Link Between Migraine And Parkinsons Found
Patients who suffer from 2 or more migraines per year may be at an increased risk of developing Parkinsons disease later in life, according to the findings of a new study from Taiwan.1
The study looked at a sizeable cohort of 41,019 subjects , who had had at least two migraines during 2001. The researchers then studied 41,019 randomly selected subjects without migraine. Patients were matched to the migraine cohort based on age, sex, pre-existing comorbidities, and socioeconomic status.
The researchers, from the National Taiwan University Hospital, noted that none of the subjects in the study had been diagnosed with PD or secondary Parkinsonism in the year prior to the study. However, at the 32-month follow-up, 148 patients with migraine were diagnosed with PD, compared to just 101 patients without migraine of 1.64 P=0.0004). The PD-free survival rate for the migraine group also was found to be significantly lower than that for the non-migraine group .1
What Are The Risk Factors For Cluster Headache
Several factors tend to increase the risk of developing cluster headache. Risk factors for cluster headache include:
-
Age 20 to 50 years
-
Family history of cluster headache
-
Male biological sex
Alcohol use, especially red wine, can trigger headaches during an episode period. However, once the episode subsides and remission begins, alcohol usually is not a problem.
Functional Exercise For Chronic/persistent Pain
There are some simple exercises that you can try around the house to help:
- If you experience pain in your legs, keep them strong by practising standing up and sitting down in a chair.
- If your shoulders are aching, start by loosening them with some shoulder rolling actions, then by lifting an object that is slightly weighty from a shelf, and then replacing it. This increases the range of movement in your back, shoulders and arms, and then your strength.
You May Like: What Is The Progression Of Parkinson’s
Limitations To The Study
The data, supplied by the Taiwanese National Health Insurance claims database, excluded relevant lifestyle factors, like past occurrence of head injury, smoking, alcohol intake, and obesity, a limitation that may have influenced the findings, according to the study authors.
The median follow-up time of 32 months may seem comparatively short compared to other longitudinal investigations, like Scher et als analysis of the AGES-Reykjavik cohort that occurred after several decades.3 Having a follow-up of < 3 years may have prevented the researchers from better understanding the long-term effects of migraines on PD risk, the authors wrote.
And while the authors noted there could be some bias to consider, given both conditions are neurological, the study benefits from its large sample size and offers useful evidence supporting a positive association between migraine and PD for researchers to consider further.
Experts now suggest that future studies, perhaps using targeted brain imaging and neurologic examinations , someday could elucidate even more insights behind the cerebral vulnerability migraine possibly shares with PD, a development that could lead to a better understanding and treatment of the 2 conditions.
Dont Miss: On Off Phenomenon In Parkinsons Disease
Improve Your General Fitness
Increasing your level of fitness will help you manage your weight and ensure your joints arent under any added pressure. You could try walking, swimming, dancing, cycling or aerobics its up to you.
Many of Parkinsons UKs local groups have physiotherapist-led exercise classes you can join. Visit our Local Support page or call our helpline on 0808 800 0303 to find one near you.
Don’t Miss: Is Parkinson’s Considered A Neurological Disease
Medical Hypothesis: Deep Brain Stimulation For Intractable Migraine
Parisa Gazerani 1,*
Department of Health Science and Technology, Faculty of Medicine, Aalborg University, Denmark
Faculty of Pharmaceutical Sciences, The University of British Columbia, Vancouver, Canada
* Correspondence: Parisa Gazerani
Received: October 26, 2020 | Accepted: December 29, 2020 | January 05, 2021
OBM Neurobiology 2021, Volume 5, Issue 1, doi:10.21926/obm.neurobiol.2101082
Recommended citation: Gazerani P, Cairns BE. Medical Hypothesis: Deep Brain Stimulation for Intractable Migraine. OBM Neurobiology2021 5:20 doi:10.21926/obm.neurobiol.2101082.
© 2021 by the authors. This is an open access article distributed under the conditions of the Creative Commons by Attribution License, which permits unrestricted use, distribution, and reproduction in any medium or format, provided the original work is correctly cited.
