When People Talk About Parkinsons They May Mention The Effects It Has On The Substantia Nigra But Did You Know That There Are Other Areas Of The Brain That Are Affected By The Condition

Parkinson’s is a condition that causes the gradual loss of the dopamine-producing brain cells of the substantia nigra — an area of the brain located just above where the spinal cord meets the midbrain. It is these cells that produce and release the neurotransmitter dopamine, which has a key role in turning thought about movement into action.
While this definition of the condition is useful to briefly explain Parkinson’s, the whole story is somewhat more complex. Over the last 30 years, it has become accepted that Parkinson’s also causes a number of non-motor symptoms, such as changes in sleep, smell and even the way we think, which likely involve other areas of the brain.
Now scientists are looking at the broader effects of the condition on the brain in an attempt to better understand why people experience different symptoms. The finding could lead us to new treatments that tackle more than just the motor symptoms of the condition.
Understanding How This Dementia Differs From Alzheimer’s Can Help Patients Know What To Expect And Feel Less Fearful
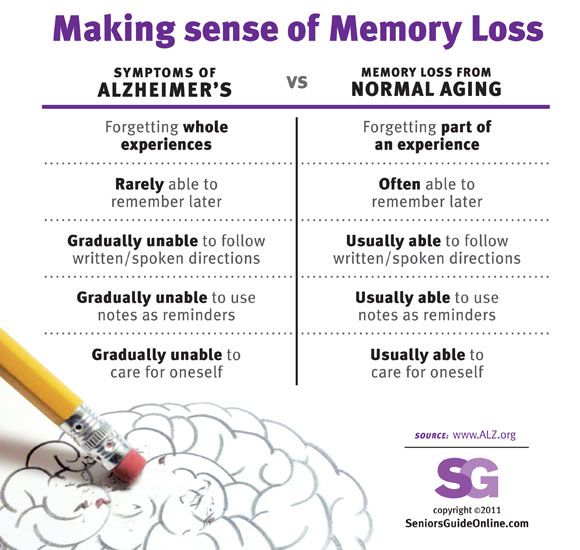
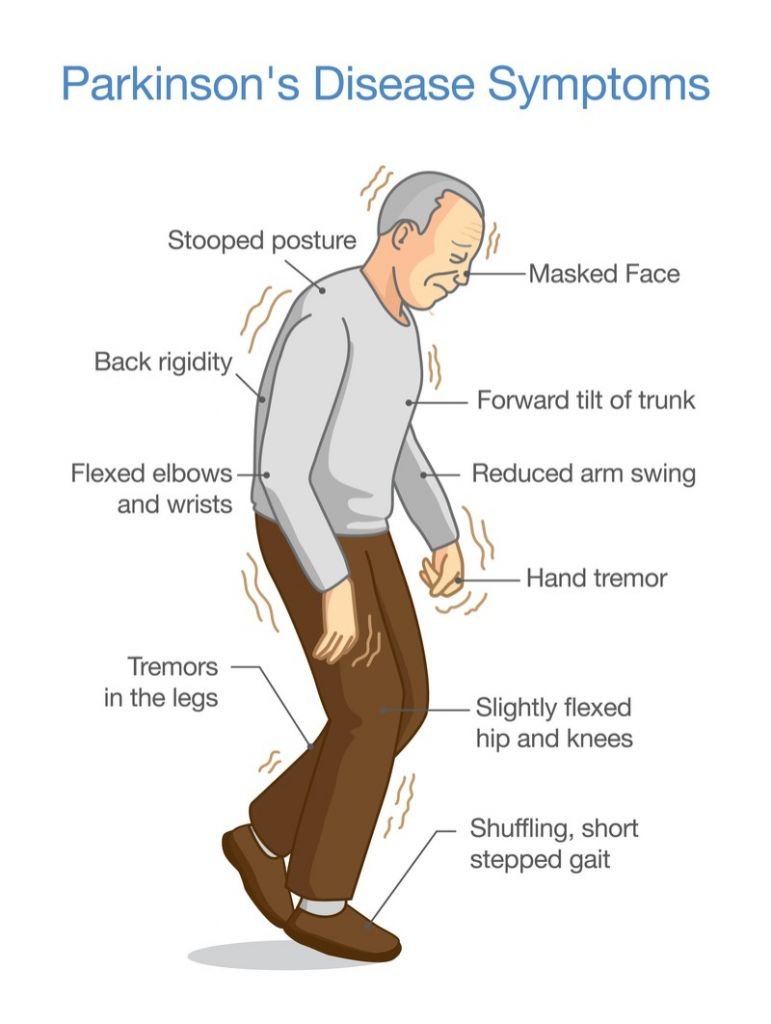
En español | Many symptoms of Parkinson’s disease — shuffling gait, quivering hands, stooped posture — are easy to spot. But this disease can also cause problems that are far less visible but no less distressing. Perhaps the most worrisome is cognitive decline, which affects about 50 percent of patients.
