What Is Needed For A Parkinsons Disease Dementia Diagnosis
There is no definitive medical test that confirms cognitive decline or dementia in Parkinsons disease. The most accurate way to measure cognitive decline is through neuropsychological testing.
- The testing involves answering questions and performing tasks that have been carefully designed for this purpose. It is carried out by a specialist in this kind of testing.
- Neuropsychological testing addresses the individuals appearance, mood, anxiety level, and experience of delusions or hallucinations.
- It assesses cognitive abilities such as memory, attention, orientation to time and place, use of language, and abilities to carry out various tasks and follow instructions.
- Reasoning, abstract thinking, and problem solving are tested.
- Neuropsychological testing gives a more accurate diagnosis of the problems and thus can help in treatment planning.
- The tests are repeated periodically to see how well treatment is working and check for new problems.
Imaging studies: Generally, brain scans such as CT scan and MRI are of little use in diagnosing dementia in people with Parkinsons disease. Positron emission tomographic scan may help distinguish dementia from depression and similar conditions in Parkinsons disease.
Rem Sleep Behavior Disorder
LBD: People with LBD sometimes experience REM sleep behavior disorder, a dysfunction where they physically act out the situations in their dreams. Some research suggests that REM sleep behavior disorder can be one of the earlier predictors of LBD.
Alzheimers:REM sleep behavior disorder is not typically present in Alzheimers, although other types of sleep disturbances may occur.
Coping With Dietary Problems
Many people with Parkinsons experience various eating and dietary problems, such as constipation, chewing and swallowing difficulties, and upset stomach. The following tips can help you minimize the symptoms.
If you suffer from constipation Drink lots of water and eat fiber-rich foods, including beans, brown rice, whole grains, and fruit.
If you have trouble chewing or swallowing food Cut foods into smaller portions to avoid choking and to encourage digestion, and remain upright for 30 minutes after eating.
If youre struggling with fatigueLimit the amount of sugar youre eating. Also avoid alcohol and caffeine, especially before bed, as they can reduce the quality of your sleep.
If you take levodopa Dont eat meat or other protein-rich foods for at least 30-60 minutes after taking levodopa, as protein blocks your bodys ability to absorb the medication.
If your medication gives you an upset stomach Take your medication with a full glass of water and a small non-protein based snack, such as a piece of toast or fruit.
Some Parkinsons disease medications need to be taken promptly at specified times before or after eating, so it can also help to establish a regular routine for meal and medication times.
You May Like: Is Parkinson’s Fatal
The Differences Between Alzheimer’s And Parkinson’s
16 October, 2020
Do you know the differences between Alzheimers and Parkinsons? First of all, we must say that both diseases constitute two of the causes of dementia. Now, lets be a bit more specific. According to data from the WHO , dementia due to Alzheimers disease represents 60-70% of all cases of dementia in the world.
However, its important to keep in mind that theyre very different diseases. Additionally, we must make clear that having either condition doesnt always lead to the development of dementia . In this sense, we know that between 20-60% of people with Parkinsons disease end up developing dementia.
Buter et al. conducted a study that was published in the journal Neurology. It was conducted with 233 patients with Parkinsons disease. The researchers were able to observe that about 60% of them developed Parkinsons dementia in a period of 12 years.
So whats dementia? It refers to the set of symptoms that arise as a consequence of neurological damage or disease. These symptoms involve the loss or weakening of the mental faculties and mainly affect three different areas: cognitive , behavioral , and personality .