What Are The Symptoms Of Parkinsons Disease
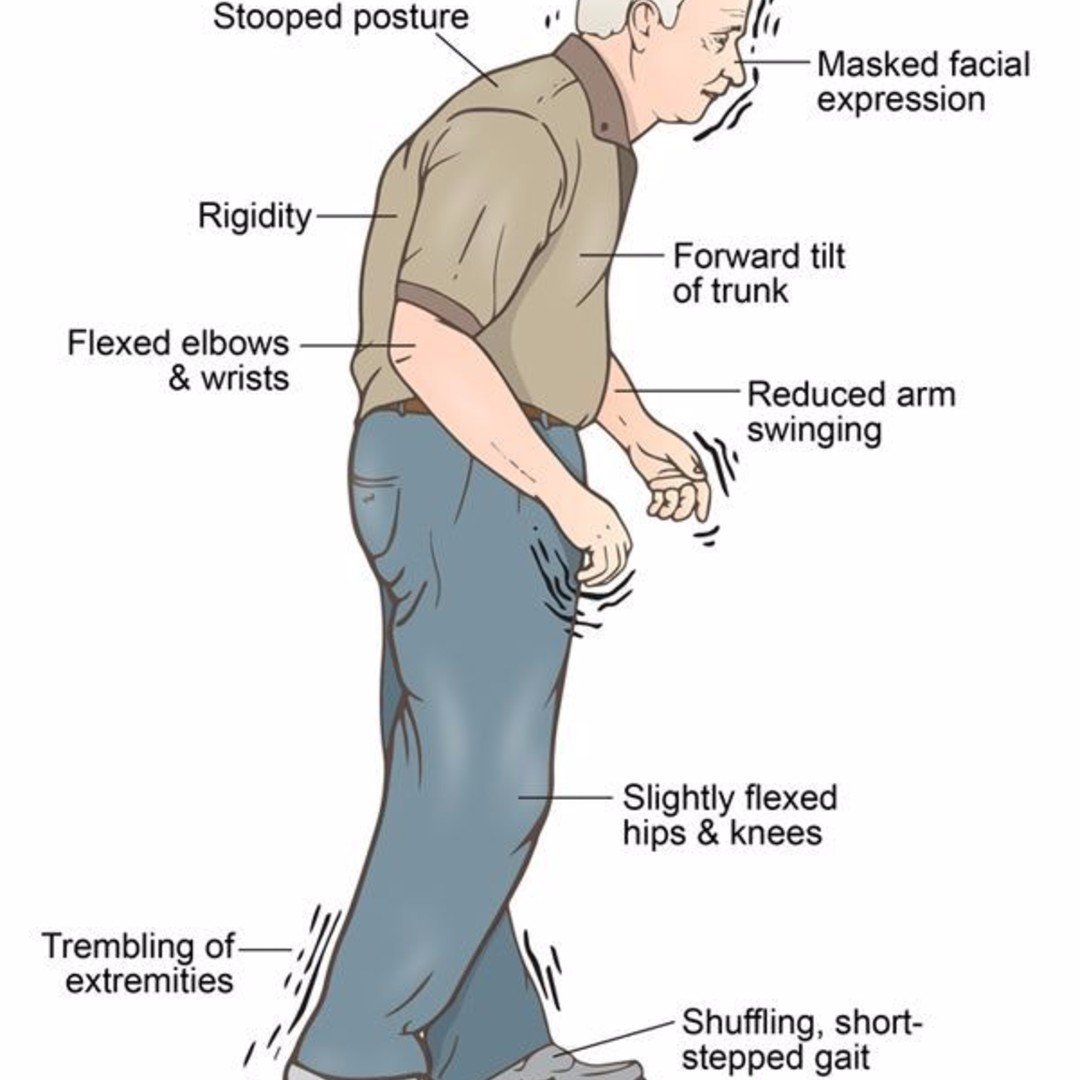
The primary symptoms of the condition include:
- Stiffness in your arms, legs, and neck
- Tremors in your hands
- Trouble making fine finger movements
- Poor balance and coordination
You might also experience less common signs of the disease, such as:
- Difficulty with urination or bowel movements
- Low blood pressure when you stand up
- Problems chewing or swallowing
You might also have difficulty walking, and may feel like your feet stick to the ground when you try to walk.