“This is a scary, confusing and concerning topic for a lot of people,” says neurologist Rachel Dolhun, M.D., senior vice president of medical communications at the Michael J. Fox Foundation. While these feelings are natural, common misconceptions can exacerbate patients’ fears.
For starters, cognitive decline doesn’t necessarily equal full-blown dementia, and many people with Parkinson’s develop only mild impairment. Another misconception is that even slight memory slippage signals that rapid deterioration is imminent — but that’s far more common with Alzheimer’s disease than it is with Parkinson’s, says Tsao-Wei Liang, M.D., chief of the movement disorders division at Jefferson Health. “It’s not always relentlessly progressive, and more often than not, symptoms can be managed with medication, caregiver support and basic organizational strategies,” he says.
It’s also important to know that many Parkinson’s patients with some cognitive impairments are able to form new short-term memories, even if they struggle with attention and multitasking. “People with Parkinson’s will often remember if you give a clue or prompt them,” Dolhun says.
Want To Learn More About The Latest Research In Parkinsons Disease Ask Your Questions In Our Research Forum
Cognitive impairment can occur due to stress, particularly if the patient feels they are a burden to their caregiver, are experiencing a decline in daily functioning, have a worsening quality of life, are dealing with rising medical costs, or are concerned about their mortality.
According to the National Parkinson Foundation, some of the common cognitive issues people living with Parkinson’s disease face include:
- Slowness of thinking
- Struggling to find the right words in conversations
- Declining visual perception
- Lack of reasoning skills
- Declining general intelligence
Some Parkinson’s disease medications can help with areas such as motivation and concentration, but there are no medications that can improve memory function.
MORE:How does Parkinson’s disease affect the brain?
Parkinsons’s News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
If Youre Experiencing Forgetfulness Or Confusion Check Your Medicine Cabinet
iStockphoto
For a long time doctors dismissed forgetfulness and mental confusion as a normal part of aging. But scientists now know that memory loss as you get older is by no means inevitable. Indeed, the brain can grow new brain cells and reshape their connections throughout life.Most people are familiar with at least some of the things that can impair memory, including alcohol and drug abuse, heavy cigarette smoking, head injuries, stroke, sleep deprivation, severe stress, vitamin B12 deficiency, and illnesses such as Alzheimer’s disease and depression.
But what many people don’t realize is that many commonly prescribed drugs also can interfere with memory. Here are 10 of the top types of offenders.
What Are Parkinson’s Disease Dementia Medical Treatment And Medications

There is no specific therapy for dementia in Parkinson’s disease. Although cognitive symptoms initially may appear to respond to drugs that promote dopamine production, the improvement is mild and transient in contrast to the early responses to motor control improvement with medication in patients with Parkinson’s disease.
Parkinson’s disease dementia medications
Various medications are used to treat the movement disorders of Parkinson’s disease, some may exacerbate symptoms related to dementia.
- These include dopamine given in the form of levodopa; medications known as dopamine agonists that act on the dopamine receptor; and medications that slow down the metabolism of dopamine. They are often used in conjunction with monoamine oxidase inhibitors such as rasagiline. In addition, anticholinergic drugs are sometimes used.
- Unfortunately, these drugs may affect cognitive symptoms and mood disorders.
- The anticholinergic drugs, for example, help balance levels of dopamine and acetylcholine, another neurotransmitter, in the brain. These drugs can improve movement disorders but often make memory loss worse.
The dementia of Parkinson’s disease may respond to drugs used in patients with Alzheimer’s disease. However, these drugs, called cholinesterase inhibitors , lead to only small and temporary improvements in cognition.
