The Last Year Of Life In Parkinson’s Disease
The study also examined nearly 45,000 hospitalizations in people with terminal Parkinson’s, meaning their end-of-life period.
Of those with terminal PD, the most common reasons for being in the hospital were:
- Heart disease
- Lung disease that was not from an infection
Less common causes for hospitalization were problems related to the stomach or intestines, muscles, nervous system, or endocrine system .
It is not surprising that infection was the most common hospitalization before death, as people with Parkinson’s are vulnerable to developing a number of infections as a result of their disease. For example, bladder dysfunction in Parkinson’s increases a person’s risk of developing urinary tract infections, which can become life-threatening if not detected and treated promptly.
In addition, research suggests that aspiration pneumonia is 3.8 times more common in people with Parkinson’s as compared to the general population. It has also been consistently reported to be the main cause of death in people with Parkinson’s.
Aspiration pneumonia results from underlying swallowing difficulties, which leads to stomach contents being inhaled into the lungs. Immobilization and rigidity, which can impair phlegm removal, also contribute to the development of pneumonia in people with Parkinson’s.
Some Parkinson’s Treatment Options
Parkinson’s disease has no cure, but there are treatment options to control your symptoms and improve your quality of life which include:
- Medication. Levodopa and other medications, which are trying to boost dopamine . There are number of those medications which can be used alone or in combination. Although many of those medications can help you significantly control your motor symptoms , you might also experience side effects and diminished efficacy over time.
- Physical, occupational, and speech therapy are usually part of your treatment plan and can improve your balance, mobility, ability to do daily tasks, and speech.
- Deep brain stimulation is a surgery performed by a neurosurgeon, and in indicated patients can help with motor symptoms, though non-motor symptoms, such as falls, constipation, low blood pressure and incontinence do not improve.
- Tai Chi is a Chinese martial art that may help sufferers regain some of their balance and strength, as well as decrease the risk of falling. Dance, such as a Zumba, may also help, as can using a stationary bicycle and rock steady boxing.
Many treatment options for Parkinson’s are most effective when used in conjunction with others such as taking medication and doing physical therapy.
You Could Have Parkinsons Disease Symptoms In Your 30s Or 40s And Not Know It
Blog post | 11 Apr 2019
You’d be forgiven for thinking that Parkinson’s is only an older person’s disease.
Many people with Parkinson’s, a progressive disease of the nervous system, are indeed at retirement age. So the world was shocked when Back to The Future actor Michael J. Fox revealed he was diagnosed with Parkinson’s disease at only 29 years old.
But Fox’s case isn’t unique. It’s believed that 1 in 10 people with Parkinson’s develop the disease some time before their 40th birthday. About 1 in 5 Australians with Parkinson’s are at ‘working age’ .
And a person can live with symptoms for many years before a diagnosis of Parkinson’s is made.
To mark World Parkinson’s Day, Thursday April 11, here’s what you need to know about the early signs of this insidious neurological disease.
Recommended Reading: Thc Treatment For Parkinson’s
What Are The Early Warning Signs Of Parkinson’s Disease
Parkinsons warning signs can be motor symptoms like slow movements, tremors or stiffness. However, they can also be non-motor symptoms. Many of the possible non-motor symptoms can appear years or even decades ahead of motor symptoms. However, non-motor symptoms can also be vague, making it difficult to connect them to Parkinson’s disease.
Non-motor symptoms that might be early warning signs include:
- Sleep problems such as periodic limb movement disorder , rapid eye movement behavior disorder and restless legs syndrome.
Consider Deep Brain Stimulation Surgery
- Talk with your doctor about whether you would be a good candidate for Deep Brain Stimulation. DBS is an FDA-approved surgical technique that involves a surgeon implanting a neurostimulator that delivers electrical current to certain parts of the brain. When these targeted areas of the brain are stimulated, it blocks the abnormal nerve signals that cause tremor and other Parkinsons symptoms. One person with YOPD described his DBS surgery as a buyback of life and daylight savings time on steroids because he noticed such a difference in his quality of life.
- Watch this panel of DBS experts weigh in on the benefits of DBS.
