What Are The Early Warning Signs Of Parkinsons Disease
Parkinsons warning signs can be motor symptoms like slow movements, tremors or stiffness. However, they can also be non-motor symptoms. Many of the possible non-motor symptoms can appear years or even decades ahead of motor symptoms. However, non-motor symptoms can also be vague, making it difficult to connect them to Parkinsons disease.
Non-motor symptoms that might be early warning signs include:
General Psychosis And Pd Psychosis
With regard to the clinical definition of the main features of psychosis, which include hallucinations, illusions, and delusions, current ICD-10 guidelines define hallucinations as a disorder characterised by a false sensory perception in the absence of an external stimulus, whereas an illusion is regarded as a misperception of an externally present stimulus. In contrast to classical hallucinations and illusions, delusions are a false interpretation of the experienced misperceptions, often involving topics of persecution, imposters, or grandiosity. Some specific forms of delusions such as the Cotard syndrome , Capgras syndrome , and Othello syndrome have further been named , the latter showing an association with dopamine agonist therapy and an improvement after its reduction. The current diagnostic criteria from ICD-10 based guidelines for acute and transient psychosis are shown in Box 1 other definitions of psychosis falling under the term of schizoaffective disorders will not be further developed in this review.
The ICD-10 classification of mental and behavioural disorders: definition criteria for acute and transient psychosis. F23, F30, F32: diagnosis codes of psychotic and mood disorders taken from ICD-10 guidelines reference: taken from WHO International classifications, ICD-10 guidelines .
Proposed criteria for psychosis in Parkinsons disease. PD, Parkinsons disease UK, United Kingdom references: Ravina et al., 2007, and Fenelon et al., 2008 .
Index To Diseases And Injuries References
The Index to Diseases and Injuries is an alphabetical listing of medical terms, with each term mapped to one or more ICD-10 code. The following references for this diagnosis code are found in the injuries and diseases index:
- – Parkinsonism – See Also: Dementia, in, diseases specified elsewhere – G20
- – with behavioral disturbance – See Also: Dementia, in, diseases specified elsewhere – G20
| 332.0 – Paralysis agitans |
| Approximate Flag – The approximate mapping means there is not an exact match between the ICD-10 and ICD-9 codes and the mapped code is not a precise representation of the original code. |
Also Check: Tremor-dominant Parkinson’s Progression
Dementia With Lewy Bodies
Dementia with Lewy bodies is named for the presence of abnormal protein deposits of alpha-synuclein that are also seen in people with PD. DLB is the second most common type of dementia after Alzheimers disease, and it is a progressive disorder. In people with DLB, the Lewy bodies are found throughout the brain. DLB is characterized by cognitive impairments, visual hallucinations, inability to focus, inflexible thinking and paranoia. DLB patients initially have these cognitive symptoms but also develop motor symptoms similar to PD such as bradykinesia, tremor, rigidity, and shuffling walk. Similar to PD, DLB patients also have REM sleep behavior disorder in which they act out their dreams. DLB is treated with cholinesterase inhibitors and atypical antipychotics. However, there is no cure for DLB.
Diseases Of The Nervous Systemtype 2 Excludes
- Dementia associated with parkinson’s disease
- Dementia in parkinsons disease
- Restrictive lung disease due to parkinsons disease
- Restrictive lung mechanics due to parkinsons disease
- 056 Degenerative nervous system disorders with mcc
- 057 Degenerative nervous system disorders without mcc
Don’t Miss: Lewy Body Vs Parkinson Dementia
Is Lewy Body Dementia Hereditary & What Is The Life Expectancy Of A Person With Lewy Body Dementia
Most patients suffering from Lewy Body Dementia prefer visiting a primary care physician at the initial stage. Diagnosing the disorder can be a real problem if the symptoms grow severe.
There are many families that have been affected by Lewy Body Dementia . However, it has been seen that very few individuals and even medical professionals are aware of the diagnostic criteria and symptoms. Some even dont have the idea whether or not the disease exists. Therefore, you should know about Lewy Body Dementia not only to save yourself but also your loved ones, families and friends. Lewy body dementia is a type of progressive dementia that comes only after Alzheimers disease dementia.
