What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
What Is The Prognosis For Parkinsons Disease
The rate at which Parkinsons progresses varies from patient to patient. Some patients experience its changes over 20 years or more. While others find the disease advances quicker.
Parkinsons is not a fatal disease. However, secondary complications from symptoms may increase falls, blood clots or pneumonia, which can be life-threatening. These are more common in later stages of Parkinsons.
In general, the average life expectancy of Parkinsons patients is similar to people without the disease.
What Doctors Look For When Diagnosing Parkinsons
Certain physical signs and symptoms noticed by the patient or his or her loved ones are usually what prompt a person to see the doctor. These are the symptoms most often noticed by patients or their families:
-
Shaking or tremor: Called resting tremor, a trembling of a hand or foot that happens when the patient is at rest and typically stops when he or she is active or moving
-
Bradykinesia: Slowness of movement in the limbs, face, walking or overall body
-
Rigidity: Stiffness in the arms, legs or trunk
-
Posture instability: Trouble with balance and possible falls
Once the patient is at the doctors office, the physician:
-
Takes a medical history and does a physical examination.
-
Asks about current and past medications. Some medications may cause symptoms that mimic Parkinsons disease.
-
Performs a neurological examination, testing agility, muscle tone, gait and balance.
What To Look For In A Parkinsons Disease Neurologist
Here is a checklist of basic questions for your prospective neurologist:
- How long have you worked in the field? How many Parkinsons patients do you see a year?
- Do you have special training in movement disorders? Are you board-certified in neurology?
- Who do I see when you are not available?
- What hospital do you use for treating patients?
Its important to understand that the online rating systems for doctors are not very accurate. Or they are, in some ways, and it is not the information you are looking for. For example, many of these ratings rank a doctor high if he is always on time and never backed up. If you think about the clinic setting and the inability to really control what happens in a typical day, and the doctor who is always time may be the doctor who never has that extra minute to give you when you need it. These ratings also often include how easy it is to get an appointment.
Of course, the doctor who is exceptional that everyone wants to see ranks poor on this measure, and the doctor who doesnt have a strong following ranks high. If you do look at these rankings, make sure to read the comments, and realize that one bad comment could simply represent one patient having a bad day after being given a diagnosis he didnt want.
What Parkinsons Diagnosis Criteria Do Doctors Use
Other Challenges Of Diagnosing Parkinsons Disease
Related: Heres whats important to remember if you were just diagnosed with Parkinsons disease.
What Causes Parkinsons Disease

Parkinsons disease occurs when nerve cells in an area of the brain called the substantia nigra become impaired or die. These cells normally produce dopamine, a chemical that helps the cells of the brain communicate . When these nerve cells become impaired or die, they produce less dopamine. Dopamine is especially important for the operation of another area of the brain called the basal ganglia. This area of the brain is responsible for organizing the brains commands for body movement. The loss of dopamine causes the movement symptoms seen in people with Parkinsons disease.
People with Parkinsons disease also lose another neurotransmitter called norepinephrine. This chemical is needed for proper functioning of the sympathetic nervous system. This system controls some of the bodys autonomic functions such as digestion, heart rate, blood pressure and breathing. Loss of norepinephrine causes some of the non-movement-related symptoms of Parkinsons disease.
Scientists arent sure what causes the neurons that produce these neurotransmitter chemicals to die.
Patients With A Previous Diagnosis Of Parkinsons Disease
The diagnosis of probable Parkinsons disease was confirmed in 109 of the 131 patients with this diagnosis , including three in whom atypical features were found but were insufficient to invalidate the diagnosis of Parkinsons disease . Two additional patients were found to have possible Parkinsons disease. However, in 20 of the 131 patients the diagnosis of Parkinsons disease was unequivocally rejected . The alternative diagnoses were non-parkinsonian tremor in four patients , vascular parkinsonism in six , progressive supranuclear palsy in four , and multiple system atrophy in three . Two patients received a diagnosis of idiopathic torsion dystonia, and one of dementia without parkinsonism. When only those patients who had seen a specialist at some point in the past were considered, the diagnosis was changed from Parkinsons disease to a different diagnosis in 11%.