Mood disorders and psychoses are usually treated with other medication.
Box 2 Diagnostic Procedure Movement Disorder Society Pdd Criteria8144
Level I — Parkinson disease dementia
-
A diagnosis of Parkinson disease based on the UK Brain Bank criteria for PD
-
PD developed prior to the onset of dementia
-
Mini-Mental State Examination below 26
-
Cognitive deficits severe enough to impact daily living independent of motor symptoms
-
Impairment in more than one cognitive domain, that is, at least two of the following aspects:
-
Months Reversed or Seven Backward
-
Lexical Fluency or Clock Drawing
-
MMSE Pentagons
-
Absence of other abnormalities that obscure diagnosis
Level II — Comprehensive assessment for characterizing PDD
The level II evaluation assesses four domains:
-
Decreased global cognitive efficiency
-
Psychosis
Computerized cognitive testing
Digital computerized cognitive testing, which can be carried out remotely from patients’ homes, has become an interesting alternative to traditional pen-and-paper testing147. Benefits of computerized testing include the opportunity for frequent testing with less learning effects, which increases the sensitivity to detect decline148, cost-efficiency and the availability of large normative databases. Opportunities for conducting both remote functional assessments and digital interventions on the same online platform are being studied147,149.
Cognition Deficits In Parkinsons Disease: Mechanisms And Treatment
1Department of Pediatrics, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China
2Department of Neurology, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China
3Department of Neurosurgery, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China
Abstract
1. Introduction
As we know, the etiopathogenesis of PD characterized by irreversible disease progression is quite complicated and still lack of consensus to date, especially on the cognitive deficits of PD. A growing chorus of up-and-coming scholars ascribes the pathogenesis of PD to multineuropeptide dysfunction. Put another way, it is not only the progressive deterioration of dopaminergic neurons but defects in nondopaminergic systems that can lead to classical motor and nonmotor manifestations . Robust research component demonstrates that the early reduction of dopaminergic uptake in the frontal lobes is of crucial importance to cognitive impairment existing in PD patients . Accumulating lines of evidence suggest that the cholinergic disturbance within brainstem and corticostriatal pathways may be implicated in the pathophysiology of cognition deficits in PD . In addition, recent progress in PD has revealed that several genetic biomarkers and gene polymorphism may be connected with the generation and development of PD with cognition deficits.
2. Cognition Deficits in Parkinson’s Disease
2.1. PD-MCI
2.2. PDD
3. Mechanisms
3.1. Neurochemical Substrates
3.1.1. Dopamine and Its Receptors
Thinking And Memory Problems Associated With Parkinsons Disease
April 29, 2020 —People living with Parkinson’s Disease may be affected by thinking and memory problems. These cognitive issues can have a significant impact on a person’s quality of life and interfere with their daily function.
To some degree, cognitive impairment affects many people with PD. The same brain changes that lead to motor symptoms can also result in slowness in memory and thinking. Stress, medication and depression can also contribute to these changes. There are two levels of cognitive impairment.
Parkinsons Disease Linked To Sleep Disorders Sleep Disturbances

Parkinson’s disease has been linked to sleep disorders and sleep disturbances. Parkinson’s disease is characterized by the loss of brain cells that control movement. Symptoms of Parkinson’s disease can include tremors, stiffness, slowness of movements, as well as balance and coordination problems. Memory problems, depression, and sleep problems can all occur in Parkinson’s disease, too.
Sleep problems and sleep disorders may occur as an early sign of Parkinson’s disease, even before motor symptoms have started. Common sleep disorders experienced in Parkinson’s disease include insomnia, excessive daytime sleepiness, nightmares, sleep attacks, REM sleep behavior disorder , periodic leg movement disorder, restless leg syndrome, sleep apnea, and nocturia, which is frequent nighttime urination.
What Is Needed For A Parkinson’s Disease Dementia Diagnosis
There is no definitive medical test that confirms cognitive decline or dementia in Parkinson’s disease. The most accurate way to measure cognitive decline is through neuropsychological testing.
- The testing involves answering questions and performing tasks that have been carefully designed for this purpose. It is carried out by a specialist in this kind of testing.
- Neuropsychological testing addresses the individual’s appearance, mood, anxiety level, and experience of delusions or hallucinations.