Frontotemporal Dementia With Parkinsonism
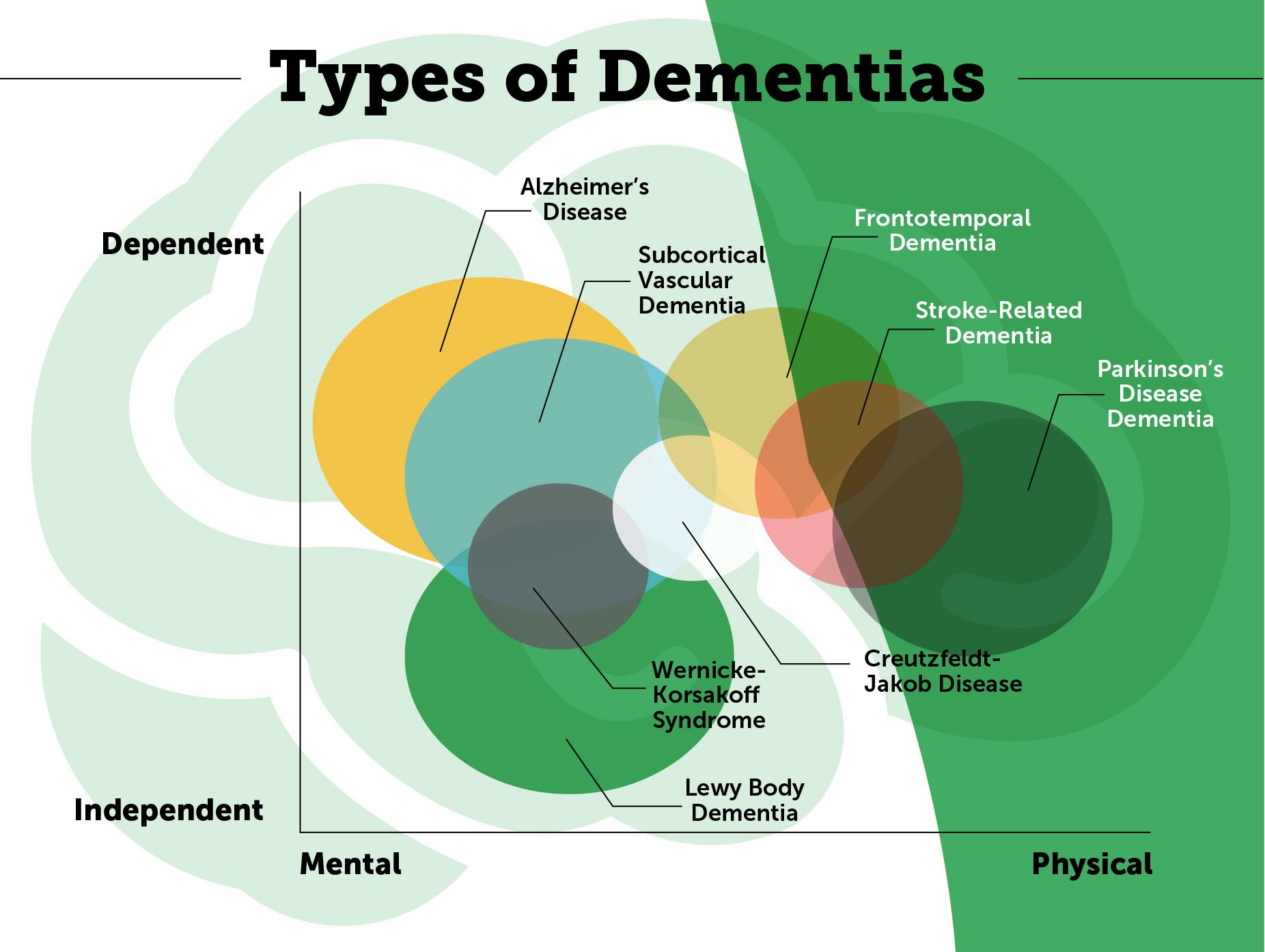
One form of familial FTD, also known as frontotemporal dementia with Parkinsonism-17 , is caused by genetic changes in the gene for tau protein, located on chromosome 17. No other risk factors for this condition are known.
FTDP-17 is rare and accounts for only three per cent of all cases of dementia. Symptoms progressively get worse over time and usually appear between the ages of 40 and 60. The condition affects both thinking and behavioural skills and movements such as rigidity, lack of facial expression and problems with balance .
