Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
The Solution For Hand Tremor Symptoms
Theres a remarkable glove gadget that can assist in controlling a persons hand tremors. Its thorough and delicate design allows it to stop the uncontrollable hand shaking enough for you to pick up and drink a cup of tea or coffee, or even write on a piece of paper. Meet the outstanding Steadi-Two glove made by us at Steadiwear. This glove uses a smart fluid that stiffens & works together with a counter-weight that moves in the opposite direction of your tremor. You can say its the solution for all of those unsteady and irritating hand tremors caused by Essential Tremor or Parkinsons.References:
How Long Can A Person Live With Stage 5 Parkinson
When patients reach stage five the final stage of Parkinson’s disease they will have severe posture issues in their back, neck, and hips. In end–stage of Parkinson’s disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
One may also ask, what do Parkinson’s patients usually die from? But the most common cause of death in those with Parkinson’s is pneumonia, because the disease impairs patients‘ ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
what happens in stage 5 Parkinson’s?
Stage Five of Parkinson’s Disease Stage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
How quickly can Parkinson’s progress?
While symptoms and disease progression are unique to each person, knowing the typical stages of Parkinson’s can help you cope with changes as they occur. Some people experience the changes over 20 years or more. Others find the disease progresses more quickly.
You May Like: What Are Early Warning Signs Of Parkinson’s Disease
Parkinsons Disease Late Stages: What Will Happen To Me
With advanced Parkinsons disease, stage 5 life expectancy can be months or years depending on how your condition presents. You are likely to need round-the-clock care at this stage, and you may not be able to move around independently. Patients with late-stage Parkinsons disease are more susceptible to pneumonia, sepsis, pyelonephritis and decubitus ulcers. Late-stage Parkinsons also leads to Parkinsons disease dementia in 50% of cases. For all of these reasons, many late-stage Parkinsons patients are cared for by loved ones or in a hospice.
How Is Parkinson’s Disease Treated
If a doctor thinks a person has Parkinson’s disease, there’s reason for hope. Medicine can be used to eliminate or improve the symptoms, like the body tremors. And some experts think that a cure may be found soon.
For now, a medicine called levodopa is often given to people who have Parkinson’s disease. Called “L-dopa,” this medicine increases the amount of dopamine in the body and has been shown to improve a person’s ability to walk and move around. Other drugs also help decrease and manage the symptoms by affecting dopamine levels. In some cases, surgery may be needed to treat it. The person would get anesthesia, a special kind of medicine to prevent pain during the operation.
Also Check: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
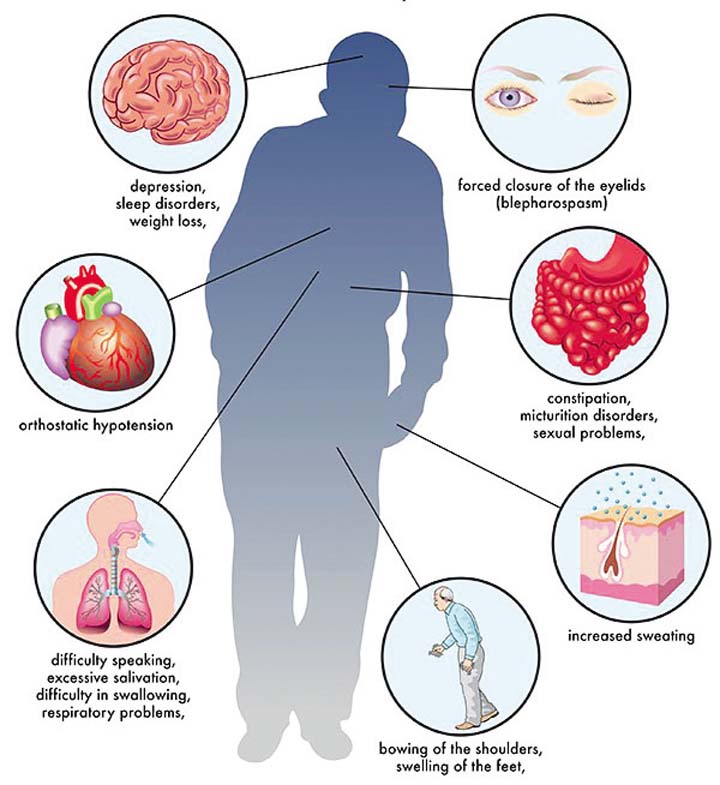
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
Don’t Miss: Parkinsons Genetic Link
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Tips For Starting Lifestyle Changes
How do you live with Parkinson’s disease? The answer is different for everyone. Adjusting to your symptoms and the lifestyle changes you need to make can be difficult. As you start adjusting your routine, keep these tips in mind.
Some people also find it helpful to talk to others who are experiencing similar situations. Look for a Parkinson’s disease support group in your area or join an online community. You can share experiences, hear stories from other people with similar symptoms and encourage one another to adapt to lifestyle changes.