Patients with an initial diagnosis of Parkinsons disease
Patients With A Previous Diagnosis Other Than Parkinsons Disease
Among all patients seen, two were referred for diagnostic purposes without a previous diagnosis, and 69 of 202 patients had a previous diagnosis other than Parkinsons disease . Among these, 56 patients had been given a diagnosis of non-parkinsonian tremor, two of vascular parkinsonism, one of atypical parkinsonism, and 10 had been prescribed an antiparkinsonian drug for parkinsonian features without a specific diagnosis . Thirteen of the 69 patients with different diagnoses and the two patients referred for diagnostic purposes fulfilled strict clinical criteria for Parkinsons disease . In two additional patients who had a previous diagnosis of non-parkinsonian tremor, a diagnosis of possible Parkinsons disease was made . If only patients who had at some point in the past seen a specialist were considered, the diagnosis was changed to probable Parkinsons disease in five and to possible Parkinsons disease in one .
Sensitivity, specificity, and predictive values for the overall sample* and by type of clinician
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
The Importance Of Early Diagnosis
Early detection and diagnosis is important because the treatments for PD are more effective in the early stages of the disease. In addition, physical therapy and exercise, which greatly improve symptoms and delay progression of the disease, are much easier to perform in the early stages.
Current diagnosis is made through the presence of motor symptoms; however, researchers have found that by the time motor symptoms occur, over 60% of all dopamine neurons in the basal ganglia of the brain have been damaged. Non-motor symptoms become apparent in people with PD long before motor symptoms, including sleep disturbances and loss of the sense of smell.3
Active areas of research include looking for markers in the blood, urine, or cerebral spinal fluid that reliably detect PD, called biomarkers. In addition, brain imaging tests that have high sensitivity for detecting PD are also being actively researched.4
Will I Die From This Disease
No! Parkinsons is not a fatal disease. But it does affect your quality of life, and it gets worse over time. As James Beck, vice president for scientific affairs at the Parkinsons Foundation, explains, People who are healthy when diagnosed will generally live about as long as other people in their age cohort. It is not a death sentence. Some of the complications of PD can be serious, however. The CDC rates complications from PD as the 14th leading cause of death in the U.S. Most of the Parkinsons-related deaths occur because of pneumonia, which is more of a risk as people lose their ability to swallow and can inhale food.8 Its important to start treatment early and to get support to keep living a healthy, active lifestyle as long as possible.
Finding The Right Doctor
Managing Parkinsons disease well can be challenging. Finding a doctor whos well-versed in PD and will help guide you on the journey makes it easier.
Its natural to begin by discussing initial symptoms with your family doctor or internist, who may refer you to a general neurologist or one specialized in movement disorders to rule out Parkinsons.
The Parkinsons Foundation recommends people diagnosed with PD seek out a movement disorders specialist one who can become a key player on your healthcare team. For people living far from an academic medical center or a specialist in private practice, we recommend a knowledgeable, nearby general neurologist for most of your care and then traveling a longer distance two to three times each year to see a specialist. Finding a specialist can seem like a daunting task, but it doesnt have to be. The Parkinsons Foundation can guide you step by step through the process of finding one.
Diagnosis Of Parkinson’s Disease
If Parkinson’s disease is suspected, symptoms are reviewed and a physical examination is performed. A neurological exam is also performed to determine how well the nerves are working. There is no definitive diagnostic test for this condition, so diagnosis may include ruling out any other conditions that may cause similar symptoms.
