Can Head Injury Cause Parkinsons Disease Understanding The Link Between Tbi And Parkinsonism
Can head injury cause Parkinson’s Disease? And does a traumatic brain injury increase a person’s chances of developing Parkinson’s?
Although it is rare for a head injury to cause Parkinson’s, it is a possible secondary effect you should be aware of.
Head injuries can also trigger certain movement disorders that look similar to Parkinson’s Disease but are in fact different.
Today you will learn more about the link between brain injury and Parkinson’s Disease. Then, at the end, we’ll show you how to treat Parkinson’s and other motor problems after head injury.
Natural Remedies And Treatments For Parkinsons Disease That Get Powerful Results
To successfully treat the symptoms of Parkinson’s, andeven reverse this disorder, there are 4 things you must do…
a) Increase your natural dopamine levels
b) Detox your body of all heavy metals andpollutants
c) Reduce all inflammation in the body,especially the brain
d) Repair the neuro pathways
These 10 natural treatments and remedies do all four. Solet’s not waste any more time then. Here they are in order of importance…
How Can I Support Someone With Parkinson’s At The Advanced Or Palliative Stage
In the advanced stages of Parkinson’s, your patient’s care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the ‘whole person’ to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinson’s may be supported by a number of professionals, including a Parkinson’s nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinson’s also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinson’s should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the person’s wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesn’t want to have in the future – this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
Dr Jay Alberts Discovers The Magic Of Forced Exercise For Parkinsons Patients
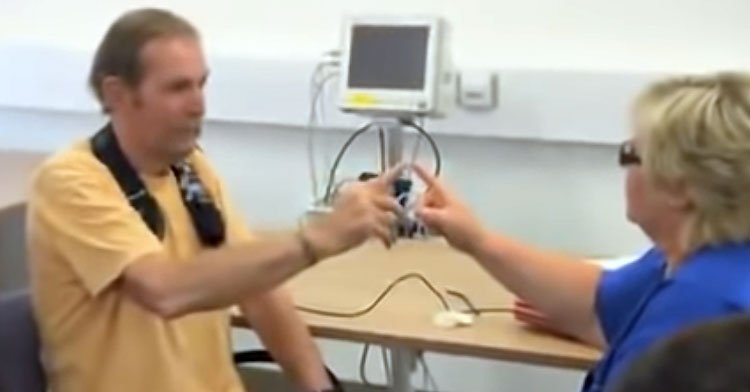
In 2003 Dr. Jay Alberts rode the Des Moines Register’s Annual Great Bike Race Across Iowa with his friend Cathy, who has Parkinson’s disease. Dr. Alberts rode the front of a tandem bicycle with Cathy pedaling behind him. Cathy remarked, “for this week it did not feel like I had Parkinson’s.” After several days of riding, Dr. Alberts noticed that Cathy’s motor control, most notably her handwriting, had improved. This set him on a path toward groundbreaking research on the benefits of forced exercise for Parkinson’s patients.
When the effects of exercise are tested in animal models of Parkinson’s, the exercise is often “forced,” meaning that the animal is forced to exercise at a more intense level than they would choose to on their own. Researchers have found that this forced exercise is far more effective than voluntary exercise in stimulating the release of neurotrophic factors and enhancing neurogenesis. Researchers suggest that “contradictory results in human and animal studies are caused by differences between voluntary versus forced exercise …patients with PD may not be able to exercise at sufficiently high rates to trigger the endogenous release of the neurotrophic factors thought to underlie global improvements in motor function.”
Q Other Than Difficulties With Movement Are There Any Other Physical Symptoms

A. Other problems – so called ‘non-motor symptoms’ – are common and can have a major effect on quality of life. These symptoms can occur at any stage of the condition and can even start before movement symptoms are noticed.
