Notable Figures With Parkinsons
Although more than 10 million people worldwide live with Parkinson’s disease , the general public’s understanding of disease symptoms is often limited to what is seen in the media. Many people only know Parkinson’s as the disease that Muhammad Ali had, or Michael J. Fox has.
However, when a household name such as Ali or Fox announces their diagnosis, Parkinson’s coverage briefly spikes. While a diagnosis is upsetting, when notable figures are public about their disease, the coverage helps increase awareness and understanding, while personalizing Parkinson’s for those with no other connection.
A PD diagnosis is universally difficult to cope with, but with a platform to speak from and fans to speak to, here’s a list of notable figures that have helped shape the Parkinson’s conversation:
What Are The Stages Of Parkinsons Disease
Parkinsons disease is often divided into two parts: early stage and advanced stage disease.
- Early stage: when symptoms appear and start to affect everyday activities, such as washing, getting dressed and walking.
- Advanced stage: when motor complications occur from the long term use of one of the main treatments for Parkinsons disease, levodopa.
What Is The Trend Over Time In The Prevalence And Incidence Of Parkinsonism In Canada
Between 20042005 and 20132014, the number of Canadians living with diagnosed parkinsonism increased from approximately 61,000 to 84,000, while the number of Canadians newly diagnosed increased from approximately 8,000 to 10,000. However, during the same period, there was no significant change in the age-standardized prevalence proportion, which remained at 0.4%, or the incidence rate, which went from 51.6 per 100,000 to 52.6 per 100,000. The sex differential also remained constant over time for both indicators .
Figure 3: Age-standardized prevalence and incidence of diagnosed parkinsonism, including Parkinsons disease, among Canadians aged 40 years and older, by sex, 20042005 to 20132014
| Indicator | |
|---|---|
| 67.8 | 40.3 |
Notes: Age-standardized estimates to the 2011 Canadian population. The 95% confidence interval shows an estimated range of values which is likely to include the true value 19 times out of 20. The 95% confidence intervals of the prevalence estimates are too small to be illustrated.Data source: Public Health Agency of Canada, using Canadian Chronic Disease Surveillance System data files contributed by provinces and territories, July 2017.
You May Like: Does Diet Soda Cause Parkinson’s
Q: How Does The Delta Variant Affect Someone With Pd
A: We do not have any specific data yet on how the Delta variant affects people with PD.
The COVID-19 virus, like all viruses, is able to mutate and create variants of itself. Many variants of COVID-19 have been identified around the world. Only a few of these variants have been of concern to public health however, because they have a characteristic that makes the virus either more easily transmissible or more likely to cause significant disease. The Delta variant is currently the variant of concern and has been shown to be more easily transmitted from person to person than prior variants of COVID.
The vaccines approved in the US do offer protection against the Delta variant, but not to the extent that was seen in the original trials. That means that fully vaccinated people are more likely to get infected with the Delta variant of COVID-19 than other variants. However, the major goal of the vaccines is to prevent severe illness, hospitalization, and death from COVID-19 and all the approved vaccines are approximately 90% effective in preventing these consequences of infection. Therefore, vaccination remains extremely valuable.
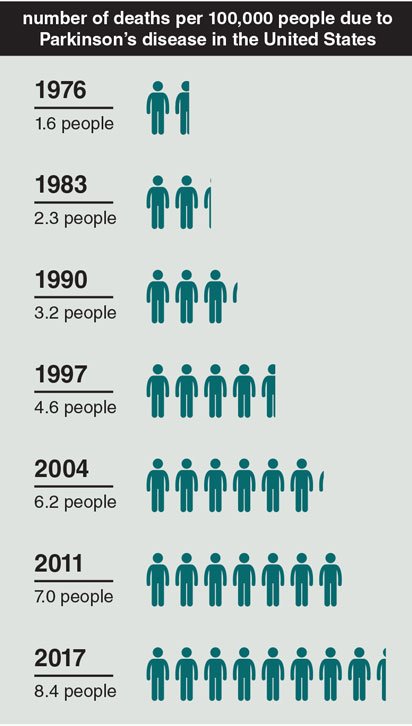
Mortality From Parkinsons Disease
With treatment, the life expectancy of people with PD is similar to that of the general population. However, dementia seems to largely impact life expectancy among people with PD, and about 50 percent to 80 percent of people with PD develop dementia in their lifetime. Risk factors for mortality include later age of onset, male sex, severity of motor impairment, presence of psychotic symptoms, and dementia. Early detection of disease, prevention of motor symptom progression, and treatment of dementia can increase life expectancy.8,9
Engage with the community by asking a question, telling your story, or participating in a forum.