What Causes The Condition
Although there are several recognized risk factors for Parkinsons disease, such as exposure to pesticides, for now, the only confirmed causes of Parkinsons disease are genetic. When Parkinsons disease isnt genetic, experts classify it as idiopathic . That means they dont know exactly why it happens.
Many conditions look like Parkinsons disease but are instead parkinsonism from a specific cause like some psychiatric medications.
Familial Parkinsons disease
Parkinsons disease can have a familial cause, which means you can inherit it from one or both of your parents. However, this only makes up about 10% of all cases.
Experts have linked at least seven different genes to Parkinsons disease. Theyve linked three of those to early-onset of the condition . Some genetic mutations also cause unique, distinguishing features.
Idiopathic Parkinsons disease
Experts believe idiopathic Parkinsons disease happens because of problems with how your body uses a protein called -synuclein . Proteins are chemical molecules that have a very specific shape. When some proteins dont have the correct shape a problem known as protein misfolding your body cant use them and cant break them down.
With nowhere to go, the proteins build up in various places or in certain cells . The buildup of these Lewy bodies causes toxic effects and cell damage.
Induced Parkinsonism
The possible causes are:
Read Also: Does Parkinson’s Affect Your Sleep
Myth : Parkinsons Disease Is Fatal
Fact: Although a diagnosis of Parkinsons is devastating, it is not as some people may still believe a death sentence. Parkinsons disease is not a direct killer, like stroke or heart attack. That said, much depends on the quality of your care, both from your medical team and yourself.
As the disease progresses, you may become more vulnerable to falls, which can be dangerous. Thats why exercise and physical therapy are so important.
Infection is another problem. In later stages of Parkinsons, people often miss those signals and may not notice somethings up until its too late. That can be, literally, a killer so be sure to stay up to date with checkups.
Also Check: Can You Drink Alcohol With Parkinsons Disease
Chart Review And Data Collection
A retrospective chart review was conducted documenting age at diagnosis and visit, sex, UPDRS-III score at each visit, the year of diagnosis, and two time variables documenting post diagnosis time. One variable was time in years from diagnosis to first UPDRS-III assessment in our clinic, and the other was interval between follow up visits and their first UPDRS-III assessment. Levodopa equivalent daily dose was analyzed at initial visit and at time of death for all patients.
Patients were classified into three age groups according to their age at PD diagnosis, < 50, 5064, and 65 years. The endpoints of the study were the trajectories of motor deterioration using UPDRS-III score prior to death, stratified by age group and sex.
Also Check: How Does Parkinson’s Disease Affect The Spinal Cord
Abnormality Of Tau Protein
PSP has been considered to be a tau protein disorder. Cortical fibrillary tangles of PSP are similar to those observed in Alzheimer disease with regard to the presence of an abnormally phosphorylated tau protein. Tau is a component of a microtubule-associated protein that is responsible for axonal transport of vesicles. The mechanism whereby this is involved in PSP has yet to be determined. PSP overlaps with corticobasal degeneration in this regard, and the latter may have a stronger association with tau protein abnormalities than does PSP.
Tau proteins exist in 6 isoforms encoded by a single gene. Different electrophoretic patterns have been identified in the various disorders associated with tau abnormalities. Thirty-two mutations have been identified in more than 100 families. About half of the known mutations have their primary effect at the protein level. They reduce the ability of tau protein to interact with microtubules and increase its propensity to assemble into abnormal filaments. The other mutations have their primary effect at the RNA level and perturb the normal ratio of 3-repeat to 4-repeat tau isoforms. When studied, this change resulted in a relative overproduction of tau protein with 4 microtubule-binding domains in the brain.
Read Also: Average Life Expectancy After Parkinsons Diagnosis
Circumstances And Societal Engagement In Yopd And Implications For Management
In general, people with YOPD tend to have different family and societal engagements to those with late-onset PD. For example, most people diagnosed with YOPD will have a job, whereas some people with late-onset PD have already retired. Additionaly, it is not unusual that people with YOPD have young children , or may want to start a family.
