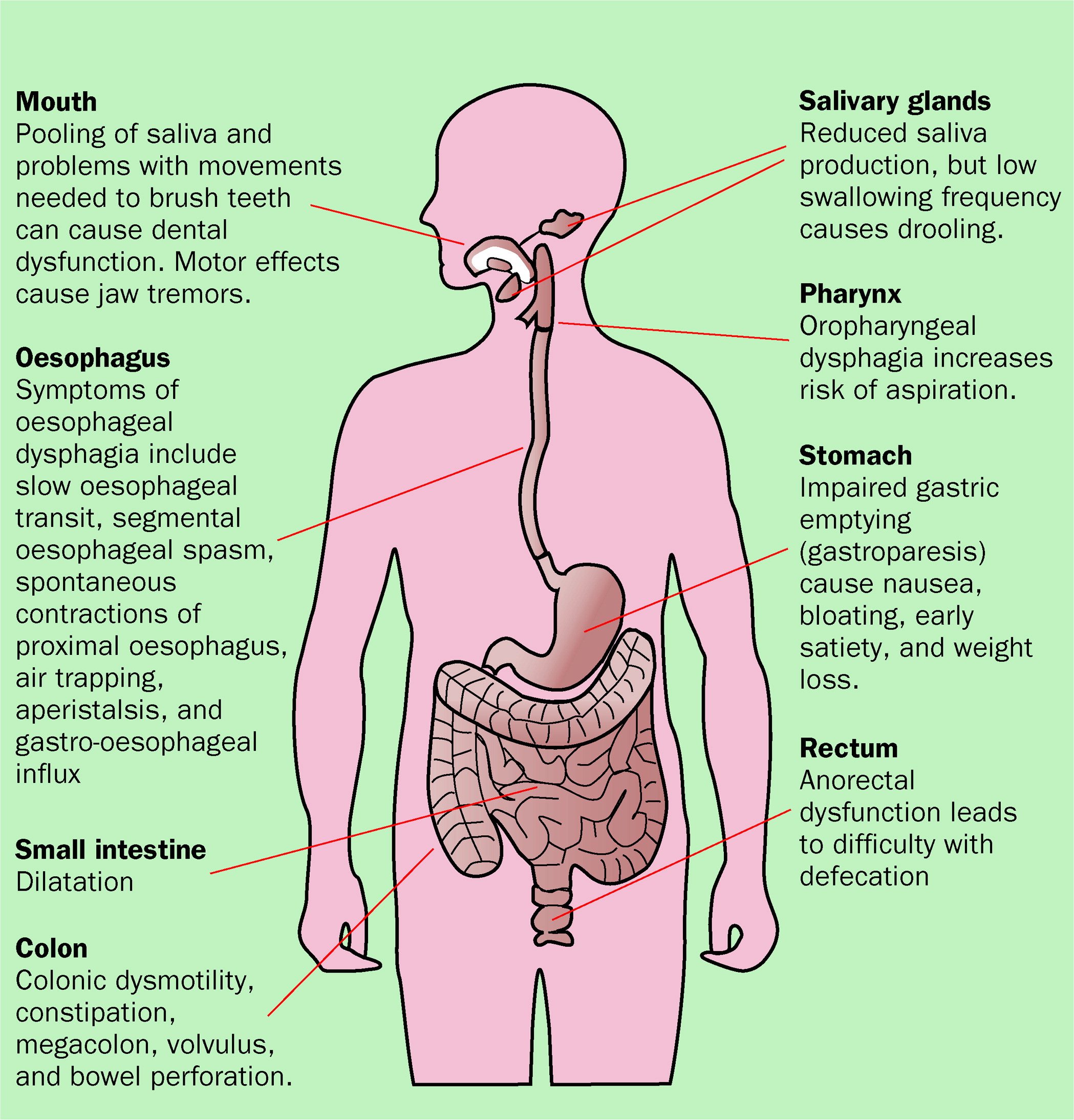
Parkinson Disease Neuropathology In The Autonomic Nervous System
Anatomically, the autonomic nervous system can be divided into central autonomic networks, sympathetic pathways, parasympathetic pathways and the enteric nervous system. Central autonomic networks integrate autonomic function, linking the neocortex, diencephalon and brainstem. At its core is the nucleus tractus solitarius which integrates somatic and autonomic nervous systems and maintains homeostasis with projections to the hypothalamus, limbic structures and descending autonomic tracts. PD pathology has been characterized by intraneuronal inclusions which contain α-synuclein known as Lewy neurites or Lewy bodies . α-synuclein is a presynaptic protein thought to maintain synaptic integrity and be involved with regulation of dopamine synthesis. Although often seen in the absence of neuronal loss, evidence suggests that α-synuclein aggregation is a precursor to neurodegeneration. PD pathology has been observed in a chain of neurons forming autonomic pathways including: the hypothalamus, preganglionic parasympathetic projection neurons in the dorsal motor nucleus of the vagus and pre-ganglionic and post-ganglionic sympathetic projection neurons . PD pathology has also been found in several end-organs including the submandibular gland, lower esophagus, duodenum, pancreas, bronchus, larynx, epicardium, adrenal medulla, parathyroid and ovary. illustrates most areas within autonomic pathways where PD pathology has been found.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Does Parkinson’s Do To The Brain
Deep down in your brain, there’s an area called the substantia nigra, which is in the basal ganglia. Some of its cells make dopamine, a chemical that carries messages around your brain. When you need to scratch an itch or kick a ball, dopamine quickly carries a message to the nerve cell that controls that movement.
