Stages Of Parkinsons Disease
The progression of Parkinsons disease is commonly divided into five stages of symptoms that worsen over time. However, while some people with Parkinsons may become severely disabled, others may not.
Not everyone experiences all the symptoms of Parkinsons, and symptoms are not necessarily experienced in the same order, says Dr. Maurer.
The stages of Parkinsons are generally defined as follows.
How Is Parkinson Disease Treated
Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
Trouble Moving Or Walking
Do you feel stiff in your body, arms or legs? Have others noticed that your arms dont swing like they used to when you walk? Sometimes stiffness goes away as you move. If it does not, it can be a sign of Parkinson’s disease. An early sign might be stiffness or pain in your shoulder or hips. People sometimes say their feet seem stuck to the floor.What is normal?If you have injured your arm or shoulder, you may not be able to use it as well until it is healed, or another illness like arthritis might cause the same symptom.
Recommended Reading: Living With Someone With Parkinson’s
Can I Travel To Other States To Receive Treatment If My State Is Not Covered By Blue Cross Blue Shield
It is our understanding that under the Blue Card Network, patients traveling outside of their home state for treatment at a facility providing MRgFUS would be subject to their home plan coverage decision. We recommend confirming coverage with your health plan and the treatment center prior to treatment.
Do Private Health Insurance Plans Cover The Treatment

Aetnas coverage of focused ultrasound treatment of essential tremor that does not respond to medications applies across the country. Also, a total of 39 Independent Blue Cross Blue Shield Association plans have adopted the National Medical Policy for coverage of MR-guided focused ultrasound to treat medication-refractory Essential Tremor.
You May Like: Can You Fly With Parkinson’s Disease
Starting Palliative Care In Patients With Pd
Patients with PD benefit early from palliative care in view of the impact of the disease impairing autonomy and quality of life. The provision of palliative care in patients with PD focuses on unmet needs and should be aligned with patient priorities. It is recommended that a palliative care approach should be applied from the early phase, throughout the course of the disease, complementing but not replacing other treatments . However, like other patients with chronic neurological condition, the individual needs may vary over time, therefore it is suggested that a model of dynamic involvement of palliative care services should be adopted . The services can be triggered at times of particular symptoms or psychosocial issuessuch as the start of new interventions or at the very end of life.
For patients with complex physical, social, psychological and/or spiritual needs that do not respond to simple or established protocols of palliative care, there should be access to the support from specialist palliative care service .
However, rate of use of hospice in PD patients has been low . Caregivers often considered palliative care services to be synonymous with hospice care, and hence they did not consider this service option . Health care workers also have uncertainty about timing of palliative care, such that it was often not introduced until a crisis point .
Motor Symptoms And Global Disability
Motor symptoms, as measured using the Unified Parkinsons Disease Rating Scale , Hoehn and Yahr Scale and the Progressive Supranuclear Palsy Rating Scale , were significant predictors of mortality in patients with PDRD. Beyer et al found higher mean UPDRS scores, 65 versus 42 , suggesting that greater motor impairment predicted death. Studies with median follow-up times ranging from 4 to 8 years estimated the association of 10-unit increases in baseline motor UPDRS Score on mortality and found statistically significant increased HRs for mortality of 1.17 up to 1.4 for each 10-unit increase in UPDRS Score. Baseline H& Y staging was significantly higher among those who died ) compared with those who survived ). Posada et al went further by splitting H& Y into early and later progression stages at baseline as a predictor for mortality and found that HRs increased by stage, from 1.5 for H& Y stages 1 and 2 to 2.3 for H& Y stages 35, both compared with patients with no PD and after controlling for comorbidities and demographic characteristics. Oosterveld et al stratified UPDRS total motor scores by greater than or equal to 30 compared with less than 30 and found an HR of 1.63 . Chiu et al compared the association of PSPRS scores on mortality and found increased HRs of 1.96 for 3548 on the PSPRS, 2.99 for 4862 and 8.55 for greater than 62 when compared with scores of 034.