Also Check: Dopamine Patches For Parkinson’s
Psychiatric And Neurobehavioral Disorders
These disorders are related to the connection between the brain and behavior. Neurobehavioral disorders are impairments associated with brain diseases like multiple sclerosis, stroke, and dementia or brain injury. Psychiatric disorders are associated with abnormal functions of the part of the brain responsible for social cognition. Historically, the study and treatment of these disorders were separate, but today doctors embrace a connection between the two in order to better treat and diagnose a wide range of conditions affecting the brain.
How Are Cluster Headaches Treated During A Cycle
When a headache starts, you can take medicine or breathe in oxygen from a machine to ease the pain or stop the headache. You use these treatments only when you feel a headache coming on. You dont use them every day.
When a cluster headache begins:
If your treatment doesnt work, ask your doctor if you can try something else. It may take time to find what works best for you.
Over-the-counter pain medicines, such as aspirin, acetaminophen, and ibuprofen, usually dont work for cluster headaches.
Dealing with repeated cluster headaches can lead to stress and depression, which in turn can continue the headache cycle. Finding ways to cope with stress and improve depression may reduce the severity or frequency of your cluster headaches.
Don’t Miss: Best Diet For Parkinson’s Patients
What Are The Recommended Pharmacological Treatments For Parkinsons Disease
There is not a cure for Parkinsons Disease. Instead, the goal of treatment is to ease symptoms. Each person with PD may have different symptoms, therefore the treatment plan will often vary person to person.
Overall, many of the medications used for Parkinsons either target dopamine or acetylcholine, two neurotransmitters believed to be involved in the physiology of the disease.
Some common medications options include:
- Carbidopa/levodopa
Advanced treatment options such as an intestinal infusion or deep brain stimulation may be recommended for those with PD patients who do not have symptom relief using oral medications or have an advanced form of the disease.
https://www.duopa.com/how-duopa-works
Other treatment options include focused ultrasound, thalamotomy and pallidotomy procedures.
Know Your Specific Triggers
For instance, one of my biggest triggers is cervical tension especially when driving, traveling, or writing on the computer for hours. Another specific trigger for me and many others with migraines is skipping a meal which sometimes due to severe nausea or gastroparesis from PD. PD meds can make eating a difficult thing.
Also Check: New Treatment For Parkinson’s
What Is The Difference Between Migraine And Cluster Headache
One of the main differences between migraine and cluster headache is that the person with cluster headache, unlike the person with migraine, becomes agitated during an attack and is unable to sit or lie down or find relief in sleeping. Where a migraine can last up to 72 hours, a cluster headache lasts less than 3 hours with the intensity of the pain peaking within a few minutes and reducing quickly at the end of the attack.
You May Like: Can Essential Tremor Become Parkinsons
Riboflavin Ameliorates Mitochondrial Dysfunction
Case reports of mitochondrial diseases have emphasized the beneficial effects of riboflavin administration. In two patients with complex I deficiency associated myopathy, complex I activity has been normalized upon riboflavin therapy with an evident clinical improvement . In comparison with controls, complex I activity has been increased from 16 to 47% upon high dose riboflavin therapy . Genetic testing has shown that ACAD9 is involved in complex I function, deficiency state, and responsiveness to riboflavin . Continuous clinical response to riboflavin therapy for a 3-year period has been reported in a female patient with skeletal myopathy attributed to complex I deficiency . In addition to complex I deficiency patients, riboflavin administration has been used in complex II deficiency patients, resulting in moderate clinical improvement, stable clinical picture, and prevented disease progression, as well as a twofold elevation in complex II activity in vitro . In complex IV deficiency, which presumably is destabilized by complex I deficiency, riboflavin has been shown to improve its activity . Riboflavin administration elevates the intra-mitochondrial FAD levels, compensating for the reduced capacity of mutant complexes to assemble . In electron-transport flavoprotein dehydrogenase gene mutations, riboflavin therapy can lead to clinical improvements .
