Genetic Study Of Lewy Body Dementia Supports Ties To Alzheimers And Parkinsons Diseases
NIH-led study locates five genes that may play a critical role in Lewy body dementia.
In a study led by National Institutes of Health researchers, scientists found that five genes may play a critical role in determining whether a person will suffer from Lewy body dementia, a devastating disorder that riddles the brain with clumps of abnormal protein deposits called Lewy bodies. Lewy bodies are also a hallmark of Parkinsons disease. The results, published in Nature Genetics, not only supported the diseases ties to Parkinsons disease but also suggested that people who have Lewy body dementia may share similar genetic profiles to those who have Alzheimers disease.
Lewy body dementia is a devastating brain disorder for which we have no effective treatments. Patients often appear to suffer the worst of both Alzheimers and Parkinsons diseases. Our results support the idea that this may be because Lewy body dementia is caused by a spectrum of problems that can be seen in both disorders, said Sonja Scholz, M.D., Ph.D., investigator at the NIHs National Institute of Neurological Disorders and Stroke and the senior author of the study. We hope that these results will act as a blueprint for understanding the disease and developing new treatments.
The study was led by Dr. Scholzs team and researchers in the lab of Bryan J. Traynor, M.D., Ph.D., senior investigator at the NIHs National Institute on Aging .
Article:
NIHTurning Discovery Into Health®
Lewy Bodies And Parkinsons Disease
A person with Parkinsons disease may develop dementia and have problems with reasoning and thinking. Lewy bodies are a feature of several brain disorders, including Parkinsons disease and Alzheimers disease, and they may cause rigid muscles and problems with movement and posture.
Research suggests that the similarity of the symptoms of Parkinsons disease and Lewy body dementia may be indicative of a shared link to how the brain processes alpha-synuclein.
It is not possible to test for the presence of Lewy bodies, so researchers must try to determine their effects by carrying out postmortem studies.
There is currently no cure for dementia. However, medication can alleviate the symptoms, while a team of medical professionals and therapists may help a person develop strategies to manage their daily activities.
The 6 Stages Of Parkinson’s And Lewy Body Disease
In 2003, Heiko Braak identified a pattern of Lewy body deposition, in the synucleinopathies , which include Parkinson’s Disease , Multiple Systems Atrophy , Progressive Supra-nuclear Palsy and Dementia .
The pattern that he identified has been termed the Braak Staging of Lewy Body inclusions. More current research shows that Lewy Body pathology can spread from one area of the nervous system to another, and it’s conceivable that this happens in a prion-like fashion. There are also some studies that show alpha-synuclein is not only just an intracellular protein but is extracellular as well, which could explain to some degree, the progression to other areas of the brain.
The first three stages of Braak’s staging, are largely “asymptomatic”to the uninformed individual.
In stage 1, inclusion bodies begin accumulating in the olfactory bulb and a part of our brainstem called the Vagus Nucleus. Symptoms at this point may include a change in the ability to smell and taste, as well as a constellation of symptoms we call autonomic symptoms, which are often casually related to “aging”. The symptoms may, or may not include: constipation, sexual dysfunction, dry eyes, dry skin, light-headedness, high blood pressure, insulin resistance, swelling of the hands and feet, bladder dysfunction, an increase in heart rate or arrhythmia, dizziness when getting out of a chair or bed, etc.
Stay tuned to the #TalkNeuro Blog!
Further Reading and Reference:
Read Also: Parkinson’s Disease And Genetics
Diagnosing Dementia With Lewy Bodies
Dementia with Lewy bodies is characterized by dementia symptoms that start beforemotor symptoms appear. Research suggests this is because Lewy body proteins first begin to accumulate in the brains cortex, causing cognitive symptoms to appear before motor ones. This is a defining feature in the diagnosis of DLB, according to the American Psychiatric Associations Diagnostic and Statistical Manual of Mental Disorders,
In addition, at least one of these core clinical features must be present for a diagnosis of DLB to be made:
- Fluctuating cognitive states, including inattention and alertness
- Recurrent visual hallucinations that are very detailed and vivid
- Features of parkinsonism , with onset that occurs after cognitive decline begins
Other diagnostic features of DLB include rapid eye movement sleep behavior disorder and severe neuroleptic sensitivity. The presence of motor symptoms is the key to distinguish DLB from Alzheimers disease, as motor or movement symptoms are not present in Alzheimers disease.