Non-motor symptoms include:
- sensory symptoms , which occur in up to 40 per cent of people with the disease;
- tiredness not relieved by resting ;
- sleep problems , which affect about 70 per cent of people;
- constipation, which is due to the digestive tract slowing down and decreased mobility;
- bladder problems that can result in needing to urinate urgently and/or more often, urinary incontinence or difficulty urinating;
- orthostatic hypotension , which causes a sudden fall in blood pressure when changing positions – usually standing up – causing fainting ; and
- depression and anxiety, which are not just due to having a chronic illness but are part of the disorder.
Constipation , urinary problems and sleep problems can be made worse by some of the medicines used to treat Parkinson’s disease.
Naturaltreatment For Parkinsons #9 Exercise And Other Alternative Therapies:
Regular exercise has been shown to help Parkinson’ssufferers by reducing muscle stiffness, increasing mobility, and enhancing postureand balance. Exercise also increases oxygen levels and neurotransmitters, alongwith releasing potent “mood elevating” chemicals called endorphins.
The type of exercise performed for PD is crucial. Aqua orwater aerobics can be particularly useful as traditional exercise is usuallyquite difficult for many Parkinson’s sufferers. Muscle decline, loss of strength,stiffness and loss of balance can make conventional exercises difficult toperform. The great thing about aqua aerobics is it still has the same benefits as other exercise regimens,but the risk of falling is eliminated.
Other types of exercises that can be beneficial for PDsufferers include Tai Chi, Yoga, dancing, walking, aerobic/jazzercise classes,and general stretching.
For more information on the different exercise programsavailable for Parkinson’s patients, you can check out this website… Exercise and Physical Therapy for Parkinson’sDisease
Q What Are The Different Types Of Medicines Used To Treat Parkinsons Disease
A. Because the symptoms of Parkinson’s disease are caused by a lack of dopamine in the brain, most drug treatments — so-called ‘antiparkinsonian medications’ — are aimed at replacing dopamine, prolonging its action or acting like dopamine.
Levodopa, also known as L-dopa, is the most effective medication available, improving symptoms in more than 80 per cent of people within 6-8 weeks. Levodopa is converted into dopamine by nerve cells in the brain. To prevent it from being converted to dopamine before it reaches your brain, it needs to be given in combination with another medication . These combination medications are called Sinemet and Madopar, respectively.
Other medicines available for the treatment of Parkinson’s disease include dopamine agonists, MAO-B inhibitors, COMT inhibitors, anticholinergics and amantadine. Although these medications are generally not as effective as levodopa, they do benefit some people. They are especially useful if levodopa is causing intolerable side effects or isn’t controlling symptoms on its own. These medicines are often used as initial therapy to control relatively mild symptoms, especially in younger patients.
A range of treatments is also available for non-motor symptoms such as depression, sleep problems, constipation and sexual dysfunction.
Whats The Difference Between Progressive Supranuclear Palsy And Parkinsons
People with PSP generally progress more rapidly than people with Parkinson’s. A person with Parkinson’s tends to lean forward while a person with PSP tends to lean backward. Tremors are common in people with Parkinson’s and rare in people with PSP. Speech and swallowing abnormalities are more severe and show up sooner in those living with PSP.
For more information on progressive supranuclear palsy, read this fact sheet and insights from the CurePSP organization website.
Q Are There Any Problems Associated With Using Levodopa In The Long Term
A. The use of medications means that most people with Parkinson’s disease can expect many years of active living. Unfortunately, the initial positive response to levodopa does not always last — its effects often become unpredictable, and various side effects start to appear after about 5 years of treatment. The main side effects associated with long-term levodopa therapy are dyskinesias and the ‘wearing-off’ effect.
Dyskinesias are involuntary twitching and jerking movements of the head, face and limbs. These uncontrolled movements are the most common adverse effect of prolonged levodopa therapy. Taking a lower dose of levodopa or combining levodopa with another antiparkinsonian medication — a dopamine agonist — may improve the problem of dyskinesia.
