Changes In Sleeping Patterns
As Parkinsons progresses, you can also develop problems with sleep patterns. These may not happen in the early stages, but can be noticeable later. You might wake up often in the middle of the night or sleep more during the day than you do at night.
Another common sleep disturbance for people with Parkinsons is rapid eye movement sleep behavior disorder. This is when you start acting out your dreams in your sleep, such as verbally and physically, which can get uncomfortable if someone is sharing your bed. Dr. Rundle-Gonzalez says many times a bed partner will be the one to notice sleep problems.
REM sleep behavior disorder can also happen in people who dont have Parkinsons. However, if this isnt something youve dealt with before, its likely related to your disease. There are medications your doctor can prescribe to help you sleep comfortably through the night.
Treating Fatigue In Parkinsons Disease
There are currently few treatments available that directly alleviate fatigue, which can make it difficult to treat. However, people with PD who experience fatigue should talk to their doctor as changes in their current medications may help relieve fatigue. Complementary therapies, such as acupuncture or massage, may help improve symptoms of fatigue. In addition, there are several lifestyle approaches that can help manage fatigue, including:
Fourth Type Of Leg Pain Is Radicular Pain
In this case, the pain is caused by compression of nerves in lumbar area which results in weakness, numbness and tingling, and loss of reflexes from buttocks to foot in a distribution of a nerve. It can be acute or chronic, and can be worse with standing and sitting, or better with laying down. Of note: in my experience many patients including myself have these symptoms not because of physically herniated disc but rather by the stretching of a nerve in the canal as it exists due to severe musculoskeletal rigidity and abnormal posturing.
Don’t Miss: Parkinsons Genetics
Potential Ways To Reduce Excessive Daytime Sleepiness
- Assess the underlying cause
- Improve nocturnal sleep through medications, cognitive behavioral therapy, diet, light therapy and more
- Evaluate all medicines being takensome have hypersomnia as a side effectand adjust as needed
- If taking dopaminergic medications, consider dose adjustment
- Watch consumption of alcohol or sleep-inducing foods/ingredients
- Experiment with caffeine
Fatigue In Parkinsons Disease: Report From A Multidisciplinary Symposium

A summary of a symposium in October, 2014, reviewing what is known about the diagnosis and treatment of fatigue, its physiology, and what we might learn from other disorders in which fatigue figures prominently, and concluding with focused recommendations to enhance understanding and treatment of fatigue in Parkinsons disease.
Read Also: Non Motor Symptoms Of Parkinson Disease
Pragmatic Management Of Fatigue In Pd
Treatment approaches focused on fatigue in PD are faced with 2 main limitations: lack of clear insight into its pathophysiology and mechanisms, and probably its multifactorial nature . Therefore, as stated by Kluger and Friedman, contemporary treatment of fatigue in PD is limited to an empirical approach based on plausible hypotheses .
What Makes Pd Hard To Predict
Parkinsonâs comes with two main buckets of possible symptoms. One affects your ability to move and leads to motor issues like tremors and rigid muscles. The other bucket has non-motor symptoms, like pain, loss of smell, and dementia.
You may not get all the symptoms. And you canât predict how bad theyâll be, or how fast theyâll get worse. One person may have slight tremors but severe dementia. Another might have major tremors but no issues with thinking or memory. And someone else may have severe symptoms all around.
On top of that, the drugs that treat Parkinsonâs work better for some people than others. All that adds up to a disease thatâs very hard to predict.
Recommended Reading: Sam Waterston Tremor
Physiology And Biomarkers For Fatigue In Pd
The physiology underlying fatigue symptoms in PD is unknown, whereas much is known about the mechanisms of motor fatigability. The only published study of physiological differences between fatigued and nonfatigued PD patients found no measurable differences in oxygen utilization during exercise, but some studies have suggested that exercising improves fatigue.,,, Whether fatigue fluctuates with motor fluctuations was looked at in one study. Subjects were assessed during their off, whereas all other studies used the subjects experience over a preceding time interval of weeks. Eighty-eight percent of their subjects were fatigued, and fatigue increased with motor ”off.” Too few subjects were nonfatigued to determine how often fatigue occurred only during motor ”off.” The physiological implications are unclear, as many other nonmotor symptoms also increased during the ”off” period.