Read Also: Thomas Daffron Wikipedia
Who Is Affected By Parkinsons Disease
Several studies have found that the incidence of PD is much more common in men than women.2,4 One estimate found that PD affects about 50 percent more men than women.2 The reasons for the differences in men and women with PD are unclear, although some suggested explanations are the protective effect of estrogen in women, the higher rate of minor head trauma and exposure to occupational toxins in men, and genetic susceptibility genes on the sex chromosomes.4
People with a close family member with Parkinsons have a small increased risk of developing the disease. About 15 percent to 25 percent of people with PD have a known relative with the disease.2
It is estimated that about 10 million people worldwide are living with PD. The incidence of the disease is higher in industrialized countries.3,4
The incidence of PD increases with age: while PD affects 1 percent of the population over the age of 60, this increases to 5 percent of the population over the age of 85.1
Approximately 5 percent of people with PD are diagnosed before the age of 60.1
Urban areas have a higher prevalence and incidence of PD.5
Freddie Roach: Boxing Trainer With Parkinson’s
Frederick “Freddie” Roach is a boxing trainer and former professional boxer. Bryant Gumbel included his story in the HBO series Real Sports, detailing Roach’s efforts to control his Parkinson’s disease with medication and continued work as a trainer. Roach, who began to show Parkinsons symptoms over 20 years ago, trains world-famous boxers at the Wild Card Boxing Club in Hollywood, California, which he owns. His client list has included the likes of Amir Khan, Manny Pacquiao, Mark Wahlberg, and Georges St. Pierre.
But having Parkinson’s hasn’t dimmed his commitment to boxing, even as it’s caused his speech to slur and his left arm to shake. “I’m in the gym every day it’s part of life. Instead of taking a vacation, I like what I do. My vacations are right here,” Roach said in a 2015 CBS interview.
Read Also: Stages Of Parkinson’s Disease Life Expectancy
Parkinsons Foundation Prevalence Project Finds Number Of People With Parkinsons Severely Underestimated
When a large population of people have a disease, like Parkinsons disease , its essential to have accurate numbers of how many people have the disease, where they live and why they have it. In our latest research initiative, we established the Parkinsons Prevalence Project to determine a more accurate representation of people living with PD today through a study called the Parkinsons Foundation Prevalence Project.
The Parkinsons Foundation Prevalence Project estimates that 930,000 people in the United States will be living with PD by the year 2020. This number will rise to 1.2 million by 2030.
“Our knowledge of Parkinsons has changed significantly and so has our understanding of how many people have this disease, said James Beck, PhD, Parkinsons Foundation Chief Scientific Officer and contributing author on the study. This study will help the Parkinsons Foundation attract the attention of federal and state government as well as the pharmaceutical industry to the growing need and urgency in addressing PD.
About The Study
The Parkinsons Foundation formed the Parkinsons Prevalence Project in 2014 to find an accurate estimate of PD prevalence because prior estimates were widely varied. The 1978 estimate extrapolated data for how many people in the nation have Parkinsons based on 26 cases of PD in a rural Mississippi county. The new Parkinsons Prevalence Project estimate is nearly double the 1978 study count.