You May Like: Why Do Parkinson’s Patients Shuffle
Pain In Parkinsons Disease
Doctors categorize pain as nociceptive, which refers to pain from tissue damage, or as neuropathic, which refers to pain that arises from the nerves. Some pain is both nociceptive and neuropathic. Most people with PD experience nociceptive pain.
This type of pain is generally localized to a specific area of the body. The most common areas for people with PD to experience pain are the neck, upper back, and the extremities . Neuropathic pain is less common in PD, although it may be caused by akathisia, an extreme restlessness.1
The pain caused by PD can generally be classified by one of five causes:
Riboflavin As A Determinant Of The Kynurenine Pathway
Kynurenine pathway is the main tryptophan catabolism pathway, with neuroactive metabolites known as kynurenines. This pathway is determined by vitamin B2 status, indicated by plasma riboflavin, and B6 status, indicated by circulating PLP since both vitamins are essential cofactors. FAD is required for the formation of 3-hydroxykynurenine. PLP is required for the formation of anthranilic acid, 3-hydroxyanthranilic acid, kynurenic acid, and xanthurenic acid. Plasma riboflavin, as well as riboflavin intake, is positively associated with 3-hydroxyanthranilic acid and xanthurenic acid . PLP is positively associated with kynurenic acid, 3-hydroxyanthranilic acid and xanthurenic acid, all formed by PLP-based enzymes, and negatively associated with 3-hydroxykynurenine, metabolized by PLP-based enzymes however, vitamin B6 intake showed null associations with kynurenines . Xanthurenic acid is determined by both riboflavin and PLP interactively .
Glutamate receptors, including NMDA and metabotropic receptors, are influenced by the kynurenines. In fact, kynurenic acid is an antagonist of NMDA and all ionotropic glutamate receptors . Xanthurenic acid is an activator of type-2 metabotropic glutamate receptors . Picolinic acid is neuroprotective, considered the brain main metal chelator . However, quinolinic acid is an agonist of NMDA . 3-hydroxykynurenine, 3-hydroxyanthranilic acid, and 5-hydroxyanthranilic acid are neurotoxic with ROS generation properties .
Recommended Reading: What Are The Early Symptoms Of Parkinson’s
Why Are They Called Cluster Headaches
Cluster headaches get their name from how they affect you. They come on in clusters, or groups, before temporarily going away for most people.
Each headache tends to last 30 to 45 minutes, though some are shorter and some longer. You may experience up to eight of these headaches within 24 hours. And this may happen for weeks or several months.
Then the clusters usually pause, for reasons that arent yet understood. The headaches go into remission for months or years before returning. Some people never get much of a break, though. They experience chronic cluster headaches. This happens to about one in five people who get cluster headaches.
You May Like: What Is The Difference Between Parkinsons And Alzheimers
Characteristics Of Cluster Headaches
Each day, patients can suffer multiple headache attacks, the duration of which can be anywhere from 15 minutes to three hours. Most of the time, patients experience pain on one side only and may suffer from drooping, tearing eyes and a runny nose at the same time. The pain has been compared to that of childbirth.
Don’t Miss: What Age Is Parkinson’s Diagnosed
The Relationship Between Migraine And Parkinsons Disease
One study assessing the migraine prevalence in 237 Parkinsons disease subjects found that 27.8% of patients had migraine within their lifetime and 13.1% of patients currently had migraine.4 Interestingly, after the onset of Parkinsons disease, almost two thirds of PD patients had improvement in their migraine attacks or complete remission.4 It is unknown how or why some migraine patients improve or enter a remission phase after the onset of Parkinsons disease.
Another notable study found that subjects with a history of migraine with aura had double the risk of Parkinsons disease compared to controls.5 They also found women in this group were more likely to have a parent or sibling with PD compared to controls.5 It is unclear why those who have migraine with aura are at a higher risk of PD, however, research is being done to understand how genetics play a role in PD.
