On And Off Periods With Parkinsons
As your Parkinsons progresses over the years, you will probably start to notice even though youre still taking your carbidopa-levodopa regularly, you experience periods where its working effectively and then periods where the medication seems to not be working . When youre on, you should feel like you can move more normally, with less tremor, stiffness and/or slowness. And then when youre off, all those stiff, rigid, slow movements and your tremor return, almost as if your medications have decided to stop working. Frustratingly, it can be hard to predict exactly how long your on and off periods will last.
Off periods are a result of the disease progressing and becoming harder to control through medication. When you first start medication, its common to go through a honeymoon period of several years, where its working well and you can hardly tell you have Parkinsons.23 Then, as the condition progresses, your body produces less dopamine, making you more dependent on your dopamine-replacement medication. Over time this leads to more and more instances where the medication is supposed to kick in, or supposed to last for several hours, but is less effective.31
Related: This story explains what it feels like to be on.
How To Help Reduce Episodes
Off times become more common after people with PD have been taking medication for a longer time and as their disease progresses. While the presence of off times happens as a normal progression of PD, there are things that can help manage or reduce these episodes:
Side Effects Of Taking Carbidopa/levodopa
I am newly diagnosed with Parkinsons disease and just started on carbidopa/levodopa. However, I feel that the medication is making me feel worse than my original symptoms. Can carbidopa/levodopa make PD worse?
Carbidopa/levodopa can definitively have an array of side effects such as nausea, fatigue and dizziness. Your neurologist will try to find a dose that helps your PD symptoms, but does not cause side effects. Carbidopa/levodopa is probably not making your PD worse per se, but it sounds like overall, you are feeling worse on this dose than you did on no medication. You should discuss this problem with your neurologist who may consider changing your medication dosage.
My husband has had PD for about 10 years. Lately he has been having significant body, arm and finger movements after a dose of levodopa which improve just before the next dose. Is there any treatment for these abnormal movements?
I was advised to take my carbidopa/levodopa at least 30 minutes after a meal. However, this caused a lot of nausea and stomach upset for me, so I now take the medication with meals which is much better for me. Is this OK to do?
I noticed that I have increased trouble with my symptoms when I eat a meal containing protein. How do I adjust my diet to accommodate this?
Dietary protein can interfere with carbidopa/levodopa absorption in some people. This is known as the protein effect. The two ways to adjust your diet is to:
Are There Any Possible Long
As with any medication, there can be long-term effects, although not every person who takes the medication will experience them. Each medication comes with an information leaflet which outlines possible effects so make sure that you read this. If you have any concerns, please discuss these with your doctor, health professional or pharmacist.
See also Managing medication.
Advantages Of Comt Inhibitors
When used with , COMT inhibitors can reduce the daily off time and increase the on time.
In many cases, the dose and frequency of levodopa can also be reduced.
The terms on/off or motor fluctuations refer to the period when people can no longer rely on the smooth and even symptom control that their drugs once gave them.
So Why Is Finding A Cure So Difficult
In the 1960s, when levodopa was first discovered, it was heralded as a cure for Parkinsons. Researchers had identified that Parkinsons symptoms were due to a lack of dopamine in the brain and had discovered a treatment that replaces this missing chemical messenger. For the first time, they had a drug with the ability to reduce and relieve symptoms of the condition. Today, levodopa is still the gold standard for Parkinsons treatment. When it comes to effective medical treatment it is actually very good, particularly in the early stages.
However, no current Parkinsons medication could be called a cure. Despite numerous improvements that have been made over the last 50 years, which make these drugs more effective and longer lasting, in the long term, these medications fail to completely relieve the symptoms of Parkinsons. The condition continues to have an ever-increasing impact on quality of life and, for many of the 145,000 people in the UK with Parkinsons, is a battle that is fought every day. Additionally, there are many symptoms, particularly non-motor symptoms like sleep problems, anxiety and pain, that are not adequately controlled by any medication. And these too progress as the condition becomes more severe.
When it comes to slowing Parkinsons, we can slow the progression of symptoms with exercise, but research has yet to provide a treatment that stops further damage to the brain. But the reasons why are actually quite simple, and can be overcome.