You May Like: Rock Steady For Parkinson’s Disease
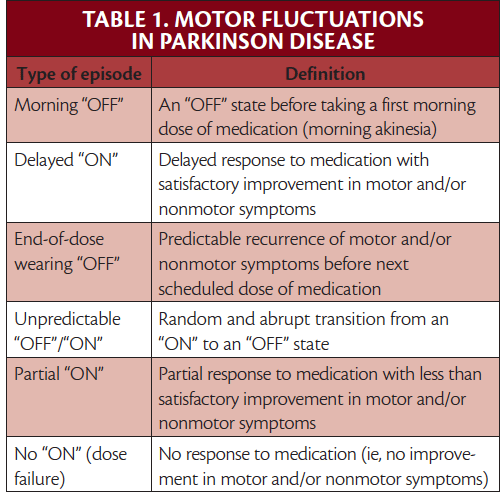
Recommendations For Pd Icd
Based on this review, the panel recommends the ICD-10-CM coding structure for PD be expanded to provide specificity to distinguish motor complications of dyskinesia and/or OFF episodes . The proposed changes include delineating between individuals without dyskinesia or fluctuations , without dyskinesia but with fluctuations , with dyskinesia but without fluctuations , and with dyskinesia and fluctuations .
Figure 1. Proposed International Classification of Diseases, Tenth Revision, Clinical Modification codes for Parkinson disease.
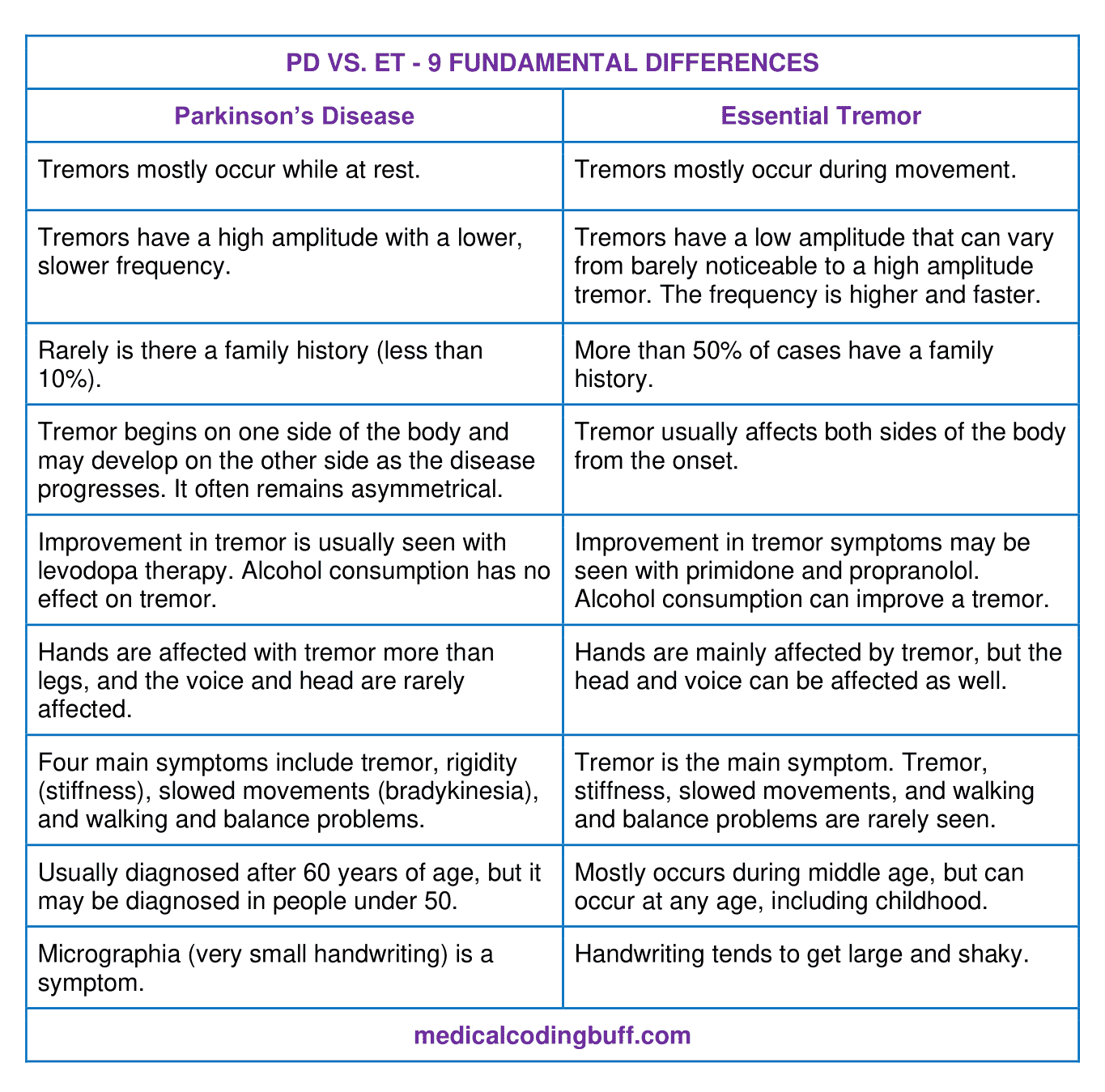
Parkinsons Disease Vs Parkinsonism: Understanding The Difference Is Essential For Icd
March 25, 2019 / By Pamela Ewing, CPC
What is Parkinsons disease? It is a neurodegenerative disorder that affects predominately dopamine-producing neurons in a specific area of the brain called the substantia nigra.