The ‘wearing-off’ effect, or end-of-dose failure, refers to a decrease in the length of time that each dose of levodopa controls symptoms. This results in periods of impaired movement that abruptly alternate with periods of improved mobility.
Taking smaller, more frequent doses of levodopa or controlled-release levodopa can help. There is a formulation of levodopa plus carbidopa that can be used in people with more advanced Parkinson’s disease who have severe fluctuations in response to levodopa. The medicine is a gel that is given directly to the small intestine via a feeding tube. By giving the medicine continuously through a feeding tube, the amount of medicine in the body is constant, reducing the wearing-off effect.
Natural Treatment For Parkinsons #3 Turmeric And Otherherbs And Spices:
A recent study published in the journal Stem Cell Research & Therapy, foundthat the extracts in turmeric, particularly curcumin and the newly discovered Ar-turmerone,can regenerate “a damaged brain” and reverse neurological disorders. Researchers said Ar-turmerone is “a promising candidate to supportregeneration in neurologic disease.” Michigan State University researcherBasir Ahmad also found that a compound in turmeric may help fight Parkinson’sdisease by disrupting the proteins responsible for the disease.
Another study published in the Pharmacognosy Magazine found that tumeric can prevent and evenreverse the toxic effects exerted on the brain from fluoride exposure. Fluorideis a nasty and dangerous heavy metal that destroys brain cells and the intricateworkings of the central nervous system. Fluoride poisoning has also beenimplicated in the development of neurological diseases such as Alzheimer’s,Parkinson’s, ALS and multiple sclerosis. 7
Turmeric is also a very potent anti-inflammatory spice. Because Parkinson’s is aninflammation type disease, turmeric will help immensely. A heaped teaspoon ofhigh quality turmeric powder taken 3 times daily in asmoothie will do the trick. Just make sure you combine it with 10-12 blackpeppercorns for enhanced absorption Turmeric is also fat soluble so you’ll need tocombine it with some coconut oil, red palm oil or fish/krill oil as well.
Neurogenesis In The Substantia Nigra And Promising Stem Cell Treatments
In last week’s post I explained that Parkinson’s disease is a degenerative neurological condition in which dopaminergic neurons in a part of the brain called the substantia nigra die off. Other parts of the brain suffer neurodegeneration as well, causing some of the non-motor symptoms of Parkinson’s. I’ll now discuss promising research about neurogenesis as it applies to Parkinson’s disease; if you’re not familiar with neurogenesis, I encourage you to read this post.
In 2003, scientists in Sweden demonstrated that neurogenesis occurs in the substantia nigra of adult mice. Their research showed that the type of dopaminergic neurons lost in Parkinson’s disease are actually regenerated throughout life. While the rate of neurogenesis in the substantia nigra is slower than in the hippocampus, if the rate of neural turnover is constant, the entire population of dopaminergic neurons in the substantia nigra could be replaced during the lifespan of a mouse. The study showed that not only does neurogenesis in the substantia nigra occur, but the newborn neurons are then integrated into neural circuits.
One of the study authors notes that the reprogrammed cells would probably be damaged by whatever caused Parkinson’s in the first place. In cell transplants for other health conditions, disease tends to catch up with transplanted cells in 15-20 years. Treatments to enhance endogenous neurogenesis will likely buy Parkinson’s patients important time, but they may need to be repeated.
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage
Parkinson’s progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinson’s about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinson’s may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more ‘off’ periods – when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinson’s symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinson’s most often die because of an infection or another condition, usually caused by Parkinson’s.
This Is How You Can Recognise The First Symptoms Of Parkinsons Disease
Parkinson’s disease is a very complex disease that can have a lot of different symptoms. Two different types of symptoms can often be distinguished: symptoms related to the motor system and non-motor symptoms like depression. The symptoms can also differ strongly from person to person, so not everyone with Parkinson’s disease experiences the same ones.
This is how you can recognise Parkinson’s disease.