Tips For Dealing With Morning Akinesia
Depending on the severity of your Parkinsonian symptoms, morning akinesia can make it difficult to dress, bathe, use the toilet and prepare breakfast for yourself. Here are some tips to help you deal with morning akinesia and the worsening of PD symptoms:
Most patients who experience morning akinesia are in the advanced stages of Parkinson’s disease, meaning their Parkinson’s symptoms are more pronounced. At this point, your doctor may suggest a different combination of medicines or see if you are eligible for surgery. If you know your Parkinsonian symptoms are worse in the morning, it’s important to seek the help you need to take care of yourself and stay safe.
APA ReferenceSmith, E. . Why Parkinsonian Symptoms Can Worsen During the Day, HealthyPlace. Retrieved on 2021, August 11 from https://www.healthyplace.com/parkinsons-disease/symptoms/why-parkinsonian-symptoms-can-worsen-during-the-day
What Are The Most Common Medicines Used To Treat Pd
Sinemet
Levodopa is the most commonly prescribed and most effective medicine for controlling the symptoms of PD, particularly bradykinesia and rigidity.
Levodopa is a chemical found naturally in our brains. When given as a medicine, it is transported to the nerve cells in the brain that produce dopamine. It is then converted into dopamine for the nerve cells to use as a neurotransmitter.
Sinemet is made up of levodopa and another drug called carbidopa. Levodopa enters the brain and is converted to dopamine while carbidopa prevents or lessens many of the side effects of levodopa, such as nausea, vomiting, and occasional heart rhythm disturbances. It is generally recommended that patients take Sinemet on an empty stomach, at least hour before or one hour after meals.
There are two forms of Sinemet: controlled-release or immediate-release Sinemet. Controlled-release Sinemet and immediate-release Sinemet are equally effective in treating the symptoms of PD, but some people prefer the controlled release version. Ask your doctor which approach is best for you.
Dopamine agonists
Dopamine agonists are medicines that activate the dopamine receptor. They mimic or copy the function of dopamine in the brain.
Parlodel, Requip, and Mirapex are all dopamine agonists. These medicines might be taken alone or in combination with Sinemet. Generally, dopamine agonists are prescribed first and levodopa is added if the patient’s symptoms cannot be controlled sufficiently.
Symmetrel
What Does Current Guidance Say On This Issue
The NICE guideline recommends levodopa as a first-line treatment in the early stages of Parkinsons to control problems with movement if symptoms are affecting the quality of life. It does not discuss delayed treatment with levodopa.
If motor symptoms are not affecting the quality of life, the guideline recommends considering other drugs such as dopamine or monoamine oxidase inhibitors based on individual circumstances and preferences.
Common Drugs For Parkinson’s Disease
Levodopa and carbidopa . Levodopa is the most commonly prescribed medicine for Parkinsons. Its also the best at controlling the symptoms of the condition, particularly slow movements and stiff, rigid body parts.
Levodopa works when your cells change it into dopamine. Thats a chemical the uses to send signals that help you move your body. People with Parkinsons dont have enough dopamine in their brains to control their movements.
Sinemet is a mix of levodopa and another drug called carbidopa. makes the levodopa work better, so you can take less of it. That prevents many common side effects of levodopa, such as , vomiting, and irregular rhythms.
Sinemet has the fewest short-term side effects, compared with other Parkinsons medications. But it does raise your odds for some long-term problems, such as involuntary movements. An inhalable powder form of levodopa and the tablet have been approved for those experiencing OFF periods, OFF periods can happen when Parkinsons symptoms return during periods between scheduled doses of levodopa/carbidopa.
People who take levodopa for 3-5 years may eventually have restlessness, confusion, or unusual movements within a few hours of taking the medicine. Changes in the amount or timing of your dose will usually prevent these side effects.
Dopamine agonists. These drugs act like dopamine in the . They include , , and , .
( may help people with mild Parkinson’s disease.
Increased Feelings Of Anxiety Or Depression
Anxiety and depression have been linked to Parkinsons. In addition to movement problems, the disease can also have an impact on your mental health. Its possible that changes in your emotional well-being can be a sign of changing physical health as well.
If you are more anxious than usual, have lost interest in things, or feel a sense of hopelessness, talk to your doctor.