Behavioral And Mood Symptoms Of Lewy Body Dementia
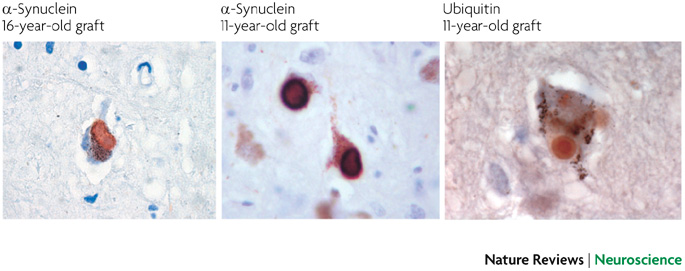
Changes in behavior and mood are possible in LBD and may worsen as the persons thinking abilities decline. These changes may include:
- Depression
- Apathy, or a lack of interest in normal daily activities or events and less social interaction
- Anxiety and related behaviors, such as asking the same questions over and over or being angry or fearful when a loved one is not present
- Agitation, or restlessness, and related behaviors, such as pacing, hand wringing, an inability to get settled, constant repeating of words or phrases, or irritability
- Delusions, or strongly held false beliefs or opinions not based on evidence. For example, a person may think his or her spouse is having an affair or that relatives long dead are still living.
- Paranoia, or an extreme, irrational distrust of others, such as suspicion that people are taking or hiding things
Recommended Reading: Parkinson’s Color Ribbon
Wait So What Is Parkinsonism
Parkinsonism refers to the motor symptoms that are typically associated with PD, such as tremors, stiffness, and walking/balance problems. Both PD and LBD are forms of Parkinsonism, meaning that PD patients and LBD patients may experience these motor symptoms.2 Because the Parkinsonism motor symptoms of PD and LBD can be very similar, it can be difficult to differentiate between the two conditions.
What Is Lewy Body Dementia Causes Symptoms And Treatments
On this page:
Lewy body dementia is a disease associated with abnormal deposits of a protein called alpha-synuclein in the brain. These deposits, called Lewy bodies, affect chemicals in the brain whose changes, in turn, can lead to problems with thinking, movement, behavior, and mood. Lewy body dementia is one of the most common causes of dementia.
LBD affects more than 1 million individuals in the United States. People typically show symptoms at age 50 or older, although sometimes younger people have LBD. LBD appears to affect slightly more men than women.
Diagnosing LBD can be challenging. Early LBD symptoms are often confused with similar symptoms found in other brain diseases or in psychiatric disorders. Lewy body dementia can occur alone or along with other brain disorders.
It is a progressive disease, meaning symptoms start slowly and worsen over time. The disease lasts an average of five to eight years from the time of diagnosis to death, but can range from two to 20 years for some people. How quickly symptoms develop and change varies greatly from person to person, depending on overall health, age, and severity of symptoms.
In the early stages of LBD, symptoms can be mild, and people can function fairly normally. As the disease advances, people with LBD require more help due to a decline in thinking and movement abilities. In the later stages of the disease, they often depend entirely on others for assistance and care.
Recommended Reading: What Are Early Warning Signs Of Parkinson’s Disease
Test Results Supporting Diagnosis
Physical and neurological examinations and various tests may help distinguish LBD from other illnesses. Specific tests that may support an LBD diagnosis include:
- A positron emission tomography scan or a single-photon emission computerized tomography scan showing reduced dopamine transporter uptake in the basal ganglia
- Abnormal 123iodine-MIBG myocardial scintigraphy showing reduced communication of cardiac nerves
- Sleep study confirming REM sleep behavior disorder without loss of muscle tone
Read more about diagnosing dementia, including tests and who can make a diagnosis.