Whats The Difference Between Dementia With Lewy Bodies And Parkinsons
In dementia with Lewy bodies, dementia always appears first. There can also be changes in alertness as well as visual hallucinations. However, because of the presence of Lewy bodies throughout the entire brain, characteristics of this disease not only include cognitive characteristics, but also physical, sleep, and behavioral changes. As the disease progresses, the motor symptoms common to Parkinson’s such as tremor, slowness, stiffness, and walking and balance problems will appear.
For more information on dementia with Lewy bodies, visit www.lbda.org.
Whats The Difference Between Corticobasal Degeneration And Parkinsons
The main difference between CBD and Parkinson’s is that it usually starts on one side with the gradual loss of use of one hand or leg , and there may be little flicks of involuntary muscle jerks. Walking and balance difficulties usually occur later in CBD than in Parkinson’s. Also, in CBD, a person may have trouble with purposeful movements, such as buttoning a shirt or cutting food.
For more information on corticobasal degeneration, read this information page.
Whats The Difference Between Multiple System Atrophy And Parkinsons
Parkinson’s and MSA both affect the movement control system and the involuntary autonomic control system and early symptoms can make a differential diagnosis a challenge. MSA, however, tends to progress faster than Parkinson’s; balance problems and a stooped posture happen earlier and get worse more quickly with MSA; and autonomic functions such as blood pressure, heart rate, breathing, sweating, bladder function, and sexual problems are more severe in people with MSA.
For more information on multiple symptom atrophy, read this fact sheet.
Q What Lifestyle Adjustments Can I Make To Help Improve My Symptoms
A. Although there are medications which are very effective for treating the symptoms of Parkinson’s disease, the effects of these medications usually diminish with time. For this reason, your doctor may recommend some lifestyle changes before starting you on medication.
Regular exercise can help you to maintain flexibility and mobility. It also improves posture, balance, strength, agility and even mood. A moderate level of exercise is best — try walking, swimming, tai chi or dancing. Always remember to ask your doctor about an appropriate fitness programme before you start.
Loss of appetite and subsequent weight loss can occur as a result of depression or a decreased sense of smell. Try to maintain a healthy and nutritious diet, with plenty of fibre to prevent constipation. Your doctor may need to prescribe an antidepressant medication if depression is severe or contributing to poor appetite and weight loss.
Whats The Difference Between Vascular Parkinsonism And Parkinsons
As the name implies, vascular parkinsonism is caused by cerebrovascular disease which affects the blood supply to the brain. Vascular parkinsonism is caused by one or more small strokes, while Parkinson’s is caused by a gradual loss of nerve cells. One major difference from Parkinson’s is that it’s not progressive, while Parkinson’s becomes worse with time. Another difference is that there are no tremors in vascular parkinsonism.
For more information on vascular parkinsonism, read this journal article.
Forced Exercise And Stress Reduction Reverse Parkinsons Symptoms
If you read last week’s post Doctors Call for an End to the Parkinson’s Pandemic, you learned that Parkinson’s disease is most often the result of a complex interplay between genetic and environmental factors, which include exposure to neurotoxic chemicals, head trauma, lack of exercise, diet, gut dysbiosis, and chronic stress.
While there is no cure for Parkinson’s disease, there are documented cases of improvement and recovery. Recovery in these cases is defined mainly by an elimination of motor symptoms. As I mentioned in last week’s post, motor symptoms begin when dopamine levels and neuron loss reach a critically low threshold—I’ll explain how that works in this post. When people are able to boost their dopamine levels and/or restore enough dopaminergic neurons that they can get past this threshold, their motor symptoms can go away.
In this post I’ll discuss why motor symptoms occur, research on neurogenesis in the substantia nigra of Parkinson’s patients, how exercise and stress reduction reduce motor symptoms, and stories of recovery from Parkinson’s disease. As you will learn, reducing and potentially eliminating motor symptoms—and even restoring sense of smell—is a realistic goal that Parkinson’s patients are already pursuing.