The new study sought to answer two main questions:
What Causes Parkinson’s Disease
Parkinson’s disease occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. Normally, these neurons produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinson’s. Scientists still do not know what causes cells that produce dopamine to die.
People with Parkinson’s also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinson’s, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying-down position.
Many brain cells of people with Parkinson’s contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons disease and Lewy body dementia.
Read Also: Essential Oils Parkinson’s
How Were These Figures Calculated
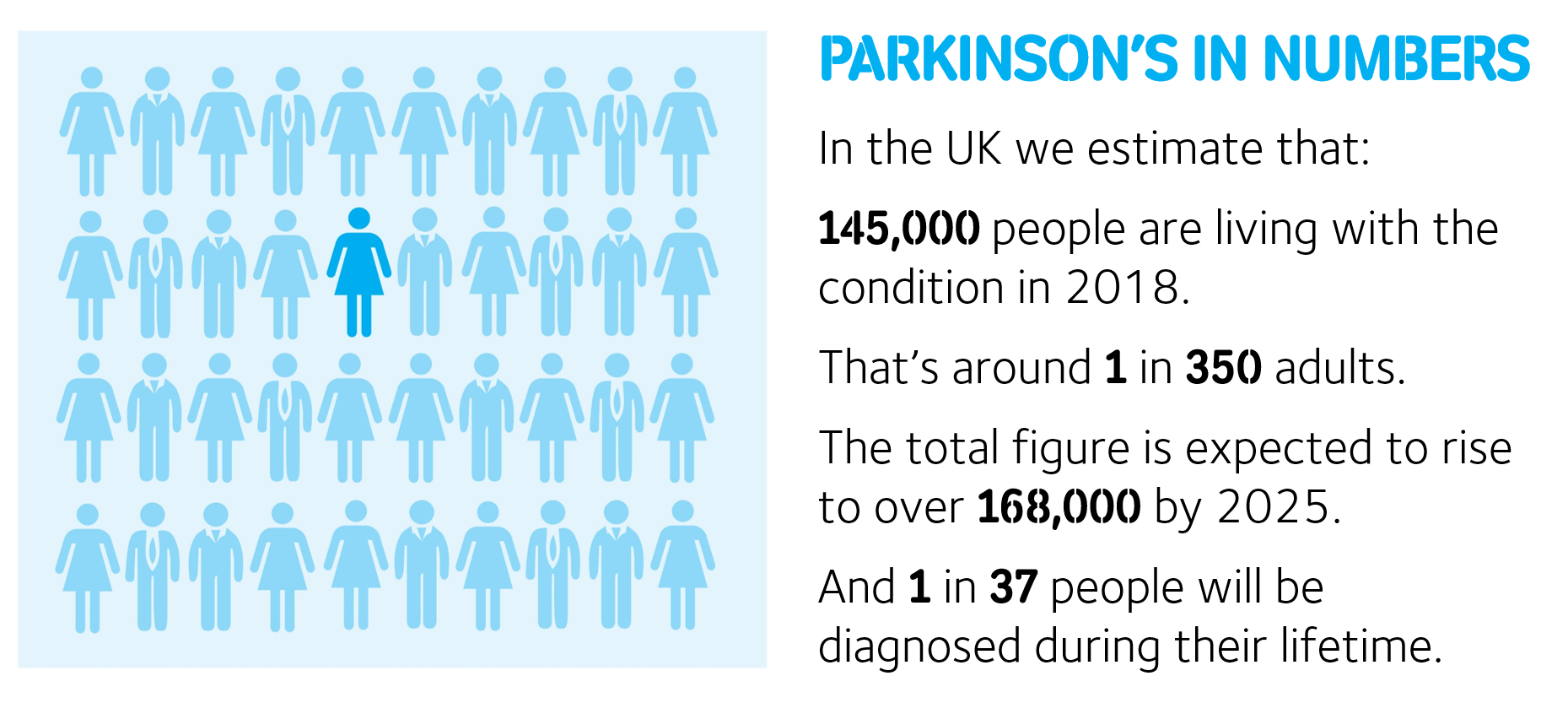
We analysed anonymous medical records of over 2.5 million individuals over the age of 20 registered with GPs in the UK from the Clinical Practice Research Datalink database.