There are no tests that can definitively diagnose LBD. Currently, only a brain autopsy after death can confirm a suspected diagnosis. However, researchers are studying ways to diagnose LBD earlier and more accurately during life. The use of certain imaging, blood, cerebrospinal fluid, and genetics tests is being studied.
How Is Lewy Body Dementia Diagnosed
There isn’t one test that can diagnose LBD. It is important to see an experienced doctor to get a diagnosis. This would usually be specialist such as a neurologist. The doctor will
- Do a medical history, including taking a detailed account of the symptoms. The doctor will talk to both the patient and caregivers.
- Do physical and neurological exams
- Do tests to rule out other conditions that could cause similar symptoms. These could include blood tests and brain imaging tests.
- Do neuropsychological tests to evaluate memory and other cognitive functions
LBD can be hard to diagnose, because Parkinson’s disease and Alzheimer’s disease cause similar symptoms. Scientists think that Lewy body disease might be related to these diseases, or that they sometimes happen together.
It’s also important to know which type of LBD a person has, so the doctor can treat that type’s particular symptoms. It also helps the doctor understand how the disease will affect the person over time. The doctor makes a diagnosis based on when certain symptoms start:
- If cognitive symptoms start within a year of movement problems, the diagnosis is dementia with Lewy bodies
- If cognitive problems start more than a year after the movement problems, the diagnosis is Parkinson’s disease dementia
You May Like: Can Essential Tremor Turn Into Parkinson’s
Robin Was Very Aware That He Was Losing His Mind And There Was Nothing He Could Do About It
Schneider added: Robin was very aware that he was losing his mind and there was nothing he could do about it.
Jacqueline Cannon said of her fathers condition: He always used to say to me, Im losing my mind. We say to people that LBD is not just about memory. Its about the other symptoms that go with it, especially the hallucinations.
In the spotlight
Like Parkinsons disease there is currently no cure for LBD, and a need to raise awareness the case of Robin Williams will no doubt help. Dedicated research centres do already exist, such as the leading Biomedical Research Unit in Lewy Body Dementia at Newcastle University.
Professor Ian McKeith, president of the Lewy Body Society, believes there is cause for hope however. In a piece published by The Conversation, he wrote: Therapeutic trials have been few and far between in LBD because of a combination of a lack of compounds to test, a pre-occupation with targeting Alzheimers and a reluctance of regulatory bodies to recognise LBD. All of these are now changing and LBD is increasingly viewed as a malleable and commercially-viable target.
Memory And Thinking Problems
You may experience forgetfulness, slowed thinking and difficulty concentrating. You might find it harder to follow conversations, and remember some words and names. This can make communication difficult.
You may also find it increasingly difficult to make decisions, plan activities and solve problems. This can make everyday activities harder.
You May Like: Beginning Symptoms Of Parkinson’s
Building A Lewy Body Dementia Care Team
After receiving a diagnosis, a person with LBD may benefit from seeing a neurologist who specializes in dementia and/or movement disorders. Your primary doctor can work with other professionals to follow your treatment plan. Depending on an individual’s particular symptoms, physical, speech, and occupational therapists, as well as mental health and palliative care specialists, can be helpful.
Support groups are another valuable resource for people with LBD and their caregivers. Sharing experiences and tips with others in the same situation can help people find practical solutions to day-to-day challenges and get emotional and social support.