The Relationship Between Parkinsons Disease And Sleep
Its unclear whether poor sleep causes parkinsonian symptoms to worsen or whether worsening parkinsonian symptoms cause poor sleep. In many cases its likely a case of bidirectionality, with each one exacerbating the other.
Fragmented sleep and sleep deprivation appear to leave the brain more vulnerable to oxidative stress, which has been tied to the development of Parkinsons disease. Parkinsons disease is not usually diagnosed until individuals have developed sufficient motor symptoms, by which time a significant portion of brain cells have already been damaged. If poor sleep quality or having sleep disorders foreshadows the development of parkinsonian symptoms, these could be useful in early diagnosis of the disease.
More research is needed to clarify the multifaceted relationship between Parkinsons disease and sleep. A better understanding of this connection may offer medical experts the unique opportunity to screen at-risk individuals and perhaps delay the onset of the disease.
Also Check: Parkinson Disease Produces Dementia As Well As:
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
Whats The Relationship Between Parkinsons And Sleep
Parkinsons disease and sleep are connected in complex ways that not even scientists completely understand quite yet.
Sometimes, Parkinsons disease directly causes sleep problems. According to one study, sleep-related symptoms may be one of the earliest signs of Parkinsons disease. These signs may include things like thrashing while youre asleep.
Other factors can also play a role. One thing is clear: For many people with Parkinsons disease, a restful nights sleep can be hard to find.
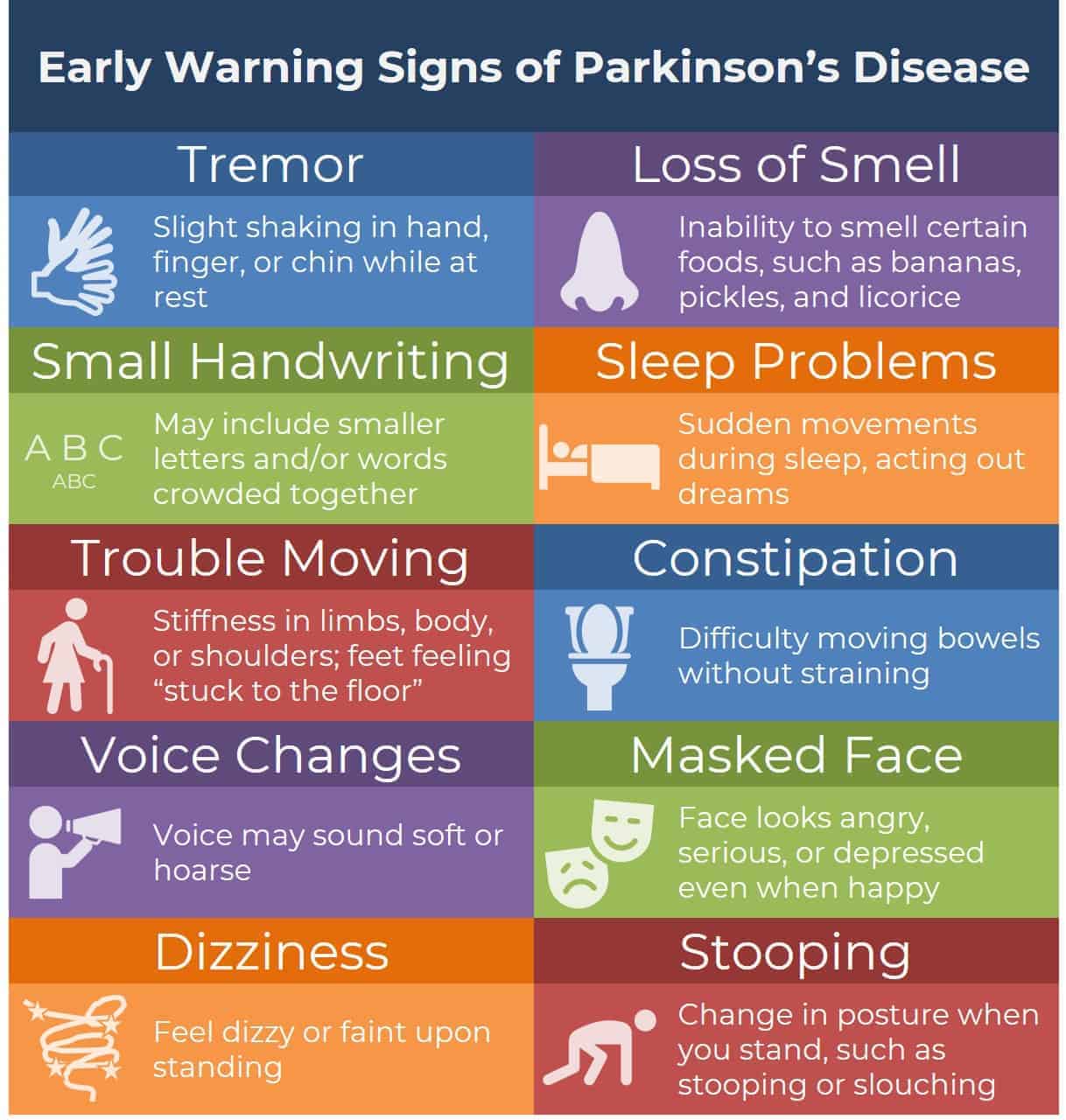
Also Check: What Are Early Warning Signs Of Parkinson’s Disease
Medication Not Working The Way It Used To
In the early stages, taking medicine works well to get rid of symptoms. But as Parkinsons progresses, your medication works for shorter periods of time, and symptoms return more easily. Your doctor will need to change your prescription.
Dr. Valerie Rundle-Gonzalez, a Texas-based neurologist, says to pay attention to how long your medicine takes to kick in and when it stops working. She says you should feel like symptoms significantly improve or are almost gone while on medication.
When To Seek Hospice Care
When you or your loved one have a life expectancy of six months or less, you become eligible for hospice care a type of comfort care provided at the end of life for someone living with end-stage Parkinsons disease. Hospice provides extra support so your loved one can live as comfortably as possible.
