Dopamine And Pathogenesis Of Parkinsons Disease
Dopamine is the organic chemical of the catecholamine family and precursor for noradrenaline. It is synthesized in presynaptic neuron from tyrosine to L-dihydroxyphenylalanine via tyrosine hydroxylase. Subsequently, aromatic amino acid decarboxylase removes a carboxyl group, form neurotransmitter, which is packed into synaptic vesicles. DA is released into the synapse during stimulation, actives dopaminergic receptors, and evokes a response in the postsynaptic cell . It plays a pivotal role in the generation of normal movements by transmission information from SN to the striatum, where movements are initiated and controlled facility and balance .
The pathomechanism of PD is progressive and subsequent degeneration of neurons in SN, which results in the decreased level of DA in the dopaminergic neurons. Further, there is also the presence of Lewy bodies , intracytoplasmic eosinophilic inclusion bodies, in others neurons in SN. The literature indicates that loss of 6070% of dopamine neurons in SN is presented as PD motor symptoms . Pathogenesis of PD involves both environmental and genetic factors. It is thought that the pathways involved in PD are impairment of cellular clearance pathways, protein aggregation, oxidative stress, mitochondria dysfunction, and neuroinflammation .
Figure 1.
Visual Losses In Early
Claudia Feitosa-Santana, Marcelo Fernandes Costa, Henrique Ballalai Ferraz, Luiz Augusto F. Andrade, Ana Laura Moura, Edson Amaro, Russell D. Hamer, and Dora Fix Ventura
Claudia Feitosa-Santana,1,2,3,*Marcelo Fernandes Costa,1,2Henrique Ballalai Ferraz,4Luiz Augusto F. Andrade,5Ana Laura Moura,6,7Edson Amaro, Jr.,5Russell D. Hamer,8and Dora Fix Ventura1,2
1Núcleo de Neurociências e Comportamento, Universidade de São Paulo, São Paulo, Brazil
2Departamento de Psicologia Experimental, Instituto de Psicologia, Universidade de São Paulo, São Paulo, Brazil
3Neurociência para Desenvolvimento Humano, São Paulo, Brazil
4Departmento de Neurologia, Escola Paulista de Medicina, UNIFESP, São Paulo, Brazil
5Hospital Israelita Albert Einstein, São Paulo, Brazil
6Disciplina de Oftalmologia, Faculdade de Medicina do ABC, Santo André, Brazil
7Departmento de Oftalmologia, Escola Paulista de Medicina, UNIFESP, São Paulo, Brazil
8Department of Psychology, Florida Atlantic University, Boca Raton, Florida 33431, USA
- Optics & Photonics Topics?
- Original Manuscript: November 6, 2019
- Revised Manuscript: March 13, 2020
- Manuscript Accepted: March 14, 2020
Genetic Risk Factors For Early
The etiology of EOPD is not completely explained. It seems that genetic factors, environmental factors, or both of them may play an important role in the pathogenesis of this disease. There have been identified several genes and their mutations associated with EOPD, but new loci are still being identified. Most of these genes are inherited autosomal recessive, for example, PRKN, PINK1, or DJ1, but some of them are associated with the autosomal dominant pattern, for example, SNCA
Genes implicated in EOPD and its clinical phenotype .
GBA mutation carriers have significantly younger AOO in comparison to non-carriers . Patients characterize of good or excellent response to L-dopa therapy and present a typical PD phenotype. Furthermore, some of them present impressive to subthalamic nucleus deep-brain stimulation. There are also cases of GBA patients that affect depression . The study of Sato et al. indicates that GBA mutation carriers have a positive history of PD in families. They present poorer motor progression, more often postural instability, persistent asymmetry, and responsive for L-dopa for more than 5 years . According to the literature data, GBA mutations are associated with cognitive impairment, which is revealed by a lower MMSE score . It is considered that patients with both GD and PD present mild Gauchers symptoms .
Also Check: How Fast Does Parkinson’s Progress
Early Onset Vs Late Onset Parkinson’s
Parkinson’s disease ranks among the most common late-life neurodegenerative diseases, affecting approximately 1.5% to 2.0% of the population older than age 60 years. Young onset Parkinsons occurs in 5-10% of people diagnosed while 20% of those affected are under the age of 50.
Regardless of age of onset, we are all united to some extent by a similar life experience that Parkinsons brings but those with YOPD may face very different obstacles, from diagnosis to disease progression and response to treatment to duration of disease those with YOPD must live longer with the complications of this diagnosis.
Not to minimize in any way the challenges that those with late onset disease face diagnosis later in life leads to a number of unique issues as well. So although the diagnosis may be shared, the experience of how this disease manifests may be different in many ways.