The substantia nigra cells produce dopamine, a chemical messenger responsible for transmitting signals within the brain that allow for coordination of movement. Loss of dopamine causes neurons to fire without normal control, leaving patients less able to direct or control their movement. Parkinsons disease is one of several diseases categorized by clinicians as movement disorders.
Parkinsons disease has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Stiffness of the limbs and trunk
- Slowness of movement
- Impaired balance and coordination
Parkinsonism refers to symptoms of Parkinsons disease , regardless of the cause, and is typically caused by another condition or external agent, such as drugs. These two conditions are not classified the same.
With the Parkinsons Disease progression listed are just a few of many symptoms. Some symptoms may include, but are not limited to:
specified NEC E21.4Parkinsons G20
We then look in the Alpha index for Parkinsons and it refers us to Parkinsonism.
Parkinsonism G20with neurogenic orthostatic hypotension G90.3arteriosclerotic G21.4dementia G31.83 with behavioral disturbance G31.83
G20 would be used to indicate Parkinsons Disease, and it would be sequenced first, followed by the manifestation.
Recommended Reading: Why Do You Die From Parkinson’s Disease
You Have Parkinsons Disease
With Parkinsons, there is too little of the messenger substance dopamine in certain parts of the brain. The messenger dopamine is important in controlling the bodys movements, for example. A lack of the messenger dopamine makes movements more difficult. The person can then no longer execute certain movements as quickly as normal. As a result, keeping ones balance may also become difficult. The muscles may also stiffen up. The hands often shake.
You have symptoms from the Parkinsons. The symptoms from your Parkinsons do not vary during the day.
Dementia In Other Diseases Classified Elsewhere Mild With Psychotic Disturbance
- 2023 – New CodeBillable/Specific CodeManifestation Code
- Dementia in other diseases classified elsewhere, mild, with psychotic disturbance such as hallucinations, paranoia, suspiciousness, or delusional state
- Major neurocognitive disorder in other diseases classified elsewhere, mild, with psychotic disturbance such as hallucinations, paranoia, suspiciousness, or delusional state
Also Check: Does Parkinson’s Run In Families
Average Life Expectancy For Seniors With Parkinsons
On average, a person with Parkinsons disease dies at the age of 81, which is equal to national life expectancy rates. Depending on age and location, overall life expectancy is somewhere between the ages of 78 and 81. However, overall life expectancy rates are skewed a little by the fact that more young people engage in risky behavior that can cause earlier death. Those who manage to survive to the age of 65 actually have a longer life expectancy84 to 86 yearswhich means seniors with Parkinsons have a slightly shorter life span than other seniors, but they still have a fairly normal life span when compared to the general population.
Also Check: Botox Injections For Parkinsons Disease
Info For Medical Coders On How To Properly Use This Icd
- Inclusion Terms:
Inclusion Terms
Inclusion Terms are a list of concepts for which a specific code is used. The list of Inclusion Terms is useful for determining the correct code in some cases, but the list is not necessarily exhaustive.
- Hemiparkinsonism
- Parkinsonism or Parkinsons disease NOS
- Primary Parkinsonism or Parkinsons disease
- Code Type-1 Excludes:
Type-1 Excludes
Type-1 Excludes mean the conditions excluded are mutually exclusive and should never be coded together. Excludes 1 means do not code here.