Clinical experts helped us assess the records to work out how many patients had a definite diagnosis of Parkinsons and then we adjusted the numbers to make sure they matched the UK population in terms of age profile and gender.
Finally, we used projected population figures from the Office of National Statistics, to estimate how many people have Parkinsons in 2018 and how many will go on to be diagnosed in 2025 and beyond.
The UK population is growing and people are living longer, which means that the number of people of people living with Parkinsons is expected to rise.
For more information, you can
Medications For People With Parkinsons Disease
Symptoms of Parkinsons disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinsons medications fit into one of the following broad categories:
- levodopa dopamine replacement therapy
- dopamine agonists mimic the action of dopamine
- COMT inhibitors used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors prevent the metabolism of dopamine within the brain.
Recommended Reading: Parkinson Disease Prognosis Life Expectancy
The Plus Side Of An Early Diagnosis
The news is not nearly all bad for those with young-onset Parkinsons. For one thing, patients with YOPD are better candidates for surgical procedures and medical innovations being used or developed to treat Parkinsons disease. For another, younger patients are less likely to be coping with other health problems at the same time.
Targeting Parkinsons-Linked Protein Could Neutralize 2 of the Diseases Causes
Researchers report they have discovered how two problem proteins known to cause Parkinsons disease are chemically linked, suggesting that someday, both could be neutralized by a single drug designed to target the link.
Q: I Am On Amantadine For My Pd I Know That It Is Also An Anti
A: We do not have evidence that amantadine acts against COVID-19, so you should continue to assume that it is not effective against this coronavirus.
Tips and Takeaways
- Most people who are infected with COVID-19 will recover completely. However, older adults and those with underlying medical issues such as advanced PD are at an increased risk of developing serious outcomes from COVID-19 as compared to those who are younger and healthier.
- Three COVID-19 vaccines have been approved in the US.
- Getting vaccinated reduces your chances of contracting COVID-19, but those who are vaccinated can still contract COVID-19.
- Vaccination is about 90% effective in protecting against severe illness, hospitalization, and death, even for the new Delta variant
- Continue to monitor CDC guidelines for information on COVID-19.
- Talk with your doctor about any concerns you have about COVID-19 or COVID-19 vaccines.
Do you have a question or issue that you would like Dr. Gilbert to explore? Suggest a Topic
Dr. Rebecca Gilbert
APDA Vice President and Chief Scientific Officer
Don’t Miss: Cardinal Signs Of Parkinson’s
What Is Parkinsons Disease
Parkinsons disease is a progressive brain disorder that affects mobility and mental ability. If you or a loved one has been diagnosed with Parkinsons, you may be wondering about life expectancy.
According to some research, on average, people with Parkinsons can expect to live almost as long as those who dont have the condition.
What Makes Pd Hard To Predict
Parkinsonâs comes with two main buckets of possible symptoms. One affects your ability to move and leads to motor issues like tremors and rigid muscles. The other bucket has non-motor symptoms, like pain, loss of smell, and dementia.
You may not get all the symptoms. And you canât predict how bad theyâll be, or how fast theyâll get worse. One person may have slight tremors but severe dementia. Another might have major tremors but no issues with thinking or memory. And someone else may have severe symptoms all around.
On top of that, the drugs that treat Parkinsonâs work better for some people than others. All that adds up to a disease thatâs very hard to predict.