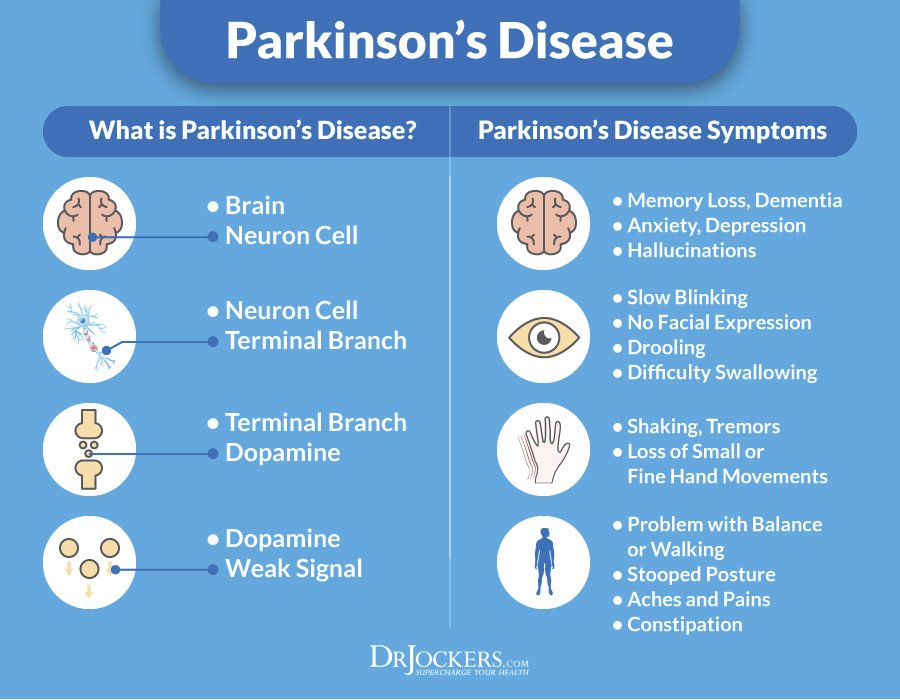
Causes Of Parkinsons Disease
At present, we do not know the cause of Parkinsons disease. In most people there is no family history of Parkinsons Researchers worldwide are investigating possible causes, including:
- environmental triggers, pesticides, toxins, chemicals
- genetic factors
- combinations of environment and genetic factors
- head trauma.
Advice For Nursing Care
People with Parkinsons have specific needs and care requirements. Most important is that they receive their medication on time, every time. Nurses should also be aware of the on/off nature of the condition.
Some patients say they are on when their drugs are working and symptoms are mostly under control. If they go off, their symptoms are not under control and it becomes harder for them to move; some may stop moving altogether. Patients might change from on to off very quickly, like a switch.
The way in which Parkinsons affects patients can vary from hour to hour and day to day, and it also varies widely between individual patients. The amount of help and support they need also varies. Nurses should therefore listen to patients and their families about how the condition affects them.
It is important to ensure that patients have access to a varied and balanced diet; nurses should take account of any swallowing or movement problems that could lead to malnutrition. It is also important to remember to give patients time to answer when talking to them. It may take them time to respond, but this does not mean they are not listening or do not understand.
Choosing The Best Treatment Plan For You
As you may know, medications are the backbone of the Parkinsons treatment plan. But because the disease affects everyone differently, and each persons response to therapy will vary, there is no hard-and-fast rule about when you should begin taking medication and what to take first. Some doctors prescribe medication upon diagnosis. Others believe that drugs, especially levodopa, should be delayed as long as possible to avoid earlier onset of medication-related side effects.
Your involvement from the very start is important because you want to be sure your doctor is addressing your individual needs. When your doctor writes a new prescription, or makes a change to an existing one, take the opportunity to ask for an explanation. If her response goes something like, I always start my Parkinsons patients on X dosage of Y, a dopamine agonist, you might want to consider switching to a movement disorders specialist, a neurologist who has had special training in Parkinsons disease and other movement disorders.
How Long Before Levodopa Stops Working In Parkinsons Disease
is a drug combination that works to reduce symptoms in Parkinson’s disease for as long as a patient takes it. Put simply, levodopa converts into dopamine in the brain, helping to control movement, while carbidopa prevents the breakdown of levodopa in the bloodstream so more levodopa can enter the brain. Carbidopa can also reduce nausea and vomiting, common levodopa side effects. As the underlying disease progresses and symptoms get worse, patients may need to increase their dose or take levodopa more frequently to experience the same reduction in symptoms.
After taking levodopa for some time, typically a few years, patients may begin to experience a wearing off period, when symptoms return before it’s time for their next dose of levodopa. This is also referred to as “off time. Off time is common, and according to patient surveys, around half of patients who take levodopa report experiencing wearing off periods. Of those patients, 25% experience it 3 to 6 hours per day, and 52% have symptoms for 1 to 3 hours a day.