YOPD patients are also at increased risk for non-motor symptoms of PD although they have a lower rate of dementia. Early onset patients also suffer an increased rate of dystonia initially and during treatment,
Regarding course of illness, the available evidence suggests that PD patients with a younger age at onset also have a slower disease progression. In one study YOPD patients took significantly longer to reach H& Y Stage 1 from symptom onset compared to late onset patients .
Works Cited
Risk Of Falls May Predict Difficulties With Swallowing Small Study Finds
This study strives to determine phenotypes of speech disorder based on the age of the PD onset, the team wrote.
The study included 24 early-onset patients and 24 late-onset patients , all of whom were newly diagnosed and never had been treated for Parkinsons. There also were matched groups of 24 younger healthy people and 24 older healthy people. Across all groups, slightly more than half the participants were men.
Each of the participants made speech recordings, and the recordings were analyzed with a technique called acoustic analysis, which provides objective, sensitive and quantifiable information for the precise assessment of speech performance from very early stages of PD, the researchers wrote.
Results suggested that, compared to healthy people their age, people with early-onset disease had weak inspirations . Inspirations in early-onset patients were generally similar to those in older individuals, with or without Parkinsons.
These differences based on age at onset may reflect differences in brain damage that occurs in early- and late-onset patients, or may have to do with differing compensatory strategies, the researchers said, noting a need for further research.
Further exploration of the pathophysiologic differences among PD speech phenotypes defined according to the gender and/or different clinical criteria is warranted to shed light on the underlying mechanisms of speech problems in Parkinsons, they concluded.
You May Like: How Does Parkinson’s Disease Affect Homeostasis
Eo Parkinsonism Associated With Other Neurological Symptoms
Dystonia-parkinsonism syndromes
Parkinsonism may be part of the clinical spectrum of syndromes defined as dystonia-parkinsonisms. This term applies to rare conditions where the severity of dystonia usually equals that of parkinsonism. Unlike the parkinsonian syndromes with additional dystonia , these conditions usually have their onset in childhood. The phenotype is often non-specific to a particular form and genetic investigations are required.
DYT-GCH1 typically presents with lower-limb dystonia, causing gait disturbance and a tendency to fall. Clinical features like diurnal fluctuation and sleep benefit are typically associated with this form and can be helpful in differentiating it from other forms of EOPD. The response to levodopa of both dystonic and parkinsonian signs is remarkable with low-doses with no development of the levodopa-induced dyskinesias.
Parkinsonism-ataxia
Parkinsonism, PEO, or optic atrophy
Parkinsonism and spastic paraplegia
Mutations in the SPG11 gene have been identified to be a major cause of autosomal recessive hereditary spastic paraplegia with thin corpus callosum. Juvenile-onset symmetric parkinsonism has been described, with variable response to dopamine intake .
Other SPG syndromes may display parkinsonism as part of the clinical picture, in particular in SPG7 and SPG15 .
Parkinsonism and intellectual disability
Phenotypes associated with mutations in WDR45 have already been discussed .
Parkinsonism and seizures
Bryans Early Onset Parkinsons Diagnosis
Bryan is a 35-year-old nurse, rock climber, husband, and new father to a four-month-old baby boy. He is also someone who is living with YOPD. YOPD is defined as Parkinsons that is diagnosed before the age of 50 and includes about 10% of people living with PD. Younger people will experience the disease differently than those who are diagnosed older, in part due to their different life circumstances. Employment, new relationships, and parenthood add particular challenges that those who are diagnosed older may not have to navigate. When and how to disclose the diagnosis is also of particular concern.
Read Also: Does Agent Orange Cause Parkinson’s
Who Gets Early Onset Parkinsons Disease
About 10%-20% of those diagnosed with Parkinsons disease are under age 50, and about half of those are diagnosed before age 40. Approximately 60,000 new cases of Parkinsons are diagnosed each year in the United States, meaning somewhere around 6,000 12,000 are young onset patients.
Is it genetic or hereditary?
The cause of Parkinsons disease is not yet known. However, Parkinsons disease has appeared across several generations of some families, which could indicate that certain forms of the disease are hereditary or genetic. Many researchers think that Parkinsons disease may be caused by genetic factors combined with other external factors. The field of genetics is playing an ever greater role in Parkinsons disease research, and scientists are continually working towards determining the cause or causes of PD.
Autopsy And Brain Study
All patients are offered autopsy at no cost and are assured that their decision would not impact ongoing care at MDCS. Consent for autopsy was granted by the next-of-kin after death of the patient. The University of Saskatchewan Ethics Board granted approval for the use of the brain for research. Retrieval, preservation and histological preparation of brain tissue has been described elsewhere.Reference Rajput, Fenton and Birdi19 Pathologic studies were performed by qualified neuropathologists. Only those patients with marked substantia nigra neuronal loss and Lewy body inclusions without evidence of other Parkinsonian-related pathology were included.Reference Rajput, Voll, Rajput, Robinson and Rajput31 Other PS variants such as multiple system atrophy and progressive supranuclear palsy were excluded.Reference Rajput, Fenton and Birdi19,Reference Rajput, Rozdilsky and Rajput22,Reference Duvoisin and Goble34,Reference Dickson, Braak and Duda36 Cases that had ablative surgery for PD were also excluded.