When that system is working well, your body moves smoothly and evenly. But when you have Parkinson’s, the cells of your substantia nigra start to die. There’s no replacing them, so your dopamine levels drop and you can’t fire off as many messages to control smooth body movements.
Early on, you won’t notice anything different. But as more and more cells die, you reach a tipping point where you start to have symptoms.
That may not be until 80% of the cells are gone, which is why you can have Parkinson’s for quite a while before you realize it.
Advancement In Parkinsons Disease
With the progress of Parkinsons disease with time, symptoms associated with the problem become worse typically and many new problems emerge. Despite patients receive benefits with the intake of anti-Parkinson medication; the benefit fails to last for a long time even when they intake it frequently.
Most of the patients usually experience involuntary movements to make them, as looking fidgety when they intake the medicine and otherwise works the best. Hence, it is very much essential to emphasize such movements typically and do not bother about the condition of patients too much.
Other problems, which may take place with the progress of Parkinsons disease, are-
- Problems associated with balance and gait, along with falls
- Difficulty in communication or impairment of speech
- Difficulty in swallowing
- Cognitive impairment, such as memory and thinking
- Behavioral problems
- Light-headedness.
Some of the problems are of very much difficult to treat with medicines. However, any experienced doctor or a neurologist specializes in movement disorder will still may provide the necessary support and guidance for patients even during the advanced phases of the Parkinsons disease.
You May Like: Can Parkinson’s Run In The Family
The Heart Of The Matter: Cardiovascular Effects Of Parkinsons Disease
It has long been understood that Parkinsons disease does not just cause movement symptoms, but also causes a litany of non-motor symptoms with effects throughout the body. One of the organ systems that is affected is the cardiac system, encompassing the heart, as well as the major and minor blood vessels. I received this topic as a suggestion from a blog reader and we will be discussing this important issue today. Please feel free to suggest your own blog topic.
Treatment Of Parkinson’s Disease
MedicationIn addition to combating the symptoms of Parkinson’s with lifestyle changes such as exercise and/or physical therapy, medication therapy can help control Parkinson’s symptoms. Because people with the disease have low levels of dopamine, the main drug therapy is based on increasing dopamine levels in the brain.
The drug levodopa contains a substance that occurs naturally in the body. When taken, the drug is converted to dopamine when it reaches the brain. Levodopa is combined with another substance to ensure it does not convert to dopamine before reaching the brain.
As Parkinson’s disease progresses, the benefit from levodopa may become less reliable. In addition, levodopa side effects can include confusion, delusions and hallucinations, as well as involuntary movements called dyskinesia. The dose can be reduced to mitigate these side effects, but sometimes at the expense of losing the benefits of symptom control.
Other types of drugs can be used in combination with levodopa to prolong its beneficial effects. Some of these drugs work by blocking the enzymes known to break down dopamine, whether created naturally in the brain or by levodopa. Other types of medication, including anticholinergics and antivirals, are sometimes used to control physical symptoms such as tremor and involuntary movement. However, patients may find that their limited benefits do not offset the sometimes serious side effects.
External resources for Parkinson’s disease:
Also Check: Sam Waterston Parkinsons
How Parkinsons Disease Affects The Human Body
More than one million people live with Parkinsons disease in the U.S., but no two experiences are the same. Parkinsons affects individuals in vastly different ways: for some, Parkinsons may first show up as slight hand tremors, and in others, it might appear as an unusual level of stiffness. For one person it may progress slowly, and in someone else, it may spread frighteningly fast.