Don’t Miss: Does Lack Of Sleep Cause Parkinson’s
Q: Are There Any Studies Of The Effects Of The Covid
A: Currently, there is no data that the COVID-19 vaccine has any long-term negative effects on anyone, including those with PD. Some people with PD have reported a worsening of PD symptoms in the short term after vaccination, which then resolve. The Center for Disease Control instituted a vaccine safety monitoring system, called v-safe, which captures side effects of the vaccine. If you have side effects from the vaccine and have PD, you can alert the CDC using this system. This will be an invaluable tool for scientists to discover trends in vaccine side effect profiles.
How Is Parkinsons Diagnosed
Doctors use your medical history and physical examination to diagnose Parkinson’s disease . No blood test, brain scan or other test can be used to make a definitive diagnosis of PD.
Researchers believe that in most people, Parkinson’s is caused by a combination of environmental and genetic factors. Certain environmental exposures, such as pesticides and head injury, are associated with an increased risk of PD. Still, most people have no clear exposure that doctors can point to as a straightforward cause. The same goes for genetics. Certain genetic mutations are linked to an increased risk of PD. But in the vast majority of people, Parkinsons is not directly related to a single genetic mutation. Learning more about the genetics of Parkinsons is one of our best chances to understand more about the disease and discover how to slow or stop its progression.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
Men are diagnosed with Parkinsons at a higher rate than women and whites more than other races. Researchers are studying these disparities to understand more about the disease and health care access and to improve inclusivity across care and research.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
The Michael J. Fox Foundation has made finding a test for Parkinsons disease one of our top priorities.
Read Also: Is Parkinson’s Disease Fatal
Q: I Received The Covid
A: The vaccine is certainly able to cause short term side effects of fatigue, aches and even fever. There isnt extensive data yet on how it affects PD symptoms, just anecdotal data. For some people, PD symptoms are worse in the short term. This does not mean that your PD has progressed, and I would expect that you will return to your previous baseline in the next few days. I would talk with your neurologist about your worsened tremor as well.
The Impact Of Parkinsons Disease On Overall Health
Based on the Blue Cross Blue Shield Health Index, the overall health of those affected by Parkinsons is significantly lower than the general population. In 2017, the average BCBS Health Index for someone aged 30-64 with Parkinsons was 57, compared to 88 for the entire commercially insured population in this age range. This translates to an average of 10.7 years of healthy life lost for those with the condition compared to 3.4 years for the 30-64 population as a whole.4
Caring for someone with Parkinsons Disease
The majority of Parkinsons patients are cared for by informal caregivers, such as a family member. The physical, mental and emotional work this requires can be significant. The Impact of Caregiving on Mental and Physical Health found that caregivers have 26% poorer health compared to a benchmark population, as measured by the BCBS Health Index. In addition, a national survey conducted by the Blue Cross Blue Shield Association found that 1 in 4 unpaid caregivers are feeling more stress trying to balance work and family due to COVID-19.5
You May Like: Late Onset Parkinson’s
How Many Canadians Live With Parkinsonism And How Many Are Newly Diagnosed Each Year
Based on the latest estimates available , in 20132014, approximately 84,000 Canadians aged 40 years and older were living with diagnosed parkinsonism and 10,000 Canadians were newly diagnosed with this condition . The age-standardized prevalence was 1.5Footnote i times higher among males than among females , and similarly the age-standardized incidence was 1.7Footnote i times higher among males than females . The epidemiological burden of parkinsonism increases with age. In 20132014, when comparing estimates among Canadians aged 85 years and older vs. those aged 40-44 years, the prevalence of the condition was 169Footnote i times higher in the older age group , while the incidence was 48Footnote i times higher in the older age group .
Figure 1: Prevalence of diagnosed parkinsonism, including Parkinsons disease, by sex and age group, Canada, 20132014
| Age group |
|---|
| 44.7 | 55.1 |
Note: The 95% confidence interval shows an estimated range of values which is likely to include the true value 19 times out of 20. Data source: Public Health Agency of Canada, using Canadian Chronic Disease Surveillance System data files contributed by provinces and territories, July 2017.