Natural Treatment For Parkinsons #1 Cannabis/medicalmarijuana:
Cannabis, aka medical marijuana, is an incredibletreatment for Parkinson’s disease. You can have a Parkinson’s patient shakingviolently and uncontrollably, and yet within 30-40 minutes of self-administering with some cannabis, their symptoms will almost completely disappear. Watch this short 2minute video from Parkinson’s sufferer, Ian Frizell, who shows you what he waslike before self-medicating with cannabis and then again after. The change is truly astonishing!
.
Taylor French is another Parkinson’s patient thatundergoes a remarkable transformation once he ingests what he calls “nutritional vegetable extract” . This guy has an advanced form ofParkinson’s and is normally confined to a wheelchair with limited use of hisbody due to stiff and rigid muscles . But after ingestingsome cannabis he’s able to walk, and incredibly, in his video he even getsinto his car and drives off down the road!
You can view it here…
Elyse Del Francia also tells the story of her Parkinson’ssuffering husband, and the time she decided to smother his morning pancakes withsome canabutter. She said…
“Within45 minutes of eating a pancake with marijuana on it, he stopped shaking. Thatwas my lightbulb moment. That’s when I knew that I was onto something thatwould relieve his pain and suffering, because it’s horrible, horrible, to haveParkinson’s Disease and not have any relief. I feel that this is something thathelps so many people in so many ways with pain and suffering.” 5
Q How Can I Stop Parkinsons Disease Affecting My Everyday Life

A. The problems with movement do affect everyday life, but with the help of health professionals you should be able to make adjustments to your daily routine and alterations around your home to help keep you active and independent.
- Speech can become monotonous, slurred or soft, and some people stutter if they have difficulty articulating words. A speech therapist can suggest verbalisation exercises and tongue movements to help you to speak louder and enunciate more clearly.
- As the disease progresses, you may find that eating becomes difficult due to problems with chewing and swallowing. A speech therapist may also be able to help with these problems.
- You may find walking difficult, especially taking the first step. A physiotherapist can give you exercises to strengthen your muscles and improve flexibility, as well as tips on how to improve posture, balance and mobility. Installing railings in the bathroom and hallways or using a walking aid can also help, and removing rugs from your home can prevent tripping.
- There is footwear available that can help improve gait and balance problems, and clothes with fastenings that should be easy to manage . An occupational therapist can help with suggestions and devices to make everyday tasks easier.
- Your handwriting can become small, shaky, and eventually illegible due to the combination of tremor, rigidity and bradykinesia. Using a large-body pen or pencil or a felt-tip pen may help.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
For Parkinsons Patients Exercise Does What Medication Cant
We learned last week that exercising regularly helps to prevent Parkinson’s. In a study of more than 7,300 male veterans, those with the lowest level of physical fitness had a 316% higher risk of developing Parkinson’s than those with the highest level of physical fitness. And a meta-analysis of more than half a million participants found a dose-response relationship: The more moderate to vigorous physical activity you do, the more your risk of getting Parkinson’s is reduced.
Reduced physical activity is likely an early symptom of Parkinson’s disease. But neuroscientists at the University of Texas in Austin did an interesting study to explore whether or not a reduction in physical activity also speeds up the degeneration of dopaminergic neurons. By restricting the movement of rats, they were able to show that the restriction of movement led to severe and chronic loss of dopaminergic neurons and impaired motor function. Neurons that aren’t used tend to wither away and die—this is called neural pruning. When it comes to movement, the principle of “use it or lose it” applies not only to our muscles, but to the health of our brain as well.
So we know that exercise is protective against Parkinson’s—great. If you already exercise, keep doing it, and if you don’t, start. But what about if you already have Parkinson’s?
Q Is Surgery Beneficial For People With Parkinsons Disease
A. Neurosurgery is increasingly used for people who have erratic and disabling responses to prolonged levodopa therapy. Options include deep brain stimulation , pallidotomy and thalamotomy. These procedures are generally only available in large, specialist centres.