If you have experienced a significant decline in your ability to move, speak, or participate in activities of daily living without caregiver assistance, its time to speak with a hospice professional.
Read more: What is hospice care?
Some of the things that determine whether your loved one with end-stage Parkinsons is eligible for hospice include: difficulty breathing, bed bound, unintelligible speech, inability to eat or drink sufficiently, and/or complications including pneumonia or sepsis.
If you live in South Jersey, our nurse care coordinator can answer your questions and decide if your loved one is ready for hospice care. Call us 24/7 at 229-8183.
You May Like: Late Onset Parkinson’s Disease
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinsons disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable reducing symptoms during on periods and no longer controlling symptoms during off periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they cant. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
You May Like: Parkinson’s Disease Awareness Color
Parkinsons Sleep Problems: Diagnosis And Treatment
Parkinsons disease is chronic and progressive, meaning it tends to get worse over time. However, there are treatment options that can help manage symptoms and allow patients to get more restful sleep.
The simplest way to start sleeping better with Parkinsons disease is by adopting healthy sleep habits. Sleep hygiene tips for Parkinsons disease sufferers include:
- Sticking to regular bedtimes
- Following a consistent bedtime routine with soothing activities such as listening to music or reading a calming book
- Getting regular exercise, preferably early in the day
- Getting adequate exposure to light, whether outdoors or through light therapy
- Avoiding long naps and naps late in the day
- Creating a cool, dark, and comfortable sleeping environment
- Restricting bedtime activities to sex and sleep only
- Turning off screens an hour before bedtime
- Reducing liquid intake before bedtime
- Avoiding caffeine, alcohol, and tobacco
- Eating a healthy diet and avoiding large meals at night
Light therapy, exercise, and deep brain stimulation have been successfully used to improve overall sleep quality and to treat specific conditions, such as REM sleep behavior disorder, in patients with Parkinsons disease. Cognitive behavioral therapy for insomnia has proven effective at reducing insomnia in healthy adults, although further research is needed on the effects of CBT in patients with Parkinsons disease.