You May Like: Chemical Herbicide Linked To Parkinson’s
How Can I Support Someone With Parkinsons At The Advanced Or Palliative Stage
In the advanced stages of Parkinsons, your patients care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the whole person to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinsons may be supported by a number of professionals, including a Parkinsons nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinsons also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinsons should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the persons wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesnt want to have in the future this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
Treating Parkinsons With Complementary Medicine
Complementary medicine incorporates many different practices that can be used alongside conventional medicine to try to ease PD symptoms. There is typically not as much rigorous data to support the use of complementary medicine techniques, as compared to conventional medicine, but many patients find them helpful. These include yoga and massage.
Read Also: Parkinsons And Gut Health
Don’t Miss: How Does Parkinson’s Disease Develop
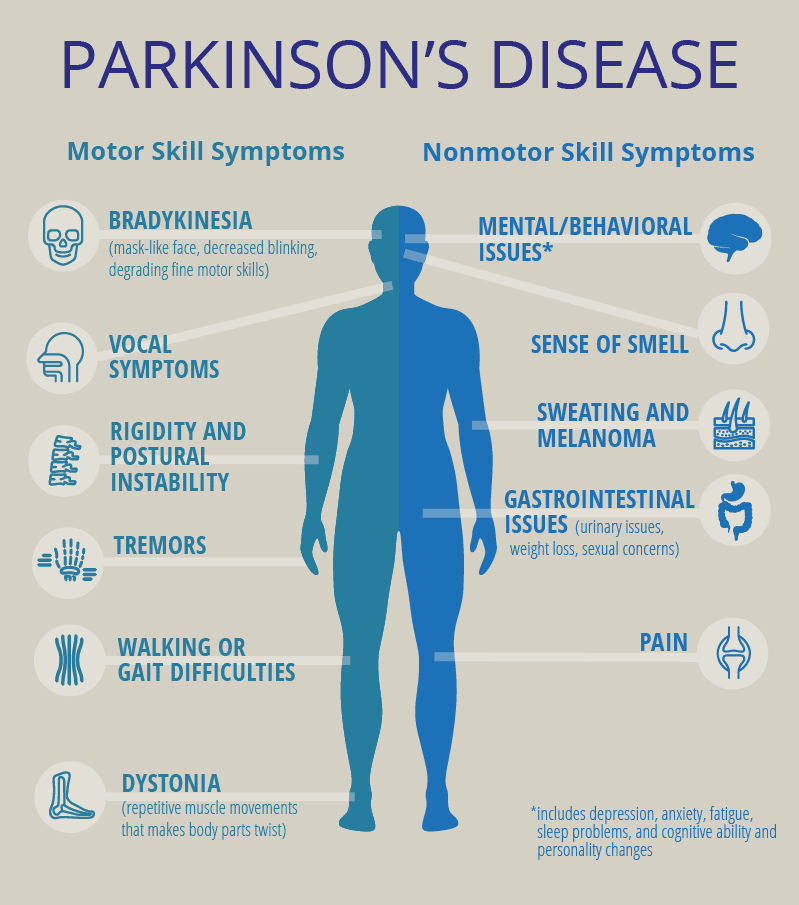
What Are The Symptoms Of Parkinsons
The main motor symptoms of Parkinsons are:
- slowness of movement
- problems with balance.
However, the condition doesnt only affect movement. People living with the condition can experience a range of non-motor symptoms that can often have a greater impact on their lives than movement difficulties.
Non-motor symptoms include:
- urinary urgency, frequency
These non-motor symptoms are present at all stages of the condition but they can become more severe in the later stages of Parkinsons and have a major impact on quality of life.
Parkinsons gets worse over time and it can be difficult to predict how quickly the condition will progress. For most people, it can take years for the condition to progress to a point where it can cause major problems. For others, Parkinsons may progress more quickly.