Common Noninvasive Neurological Examinations
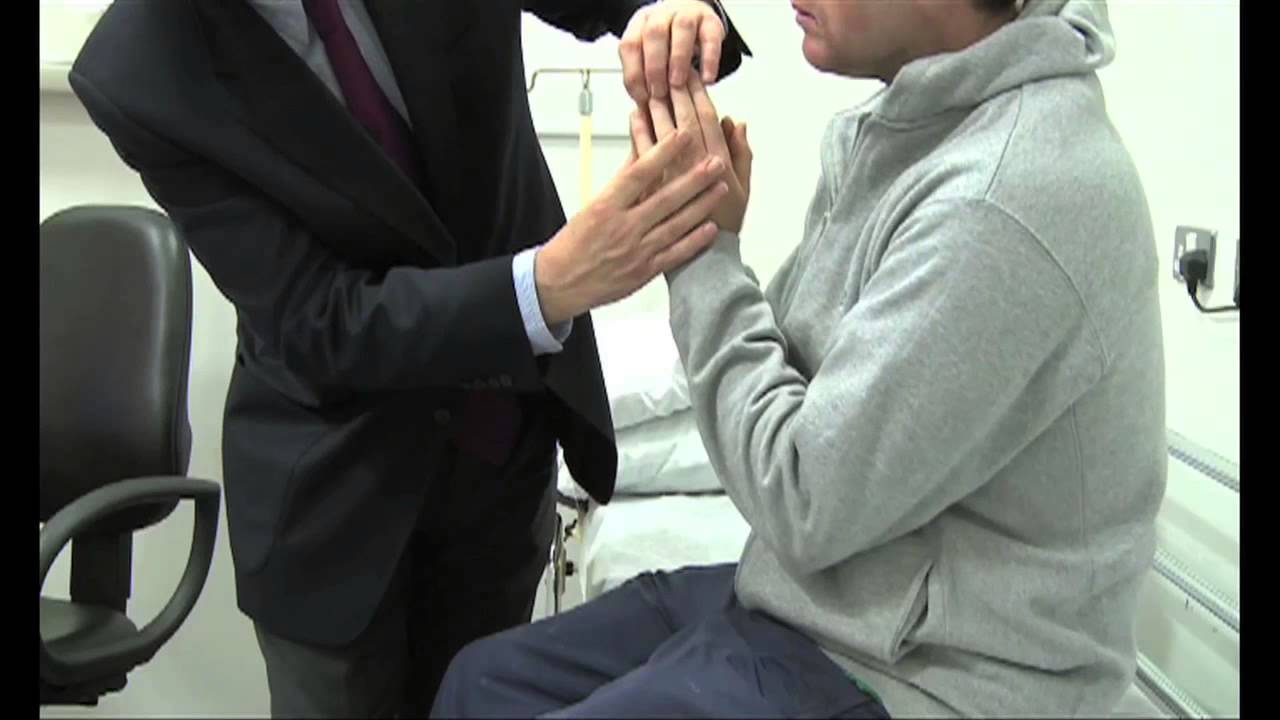
The most common tests that a neurologist may recommend to a patient with symptoms of a neurological disorder are brain scans, neuropsychological tests, and neurological exams.
These tests will help your neurologist to determine if you have a possible serious neurological condition or not.
A brain scan is a visual process where the brains functions such as motor function, speech comprehension, visual spatial awareness, and cognitive processes are evaluated using a computer.
Through this test, a neurologist will be able to identify if the patient is suffering from a possible severe brain abnormality or not.
Neuropsychological tests are conducted on patients wherein they will answer multiple questions about the factors that can cause or contribute to a patients neurological problems such as depression, trauma, repetitive movements, and intelligence.
Another very common procedure that a neurologist may suggest to his or her patient is performing neurological exercises such as motor skill training, manual dexterity, balance, vision, and speech therapy.
What Conditions Do Neurologists Treat
Western Washington Medical Group is not currently offering Neurology care. Please contact your Primary Care Provider or establish care with us today by visiting our Family Practice page or send us a message on our Contact Us page.
Of all the systems in the body, damage to the nervous system can be the most devastating. And while the inner workings of the nervous system are complex and involved, neurologists have devoted their lives to understanding it.
Are There Clinical Trials I Can Take Part In
Yes! The U.S. government National Institutes of Health maintains an ongoing database of all the clinical trials taking place around the country, at ClinicalTrials.gov. You can search by disease, trial status, age group, and location.
The Michael J. Fox Foundation offers an online clinical trial matching tool that helps PD patients connect with studies that need participants.
Centerwatch is an information service for patients and providers that helps match participants with clinical studies.
The Parkinsons Study Group is the largest non-profit cooperative of accredited Parkinsons centers in North America. The organization plans, prioritizes, and conducts clinical trials around the country as well as maintaining a searchable list of past and current trials on its website.
Top Neurologists In Midtown Miami
Our top Neurologists in Midtown Miami include:
Jeffrey Gelblum, MD has successfully treated thousands of patients over a quarter-century, from South Florida, and around the world. He is considered a global thought leader in the neurologic treatment of dementia, seizure disorders, Parkinsons, Familial Amyloid Polyneuropathy, trauma, and chronic pain, and has hosted educational symposia in the U.S. and overseas.