- It assesses cognitive abilities such as memory, attention, orientation to time and place, use of language, and abilities to carry out various tasks and follow instructions.
- Reasoning, abstract thinking, and problem solving are tested.
- Neuropsychological testing gives a more accurate diagnosis of the problems and thus can help in treatment planning.
- The tests are repeated periodically to see how well treatment is working and check for new problems.
Imaging studies: Generally, brain scans such as CT scan and MRI are of little use in diagnosing dementia in people with Parkinson’s disease. Positron emission tomographic scan may help distinguish dementia from depression and similar conditions in Parkinson’s disease.
Dementia With Lewy Bodies And Parkinson Disease Dementia
, MD, PhD, Department of Neurology, University of Mississippi Medical Center
Dementia with Lewy bodiesParkinson disease dementia
Dementia is chronic, global, usually irreversible deterioration of cognition.
Dementia with Lewy bodies is the 3rd most common dementia. Age of onset is typically > 60.
Lewy bodies are spherical, eosinophilic, neuronal cytoplasmic inclusions composed of aggregates of alpha-synuclein, a synaptic protein. They occur in the cortex of some patients who have dementia with Lewy bodies. Neurotransmitter levels and neuronal pathways between the striatum and the neocortex are abnormal.
Lewy bodies also occur in the substantia nigra of patients with Parkinson disease, and dementia may develop late in the disease. About 40% of patients with Parkinson disease develop Parkinson disease dementia, usually after age 70 and about 10 to 15 years after Parkinson disease has been diagnosed.
Because Lewy bodies occur in dementia with Lewy bodies and in Parkinson disease dementia, some experts think that the two disorders may be part of a more generalized synucleinopathy affecting the central and peripheral nervous systems. Lewy bodies sometimes occur in patients with Alzheimer disease, and patients with dementia with Lewy bodies may have neuritic plaques and neurofibrillary tangles. Dementia with Lewy bodies, Parkinson disease, and Alzheimer disease overlap considerably. Further research is needed to clarify the relationships among them.
How To Talk To Someone With Hallucinations Or Delusions
- It is usually not helpful to argue with someone who is experiencing a hallucination or delusion. Avoid trying to reason. Keep calm and be reassuring.
- You can say you do not see what your loved one is seeing, but some people find it more calming to acknowledge what the person is seeing to reduce stress. For example, if the person sees a cat in the room, it may be best to say, “I will take the cat out” rather than argue that there is no cat.
Page reviewed by Dr. Chauncey Spears, Movement Disorders Fellow at the University of Florida, a Parkinson’s Foundation Center of Excellence.
What Are The Symptoms Of Parkinson’s Disease Dementia

Cognitive impairment in Parkinson’s disease may range from a single isolated symptom to severe dementia.
- The appearance of a single cognitive symptom does not mean that dementia will develop.
- Cognitive symptoms in Parkinson’s disease usually appear years after physical symptoms are noted.
- Cognitive symptoms early in the disease suggest dementia with Parkinsonian features, a somewhat different condition.
Cognitive symptoms in Parkinson’s disease include the following:
- Loss of decision-making ability
- Loss of short- and long-term memory
- Difficulty putting a sequence of events in correct order
- Problems using complex language and comprehending others’ complex language
Persons with Parkinson’s disease, with or without dementia, may often respond slowly to questions and requests. They may become dependent, fearful, indecisive, and passive. As the disease progresses, many people with Parkinson’s disease may become increasingly dependent on spouses or caregivers.
Major mental disorders are common in Parkinson’s disease. Two or more of these may appear together in the same person.
The combination of depression, dementia, and Parkinson’s disease usually means a faster cognitive decline and more severe disability. Hallucinations, delusions, agitation, and manic states can occur as adverse effects of drug treatment of Parkinson’s disease, this might complicate the diagnosis of Parkinson’s dementia.
ADHD Symptoms in Children?
Parkinson’s Disease Dementia Surgery And Gene Therapy
- Great strides have been made in the surgical treatment of Parkinson’s disease. Several different procedures are now available, and they are successful in many patients in relieving movement symptoms. Unfortunately, surgery has no effect on cognitive symptoms. In fact, most people with dementia are not candidates for surgery.