It can be distressing to be told that you have a genetic disorder or are at risk of having one. Genetic counselling provides the person and their family with information about a genetic disorder and its likely impact on their lives. This can assist a person with FTDP-17 to make informed medical and personal decisions about how to manage their condition and the challenges it presents to their health and wellbeing. Prenatal genetic counselling is also available for parents to help them decide about a pregnancy that may be at risk of FTDP-17.
Also Check: How Does Levodopa Help Parkinson’s
Lewy Bodies: More Than Lbd
LBD is characterized by the presence of Lewy bodies in the nerve cells of the brain, meaning that LBD patients have Lewy bodies in the brain.2 However, Lewy bodies are also common with other conditions, such as Alzheimers and Parkinsons disease. In fact, most people with PD also have Lewy bodies in their brain. However, even if they have Lewy bodies, not all Parkinsons patients will also develop LBD.2
What Is Parkinsons Disease Dementia
Parkinsons disease dementia is a brain disorder that occurs in somebut not allpeople living with Parkinsons disease. The brain cell damage caused by the disease can lead to a loss of memory and other cognitive functions such as problem solving and speed of thinking. These changes in thinking and behavior can impact your daily living, independence, and relationships.
In those who do develop Parkinsons disease dementia, there is at least one yearand usually 10 to 15 yearsbetween the Parkinsons diagnosis and the onset of dementia. According to estimates by the Alzheimers Association, 50% or more of people with Parkinsons disease eventually experience dementia, although there are a number of risk factors that impact the likelihood of developing symptoms:
- Parkinsons patients who experience hallucinations, excessive daytime sleepiness, and more severe motor control problems are at higher risk for dementia.
- Dementia is more common in people who are older at onset of Parkinsons.
- Dementia is a bigger risk factor in non-tremor predominant Parkinsons.
- Overwhelming stress, cardiovascular disease, and adverse reactions to the Parkinsons disease drug levodopa can also indicate an increased risk for developing dementia.
- Dementia is relatively rare in people who develop Parkinsons before age 50, no matter how long they have had the disease.
Read Also: Does David Brooks Parkinson’s
Comparing Trajectories And Conceptualization Of Palliative Care For Dementia And Pd
The two disease trajectories may overlap partly as dementia is a frequent manifestation of PD. Mild cognitive impairment may already present upon diagnosis of PD . Importantly, it is independently associated with lower quality of life . Across studies, typically about a quarter of patients with PD have dementia , but ultimately, most develop dementia .
A clear conceptualization of palliative care in chronic-progressive diseases is important for the development of healthcare systems that facilitate the integration of a palliative approach . Therefore, in this article we compare the disease trajectories of dementia and PD in as far as relevant for the conceptualizations of palliative care. We do not include atypical Parkinsonian disorders such as multiple system atrophy because these warrant a special approach with earlier palliative care . We first provide background on where we are by describing how palliative care for dementia and PD developed.
What Is Parkinson’s Disease
Parkinson’s disease was named by James Parkinson nearly 100 years before Dr. Alois Alzheimer described the type of dementia called Alzheimer’s disease .
This disease was colloquially referred to as the “shaking palsy” by James Parkinson. It is diagnosed in people who exhibit at least two of these three symptoms: slowed movements , muscle rigidity, and tremor even at rest.
Other recognized associated signs of Parkinson’s Disease include having an expressionless face, difficulty swallowing, cramped handwriting, trouble getting out of a chair, and a shuffling gait. Many of the symptoms are a result of nerve cell death in those that produce dopamine.
In addition to movement-related symptoms, Parkinson’s symptoms may be non-motor. Examples of non-motor symptoms include indifference, depression, constipation, sleep disorders, loss of the ability to smell, and cognitive impairment.
Also Check: Parkinson’s Warning Signs
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
How Can We Manage Hallucinations
It may not be necessary to treat all hallucinations of a person with PDD. Hallucinations are often harmless, and it is okay to allow them to happen, as long as they are not disruptive or upsetting to the person or surroundings. Sometimes, recognizing the hallucination and then switching the topic might be an efficient way of handling frustrations that occur because of a hallucination. If hallucinations need medical treatment, your provider may be able to discuss and suggest some options. However, many of the medications used to treat hallucinations may make movement symptoms worse.