Don’t Miss: Is Neuropathy A Symptom Of Parkinson’s
Eo Parkinsonism Associated With Additional Characteristic Features
EO parkinsonism and metals in the brain
Brain metal accumulation can manifest clinically as early-onset parkinsonism in several neurological disorders. Various metals can be accumulated in the brain and other body tissues in these conditions , calcium in Fahrs disease, and manganese in hypermanganesemia). Some of these disorders are genetically inherited, while others are acquired .
Typically, the clinical suspect for these conditions emerges after brain imaging studies . However, associated systemic findings, such as hepatic involvement in Wilsons disease and hypermanganesemia, can be the first clue to suspect metal accumulation in the brain .
Wilsons disease
Wilsons disease is distributed worldwide, with an estimated prevalence of 1 case per 30,000 live births in most populations . However, in some isolated populations, such as a small mountain village on the island of Crete, the prevalence is much higher , due to high rates of consanguinity .
Copper accumulation is associated with a progressive neurodegeneration of basal ganglia leading to a complex movement disorder often associated with bulbar symptoms. The movement disorder is usually characterized by tremor, dystonia, and/or parkinsonism. Bulbar symptoms consist of dysarthria, drooling and/or dysphagia. In addition, a range of additional neurologic features may be present, including cerebellar ataxia, chorea, hyperreflexia, seizures, cognitive impairment, and psychiatric features .
Fahrs disease
Mr Data Acquisition And Preprocessing
All MR data were obtained on a 3.0 T MRI scanner . High-resolution T1-weighted transverse images were acquired as a volumetric three-dimensional magnetization-prepared rapid gradient-echo sequence . Functional images were obtained by echo-planar imaging . Participants were instructed to remain relaxed with their eyes closed but without falling asleep during the scan a foam cushion was used to reduce head movement and participants wore earplugs to minimize noise.
Data preprocessing was carried out using the Resting-State fMRI Data Analysis Toolkit v1.21 1 as previously described . Briefly, the first 10 time points from each subjects series were discarded this was followed by realignment and correction for head motion , co-registration between T1 and EPI images, spatial normalization to a standard Montreal Neurological Institute template, and voxel resampling to a voxel size of 3 × 3 × 3 mm3. Linear trends and nuisance signals were removed, followed by denoising and bandpass filtering.
Also Check: How To Stop Parkinson’s From Progressing
What Is Early Onset Parkinsons Disease
When someone who is 21-50 years old receives a diagnosis of Parkinsons disease, it is referred to as early onset Parkinsons disease, or young onset Parkinsons disease . While the symptoms of the disease are mostly the same at whatever age it develops, younger people will experience the disease differently due to their unique life circumstances. Managing the disease can be particularly challenging for a younger person and their family from a medical, psychological and social standpoint.
Differences In Global Synchronization
DC was increased in the left superior frontal gyrus , precuneus, and decreased in bilateral Rolandic operculum and left insula of EOPD patients compared to YC subjects . DC was increased in the right cerebellum-crus1 and decreased in the right putamen, mid-cingulate cortex, bilateral Rolandic operculum, and left insula of the LOPD group compared to the OC group . Table 2 lists the local maxima of DC values determined with the two-sample t-test.
Figure 1. Comparison of degree centrality between EOPD and YC groups. DC was increased in the left superior frontal gyrus , precuneus, and decreased in bilateral Rolandic operculum and left insula in the EOPD group .
Figure 2. Comparison of DC between LOPD and OC groups. DC was increased in the right cerebellum-crus1 and decreased in the right putamen, mid-cingulate cortex, bilateral Rolandic operculum, and left insula in the LOPD group .
Table 2. Degree centrality analysis of altered brain regions in functional magnetic resonance imaging in early- and late-onset Parkinson disease patients and sex-and age-matched healthy control subjects*.
Read Also: What Tests Are Done To Diagnose Parkinson’s
Why Is Distinguishing Young
Socially, people who are affected by PD at a younger age experience the disease differently they may be at a different stage of their career and often have less time to engage in their own care. They may also have children or are planning to have children and have questions regarding passing on PD genes.
Medically, doctors tailor treatment when it is a younger person with PD. The younger you are, the more likely the disease is genetic. Your care team may offer genetic testing or counseling. Younger brains also have a higher neuroplasticity potential which allows the brain to handle and respond to disease and therapy differently.