Also Check: Zhichan Capsule
Comparing Cbd With Levodopa For Parkinsons
Levodopa is an established treatment for Parkinsons disease. Although its not perfect, its currently the most effective treatment for PD. It helps boost the level of dopamine in the brain.
Levodopa is effective at targeting the motor symptoms of the condition, such as tremors or muscle stiffness.
However, this medicine does little to combat the nonmotor symptoms of Parkinsons disease. These are the problems that can significantly affect a persons daily life. They include anxiety, sleep disturbance, fatigue, irritation, and depression.
Furthermore, prolonged use of levodopa may result in side effects like elevated anxiety, agitation, confusion, and nausea. It may also trigger tremors that result from the medication itself, not PD.
CBD appears to help with those nonmotor symptoms and potential side effects, rather than physical problems. A study with more than 200 participants found that regular use of cannabis was highly effective on non-motor symptoms of Parkinsons Disease. However, this study included a combination of THC with CBD, not CBD oil alone.
You May Like: Helping Someone With Parkinson’s Disease
How Is It Treated And Is There A Cure
For now, Parkinsons disease is not curable, but there are multiple ways to manage its symptoms. The treatments can also vary from person to person, depending on their specific symptoms and how well certain treatments work. Medications are the primary way to treat this condition.
A secondary treatment option is a surgery to implant a device that will deliver a mild electrical current to part of your brain . There are also some experimental options, such as stem cell-based treatments, but their availability often varies, and many aren’t an option for people with Parkinsons disease.
Bilateral Or Midline Involvement Without Impairment Of Balance
Months or years later similar symptoms and signs are noticed on the opposite side of the body, or other signs appear in midline what physicians call Axial signs. These may include: bilateral loss of facial expression decreased blinking speech abnormalities soft voice, monotony, fading volume after starting to speak loudly, slurring, stiffness of truncal muscles making the patient appear awkward and stiff or resulting in neck and back pain postural abnormalities causing stooping, generalized slowness in, but still capable of, carrying out all activities of daily living, sometimes an aggravation to those waiting for the patient to complete tasks.
Usually the diagnosis is easy at this Stage if it has been preceded by a clear cut tremor or other symptom on one side. But not all Parkinsons patients have tremor or other definite signs of Stage I unilateral Parkinsonism. If Stage I was missed and the predominant symptoms at Stage II are only slowness and a lack of spontaneous movement, the diagnosis may still be in doubt. For example, even in Stage II, Parkinsonism may be interpreted as only advancing age.
Recommended Reading: The New Definition And Diagnostic Criteria Of Parkinson’s Disease
What Is Parkinsons Disease
Parkinsons disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinsons disease and the degree of impairment varies from person to person. Many people with Parkinsons disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinsons disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinsons disease will increase in the future. Adult-onset Parkinsons disease is most common, but early-onset Parkinsons disease , and juvenile-onset Parkinsons disease can occur.
You May Like: Yopd Life Expectancy
How Is Parkinson’s Disease Diagnosed
Diagnosis is difficult at every stage of the disease, but particularly in the early stages. No single test can provide a diagnosis. A diagnosis will likely involve physical and neurological examinations, conducted over time to assess changes in reflexes, coordination, muscle strength, and mental function. Your doctor might also see how you respond to medicine.
You may need to have brain imaging tests to rule out other conditions that might be causing your symptoms. Such tests could include MRI and CT scans and possibly some other types of scans. Blood tests may also be done to exclude other illnesses.
Don’t Miss: Emory Parkinson’s Disease Research
What Are The Stages Of Parkinsons
Doctors sometimes use five stages to describe the progress of Parkinsons disease. Each stage presents new or changing symptoms that a person is likely to encounter.
It is worth noting that not everyone will reach the advanced stages. Some people find that the symptoms remain mild and that they can continue to live independently and be mobile.