“Off” time can last anywhere from 15 minutes to several hours, depending on your current medication dosage. Talk to your doctor if you’ve noticed that your symptoms, such as tremors, return before it’s time for your next dose. There are a few adjustments that can help, including increasing your dosage, changing medications, and adjusting protein intake.
Build A Unique Schedule
Establish a method and process to create and communicate the patients individualized medication schedule in order to control symptoms throughout the day. This requires clear communication between the patient-care unit and the pharmacy so patient-specific schedules are not overridden with standard dosing schedules.
We Dont Fully Understand The Causes
If we are to design a treatment that stops the condition at its source we really need to know why brain cell death happens in the first place.
In history, blind luck has led scientists to stumble upon effective treatments for conditions like smallpox and infections that are responsive to penicillin. But for a condition as complex as Parkinsons we should invest in research that fills in our incomplete view of what is happening inside the brain as it will give us the best chance of developing treatments that tackle the underlying causes of brain cell loss. Fortunately, there are some extremely talented and dedicated researchers, working with cutting-edge science and technology, trying to better understand Parkinsons and they are making new discoveries all the time.
Incidence Of Parkinsons Disease
Its estimated that approximately four people per 1,000 in Australia have Parkinsons disease, with the incidence increasing to one in 100 over the age of 60. In Australia, there are approximately 80,000 people living with Parkinsons disease, with one in five of these people being diagnosed before the age of 50. In Victoria, more than 2,225 people are newly diagnosed with Parkinsons every year.
Other Medication Safety Concerns
Even with correct administration timing based on the patients home medication schedule, dosing errors have been reported with carbidopa/levodopa. The drug is available in many different strengths and forms, from an orally disintegrating tablet to extended- and immediate-release formulations. Levodopa, which converts to dopamine in the brain, can cause episodes of acute psychosis and dyskinesia when given in large doses, which can unnecessarily extend hospitalization. Also, patients may take different strengths of carbidopa/levodopa each time throughout the day, increasing the risk for errors. Documenting a complex scheduleeven if well understoodmay be difficult and even more challenging in some electronic health records.
Dysphagia is another manifestation of Parkinsons disease and can affect the patients ability to swallow medications. The symptoms include frequent coughing while drinking and taking medications and a gurgling voice.
Many Don’t Manage Off Time Well
In the Parkinsons Disease in America 2017 survey, 80% of people with PD reported they currently use a carbidopa/levodopa therapy to treat their symptoms. Carbidopa/levodopa treatment is the most effective treatment available for the management of motor symptoms of PD.
However, half of the survey respondents who use carbidopa/levodopa therapy are experiencing off times. Twenty-five percent of those experiencing off times notice their symptoms for 3 to 6 hours a day.
Another 52% report 1 to 3 hours a day when their symptoms are noticeable and affecting their daily activities. Yet 43% of those experiencing an off time report that they dont take any action to manage these episodes.
What Could Help Me To Manage My Medication Better Eg Pill Dispensers Dosing Alarms Etc
![Neural Stem Cell Therapy for Parkinsons Disease [PD]](https://www.parkinsonsinfoclub.com/wp-content/uploads/neural-stem-cell-therapy-for-parkinsons-disease-pd.jpeg)
If you have a number of different medications to take throughout the day, you may find it helpful to use a timer, rather like an alarm clock, which will remind you take another dose.
You can also buy various types of tablet organisers that have a compartment for each day which can be very useful to keep with you if you are going out. For advice on this speak to your pharmacist or look online, for example theDisabled Living Foundation website or commercial companies such as.
See alsoManaging medication.
Looking Out For Side Effects If You’re A Carer
If youre a carer of someone with Parkinsons, medication side effects can be difficult and tiring to cope with.
It may be that the person having side effects such as hallucinations and delusions or impulsive and compulsive behaviour does not realise they are experiencing them.
Its important to seek help from your specialist as soon as you can.
Why Parkinsonian Symptoms Can Worsen During The Day
Parkinsonian symptoms can get worse at certain times, and many people have good days and bad days with Parkinson’s disease. While symptoms can fluctuate naturally, patients can also experience periods where their medication doesn’t work as effectively as usual, typically when they’ve been taking it for a long time. Some people with Parkinson’s disease find that their symptoms are worse due to the decreased effects of levodopa medication that occur over time. Lets look at why this happens and explore ways to treat daytime Parkinsonian symptoms.