There are some consistencies in how the disease works, however, and understanding these similarities can help prepare for what to expect if you or a loved one is diagnosed with Parkinsons disease. From how it starts to how it progresses through its five stages, here are some of the ways Parkinsons affects the human body.
When Does Parkinson Disease Really Start
This is one of the million dollar questions in Parkinsons disease research.; We actually dont know the answer. From the clinical trial or research perspective, we arbitrarily base the answer on either the occurrence of the first symptom or alternatively the date of diagnosis.; The date of diagnosis is however biased, and largely based on obvious motor symptoms such as tremor, stiffness, or slowness. We know that this estimate therefore is grossly inaccurate. In fact, by the time a Parkinsons disease patient manifests the first symptom , significant degeneration of the dopaminergic neurons in the brain has already occurred.
We now know that the loss of the sense of smell, constipation, depression, personality changes, sleep problems, and even anxiety may long precede the motor symptoms of Parkinsons disease. The problem with using these symptoms as diagnostic markers however, is that they commonly occur in the general population, making it very difficult to judge what is part of Parkinsons disease, and what is not.
Complicating the picture as to the onset of Parkinsons disease has been the discovery that many patients may have rapid eye movement sleep disorders many years prior to the onset of motor symptoms.; Additionally, Braak and colleagues have recently proposed that the degeneration in Parkinsons disease actually starts well before dopaminergic cells in the midbrain begin to die. The cells that die in Parkinsons disease are deep in an area called the brainstem.
Read Also: Can Parkinson’s Run In The Family
Hospice Eligibility For Parkinsons Disease
Due to the progressive nature of Parkinsons disease, it can be challenging for families to know when their loved one is eligible for the support of hospice care. If a loved one has been diagnosed with six months or less to live or if they have experienced a decline in their ability to move, speak, or participate in the activities of daily living without caregiver assistance, it is time to speak with a hospice professional about next steps.;
Incidence Of Parkinsons Disease
Its estimated that approximately four people per 1,000 in Australia have Parkinsons disease, with the incidence increasing to one in 100 over the age of 60. In Australia, there are approximately 80,000 people living with Parkinsons disease, with one in five of these people being diagnosed before the age of 50. In Victoria, more than 2,225 people are newly diagnosed with Parkinsons every year.
Recommended Reading: Katharine Hepburn Parkinsons
How Does Parkinsons Disease Affect The Body
Recognising the signs
A combination of signs can help a doctor make an early diagnosis. If Parkinsons disease is diagnosed early, the chances of being able to treat and manage the condition are greater.;Individual signs may not be an indication of Parkinsons disease.;Some signs such as loss of smell could be caused by an infectious illness, or;joint stiffness by conditions like arthritis.
Parkinsons is most commonly diagnosed with a very;physical examination;and assessment of a persons;medical history. There are very specific markers for diagnosis which doctors use to assess for possible Parkinsons disease. These markers have a lot to do with a combination of very specific signs and symptoms and if recognised early enough, can be better managed.
1. Primary motor symptoms
2. Secondary motor symptoms
Other motor symptoms include:
Some individuals may also experience the following:
- Hunched over / stooped posture – When standing, the body may begin to slouch or lean inwards, causing a hunched over appearance.
- Impaired gross motor coordination
- Impaired fine motor dexterity and motor coordination
- Difficulties with swallowing or chewing
- Cramping
- Production of excess saliva and drooling
- Sexual dysfunction
- Dystonia
- Akathisia
3. Non-motor symptoms
Symptoms that do not involve physical movement or coordination, and often precede motor problems, can include:
Symptoms are initially mild, even if they develop suddenly, and typically affect one side of the body at first.
What Are The Symptoms
Symptoms of PD vary from person to person, as does the rate of progression. A person who has Parkinson’s may experience some of these more common “hallmark” symptoms:
- Bradykinesia – slowness of movement, impaired dexterity, decreased blinking, drooling, expressionless face.
- Tremor at rest – involuntary shaking that decreases with purposeful movement. Typically starts on one side of the body, usually the hand.
- Rigidity – stiffness caused by involuntary increase in muscle tone.
- Postural instability – sense of imbalance. Patients often compensate by lowering their center of gravity, which results in a stooped posture.
Other symptoms that may or may not occur:
Freezing or being stuck in place Shuffling gait or dragging of one foot Stooped posture Cognitive impairment
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
