Dopaminergic Features And Their Treatment
Patients with PD usually present with features indicative of degeneration of nigrostriatal pathways. A useful clinical definition for PD is asymmetric onset of an akinetic rigid syndrome with resting tremor and a good response to levodopa. When applied by neurologists with an interest in movement disorders, this definition has a pathological correlation exceeding 98%. When treatment is considered appropriate, and this is a topic discussed in detail below, a variety of options is available. The use of dopaminergic drugs improves motor function, significantly reduces both the morbidity and mortality of PD, and improves quality of life.
Levodopa remains the drug most commonly used in PD. It is very effective in improving bradykinesia and rigidity, and in practice remains the gold standard against which other drugs are judged. Some studies, predominantly in vitro, have suggested that levodopa may be toxic. However, such data are conflicting, and some laboratory studies have suggested a growth factor-like effect for levodopa. Overall, the pre-clinical evidence for levodopa toxicity is not convincing and there are no data to indicate that any toxic action is of clinical relevance.
Table 1
Percentage of patients remaining on dopamine agonist monotherapy at years 14 and years 15 during treatment trials
Keep A Medicine And Symptoms Diary
Keeping a diary can help you to monitor your condition and keep track of your medicines. A diary can be a useful way of letting your doctor know what problems youre experiencing, any changes in your condition from day-to-day or over a period of time, and how well your medicine is controlling your symptoms. It can also help remind you of things you want to discuss during your appointment that you may otherwise forget. You can also use it to record any embarrassing issues that you want help with but find difficult to ask about. Here is some advice on the type of information you might want to keep track of if you have Parkinsons yourself, or if you are caring for somebody else with Parkinsons.
What Are The Early Warning Signs Of Parkinson’s Disease
Parkinsons warning signs can be motor symptoms like slow movements, tremors or stiffness. However, they can also be non-motor symptoms. Many of the possible non-motor symptoms can appear years or even decades ahead of motor symptoms. However, non-motor symptoms can also be vague, making it difficult to connect them to Parkinson’s disease.
Non-motor symptoms that might be early warning signs include:
- Sleep problems such as periodic limb movement disorder , rapid eye movement behavior disorder and restless legs syndrome.
Read Also: How Long Can You Live With Parkinson’s
What Medications And Treatments Are Used
Medication treatments for Parkinsons disease fall into two categories: Direct treatments and symptom treatments. Direct treatments target Parkinsons itself. Symptom treatments only treat certain effects of the disease.
Medications
Medications that treat Parkinsons disease do so in multiple ways. Because of that, drugs that do one or more of the following are most likely:
Several medications treat specific symptoms of Parkinson’s disease. Symptoms treated often include the following:
- Erectile and sexual dysfunction.
- Hallucinations and other psychosis symptoms.
Deep brain stimulation
In years past, surgery was an option to intentionally damage and scar a part of your brain that was malfunctioning because of Parkinsons disease. Today, that same effect is possible using deep-brain stimulation, which uses an implanted device to deliver a mild electrical current to those same areas.
The major advantage is that deep-brain stimulation is reversible, while intentional scarring damage is not. This treatment approach is almost always an option in later stages of Parkinson’s disease when levodopa therapy becomes less effective, and in people who have tremor that doesnt seem to respond to the usual medications.
Experimental treatments
Researchers are exploring other possible treatments that could help with Parkinsons disease. While these arent widely available, they do offer hope to people with this condition. Some of the experimental treatment approaches include:
Complementary And Alternative Therapies
Some people with Parkinsons disease find complementary therapies help them feel better. Many complementary treatments and therapies claim to ease the symptoms of Parkinsons disease.
However, theres no clinical evidence theyre effective in controlling the symptoms of Parkinsons disease.
Most people think complementary treatments have no harmful effects. However, some can be harmful and they shouldnt be used instead of the medicines prescribed by your doctor.
Some types of herbal remedies, such as St Johns wort, can interact unpredictably if taken with some types of medication used to treat Parkinsons disease.
If youre considering using an alternative treatment along with your prescribed medicines, check with your care team first.
Don’t Miss: Drugs To Treat Parkinson’s Tremor
When Should I See My Healthcare Provider Or When Should I Seek Care
You should see your healthcare provider as recommended, or if you notice changes in your symptoms or the effectiveness of your medication. Adjustments to medications and dosages can make a huge difference in how Parkinsons affects your life.
When should I go to ER?
Your healthcare provider can give you guidance and information on signs or symptoms that mean you should go to the hospital or seek medical care. In general, you should seek care if you fall, especially when you lose consciousness or might have an injury to your head, neck, chest, back or abdomen.
Who Does It Affect
The risk of developing Parkinsons disease naturally increases with age, and the average age at which it starts is 60 years old. Its slightly more common in men or people designated male at birth than in women or people designated female at birth .