Raul Grosz, MD is Board Certified in neurology. His specialties include migraine headaches, memory loss, seizure disorders, Parkinsons disease, carpal tunnel syndrome, neuropathy, pinched nerve, sciatica, and radiculopathy and treats all conditions of the nervous system.
Neurologists Can Provide Most Informed Referral To A Surgeon As Last Resort
- Neurologists are very knowledgeable about the human body.
- They are highly trained medical specialists and masters in their field who have obtained certifications from either the American Board of Medical specialties or the American neurologic association.
- Their areas of specialization are brain functioning, neurology, psychology and behavioral health.
- A neurologist is also certified by the state to provide diagnostic and therapeutic services in neurology and brain injury/illness.
- They are also qualified to treat brain injuries. There are many neurologists around the country, but some specialize in treating the following conditions; stroke, traumatic brain injury, Multiple sclerosis, Parkinsons disease and Cerebral palsy.
As you may understand, there are many risks when referring someone for surgery or procedure such as a neurological procedure.
Due to the nature of neurology, not every hospital has one of these highly trained doctors on staff.
Many times neurologists who perform invasive procedures are referred to plastic surgeons due to the complexity of the procedure.
Because of the nature of plastic surgeons, it is imperative that the patient fully understands everything that is involved and that their neurologist is willing to explain everything to them. This allows the plastic surgeon to make the best decision possible and ensure that the patient receives the best outcome possible.
Hip Fractures And Survival
To investigate whether treatment by a neurologist was associated with differences in clinical outcomes among patients with PD, we compared 1-year risk of hip fracture between neurologist-treated and primary care physiciantreated patients with PD. Because race and sex also have been shown to affect baseline hip fracture risk, our logistic regression model for this analysis consisted of hip/pelvic fracture as the main effect variable, with race, sex, socioeconomic deprivation, and modified comorbidity index and age as covariates.
For survival analyses, we extracted vital status information for each patient from 2002 to 2008. Cox proportional hazards models were used to compare survival between neurologist- and primary care physiciantreated patients with PD, controlling for age at diagnosis, race, socioeconomic deprivation score, and modified comorbidity index. The time-to-event variable was from the beginning of the study period to the date of death . The surviving patients were censored at the end of the calendar year 2008.
Find A Parkinsons Expert
Finding a doctor who is an expert in Parkinsons disease can help you get the best possible care. Look for a neurologist, a doctor who works with brain and central nervous system conditions such as Parkinsons. When possible, a movement disorder specialist a neurologist with additional training to treat people with Parkinsons at every stage of the disease can be a key addition to a quality care team.
Neurologists with Parkinsons expertise and movement disorder specialists can often recommend other healthcare professionals who can help treat day-to-day challenges. A holistic, team-based care approach can help you live well with PD.
Where Can I Find Reliable Information On Parkinsons Disease
There are multiple national patient advocacy and research organizations that focus on Parkinsons disease. Some of these include ParkinsonsDisease.net, the Parkinsons Foundation, the American Parkinson Disease Association, and The Michael J. Fox Foundation for Parkinsons Research. The National Institutes of Health and its associated resources are also a reliable source for disease information.
Neurology And Psychiatry: Common Ground And Differences
Essentially both specialties deal with disorders that stem from the same organ of the human body, namely the brain. Distinguishing between what constitutes the subject of each specialty, can be done according to the following:
- Phenomenology of symptoms:Psychiatry focuses on disorders of mood, behavior and thought . The most common neurological symptoms have already been mentioned in the first section of this article.
- Organicity of symptoms:The term organicity implies that symptoms are a direct result of identifiable lesions in the nervous system . As a general rule, Psychiatry is focused primarily on disorders that do not have a clear organic substrate, while Neurology deals with everything that is related to identifiable lesions.
It should be stressed that the above criteria are not absolute. Furthermore, the exact meaning of the term organicity is constantly revised, as diagnostic procedures become more sensitive and new evidence regarding the etiopathogenesis of mental disorders come to light.