You May Like: Is Parkinson’s Disease Fatal
How Parkinsons And Alzheimers Affect The Body And Brain Differently
Alzheimers and Parkinsons are both neurological illnesses. Both diseases are caused by damaged brain cells. Both conditions can involve dementia, as well as depression, anxiety, and sleep disturbances. Both conditions can lead to psychotic symptoms such as delusions and hallucinations.
While Alzheimers and Parkinsons share certain causes and effects, the two diseases are different. They impact the brain and progress in different ways. Both disorders affect people differently, manifest themselves differently, and progress at different rates.
I had a father with Parkinsons and a mother with dementia. My experience was that the Parkinsons progressed at a slower rate and was more motor-related than mental.
My father experienced tremors, as well as changes in his walking and facial expressions. But his cognitive ability was relatively intact up to the very last stages of the disease. My mothers dementia made her feeble and uncertain on her feet, but she remained active and mobile, even as her cognitive ability declined.
Symptoms Of Parkinsons Disease
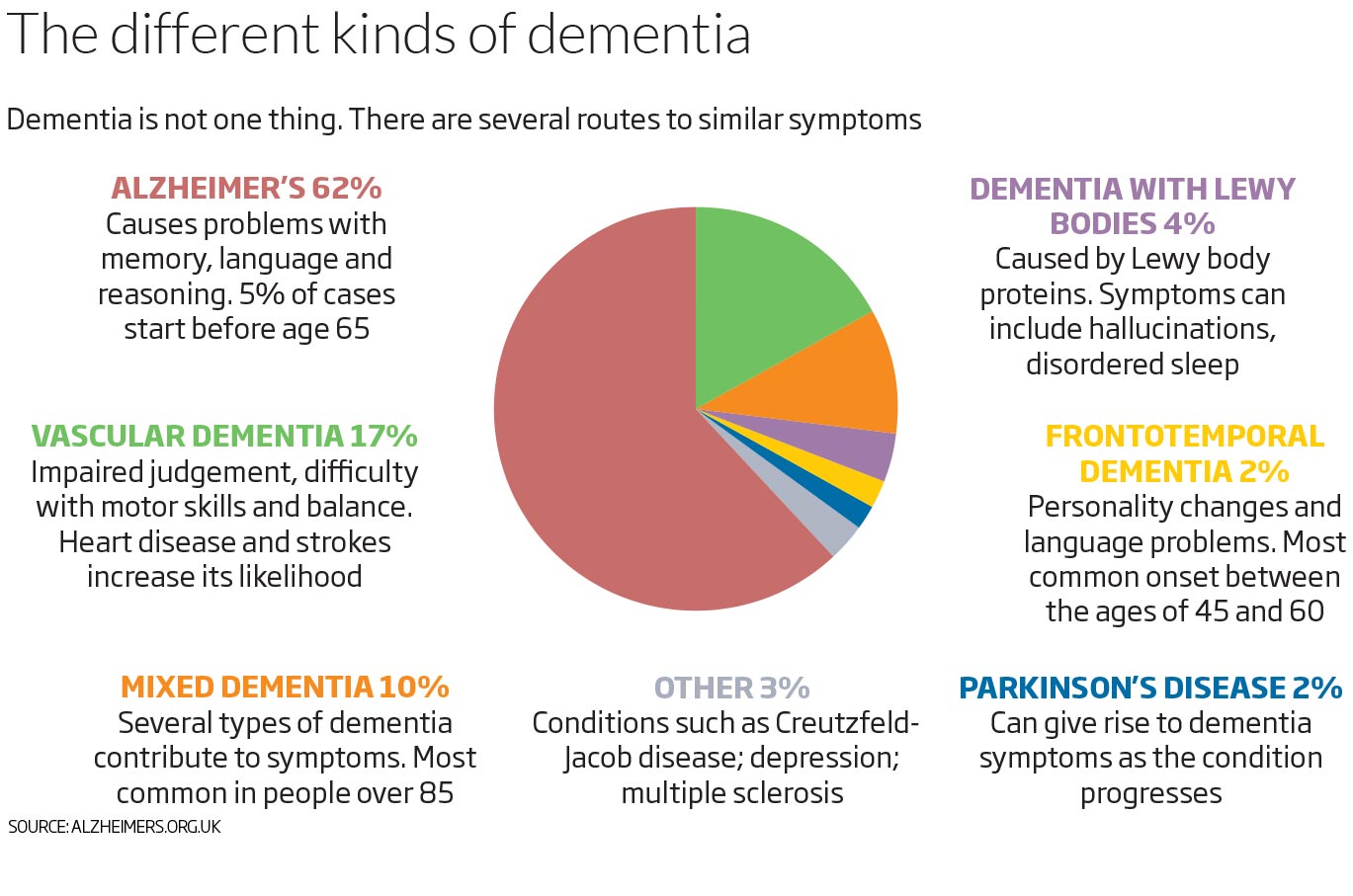
- Apathy
- Feeling, seeing, smelling, hearing and tasting things that arent there
- Hallucinations and delusions
Parkinsons disease is usually expressed through the following five stages:
- Stage one Mild symptoms dont interfere with daily tasks, tremors occur on one side of the body, and posture, gait and facial expression changes may happen.
- Stage two Symptoms worsen, tremors and stiffness affect the entire body and walking and standing are more difficult. At this stage, people may have some trouble performing daily activities.
- Stage three Trouble moving quickly, and balance issues can make it hard to eat or get dresses. Patients may be more likely to fall.
- Stage four Patients may need a walker to move around. Most people are unable to live alone at this stage because they need help with daily activities.
- Stage five It may be impossible to stand or walk. A wheelchair may help with mobility. A caregiver should be present at all times during this stage.