While Parkinsons disease is usually age-related, it can happen in adults as young as 20 .
Also Check: How Do People Get Parkinson’s Disease
Impulsive And Compulsive Behaviours
People who experience impulsive and compulsive behaviours cant resist the temptation to carry out an activity often one that gives immediate reward or pleasure.
Behaviours may involve gambling, becoming a shopaholic, binge eating or focusing on sexual feelings and thoughts. This can have a huge impact on peoples lives including family and friends.
Not everyone who takes Parkinsons medication will experience impulsive and compulsive behaviours, so these side effects should not put you off taking your medication to control your symptoms.
If you have a history of behaving impulsively you should mention this to your GP, specialist or Parkinsons nurse.
Asking your specialist to make changes to your medication regime or adjusting the doses that you take is the easiest way to control impulsive and compulsive behaviours. So, if you or the person you care for is experiencing this side effect, tell your healthcare professional as soon as possible before it creates large problems.
If you are not able to get through to your healthcare professional straight away, you can call our Parkinsons UK helpline on 0808 800 0303.
We have advice that can help you manage impulsive and compulsive behaviours as well as information on what behaviour to look out for.
If you’re under treatment for coronavirus, and are experiencing side effects with your Parkinson’s treatment, please report it on the government’s Yellow Card website.
Why Is This Medication Prescribed
The combination of levodopa and carbidopa is used to treat the symptoms of Parkinsons disease and Parkinsons-like symptoms that may develop after encephalitis or injury to the nervous system caused by carbon monoxide poisoning or manganese poisoning. Parkinsons symptoms, including tremors , stiffness, and slowness of movement, are caused by a lack of dopamine, a natural substance usually found in the brain. Levodopa is in a class of medications called central nervous system agents. It works by being converted to dopamine in the brain. Carbidopa is in a class of medications called decarboxylase inhibitors. It works by preventing levodopa from being broken down before it reaches the brain. This allows for a lower dose of levodopa, which causes less nausea and vomiting.
You May Like: Does Anesthesia Affect Parkinson’s Disease
Speech And Occupational Therapy
Parkinsons disease can lead to slurred speech and difficulty swallowing. A speech and language therapist can provide muscle training techniques that may help overcome some of these problems.
An occupational therapist can help identify everyday tasks that can be challenging and work with the person to find practical solutions.
This may include new strategies for dressing, preparing meals, performing household chores, and shopping. Adaptations to the home environment can also make daily living easier.
For people with Parkinsons disease, deep brain stimulation may help manage:
- an electrode inside the part of the brain that controls movement
- a pacemaker-like device, or neurostimulator, under the skin in the upper chest
- a wire under the skin connecting the neurostimulator to the electrode
The neurostimulator sends electrical impulses along the wire and into the brain via the electrode. These impulses can prevent symptoms by interfering with the electrical signals that cause them.
There is a small risk of brain hemorrhage, infection, and headaches. Some people may see no improvement, or their symptoms may worsen. There may also be discomfort during stimulation.
Nevertheless, the AAN considers this treatment safe and effective for specific people and say any adverse effects are usually mild and reversible. Anyone considering this treatment should discuss the pros and cons with a healthcare professional.
Which Medication Will I Take
You will be prescribed levodopa, a dopamine agonist or an MAO-B inhibitor. Which medication you take depends on how much your symptoms affect you and other factors, such as your age and your lifestyle.
Most people find they tolerate their treatment well and will return to clinic after six to eight weeks to review their response. This is when your specialist or Parkinsons nurse will increase or decrease the doses, the frequency, or add new drugs until your symptoms are as controlled as possible.
Before leaving the clinic you should get the contact details of your Parkinsons nurse or the number of the clinic in case you have any problems with side effects.
Don’t Miss: Parkinson’s Stages And Symptoms
New Medications For Off Time
A number of new medications approved recently are designed to reduce OFF time. These medications fall into two major categories:
- Medications that lengthen the effect of a carbidopa/levodopa dose
- Medications that are used as needed if medication effects wear off
Well give specific examples below. In general, new medications that extend the length of a carbidopa/levodopa dose are used if OFF time is somewhat predictable and occurs prior to next dose. New medications that are used as needed are most beneficial when OFF time is not predictable.
New medications that lengthen the effect of a dose of carbidopa/levodopa
- Istradefylline is an adenosine A2A receptor antagonist which was approved in the US in 2019 as an add-on therapy to levodopa for treatment of OFF time in PD. Unlike many of the other medications, it has a novel mechanism of action and is the first medication in its class to be approved for PD. It acts on the adenosine receptor, which modulates the dopaminergic system, but is not directly dopaminergic. The drug was developed in Japan and underwent clinical trials both in Japan and in the US.