What Is Lewy Body Dementia
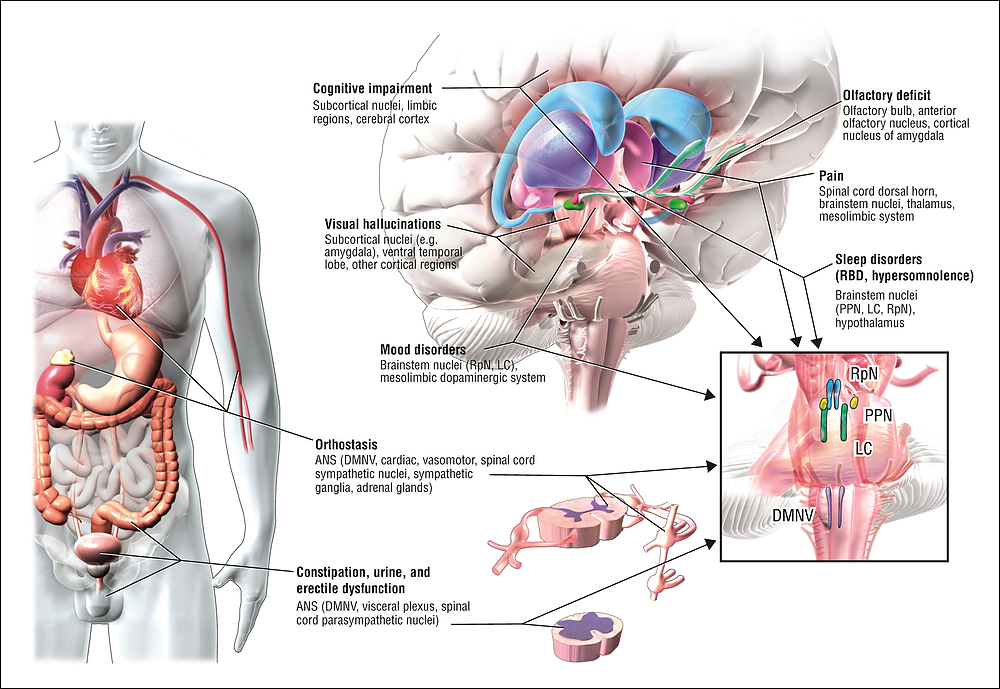
Lewy body dementia is not a single disorder but rather a spectrum of closely-related disorders involving disturbances of cognition, behavior, sleep, movement and autonomic function.
In these progressive disorders, Lewy bodies build up in the brain. Lewy bodies in the brain stem cause a disruption in the production of chemical messengers called dopamine. Too little dopamine can cause parkinsonism, a clinical syndrome thats characterized by tremor, bradykinesia , rigidity and postural instability. Parkinsonism can be caused by Parkinsons disease itself as well as by other underlying neurological conditions such as LBD. These Lewy bodies are also found throughout other areas of the brain, including the cerebral cortex. The neurotransmitter acetylcholine is also depleted, causing disruption of perception, thinking and behavior.
A German neurologist, Friederich H. Lewy, first discovered the abnormal protein deposits in the early 1900s as he was conducting research on Parkinsons disease.
Recommended Reading: Parkinson’s Ribbon Color
What Can I Expect If I Or My Loved One Have A Diagnosis Of Lewy Body Dementia
Each persons experience with Lewy body dementia is unique to them. How slowly or quickly the disease progresses is impossible to know, but may be influenced by your general health and any existing diseases you may have. Because LBD is a progressive disease, difficulties with mind and body functions get worse over time. Currently, there is no known way to stop the progression of the disease. After diagnosis, most people with LBD live between five and seven years. Some people with LBD live up to 20 years after their diagnosis.
However, theres always hope. Research on LBD, dementia with lewy bodies, Alzheimers disease, Parkinsons disease with dementia are ongoing. New medications are being developed and new approaches to treatment are being investigated.
Progression Of Lewy Body Pathology
Lewy body pathology begins in the medulla and olfactory bulbs, spreading progressively through six Braak stages to involve the pons, midbrain, limbic lobe, amygdala and neocortex . Cortical Lewy bodies are similar to those encountered in the brain stem, but do not have a halo and are present even in cases without dementia. Pathological inclusions are also found in the autonomic nervous system, including the enteric nervous system in the gastrointestinal tract.