Deep brain stimulation is where electrodes are inserted in the parts of the brain that control smooth motor control. These electrodes are connected to a device that is implanted under the skin near your collarbone.
The main difference between deep brain stimulation and traditional surgery is that you are able to activate and control the device, which sends tiny bursts of electricity to your brain to help control tremor and dyskinesias.
For people taking levodopa, it can help stabilise medication fluctuations and dyskinesia. Rigidity and bradykinesia can also improve with this treatment.
Unfortunately, this procedure is generally not helpful for people who have not responded to levodopa, except for those whose main symptom is tremor. Deep brain stimulation is not suitable for people with dementia, a psychotic illness or a major medical condition.
Pallidotomy, which involves destroying overactive cells in a region of the brain called the globus pallidus, is generally reserved for people with advanced disease that is not controlled by medicines. It can also treat the dyskinesias that result from long-term levodopa therapy, and allow continued use of levodopa.
Periodic Limb Movement Disorder And Restless Legs Syndrome
Do you often feel the irresistible urge to move your legs around during the night in order to get comfortable? If so, you might have restless legs syndrome . This condition can be associated with PLMD . PLMD causes slow rhythmic movements of the legs and feet, whereas restless legs syndrome causes more twitchy unpleasant sensations in the legs. Naturally, if you are frequently moving your legs, you are likely to wake up throughout the night, limiting your ability to get a good night’s sleep. Periodic limb movements are quite common in older adults as well as those with Parkinson’s. Restless legs syndrome frequently affects middle-aged and older adults in addition to people with PD.
Natural Remedies And Treatments For Parkinsons Finalnote
So there you have our top 10 natural remedies andtreatments for reversing Parkinson’s disease. We believe this is one of the most informative andthorough health articles on this disease you’ll find anywhere on the internet. Ifyou follow these 10 tips to-the-letter and continue to use them consistently,we guarantee that in 3-6 months’ time you will be truly astounded at themiraculous level of improvement you’ll see. In 12 months’ time you will scarcely recognize yourself! . But of course, you must stickwith them and follow through with each remedy every day if you want them towork. We sincerely hope you do.
Good luck and best wishes.
P.S. Because Parkinson’s is closely linked to Alzheimer’s disease and actually goes under the “dementia umbrella”, we recommend you take the time to read our “Powerful Natural Remedies for Dementia and Alzheimer’s” article for a more complete and comprehensive understanding on the causes and treatments for these diseases. You can click on the link below to go there…
Q What Is The Outlook For People With Parkinsons Disease
A. Most people can continue to work full time and lead relatively normal lives for many years after being diagnosed. The disease does not affect your life expectancy, and your age at diagnosis does not seem to have any effect on your long-term outlook. However, due to the progressive nature of the disease, many people do eventually become disabled.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease

Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Motor Symptoms Occur When The Nogo Pathway Is Activated
The motor symptoms of Parkinson’s disease typically appear years after the disease process has begun—often 20 or more years after. It’s estimated that motor symptoms appear when approximately 30% to 60% of dopaminergic neurons in the substantia nigra are lost. Studies show varied results when it comes to the actual percentage of substantia nigra neuron loss necessary to produce motor symptoms, and it’s safe to say that the exact percentage is different from person to person. Regardless of the percentage, it is understood that when dopamine levels decrease to a critical threshold, tremor or other motor symptoms may be felt—sometimes suddenly. For many people, this is the first noticeable sign of the disease.
Dopaminergic neurons in the substantia nigra send dopamine into two basal ganglia motor loops, referred to as the direct pathway of movement and the indirect pathway of movement. Dopamine regulates motor activity by acting on dopamine receptors, of which there are two types: D1-like receptors are present in the direct pathway, and D2-like receptors are present in the indirect pathway .
The direct pathway allows us to move in ways that we want to; activation of the direct pathway increases ease of movement and of initiating movement. In contrast, the indirect pathway allows us to suppress unwanted movement.