- Opicapone is a catechol-O-methyltransferase inhibitor that is taken once a day. It was approved in the US in 2020 as an add-on therapy to levodopa for motor fluctuations.
New formulations of levodopa designed to be used as needed if medication effects wear off
Other medications used as needed if medication effects wear off
What Are The Side Effects Of Parkinsons Drugs
The most common reactions include nausea, vomiting, dizziness , sleepiness and visual hallucinations.
In the last few years, levodopa and dopamine agonists in particular have been associated with the emergence of behavioral changes such as impulse control disorders. These are characterized by failure to resist an impulse to perform certain actions.
Impulse control disorders include a range of behaviors such as compulsive gambling or shopping, hypersexuality, binge eating, addiction to the Internet or to other recreational activities. These activities are often pleasant in the moment, but over time may become harmful to you or to others. If you are experiencing these behaviours, tell your neurologist/doctor. Often the medication can be adjusted which can reduce or control the behaviour.
Care partners can play an important role in helping to identify when these behaviours occur. If you are a care partner, tell the person if you have noticed a change in his/her behaviour or personality and encourage him/him/her to speak with the doctor immediately so medication can be adjusted.
Read Also: What Are The Odds Of Getting Parkinsons Disease
You May Like: Is Parkinson’s A Neurological Disease
What Can I Expect If I Have This Condition
Parkinsons disease is a degenerative condition, meaning the effects on your brain get worse over time. However, this condition usually takes time to get worse. Most people have a normal life span with this condition.
You’ll need little to no help in the earlier stages and can keep living independently. As the effects worsen, youll need medication to limit how the symptoms affect you. Most medications, especially levodopa, are moderately or even very effective once your provider finds the minimum dose you need to treat your symptoms.
Most of the effects and symptoms are manageable with treatment, but the treatments become less effective and more complicated over time. Living independently will also become more and more difficult as the disease worsens.
How long does Parkinsons disease last?
Parkinsons disease isnt curable, which means its a permanent, life-long condition.
Whats the outlook for Parkinsons disease?
Parkinson’s disease isn’t fatal, but the symptoms and effects are often contributing factors to death. The average life expectancy for Parkinson’s disease in 1967 was a little under 10 years. Since then, the average life expectancy has increased by about 55%, rising to more than 14.5 years. That, combined with the fact that Parkinson’s diagnosis is much more likely after age 60, means this condition doesn’t often affect your life expectancy by more than a few years .
Can Parkinson’s Disease Be Cured
No, Parkinson’s disease is not curable. However, it is treatable, and many treatments are highly effective. It might also be possible to delay the progress and more severe symptoms of the disease.
A note from Cleveland Clinic
Parkinson’s disease is a very common condition, and it is more likely to happen to people as they get older. While Parkinson’s isn’t curable, there are many different ways to treat this condition. They include several different classes of medications, surgery to implant brain-stimulation devices and more. Thanks to advances in treatment and care, many can live for years or even decades with this condition and can adapt to or receive treatment for the effects and symptoms.
Also Check: How To Diagnosis Parkinson’s Disease
Levodopa: The Most Effective Drug For Treating Parkinsons
Levodopa, also known as L-DOPA, has long been, and continues to be, the most effective drug in treating Parkinsons disease symptoms. Most people with Parkinsons disease will take this drug at some point. There are side effects that can occur with Levodopa including nausea, fatigue and orthostatic hypotension. Often these side effects can be successfully treated so that Levodopa can be tolerated better. In addition, as the disease progresses and the brain has less ability to produce and process dopamine, dyskinesias, or involuntary movements can develop from Levodopa.
Symptoms Of Parkinsons Disease
Parkinsons has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Muscle stiffness, where muscle remains contracted for a long time
- Slowness of movement
- Impaired balance and coordination, sometimes leading to falls
Other symptoms may include:
The symptoms of Parkinsons and the rate of progression differ among individuals. Early symptoms of this disease are subtle and occur gradually. For example, people may feel mild tremors or have difficulty getting out of a chair. They may notice that they speak too softly, or that their handwriting is slow and looks cramped or small. Friends or family members may be the first to notice changes in someone with early Parkinsons. They may see that the persons face lacks expression and animation, or that the person does not move an arm or leg normally.