How Are Cluster Headaches Treated
Unfortunately, there is no cure for cluster headaches. But you do have treatment options that can make them a little less painful. Treatment options include:
- Abortive treatment to stop attacks: Often, a headache will stop before you have a chance to see a healthcare provider. But if you get there in time, there are several effective ways to stop a cluster headache. A healthcare provider may give you injected medications or a nasal spray. These include sumatriptan, dihydroergotamine and zolmitriptan. The provider may also give you oxygen through a mask.
- Medications to improve quality of life: Prescription medications can shorten a headache cycle. They can also make the headaches less severe. Calcium channel blockers, verapamil, lithium carbonate, divalproex sodium, melatonin or topiramate may help. There is a new preventive therapy that is a calcitonin gene-related peptide monoclonal antibody.
- Other options when needed: Surgeons have tried operations for cluster headaches. But they havent had much success preventing them. Researchers are now testing newer therapies to see if they can work. One option uses mild electrical stimulation on the neck. Another creates electrical stimulation by placing a medical device through the upper gums.
Read Also: What Causes Shaking In Parkinsons Disease
Also Check: Antipsychotics In Parkinson’s Disease
Commonalities Between Migraine And Parkinsons Disease
- Migraine and Parkinsons disease are comorbid with many of the same diseases such as depression, sleep disorders, anxiety and cardiovascular disease.
- Traumatic brain injury can increase the risk of developing Parkinsons disease later in life and can also trigger the onset of migraine but it is unclear how a TBI can cause either of these conditions.
- The use of deep brain stimulation can be used for both conditions. While it is a commonly used treatment for PD, it is not routinely used for migraine.
- Lower dopamine levels have been seen in both migraine and PD patients. In PD, this is treated with medications that target the dopamine receptor. In migraine, lower dopamine levels have been linked to sensitivity to pain and stimulation 6
- Iron accumulation has been found in both Parkinsons disease and migraine patients.5 In those with PD, iron accumulation was identified in the substantia nigra and in migraine it was identified in the deep brain nuclei.5
- Non-invasive vagus nerve stimulation is FDA approved for the acute and preventive treatment of migraine and is currently being studied for Parkinsons disease.7,8
The Prevalence Course And Clinical Correlates Of Migraine In Parkinsons Disease: A Multicentre Case
- Dawn C. Buse and more…Encyclopedia of Lifestyle Medicine & Health2012
- Encyclopedia of Stem Cell Research2008
- Steven M. Baskin and more…Handbook of Mind-Body Medicine for Primary Care2003
- Kenneth L. Lichstein and more…Treatment of Late-Life Insomnia
- The SAGE Encyclopedia of Abnormal and Clinical Psychology2017
- The SAGE Encyclopedia of Abnormal and Clinical Psychology2017
- The SAGE Encyclopedia of Abnormal and Clinical Psychology2017
- The SAGE Encyclopedia of Abnormal and Clinical Psychology2017
Also Check: Can An Mri Detect Parkinson’s
A Lawyer For Malpractice Cases
Besides ignorance, several factors can go into a diagnostic error for example, lack of communication between medical specialists and a lack of follow-through. You may have good grounds for a medical malpractice case if your doctors negligence caused the error. If your case succeeds, you may be reimbursed for the expense of all those unnecessary treatments and lost wages and pain and suffering.
A lawyer may be of great help since filing a claim is far from easy. You may especially want an attorney to negotiate a settlement for you with the other side.
Possible Cause Of Migraine
Scher believes that a neurological explanation could be behind her teams findings:
A dysfunction in the brain messenger dopamine is common to both Parkinsons and RLS, and has been hypothesized as a possible cause of migraine for many years. Symptoms of migraine such as excessive yawning, nausea and vomiting are thought to be related to dopamine receptor stimulation.
She says that the findings should lead to future investigations, and that more research should focus on exploring this possible link through genetic studies.
The findings suggest that there may be some common ground between Parkinsons and migraine the conditions of which are not well known and further research in this direction may be able to shed further light on these debilitating diseases.
Recently, Medical News Today reported on a phone app that could measure Parkinsons progression in its users.
Also Check: Does Magnesium Help Parkinson’s