Recommended Reading: Treatment Of Parkinson’s Psychosis
Life Expectancy With And Without Parkinsons Disease In The General Population
L. Dommershuijsen, A.. Ikram, K. Ikram
Session Time: 1:15pm-2:45pm
Location: Les Muses, Level 3
Objective: To determine the burden of Parkinsons disease in the general population and the life expectancy after the diagnosis of PD.
Background: Detailed estimates of the prevalence and incidence of PD have been reported in the literature. However, data on life years lived with and without PD are still limited. Life expectancy estimates are important both for healthcare policy making and for care planning of individual patients.
Method: We conducted this study as part of the Rotterdam Study, an ongoing, population-based cohort study in the Netherlands. We included 12,400 participants of 50 years and older, free of PD. We constructed multistate life tables with three states, and transitions were possible from no PD to PD, no PD to death and PD to death. For each transition we calculated age- and sex-specific rates with Poisson regression using the Gompertz distribution to estimate the remaining life expectancy per year of age. From these rates we calculated the proportion of the remaining life expectancy lived with PD among the general population, and the remaining life expectancy among those with incident PD.
Among the general population, the proportion of the life expectancy lived with PD is small. Nevertheless, among PD patients, a large negative impact of the disease can be found on the remaining life expectancy.
To cite this abstract in AMA style:
Mov Disord.
Identifying Risk Factors For Parkinsons
The risk for early death increased by about 40% for every 10-year increase in age at diagnosis.
Parkinsonâs researcher Tobias Kurth, MD, agrees that identifying risk factors for early death could help clinicians better manage the disease.
Kurth is an adjunct associate professor of epidemiology at Harvard School of Public Health.
âThis is important research that adds to our understanding of the impact of specific features of Parkinsonâs disease on outcomes,â he tells WebMD.
His own study of Parkinsonâs-associated death matched Parkinsonâs patients with people without the disease who had similar non-Parkinsonâs-related illnesses.
Like the newly reported study, patients who were older when their Parkinsonâs disease was diagnosed had a greater risk for early death.
Read Also: Is Constipation A Symptom Of Parkinson’s Disease
Dementia In Other Diseases Classified Elsewhere Unspecified Severity With Psychotic Disturbance
- 2023 – New CodeBillable/Specific CodeManifestation Code
Support For Revision Of Icd
The American Academy of Neurology supports the need to update the ICD-10-CM coding to better reflect the progression of PD. Patient advocacy groups also support this need, including the Michael J. Fox Foundation for Parkinsons Research and the Unified Parkinsons Advocacy Council , which is a group of national, regional, and state organizations including the Parkinsons Foundation, the American Parkinson Disease Association, and the Davis Phinney Foundation for Parkinsons among others.
Read Also: Parkinson’s Brain Mri Vs Normal
Dementia In Other Diseases Classified Elsewhere With Behavioral Disturbance
- 2016201720182019202020212022Billable/Specific CodeManifestation Code
Common Parkinsons Plus Syndromes
There are several different Parkinsons plus syndromes, but some have not yet been defined or named. However, the most common syndromes and their unique characteristics include:
Multiple system atrophy . Also known as Shy-Drager syndrome , MSA is a term made up of several neurodegenerative disorders which causes one or more body systems to stop working. This is the second most common form of atypical parkinsonism.
Typical symptoms include:
- vision problems
- changes in personality
Individuals with PSP often have a worried facial expression. Tremors are rare in PSP.
Diagnosis is made based on the clinical features, but there is no particular test that will definitively diagnose it. The focus of treatment is on the symptoms. Patients do not do well with PD medications, such as levodopa.
Corticobasal syndrome . Also known as corticobasal degeneration and cortical basal ganglionic degeneration , according to theBaylor College of Medicine. This is the rarest type of atypical parkinsonism that is characterized by cell loss and deterioration of particular areas of the brain.
Symptoms include:
- stiffness in one side or the other
- jerky and involuntary movements in the hand or leg
- abnormal posture and twisting
There is no specific test for CBS and no treatment available to slow the progression of CBS. Symptoms can be treated with physical, occupational, and speech therapy.
Don’t Miss: Sleep Disorders And Parkinson’s