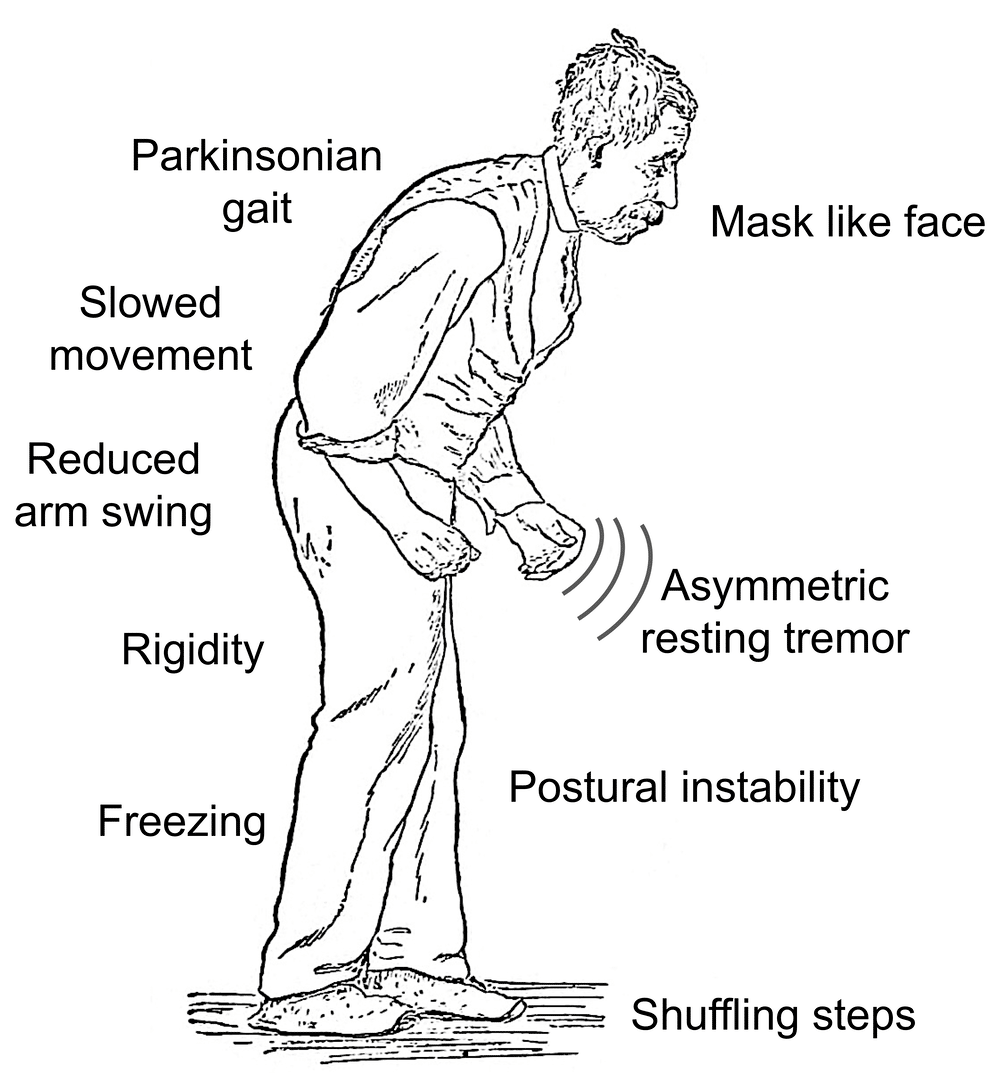
People with Parkinson’s disease often develop a parkinsonian gait that includes a tendency to lean forward take small, quick steps and reduce swinging their arms. They also may have trouble initiating or continuing movement.
Symptoms often begin on one side of the body or even in one limb on one side of the body. As the disease progresses, it eventually affects both sides. However, the symptoms may still be more severe on one side than on the other.
Recommended Reading: Does Susan Collins Have Parkinson Disease
Poorly Tolerated Or Unproven Treatments
Until recently, the only available treatments for psychosis consisted of reducing dopaminergic tone. At its extreme, this consisted of removing all antiparkinsonian medications for a period of time, a so-called drug holiday. As Friedman observed, however, this was not a holiday in the usual sense, since motor function quickly worsened . In fact, patients could develop a neuroleptic malignant syndromelike presentation, which occasionally could be lethal. Dopamine D2-like receptor antagonists prior to the 1990s all had unacceptable motor side effects.
In the 1990s and 2000s, newer antipsychotics were tried eagerly in PD psychosis in hopes of better tolerability . Like their predecessors, they block dopamine at D2-like receptors, but have more complex pharmacology, often including serotonin 5HT2 receptor antagonism or lower affinity for striatal D2Rs, and cause fewer motor side effects in patients with schizophrenia . Small, open trials with remoxipride and zotepine generally seemed positive, but several patients experienced intolerable motor side effects . Risperidone at low dose showed some promise in early reports , but intolerable motor side effects in others . In the only controlled trial with risperidone in PD, it was more effective than clozapine but less well tolerated . In controlled trials, olanzapine proved superior to placebo for PD psychosis , but worsened motor function .