Spread of Lewy body pathology may reflect selective vulnerability of certain brain regions or could be due to stepwise spread along anatomical pathways. Since the olfactory bulb is affected first, the possibility of a pathogenic virus infection gaining access to the brain via the nasal mucosa has been postulated.
Mariah Lelos, in, 2020
Read Also: What Is Life Expectancy Of Parkinson’s Patients
What Causes Dementia With Lewy Bodies
Lewy bodies are named after the German doctor who first identified them. They are tiny deposits of a protein that appear in nerve cells in the brain. Researchers don’t have a full understanding of why Lewy bodies appear, or exactly how they contribute to dementia. However, this is linked to two factors:
- low levels of important chemicals that carry messages between nerve cells
- a loss of connections between nerve cells, which then die.
Lewy bodies are the cause of DLB and Parkinson’s disease. They are two of several diseases caused by Lewy bodies that affect the brain and nervous system and get worse over time. These are sometimes called Lewy body disorders.
The way someone is affected by DLB will depend partly on where the Lewy bodies are in the brain:
- Lewy bodies at the base of the brain are closely linked to problems with movement . These are the main feature of Parkinson’s disease.
- Lewy bodies in the outer layers of the brain are linked to problems with mental abilities , which is a feature of DLB.
People with a Lewy body disorder can have problems with movement and changes in mental abilities at the same time.
A person with Parkinson’s disease is at high risk of going on to develop dementia as their condition progresses. Dementia may be more likely in a person who has developed Parkinson’s later in life or who has been living with it for several years.
Differences Between Pdd And Dlb
So, how are PDD and DLB different from each other? That depends on whom you ask. Some clinicians feel that these two conditions are simply different versions of the same disorder. In fact, some professionals use the terms interchangeably. Yet, according to currently agreed-upon diagnostic guidelines, there are some differences.
Also Check: How Long Do People With Parkinson’s Live
Can Imaging Tests Diagnose Lewy Body Dementia
Imaging tests, such as computed tomography or magnetic resonance imaging , are done to rule out other causes of dementia such as brain tumors, brain bleeds, stroke, hydrocephalus or other structural causes. Imaging studies for Lewy body dementia are usually normal. The only way to make an absolute diagnosis of LBD is by examining the brain at autopsy.
Apda In Your Community
APDAParkinson’s Disease SymptomsLewy Bodies, Dementia, and Parkinsons What Does it all Mean?
Here are two common scenarios that may sound familiar:
Scenario 1A patient develops a series of neurologic symptoms, is evaluated by a neurologist and is told that she has Parkinsons disease . She then visits another neurologist for a second opinion and is told she has Lewy Body Dementia .
Scenario 2A patient has his first visit with his neurologist and is told that he has PD, at a subsequent visit the diagnosis is changed to Parkinsons disease dementia , and at a follow up visit the diagnosis is changed yet again to Dementia with Lewy Bodies .
Both of these situations understandably cause great uncertainty and frustration.
You May Like: Parkinson’s Today
Mild Cognitive Impairment And Dementia In Parkinson Disease
Contrary to Dr James Parkinsons introduction to An Essay on the Shaking Palsy, the intellect is not uninjured in PD. Although patients with PD first come to medical attention because of characteristic motor signs, including rest tremor, rigidity, bradykinesia, and gait abnormality, specific cognitive impairments in executive function, visual-spatial skill, and even memory function in patients with PD are common and have been known for more than 40 years. PD hastens deterioration of these cognitive abilities over time, with the incidence and prevalence of cognitive impairments increasing with duration and severity of illness. In this sense, PD can be considered a risk factor for dementia. Formal criteria have been developed for mild cognitive impairment in PD . These criteria attempt to account for the contribution of motor impairment to functional decline and are now being validated.