Dividing the condition into stages helps doctors and caregivers understand and address some of the challenges a person is experiencing as it progresses.
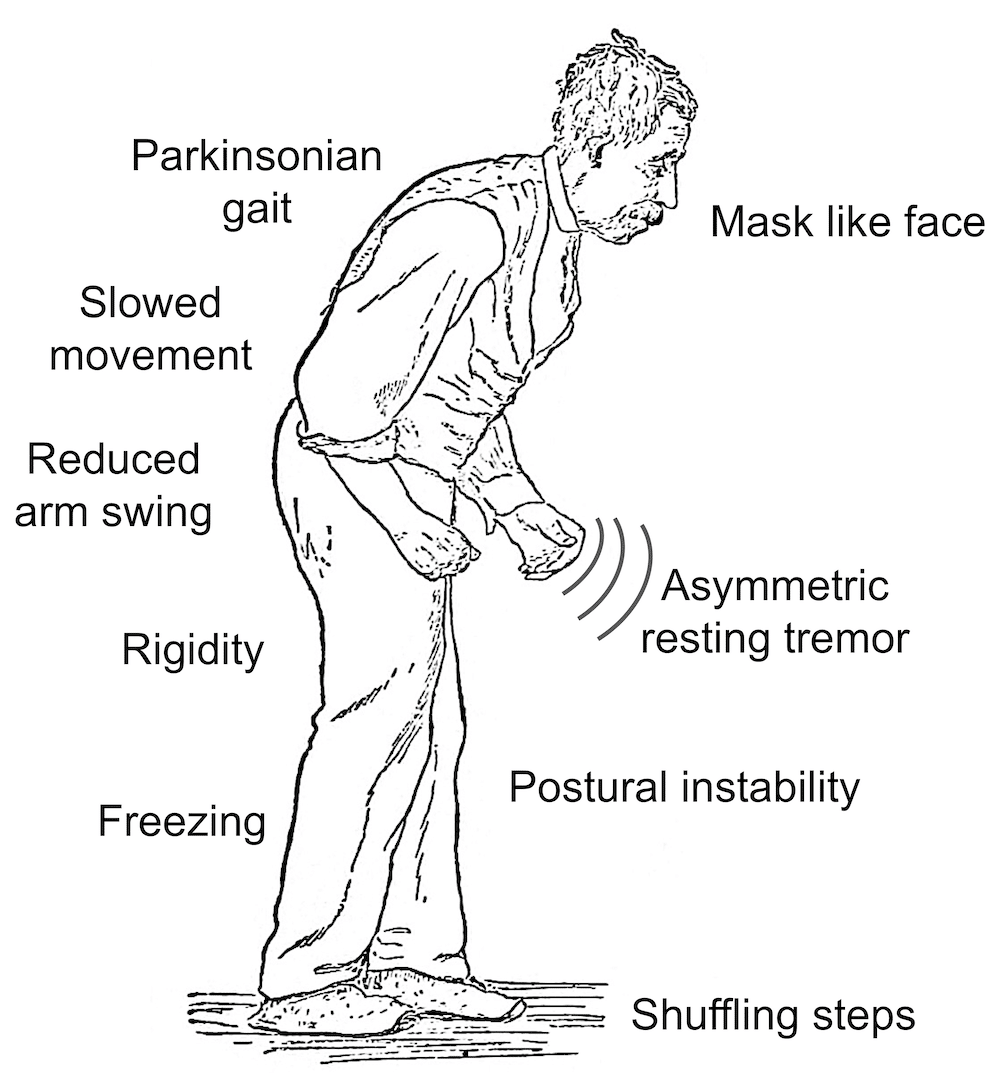
What Are The Primary Motor Symptoms Of Parkinsons Disease
There are four primary motor symptoms of Parkinsons disease:
- postural instability
Observing two or more of these symptoms is the main way that physicians diagnose Parkinsons.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinsons disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinsons disease has a tremor, nor is a tremor proof of Parkinsons. If you suspect Parkinsons, see a neurologist or movement disorders specialist.