Recommended Reading: What Is The Medicine For Parkinson’s Disease
Diagnosing Early Onset Parkinsons Disease
There is no single test to detect Parkinsons. A diagnosis may be difficult and take a while. The condition is usually diagnosed by a neurologist based on a review of your symptoms and a physical exam.
A DaTscan to visualize your brains dopamine system may help confirm diagnosis. Blood tests and other imaging tests, such as an MRI scan, dont diagnose Parkinsons. However, they may be used to rule out other conditions.
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinsons disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinsons. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinsons disease. Electrical impulses are introduced to the brain, which has the effect of normalising the brains electrical activity reducing the symptoms of Parkinsons disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
You May Like: How To Get Checked For Parkinson’s Disease
What Are The Later Secondary Signs And Symptoms Of Parkinson’s Disease
While the main symptoms of Parkinson’s disease are movement-related, progressive loss of muscle control and continued damage to the brain can lead to secondary symptoms. These secondary symptoms vary in severity, and not everyone with Parkinson’s will experience all of them, and may include:
Prevalence Of Parkinsons State
Western and Southern states appear to have lower rates of Parkinsons disease, while Northeastern and many Midwestern states have higher rates . Mississippi and Montana have the lowest rates of Parkinsons, at 5.1 per 10,000. Vermont has the highest rate of Parkinsons at 9.9 per 10,000.
Exhibit 2: Prevalence of Parkinsons Disease, by geography
Don’t Miss: Is Parkinson’s Considered A Neurological Disease
Complications Related To Parkinson’s Can Affect Survival
Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology.
Parkinson’s is a common neurodegenerative disease, and although it is not fatal, research suggests it may influence life expectancy.
A 2012 study in Archives of Neurology examined the six-year survival of nearly 140,000 Medicare beneficiaries with Parkinson’s disease in the United States. During the six-year period, 64% of the participants with Parkinson’s disease passed away.
The risk of death of those with Parkinson’s was then compared to Medicare beneficiaries who did not have Parkinson’s or any other common diseases, including:
When controlling for variables like age, race, and gender, the six-year risk of death among people with Parkinson’s was found to be nearly four times greater than those Medicare beneficiaries without the disease or other common diseases.
At the same time, the rate of death among those with Parkinson’s disease was similar to those with hip fracture, Alzheimer’s dementia, or a recent heart attackalthough it was higher than those who had been newly diagnosed with either colorectal cancer, stroke, ischemic heart disease, or chronic obstructive pulmonary disease.
Influence Of Sex On Nms: Onset Analysis
We compared mean values for NMS for the 3 cohorts categorized by sex of subject .
Prevalence of NMS at onset, categorized by sex. NMS mean scores were categorized by sex of participant or male ) for Parkinsons disease , SWEDD , and healthy controls . NMS scales analyzed are displayed A through Q indicating the score range in the title. Higher number indicates more dysfunction except for MoCA Cognition and USPIT Olfaction . Pairwise differences within the cohort were evaluated with independent-samples MannWhitney U test with Bonferroni correction for multiple comparisons. Differences between cohorts for each sex were evaluated using the independent-samples KruskalWallis test. Statistical differences within cohorts males) are indicated by an asterisk . Post hoc analyses signifying differences between the HC, PD, and SWEDD cohorts are indicated for females and males as a=HC versus PD, b=HC versus SWEDD, and c=PD versus SWEDD. p< 0.05.
Within the PD cohort, females reported significantly higher mean scores for overall autonomic dysfunction ), thermoregulatory dysfunction ), anxious mood ), and pain and other sensations ). Males reported a significantly higher degree of sexual dysfunction ), urinary dysfunction ), cognitive dysfunction and 1), and hyposmia ).
Within the SWEDD cohort, females reported significantly higher mean scores for gastrointestinal dysfunction and 1), anxious mood ), and pain and other sensations ).