- Gene therapy is in its infancy; there are ongoing human and animal trials with various methods to insert genes into neuronal cells to reduce or stop Parkinson’s disease symptoms by causing cells to produce dopamine coded by the newly inserted genes. Early results with the treatment termed ProSavin are encouraging. However, it is not clear if such therapy could prevent or reverse Parkinson’s disease dementia.
Early Weight Loss With Parkinson’s May Be Red Flag
Researchers suspect this could indicate worse form of disease
HealthDay Reporter
MONDAY, Jan. 11, 2016 — People who lose weight in the early stages of Parkinson’s disease may have a more serious form of the movement disorder, according to a new study.
Parkinson’s is a chronic and progressive disease marked by tremors, impaired coordination, and slowness and/or stiffness. The cause and cure are unknown.
Weight loss is common in Parkinson’s patients, according to background information from the study. But the study findings, published online Jan. 11 in the journal JAMA Neurology, suggest that weight loss in the early stages of the disease could be a red flag for doctors.
“I suspect we may be looking at several subtypes of this disease,” study lead author Dr. Anne-Marie Wills, of Massachusetts General Hospital’s neurological clinical research institute, said in a hospital news release.
“The patients who experience early weight loss appear to have a more severe, systemic form of the disease, possibly due to involvement of the neuroendocrine system or the gastrointestinal nervous system, while those who gained weight may have a milder form of the disease,” she explained.
For the study, conducted between 2007 and 2013, the researchers examined data from more than 1,600 people who had been diagnosed with Parkinson’s within the previous five years.
It’s not known if maintaining or increasing weight could slow the progression of Parkinson’s.
Lewy Body Dementia Vs Parkinsons Disease Dementia
Diagnoses of Lewy body dementia include dementia with Lewy bodies and Parkinson’s disease dementia. Symptoms in both of these diagnoses can be similar.
Lewy body dementia is a progressive dementia caused by abnormal deposits of a protein called alpha-synuclein in the brain. Lewy bodies are also seen in Parkinson’s disease.
The overlap in symptoms between Lewy body dementia and Parkinson’s disease dementia include movement symptoms, rigid muscles, and problems with thinking and reasoning.
This seems to indicate that they could be linked to the same abnormalities, though more research is needed to confirm that.
The later stages of Parkinson’s disease have more severe symptoms that may require help moving around, around-the-clock care, or a wheelchair. Quality of life can decline rapidly.
Risks of infection, incontinence, pneumonia, falls, insomnia, and choking increase.
Hospice care, memory care, home health aides, social workers, and support counselors can be a help in later stages.
Parkinson’s disease itself isn’t fatal, but complications can be.
Research has shown a median survival rate of about
What Are The Complications Of Parkinson Disease

Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may arise later. As the disease gets worse with time, many people develop dementia. This can cause profound memory loss and makes it hard to maintain relationships.
Parkinson disease dementia can cause problems with:
- Speaking and communicating with others
- Problem solving
- Forgetfulness
- Paying attention
If you have Parkinson disease and dementia, in time, you likely won’t be able to live by yourself. Dementia affects your ability to care of yourself, even if you can still physically do daily tasks.
Experts don’t understand how or why dementia often occurs with Parkinson disease. It’s clear, though, that dementia and problems with cognitive function are linked to changes in the brain that cause problems with movement. As with Parkinson disease, dementia occurs when nerve cells degenerate, leading to chemical changes in the brain. Parkinson disease dementia may be treated with medicines also used to treat Alzheimer’s disease, another type of dementia.
Is There A Test For Parkinsons Disease Dementia
There is currently not one single test for Parkinson’s disease dementia. When a person is diagnosed with Parkinson’s disease, their doctor will closely monitor their health including any symptoms that may indicate a change in cognitive health. If deemed necessary, the doctor may order an MRI to determine the exact nature of any brain changes that are affecting thinking.
Mood And Memory Changes In Parkinson’s Disease
Most people with Parkinson’s disease notice some decline in their memory and mental agility, even very early in the course of the disease. Chances are that your PD will also affect your thinking to some extent. But the effects are subtle.
For example, you may notice that it takes you a bit longer to retrieve a memory, come to a decision, calculate a cost or plan a trip. This overall mental sluggishness is influenced by your mood and, in turn, your memory struggles can sometimes negatively influence your mood as well.
The good news is that new research has begun in the area of cognitive rehabilitation that can very effectively reverse this mental sluggishness.