Introducing an easier way to track your symptoms and manage care.
Also Check: What Is The Meaning Of Parkinson’s Disease
Diagnosis And Management Of Parkinsons Disease
There are no diagnostic tests for Parkinsons. X-rays, scans and blood tests may be used to rule out other conditions. For this reason, getting a diagnosis of Parkinsons may take some time.
No two people with Parkinsons disease will have exactly the same symptoms or treatment. Your doctor or neurologist can help you decide which treatments to use.
People can manage their Parkinsons disease symptoms through:
- seeing a Doctor who specialises in Parkinsons
- multidisciplinary therapy provided for example, by nurses, allied health professionals and counsellors
- deep brain stimulation surgery .
What Is Focused Ultrasound
Focused Ultrasound is a treatment option where sound waves can be focused through the skull to target a very specific location deep within the brain without the need for incisions or holes in the skull. This is the same target used for years with other more invasive surgery, but now can be reached without incisions or anesthesia.
Focused Ultrasound waves converge at a focal point to create a small lesion in the targeted area of the brain.
The MRI system is the eyes of the treatment, enabling the physician to identify and target the treatment area with high precision as well as monitor the temperature during treatment.
Risks associated with any thalamotomy, include transient and/or permanent sensory numbness, imbalance, and/or gait disturbance. These events are generally transient and mild or moderate in severity. Other risks and adverse events associated with the treatment include brief sonication-related pain, brief sonication-related dizziness, nausea and potential for deep vein thrombosis associated with lengthy time on the treatment bed.
Focused Ultrasound may be a treatment option for patients with medication-refractory essential tremor who are at least 22 years old.
Don’t Miss: How Do You Contract Parkinson’s Disease
What Does Kill People With Parkinsons
While no one dies directly from Parkinsons, you may be asking yourself what does typically cause death in Parkinsons patients. The two of the biggest causes of death for people with Parkinsons are Falls and Pneumonia:
Falls Parkinsons patients are typically at an increased risk of falls due to postural instability and other symptoms of Parkinsons. This poses a great risk to those with PD because falls are the leading cause of injury-related deaths among those 65 years or older according to the CDC. It is important to take precautions to limit the risk of falling in your home. This can be done by wearing special grip socks to prevent slipping or installing handrails in high-risk areas like the shower or staircase. In addition, you should talk with your doctor about getting a physical therapy evaluation periodically to strengthen your balance reflexes and help you develop other strategies to keep you safe in the home.
How Fast Does Parkinson’s Disease Progress
People tend to move through the Parkinson’s disease stages slowly, usually over the course of years. Research has shown that the disease tends to progress less rapidly in people who are diagnosed at a younger age than those diagnosed later in life.
What’s more, Parkinson’s disease may begin decades before a patient even notices a single motor symptom.
“We know that Parkinson’s disease actually starts many, many years before you see that tremor or that shuffling,” Lynda Nwabuobi, MD, assistant professor of clinical neurology at Weill Cornell Parkinson’s Disease and Movement Disorders Institute, tells Health. “We think at least 30 years.”
That early stage of Parkinson’s disease is called the “pre-motor” stage. It happens before a person has been diagnosed, and may include symptoms like loss of smell, REM sleep behavior disorder , and constipation.
“Patients will often tell you, ‘Yeah, I haven’t had a good sense of smell for many, many years,'” Dr. Nwabuobi says. “Or their spouse says, ‘He kicks a lot in his sleep. He’s done that since we were married.'”
But the reality is that, as with Parkinson’s disease symptoms, Parkinson’s disease progression will vary from person to person. “Some people have had Parkinson’s for two years and they’re not doing so well,” Dr. Nwabuobi says. “And then some people have Parkinson’s for 20 years and they’re doing great and living their lives.”
Also Check: Is There A Test To See If You Have Parkinson’s