- Was this article helpful?
Cognitive And Psychiatric Symptoms
- depression and anxiety
- mild cognitive impairment slight memory problems and problems with activities that require planning and organisation
- dementia a group of symptoms, including more severe memory problems, personality changes, seeing things that are not there and believing things that are not true
Read Also: Rso For Parkinson’s
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
What Are The Complications Of Parkinson Disease
Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may arise later. As the disease gets worse with time, many people develop dementia. This can cause profound memory loss and makes it hard to maintain relationships.
Parkinson disease dementia can cause problems with:
- Speaking and communicating with others
- Problem solving
- Forgetfulness
- Paying attention
If you have Parkinson disease and dementia, in time, you likely won’t be able to live by yourself. Dementia affects your ability to care of yourself, even if you can still physically do daily tasks.
Experts don’t understand how or why dementia often occurs with Parkinson disease. Its clear, though, that dementia and problems with cognitive function are linked to changes in the brain that cause problems with movement. As with Parkinson disease, dementia occurs when nerve cells degenerate, leading to chemical changes in the brain. Parkinson disease dementia may be treated with medicines also used to treat Alzheimer’s disease, another type of dementia.
Recommended Reading: Signs Of Parkinson’s In Young Adults
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesn’t go away and continues to get worse over time.
How Is Parkinson Disease Treated

Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
Also Check: What Are Early Warning Signs Of Parkinson’s Disease
How Can I Help Myself
The general rule is to keep as mentally and physically active as possible. The following suggestions may be helpful:
Daily activities:
- Plan your most vigorous activities around when your medication is most effective. You may find keeping a diary to track your symptoms and medication helps with timing when you are likely to be more mobile and energetic.
- Learn how to pace yourself, taking regular short rests and periods in which to relax throughout the day.
- If tasks are complicated or likely to take time, break them down into smaller stages so that you can rest between each stage. Share tasks if you live with someone and make use of labour saving devices such as a dishwasher or microwave.
- Recognise your limitations, identify the priorities of the day and get to know your energy reserves.
- Plan your major activities in advance and ensure that you have time for recovery afterwards. For instance, if you have a big social function such as a wedding, rest more in the days leading up to the event and also plan to have a few restful days afterwards.
Work:
- if you work, talk with your employer to see if you can take regular short breaks, even if its only to make a drink or talk with colleagues
Diet and exercise:
Sleep and rest:
Content last reviewed: May 2018
General wellbeing:
What Are The Symptoms Of End
Stage four for Parkinsons disease is often called advanced Parkinsons disease because people in this stage experience severe and incapacitating symptoms. This is when medication doesnt help as much and serious disabilities set in.
Theres an increased severity in:
- How you speak a softer voice that trails off.
- Falling and trouble with balance and coordination.
- Freezing a sudden, but temporary inability to move, when you start to walk or change direction.
- Moving without assistance or a wheelchair.
- Other symptoms such as constipation, depression, loss of smell, low blood pressure when going to stand up, pain, and sleep issues.
Many times someone with advanced PD cant live on their own and needs help with daily tasks.
Stage five is the final stage of Parkinsons, and assistance will be needed in all areas of daily life as motor skills are seriously impaired. You may:
- Experience stiffness in your legs. It may make it impossible to walk or stand without help.
- Need a wheelchair at all times or are bedridden.
- Need round-the-clock nursing care for all activities.
- Experience hallucinations and delusions.
As Parkinsons disease progresses into these advanced stages, its symptoms can often become increasingly difficult to manage. Whether you or your loved one with end-stage Parkinsons lives at home, in an assisted living facility or a nursing home, hospice services can optimize your quality of life and that of your family members as well.
Read Also: What Color Represents Parkinson’s Disease