Many With Parkinson’s May Have Memory Problems
Brain scans revealed changes in white and gray matter
HealthDay Reporter
FRIDAY, Sept. 4, 2015 — Many people with Parkinson’s disease have memory problems, researchers report.
The study included 40 people with early stage Parkinson’s disease and 40 healthy older adults. While the disease is generally viewed as a movement disorder, about half of the Parkinson’s patients had difficulty with some aspect of memory, such as learning and retaining information, or recalling spoken information, the investigators found.
“And then half of those participants, or nearly one-quarter of all participants with Parkinson’s, were really having a difficult time consistently with their memory, enough that it would be noticeable to other people,” said study author Jared Tanner. Tanner is an assistant research professor in the department of clinical and health psychology at the University of Florida at Gainesville.
Still, there was good news: Most of the Parkinson’s patients did not have significant memory problems, according to the authors of the study published online recently in the journal PLoS One.
Because of the study’s design, the researchers could only show an association between Parkinson’s disease and memory problems; they couldn’t prove a cause-and-effect relationship.
“People with Parkinson’s disease who had stronger connections between these areas of the brain did better at remembering information,” he said.
How Can We Support The Sleep/wake Cycle Of Pdd

For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a “lights out” routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
Behaviors Seen In Parkinsons Disease Dementia
As dementia progresses, managing disorientation, confusion, agitation, and impulsivity can be a key component of care.
Some patients experience hallucinations or delusions as a complication of Parkinson’s disease. These may be frightening and debilitating. Approximately 50 percent of those with the disease may experience them.
The best thing to do when giving care to someone experiencing hallucinations or delusions from Parkinson’s disease dementia is to keep them calm and reduce their stress.
Take note of their symptoms and what they were doing before they exhibited signs of hallucinating and then let their doctor know.
This element of the disease can be particularly challenging for caregivers. Patients may become unable to care for themselves or be left alone.
Some ways to make caregiving easier include:
- sticking to a normal routine whenever possible
- being extra comforting after any medical procedures
- limiting distractions
- using curtains, nightlights, and clocks to help stick to a regular sleep schedule
- remembering that the behaviors are a factor of the disease and not the person
How Is Parkinsons Disease Dementia Diagnosed
No single test can diagnose Parkinson’s disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinson’s and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinson’s dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
Managing Cognitive Impairments In Parkinsons
After a thorough evaluation to rule out other causes of cognitive impairment, patients with PD may be treated with medication, occupational therapy, and/or speech therapy. The medications used to treat cognitive impairments in people with PD are based on treatments used for Alzheimer’s disease. Occupational therapy can help a person with PD by providing adaptive strategies for daily activities. Speech therapy can help with language functions, as well as information processing. 3,4
The Profile Of Memory And Cognitive Changes

Even in the very early stages of Parkinson’s disease people can have difficulty with their thinking processes. Most authorities agree that the primary difficulty lies with the so-called executive cognitive functions.
Executive cognitive functions refer to such thinking processes as memory retrieval, planning, generation of words or concepts, attention, and monitoring and adjustment of non-routine and goal-directed behaviors. The common denominator in all of these executive functions is that they require cognitive control in order to operate smoothly.
The term cognitive refers to processes or operations involved in the processing of all kinds of information. So cognitive control processes are those processes that are used by the mind and brain to regulate the storage, retrieval, and usage of information .
Problems with executive functions are typically mild in early PD. They usually involve a generalized slowing of cognitive processing speed and subtle deficits in attention and working memory. It may be difficult, for example, to hold two different pieces of information in the mind at the same time, or to efficiently generate words and concepts as quickly as one used to. As the disease progresses, these executive cognitive deficits are made more severe by common Parkinson-related mood disorders and Parkinson-related emotional problems such as depression and anxiety.
Parkinsons Disease Treatment And Its Future
Parkinson’s disease has no cure. However, millions of dollars are going into research every year to help better understand the disease, from how it’s defined to how it’s treated. The ultimate end goal is developing a cure for Parkinson’s, but in the meantime, doctors and researchers have developed treatment plans based on what they presume is causing the disease in the first place—most often the lack of certain brain chemicals and cells like dopamine.