You May Like: Dry Mouth And Parkinson’s
Support For People With Parkinsons Disease
Early access to a multidisciplinary support team is important. These teams may include doctors, physiotherapists, occupational therapists, speech therapists, dietitians, social workers and specialist nurses. Members of the team assess the person with Parkinsons disease and identify potential difficulties and possible solutions.There are a limited number of multidisciplinary teams in Victoria that specialise in Parkinsons disease management. But generalist teams are becoming more aware of how to help people with Parkinsons disease.
Seven Signs Of Early Onset Parkinsons
There are a series of symptoms that can alert us to the early onset of Parkinsons disease. There are more signs, but were going to focus on these seven:
- Sleep disorders. The most common disorders are insomnia , restless legs syndrome, and REM sleep behavior disorder.
- Depression. This is one of the first symptoms to appear and is in fact considered an early indicator of the disease.
- Other mood changes. In addition to depressive symptoms, anxiety and apathy are very common. These symptoms can negatively influence the desire to seek help and resolution.
- Cognitive changes. Many people with early onset Parkinsons usually find it difficult to do more than one thing at once. Poor task execution, slower thinking speed, attention and concentration problems, memory problems, and dementia are all symptoms of early onset Parkinsons.
- Tremors. Although they usually start in the hands, they start in the jaw or on the feet in other patients. The most characteristic thing about these tremors is that they occur at rest.
- Bradykinesia. This is a gradual loss of spontaneous movement. General movement simply slows down. This is one of the most disabling and frustrating symptoms for those affected.
- Fatigue. With early onset Parkinsons, the patient feels tired all the time without having exerted themselves at all.
Recommended Reading: Parkinsons Disease Stage 1 Symptoms
Don’t Miss: Can You Inherit Parkinson’s Disease
Managing Early Onset Parkinsons Disease
According to Dr. Gilbert, while PD tends to progress more slowly in younger people, managing the disease can be particularly challenging from a psychological and social standpoint.
Younger patients may be dating, or have young families, and are building their careers, she explained. All of a sudden, they are grappling with something that nobody else at their stage of life is familiar with. It can be incredibly isolating. But its important to realize that a PD diagnosis is not the end of their life. With the right perspective and support, they can continue to work, support their families and engage with friends and loved ones.
Dr. Gilbert recommends that once diagnosed, patients start building a care team headed by a neurologist ideally a movement disorder specialist. Other key members of a PD care team include physical and occupational therapists to help maximize fine and gross motor skills a speech pathologist to work on soft or garbled speech and a dietician to address dietary changes, weight loss and constipation.
Whats Different About Young
The age of diagnosis matters for a variety of reasons, from probable causes of early cases to symptoms and treatment:
- Genetics. As with any case of Parkinsons disease, the exact cause is usually unknown. That said, The young-onset cases of Parkinsons disease are, on average, a bit more likely to be familial or genetic, says Gregory Pontone, M.D., director of the Johns Hopkins Movement Disorders Psychiatry Clinic.
- Symptoms. In many patients with YOPD, dystonia is an early symptom. People with YOPD also report more dyskinesia . They also tend to exhibit cognitive problems, such as dementia and memory issues, less frequently.
- Progression. Patients with young-onset Parkinsons appear to have a slower progression of the disease over time, says Pontone. They tend to have a milder course, staying functional and cognitively intact for much longer.
- Treatment. Most patients with Parkinsons take the medication levodopa. However, other drugs, such as MAO-B inhibitors, anticholinergics, amantadine, and dopamine receptor agonists, may be used before levodopa.
Don’t Miss: What Does Parkinson’s Disease Do
Support For People Living With Parkinsons Disease
While the progression of Parkinsons is usually slow, eventually a persons daily routines may be affected. Activities such as working, taking care of a home, and participating in social activities with friends may become challenging. Experiencing these changes can be difficult, but support groups can help people cope. These groups can provide information, advice, and connections to resources for those living with Parkinsons disease, their families, and caregivers. The organizations listed below can help people find local support groups and other resources in their communities.
Complications Related To Parkinsons Can Affect Survival
Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology. She is an associate professor of neurology at Tufts Medical School and medical director of the Lahey Clinic Multiple Sclerosis Center in Lexington, Massachusetts.