The Plus Side Of An Early Diagnosis
The news is not nearly all bad for those with young-onset Parkinsons. For one thing, patients with YOPD are better candidates for surgical procedures and medical innovations being used or developed to treat Parkinsons disease. For another, younger patients are less likely to be coping with other health problems at the same time.
You May Like: Is Parkinson’s Disease Hereditary Or Genetic
A Practical Approach To Early
Article type: Review Article
Authors: Riboldi, Giulietta M.a * | Frattini, Emanueleb c | Monfrini, Edoardob c | Frucht, Steven J.a | Di Fonzo, Alessiob
Affiliations: The Marlene and Paolo Fresco Institute for Parkinsons and Movement Disorders, Department of Neurology, NYU Langone Health, New York, NY, USA | IRCCS Ca Granda Ospedale Maggiore Policlinico, Neurology Unit, Milan, Italy | Dino Ferrari Center, Neuroscience Section, Department of Pathophysiology and Transplantation, University of Milan, Milan, Italy
Correspondence: Correspondence to: Giulietta M. Riboldi, The Marlene and Paolo Fresco Institute for Parkinsons and Movement Disorders, Department of Neurology, NYU Langone Medical Center, 222 East 41st Street, 13th Floor, New York, NY 10017, USA. Tel.: +1 212 263 4838 Fax: +1 212 263 4837 E-mail: .
Keywords: Parkinsonian disorders, Parkinsons disease, autosomal recessive early-onset, secondary Parkinsons disease, dopa-responsive dystonia, adult-onset dystonia-parkinsonism, genetic counseling
DOI: 10.3233/JPD-212815
Journal: Journal of Parkinson’s Disease, vol. 12, no. 1, pp. 1-26, 2022
Abstract
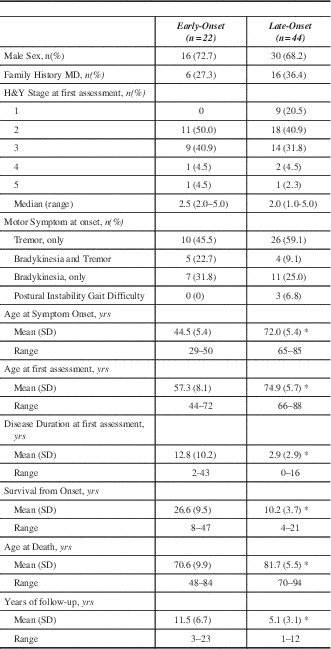
Demographics And Clinical Characteristics Of The Study Population
Demographic and clinical characteristics of the study population are shown in Table 1. Apart from median age and age of onset, EOPD and LOPD groups had similar profiles including disease duration and severity and clinical assessment scale scores. The HDS scores of EOPD and LOPD patients were higher than those of the respective age-matched control groups , whereas no significant differences were observed in terms of age, sex, education level, DLED, and MMSE score.
Don’t Miss: Do Parkinson’s Patients Have An Odor
Whats Different About Young
The age of diagnosis matters for a variety of reasons, from probable causes of early cases to symptoms and treatment:
- Genetics. As with any case of Parkinsons disease, the exact cause is usually unknown. That said, The young-onset cases of Parkinsons disease are, on average, a bit more likely to be familial or genetic, says Gregory Pontone, M.D., director of the Johns Hopkins Movement Disorders Psychiatry Clinic.
- Symptoms. In many patients with YOPD, dystonia is an early symptom. People with YOPD also report more dyskinesia . They also tend to exhibit cognitive problems, such as dementia and memory issues, less frequently.
- Progression. Patients with young-onset Parkinsons appear to have a slower progression of the disease over time, says Pontone. They tend to have a milder course, staying functional and cognitively intact for much longer.
- Treatment. Most patients with Parkinsons take the medication levodopa. However, other drugs, such as MAO-B inhibitors, anticholinergics, amantadine, and dopamine receptor agonists, may be used before levodopa.
Treatment For Young Onset Parkinsons
To date, there is no known cure or way to prevent Parkinsons disease. However, research is ongoing and remarkable progress is being made. There is very real hope that the causes, whether genetic, environmental, or some combination of the two, will soon be identified and the precise effects of these causes on brain function will be understood. Although there is no cure for the disease at this time, by identifying symptoms and determining a proper course of treatment, most people with the disease are able to remain active and lead fulfilling lives.
Are there doctors who specialize in Parkinsons disease?
Doctors who are specially trained to diagnose and treat conditions of the brain and nervous system are called neurologists. Some neurologists have a subspecialty in movement disorders and work extensively with patients who have Parkinsons disease and other similar conditions. These doctors also may have experience dealing with early onset Parkinsons symptoms. You can ask your physician if they have specific experience with younger patients, or whether they can refer you to a doctor who does.
How do I find a Parkinsons disease specialist?
Early Onset Resources
You May Like: What Do Patients With Parkinson Die From