Don’t Miss: Late Onset Parkinson’s Disease
Psychotic Symptoms And Others
In addition to the symptoms we already mentioned, other symptoms may appear in both diseases. For example, in Alzheimers disease, delirium appears occasionally, while it rarely ever does in Parkinsons. Its vital to remember that delirium is an organic disorder that mainly affects consciousness and attention.
Regarding psychotic symptoms, visual hallucinations can appear in both diseases, more or less in the same proportion. Delusions may also arise. They occur often in Alzheimers and occasionally in Parkinsons.
Identification Of Common Molecular Mechanisms
Common molecular mechanisms between AD and PD were identified with the help of a systematic literature mining approach with post-hoc manual curation. More specifically, the text mining engine SCAIView was used to construct cause-effect relationships between molecules, pathways, biological processes and imaging features in both, AD and PD, see Domingo-Fernandez et al. and Kodamullil et al. for details, for details. After manual curation, two computable disease maps, one for AD and one PD were created. Finally, we have also made them interactively usable via a dedicated web application .
Calculation of the intersection of cause-effect relationships described in the AD and PD disease maps resulted into 27 genes grouped into 15 cause-effect relationship sub-graphs, called mechanisms from now on . While some of these mechanisms describe only posttranslational modifications of a single protein, others reflect more complex proteinprotein interactions and signaling cascades . Key proteins described in both diseases include e.g. APOE, TAU, SNCA and TOMM40. These proteins are involved into several known disease relevant processes that we have made computationally accessible via our earlier developed NeuroMMSig database.
We mapped 148 genetic variants measured in ADNI1, ADNI2/GO as well as PPMI to the 27 common AD/PD disease genes via a combination of two strategies: a) proximity and b) eQTL mapping, see details in Supplements on page 2.