The plans vary per patient, and some of these treatment options include:
There isn’t any real way to definitively prevent the disease, either. As with prevention for any disease or malady, it’s suggested that you maintain a healthy lifestyle before and after a diagnosis. Remaining physically engaged through activities like running, yoga, and weight lifting and eating healthy are both ways to provide your body with the best opportunity for a healthy life.
Clinical trials are also viewed as a “treatment option” because they may give you as good of a chance of relieving symptoms as other already-existent treatments. There are clinical trials happening year-round with various institution and foundations, and your demographic may fit a trial in its beginning pre-clinical stage or an advanced stage.
Talk to your doctor about any available clinical trials that you may qualify for and how to become a part of them. Also stay in contact with your doctor regarding any concerns that you may have with Parkinson’s or how to get it treated.
How Common Is Parkinson’s Disease Psychosis
Between 20-40% of people with Parkinson’s report the experience of hallucinations or delusions. When followed as the disease progresses over the years, this number increases. The increase does not mean that the hallucinations are persistent across the majority of patients. However, it is important to note that these statistics sometimes include “delirium,” in which the symptoms are temporary due to medication that needs to be adjusted or infection that needs to be treated, and “isolated minor symptoms” or “minor hallucinations,” including illusions, where instead of seeing things that are not there , people misinterpret things that are really there. These are the most common types of psychosis in people with PD, with different studies placing the occurrence between 25-70% of people with Parkinson’s. Typically, if the person with PD only has these minor hallucinations, their doctor will not prescribe an antipsychotic medication, though more significant psychosis that requires medication may develop over time. In one study, 10% of those with minor hallucinations had their symptoms resolved within a few years, while 52% saw their symptoms remain the same and 38% saw their psychosis symptoms get worse.
We recommend that people with Parkinson’s not use a single percentage to represent the prevalence of hallucinations and PDP. Parkinson’s is a complex disease and as it progresses the percentages and risk of symptoms will change.
What Are The Symptoms Of Parkinson Disease
Parkinson disease symptoms usually start out mild, and then progressively get much worse. The first signs are often so subtle that many people don’t seek medical attention at first. These are common symptoms of Parkinson disease:
- Tremors that affect the face and jaw, legs, arms, and hands
- Slow, stiff walking
How Is Parkinsons Disease Dementia Treated
Treatment for Parkinson’s disease dementia currently focuses on management of symptoms. Your doctor will determine which medications may be most beneficial to you. At this time, some options include:
- Cholinesterase inhibitors are often used in the treatment of Alzheimer’s and can also be of help to people with Parkinson’s dementia.
- L-dopa is sometimes used to inhibit the movement symptoms associated with Parkinson’s. However, it can aggravate hallucinations and other symptoms in some dementia patients. Therefore, close monitoring by a doctor while using this medication is vitally important.
- Antidepressants are commonly used to treat depression in people who have Parkinson’s disease dementia.
- Clonazepam can be used to treat REM sleep disorder.
- Antipsychotic drugs are sometimes used to address behavioral issues. They must be used with extreme caution due to the risk of serious side effects.
People who have Parkinson’s disease dementia can also benefit from high quality memory care. At Parc Provence, our proven programs combine engaging therapies with an environment designed to bring out the best in our memory care residents. Calming therapies and a secure, home-like atmosphere create a comfortable setting where residents and their families can find peace of mind. Our robust activity schedule encourages mental engagement so members of the Parc Provence community live fulfilling lives. Our goal is to bring out the best in every resident at every stage.
Classification Issues And Prodromal Stages
The proposal that dementia prior to or simultaneous with motor symptoms can be included in the diagnostic criteria for PD13,256 has reopened the long-standing debate on whether PDD and DLB should be considered the same disease257,258,259,260. A deeper understanding of the pathophysiological processes underlying these two synucleinopathies, such as the relative contribution of ?-amyloid and tau pathology in cortex and striatum, the extent of cortical Lewy pathology and ?-synuclein load in the hippocampus, the severity of neuronal loss in the substantia nigra, and cholinergic cell loss260, is required to better understand the relationship between PD and DLB.
Although some risk factors for cognitive impairment have been identified46,48,261, further research is needed to better identify any early evidence of cognitive impairment in genetic at-risk populations and in individuals with clinical features of prodromal PD to provide opportunities for prevention strategies and early precision therapy interventions.