Read Also: What Are Early Warning Signs Of Parkinson’s Disease
What Research Is Being Done
The National Institute of Neurological Disorders and Stroke , a component of the National Institutes of Health, is the primary funder of research on the brain and nervous system. NIH is the leading funder of biomedical research in the world.
PSP is one of the diseases being studied as part of the NINDS Parkinsons Disease Biomarkers Program. This major NINDS initiative is aimed at discovering ways to identify individuals at risk for developing Parkinsons disease and related disorders, and to track the progression of these diseases. NINDS also supports clinical research studies to develop brain imaging that may allow for earlier and more accurate diagnosis of PSP.
Genetic studies of PSP may identify underlying genetic causes. Previous studies have linked regions of chromosomes containing multiple genes, including the gene for the tau protein , with PSP. Researchers hope to identify specific disease-causing mutation and are also studying how genetics and environment interaction may work together to contribute to disease susceptibility.
Animal models of PSP and other tau-related disorders, including fruit fly and zebrafish models, may identify basic disease mechanisms and lead to preclinical testing of potential drugs. Other studies in animal models focus on brain circuits affected by PSP, such as those involved in motor control and sleep, which may also yield insights into disease mechanisms and treatments.
Tips For Living With Parkinsons Disease
The challenges of living with Parkinson’s disease often go misunderstood. Therefore, if you’re living with Parkinson’s disease, it’s important to educate yourself about the condition, so you know what to expect and when to ask for help. Here are some tips to help you live better with Parkinsons disease:
- Stick to your medication schedule write it down or keep a diary if you have to
- Establish a daily routine to keep your medications, mealtimes and sleep cycles on track
- Relieve stress practice yoga, meditation or mindfulness to keep stress at bay
- Get regular exercise to improve your balance, flexibility and mental health
- Maintain a healthy, balanced diet thats high in fiber and low in processed foods
- Follow your bodys signals take a break or rest if you feel low on energy
- Establish a rapport with a specialist and attend regular medical appointments
- Make sure you have a support system whether thats your family, a group of friends or neighbors or a Parkinsons support group
- Dont be afraid to ask for help from your loved ones or carers
- Take up a hobby that takes your mind off your symptoms, such as painting, journaling or gardening
Living with Parkinsons disease comes with many challenges. If you have just been diagnosed with PD or you know someone who has, its important to educate yourself about Parkinsons so you know what to expect. If you have any questions, you can consult your doctor or call the National Parkinsons Foundation helpline at 1-800-4PD-INFO .
Recommended Reading: Cardinal Signs Of Parkinson’s
Living With Parkinsons Disease
Depending on severity, life can look very different for a person coping with Parkinsons Disease. As a loved one, your top priority will be their comfort, peace of mind and safety. Dr. Shprecher offered some advice, regardless of the diseases progression. Besides movement issues Parkinsons Disease can cause a wide variety of symptoms including drooling, constipation, low blood pressure when standing up, voice problems, depression, anxiety, sleep problems, hallucinations and dementia. Therefore, regular visits with a neurologist experienced with Parkinsons are important to make sure the diagnosis is on target, and the symptoms are monitored and addressed. Because changes in your other medications can affect your Parkinsons symptoms, you should remind each member of your healthcare team to send a copy of your clinic note after every appointment.
Dr. Shprecher also added that maintaining a healthy diet and getting regular exercise can help improve quality of life. Physical and speech therapists are welcome additions to any caregiving team.
What Are The Symptoms Of End
Stage four for Parkinsons disease is often called advanced Parkinsons disease because people in this stage experience severe and incapacitating symptoms. This is when medication doesnt help as much and serious disabilities set in.
Theres an increased severity in:
- How you speak a softer voice that trails off.
- Falling and trouble with balance and coordination.
- Freezing a sudden, but temporary inability to move, when you start to walk or change direction.
- Moving without assistance or a wheelchair.
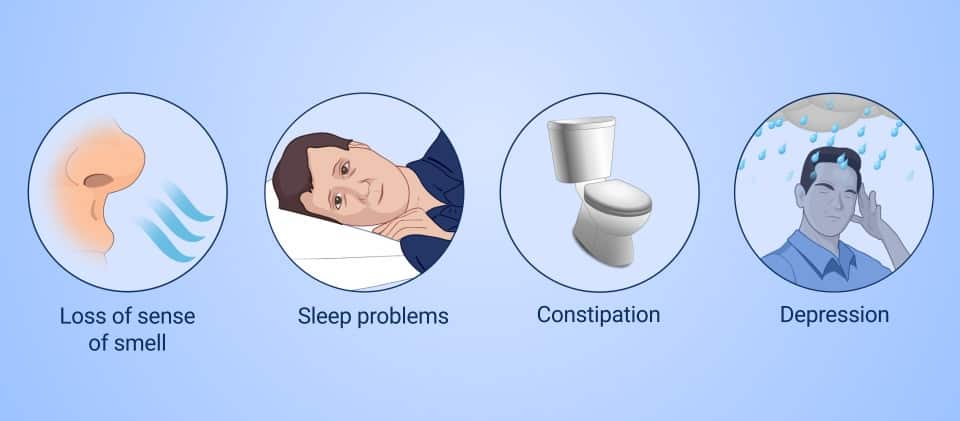
- Other symptoms such as constipation, depression, loss of smell, low blood pressure when going to stand up, pain, and sleep issues.