You May Like: Does John Lithgow Have Parkinson’s Disease
Number Of People Affected
Parkinsons disease is thought to affect about 2 percent of Americans over 65. Of those, about 50 to 80 percent will go on to develop Parkinsons-related dementia.1 The Parkinsons Foundation estimates that nearly 1 million Americans will be living with Parkinsons by 2020. The disease affects 1.5 times more men than women.7
Approximately 5.8 million Americans are currently living with Alzheimers disease. That number is expected to increase to 14 million by 2050.8 There is little difference between numbers of men and women who develop Alzheimers, but there are more women with the disease, because women tend to live longer than men.3
The Effects Of Alzheimers On The Brain
Damage to the brain begins years before symptoms appear. Abnormal protein deposits form plaques and tangles in the brain of someone with Alzheimers disease. Connections between cells are lost, and they begin to die. In advanced cases, the brain shows significant shrinkage.
Its impossible to diagnose Alzheimers with complete accuracy while a person is alive. The diagnosis can only be confirmed when the brain is examined under a microscope during an autopsy. However, specialists are able to make the correct diagnosis up to
- behavioral changes
- difficulty speaking, swallowing, or walking in advanced stages of the disease
Some types of dementia will share some of these symptoms, but they include or exclude other symptoms that can help make a differential diagnosis. Lewy body dementia , for example, has many of the same later symptoms as Alzheimers. However, people with LBD but are more likely to experience initial symptoms such as visual hallucinations, difficulties with balance, and sleep disturbances.
People with dementia due to Parkinsons or Huntingtons disease are more likely to experience involuntary movement in the early stages of the disease.
Treatment for dementia will depend on the exact cause and type of dementia, but many treatments for dementia and Alzheimers will overlap.
Recommended Reading: Parkinson’s And Shortness Of Breath
Tip : Make It A Priority To Be Socially Engaged
The more socially active you are, the more you connect face-to-face with others, the stronger your memory and cognition is likely to be. You dont need to be a social butterfly or the life of the party, but you do need to regularly connect with people who care about you.
Connecting with others is the most effective means of relieving stress which left unchecked can exacerbate symptoms of Parkinsons disease. Staying socially engaged also stimulates immune function that may slow the progress of disease. While many of us become more isolated as we get older, its never too late to meet others and develop new friendships.
Tips for meeting new people
- Volunteer
Hotlines and support
In the U.S.: Call the Helpline at 1-800-473-4636 or visit Parkinsons Foundation for resources and support. For Parkinsons Disease Dementia, call the Alzheimers Association helpline at 1-800-272-3900.
UK: Call the helpline at 0808 800 0303 or visit Parkinsons UK to find support
Australia: Call the info line at 1800 644 189 or visit Parkinsons Australia for links to state organizations that provide support and services.
Canada: Call 1 800 565-3000 for information or referrals or visit Parkinson Society of Canada for regional resources and support.
Recommended Reading: What Color Ribbon Is Alzheimers
What Causes Lewy Body Dementia
The causes of LBD are not yet well understood, but research is ongoing in this area. There are probably multiple factors involved, including genetic and environmental risk factors that combine with natural aging processes to make someone susceptible to LBD.
For more information, visit www.lbda.org.
Modified with permission from the Lewy Body Dementia Association
To learn more about motor symptoms related to Parkinsons, visit here.
To learn more about non-motor symptoms related to Parkinsons, visit here.
You May Like: Parkinsons Dyskinesia
Lewy Body Dementia: A Common Yet Underdiagnosed Dementia
While its not a household word yet, Lewy body dementia is not a rare disease. It affects an estimated 1.4 million individuals and their families in the United States. Because LBD symptoms can closely resemble other more commonly known disorders like Alzheimers disease and Parkinsons, it is often underdiagnosed or misdiagnosed. In fact, many doctors or other medical professionals still are not familiar with LBD.
Recommended Reading: What Are The Last Stages Of Vascular Dementia
What Happens In Pdd
People with PDD may have trouble focusing, remembering things or making sound judgments. They may develop depression, anxiety or irritability. They may also hallucinate and see people, objects or animals that are not there. Sleep disturbances are common in PDD and can include difficulties with sleep/wake cycle or REM behavior disorder, which involves acting out dreams.
PDD is a disease that changes with time. A person with PDD can live many years with the disease. Research suggests that a person with PDD may live an average of 57 years with the disease, although this can vary from person to person.
You May Like: Does Parkinson’s Run In The Family