Parkinsons is a common neurodegenerative disease, and although it is not fatal, research suggests it may influence life expectancy.
A 2012 study in Archives of Neurology examined the six-year survival of nearly 140,000 Medicare beneficiaries with Parkinsons disease in the United States. During the six-year period, 64% of the participants with Parkinsons disease passed away.
The risk of death of those with Parkinsons was then compared to Medicare beneficiaries who did not have Parkinsons or any other common diseases, including:
When controlling for variables like age, race, and gender, the six-year risk of death among people with Parkinsons was found to be nearly four times greater than those Medicare beneficiaries without the disease or other common diseases.
At the same time, the rate of death among those with Parkinsons disease was similar to those with hip fracture, Alzheimers dementia, or a recent heart attackalthough it was higher than those who had been newly diagnosed with either colorectal cancer, stroke, ischemic heart disease, or chronic obstructive pulmonary disease.
Recommended Reading: How Long Does A Person Live With Parkinsons Disease
Don’t Miss: Can Parkinson’s Disease Cause Dementia
Causes Of Parkinsons Disease
Parkinsons disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinsons disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Dont Miss: Wearable Technology For Parkinson Disease
Who Does It Affect
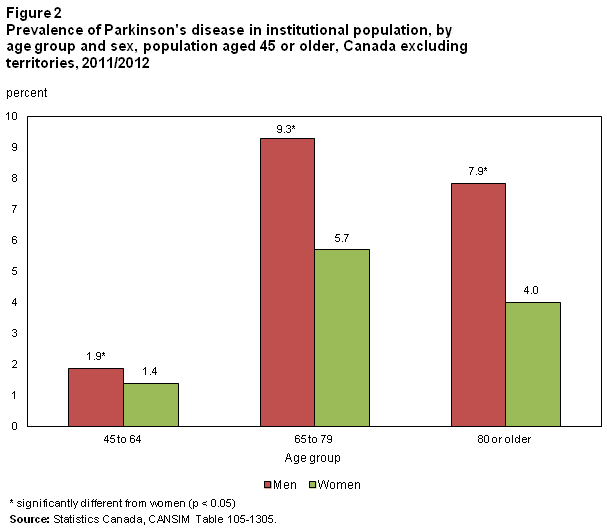
The risk of developing Parkinsons disease naturally increases with age, and the average age at which it starts is 60 years old. Its slightly more common in men or people designated male at birth than in women or people designated female at birth .
While Parkinsons disease is usually age-related, it can happen in adults as young as 20 .
Also Check: What Happens When You Have Parkinson’s Disease
Changes In Cognition And Parkinsons Disease
Some people with Parkinsons may experience changes in their cognitive function, including problems with memory, attention, and the ability to plan and accomplish tasks. Stress, depression, and some medications may also contribute to these changes in cognition.
Over time, as the disease progresses, some people may develop dementia and be diagnosed with Parkinsons dementia, a type of Lewy body dementia. People with Parkinsons dementia may have severe memory and thinking problems that affect daily living.
Talk with your doctor if you or a loved one is diagnosed with Parkinsons disease and is experiencing problems with thinking or memory.
How Is It Treated And Is There A Cure
For now, Parkinsons disease is not curable, but there are multiple ways to manage its symptoms. The treatments can also vary from person to person, depending on their specific symptoms and how well certain treatments work. Medications are the primary way to treat this condition.
A secondary treatment option is a surgery to implant a device that will deliver a mild electrical current to part of your brain . There are also some experimental options, such as stem cell-based treatments, but their availability often varies, and many aren’t an option for people with Parkinsons disease.
Don’t Miss: Is It Parkinson’s Or Something Else
The 5 Stages Of Parkinsons Disease
Getting older is underrated by most. Its a joyful experience to sit back, relax and watch the people in your life grow up, have kids of their own and flourish. Age can be a beautiful thing, even as our bodies begin to slow down. We spoke with David Shprecher, DO, movement disorders director at Banner Sun Health Research Institute about a well-known illness which afflicts as many as 2% of people older than 65, Parkinsons Disease.
Recommended Reading: Parkinsons Disease And Rls