Many times someone with advanced PD cant live on their own and needs help with daily tasks.
Stage five is the final stage of Parkinsons, and assistance will be needed in all areas of daily life as motor skills are seriously impaired. You may:
- Experience stiffness in your legs. It may make it impossible to walk or stand without help.
- Need a wheelchair at all times or are bedridden.
- Need round-the-clock nursing care for all activities.
- Experience hallucinations and delusions.
As Parkinsons disease progresses into these advanced stages, its symptoms can often become increasingly difficult to manage. Whether you or your loved one with end-stage Parkinsons lives at home, in an assisted living facility or a nursing home, hospice services can optimize your quality of life and that of your family members as well.
Read Also: Parkinson’s Personality Changes
Impact Of Clinical Features On Pdq
Patients with high levels of depression , a mini mental state score of 24 or less ,postural instability on examination , and a history of falls or of gait difficulties had significantly worse PDQ-39 summary index scores than patients without these features . QoL scores of patients with the akinetic rigid subtype of Parkinson’s disease were also worse than those with tremor dominant disease. This difference could not be explained by older age or longer disease duration, as age and disease duration were similar between those with tremor dominant and those with akinetic rigid Parkinson’s disease. The difference of QoL scores between those with and those without a history of hallucinations just failed to reach significance . No difference in PDQ-39 scores was found between men and women and between patients with or without a poor initial or current response to antiparkinsonian medication. A history of dyskinesias or fluctuations, incontinence, orthostatic symptoms, insomnia, pain, speech or swallowing impairment, a family history of Parkinson’s disease, and symptom at onset had no significant impact on QoL scores. There was also no difference between those who were unemployed or had retired early due to the disease and those who were not, those with disease onset before or after the age of 50, and those with current age older than 60 or 70.
Clinical features associated with significantly impaired quality of life scores
How Is Psp Diagnosed
Currently there are no tests or brain imaging techniques to definitively diagnose PSP. An initial diagnosis is based on the persons medical history and a physical and neurological exam. Identifying early gait problems, problems moving the eyes, speech and swallowing abnormalities, as well as ruling out other similar disorders is important. Diagnostic imaging may show shrinkage at the top of the brain stem and look at brain activity in known areas of degeneration.
Don’t Miss: What Color Is The Ribbon For Parkinson’s
Contact Our Information And Referral Helpline
The Parkinson Canada Information and Referral Helpline is a toll-free Canada-wide number for people living with Parkinsons, their caregivers and health care professionals. We provide free and confidential non-medical information and referral services. When you have questions or need assistance, our information and referral staff help connect you with resources and community programs and services that can help you. We provide help by phone or email, Monday to Friday, 9:00 a.m. 5:00 p.m. ET.
Stage Four Of Parkinsons Disease
In stage four, PD has progressed to a severely disabling disease. Patients with stage four PD may be able to walk and stand unassisted, but they are noticeably incapacitated. Many use a walker to help them.
At this stage, the patient is unable to live an independent life and needs assistance with some activities of daily living. The necessity for help with daily living defines this stage. If the patient is still able to live alone, it is still defined as stage three.
Also Check: Can Parkinson’s Change Your Personality
Maintaining & Improving Quality Of Life While Living With Pd
The motor and non-motor symptoms of PD can contribute to changes in many aspects of ability and lifestyle. The goal of Parkinsons treatment is to reduce symptoms and maintain functioning for as long as possible. Diminished capacity to function normally and independently can be challenging or even devastating for those with PD. Individuals with Parkinsons can face a multitude of challenges to their quality of life throughout the disease. Areas that may be impacted include: employment, driving, traveling, dental health, falls, hospitalization, and financial issues.
This page also contains information on prescription assistance, elder law, and late stage PD. Parkinsons disease is different for every individual, but you are not alone. Form your multidisciplinary team early your team could include: your neurologist, primary physician, family caregiver, mental health professional, attorney, pharmacist, social worker, and others. Please call us toll-free at 1-866-903-PARK if you would like to discuss specific resources in your area.
Stage Two Of Parkinsons Disease
Stage two is still considered early disease in PD, and it is characterized by symptoms on both sides of the body or at the midline without impairment to balance. Stage two may develop months or years after stage one.
Symptoms of PD in stage two may include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities, soft voice, monotone voice, fading volume after starting to speak loudly, slurring speech, stiffness or rigidity of the muscles in the trunk that may result in neck or back pain, stooped posture, and general slowness in all activities of daily living. However, at this stage the individual is still able to perform tasks of daily living.
Diagnosis may be easy at this stage if the patient has a tremor however, if stage one was missed and the only symptoms of stage two are slowness or lack of spontaneous movement, PD could be misinterpreted as only advancing age.
You May Like: Difference Between Parkinson’s Disease And Parkinsonism
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