Do I Need To Take Medication How And When Should I Take It
In the beginning, a single medication or a combination of different medications can be used with medical treatment being started in low doses and increased gradually. Medication is always individual and can vary greatly between people. Therefore, medical treatment requires follow-up by a physician with a good knowledge of the condition.
Your doctor will be on hand to advise when to take your medication so that it works best for you, for example before, with or after eating, whether you should take with or without protein etc. By working closely with your doctor, you will be able to find the right balance and combination of medications to suit you. It is important that you monitor your response to the medication regularly so that medicine remains as effective as possiblein managing your symptoms. Again, if you are unsure or do not understand everything the doctor has told you, please ask him or her to explain again as it is important for you to follow the advice you are given accurately.
Some people find that combining medication with conventional therapies such asphysiotherapy,occupational therapyandspeech and language therapy, as well as surgical treatments or complementary therapiessuch asaromatherapy,reflexology,yoga,tai chi is helpful. But if you are considering these therapies it is always advisable to discuss with your doctor first.
See also:
See also and .
Quantitative Electromyographic Analysis Of Reaction Time To External Auditory Stimuli In Drug
1Department of Neurology, Korea University College of Medicine, Ansan Hospital, 516 Gojan-1-dong, Danwon-gu, Ansan-city, Gyeonggi-do 425-707, Republic of Korea
2Department of Physical Medicine & Rehabilitation, Korea University College of Medicine, Ansan Hospital, 516 Gojan-1-dong, Danwon-gu, Ansan-city, Gyeonggi-do 425-707, Republic of Korea
3School of Biomedical Engineering, Konkuk University, Seoul, Republic of Korea
4Department of Control and Instrumentation Engineering, Korea University, Seoul, Republic of Korea
Academic Editor:
Abstract
1. Introduction
2. Methods
2.1. Subjects and Methods
2.2. RT Measurements Using Surface EMG
2.3. Data Analysis
3. Results
| Control ( |
| Mean latency ± SD |
4. Discussion
4.1. Correlation of RT and Clinical Data in Patients with PD
Conflict of Interests
Side Effects And Problems With Levodopa
In the early days of taking levodopa, you may feel sickness or nausea. In most people this will pass as your body adjusts to the medication.
Overtime as Parkinsons the levodopa dose will need to be adjusted. Many people will become more aware that symptoms sometimes return between doses of medication. This is called wearing off and is a sign your dose needs to be adjusted.
As levodopa is absorbed through the gut, or other stomach problems may impact on uptake of the medication. In some people who have had Parkinsons for sometime extra involuntary movements can occur. Your neurologist will be able to help adjust medications to minimise dyskinesia.
Other side effects may include:
- Confusion
- Psychological changes
- , fainting or dizziness
Side effects of levodopa can sometimes be improved by changing your dose, the form of the drug or how often you take it. If this doesnt work, other types of drug may be combined with levodopa.
Speak to your GP or specialist about the right treatment for you.
Managing Medication Interactions And Side Effects
All prescribed medications can have potential side effects, including those used to treat Parkinsons. Some things you think are of Parkinsons may actually be side effects of medication. Some peoples side effects will have a big impact on their lives and have to be kept under control along with the symptoms.
Taking A Closer Look At Your Options
Since the drug levodopa was synthesized in the 1960s, levodopa in combination with carbidopa , has been the gold standard for treating the symptoms of Parkinsons. However, after several years of taking this medication some people experience dyskinesias, or involuntary writhing movements. This is sometimes referred to as levodopa-induced dyskinesias or LIDS. The fear of these side effects has led many clinicians and patients to avoid levodopa-carbidopa for as long as possible.
But some experts do not believe this levodopa phobia is warranted . In short, they say that levodopa can be considered as a potential first-line therapy in all age groups—although caution should be exercised in younger patients. In most cases, the dosage will start low then increase slowly, often in combination with other medications, to adjust to a persons changing condition.
Other first-line medications that can be used to control Parkinsons symptoms include drugs known as dopamine agonists and monamine oxidase inhibitors. Dopamine agonists provide relief by mimicking the action of dopamine within the brain, and monamine oxidase inhibitors help maintain motor control by slowing the breakdown of dopamine within the brain. These drugs can help younger patients buy some time before starting levodopa-carbidopa.