In everyday clinical practice, collaboration between neurologists and psychiatrists is common, owing to the fact that many psychiatric disorders present with neurological symptoms and vice versa. In addition, the occurrence of mixed symptomatology is not rare. The following examples illustrate the close relationship between Neurology and Psychiatry:
Search
Preparing For The Initial Visit
- Laboratory or other test results from previous treatment for Parkinsons symptoms.
- Films or CDs of brain imaging.
- Names and contact information for all doctors you see .
- Lists of your movement and non-motor symptoms .
- List of all medications you take and the actual pills, including over-the-counter drugs and supplements .
- Your insurance or Medicare card.
- Perhaps most importantly, bring a family member or friend who can take notes and help ask and answer questions. You will receive a lot of information during this visit. Later, it may help you to talk it over with the person who went with you.
Diagnosis Of Parkinsons Disease
The movement disorder specialists at Mount Sinai are expert in diagnosing and treating Parkinsons disease. There is no one test that diagnoses Parkinsons disease. Instead, we conduct a comprehensive history of symptoms and a detailed neurologic examination. After we confirm the diagnosis, we develop a comprehensive treatment plan, personalized to your needs.
Our neurosychologists and neuropsychiatrists evaluate patients who are being considered for certain medications or treatments , provide support and counseling, and oversee treatments and strategies for dealing with mood, memory, or other challenges.
When A Neurologist Performs Electromyography
- Many people wonder if the neurologist can be used to test and diagnose neck, back, and leg pain.
- In fact, the use of this testing is becoming more commonplace in medicine as more is learned about the relationship between the nervous system.
- Neurons in the brain send signals to and from other neurons in the body and when those signals are disturbed due to disease, neurological disorders or trauma, these symptoms become apparent in various parts of the body.
- Neuromuscular pathways may be affected in the spinal cord, which is why so many people have painful herniated disks, Back pain, and other related conditions. If a neurologist were to perform EMG for back pain, they would be looking for any abnormal changes in the electrical activity of the muscles, which might indicate a neurological issue.
Before testing can begin, it is necessary for the patient to provide some information.
The patient will need to describe which symptoms they are experiencing as well as any past medical history of similar issues. EMG testing can also help to rule out other conditions such as Parkinsons disease or Alzheimers disease.
Many times a patient will experience numbness, tingling or weakness while performing some tasks; these symptoms may point toward neurological problems as well.
I Do My Best To Remain Optimistic And Cling To The Fact That The Parkinsons Diagnosis Is Overturned
Neurologists told me that the three drug components of Stalevo would be out of my system within a few weeks, but my brain only felt clear in February 2016 four months after Id stopped taking it. The huge range of motor and non-motor symptoms persists and other new ones have arrived since my body stopped receiving the added, yet unnecessary, dopamine. I do my best to remain optimistic and cling to the fact that the Parkinsons diagnosis is overturned.
Look out for another article by Joanne in the coming weeks, discussing the issue of misdiagnosis in more depth. Joanne has written about her experiences on her blog here
What Are The Symptoms Of Parkinson’s Disease
The main symptoms of Parkinson’s disease are:
- tremor or shaking, often when resting or tired. It usually begins in one arm or hand
- muscle rigidity or stiffness, which can limit movement and may be painful
- slowing of movement, which may lead to periods of freezing and small shuffling steps
- stooped posture and balance problems
The symptoms of Parkinson’s disease vary from person to person as well as over time. Some people also experience:
- loss of unconscious movements, such as blinking and smiling
- difficulties with handwriting
- drop in blood pressure leading to dizziness
- difficulty swallowing
- sweating
Many of the symptoms of Parkinson’s disease could be caused by other conditions. For example, stooped posture could be caused by osteoporosis. But if you are worried by your symptoms, it is a good idea to see your doctor.
Risk Factors For Parkinsons Disease
- Age people over 60 years old are more likely to develop Parkinsons disease, and the risk increases as people age.
- Gender men are more likely to develop Parkinsons disease than women.
- Family history if you have a family history of Parkinsons disease, you are more likely to develop it yourself.
- Exposure to toxins research has linked herbicides or pesticides to an increased risk of developing Parkinsons disease.
- Race Caucasians are more likely to develop Parkinsons disease.
- Living in a rural location people who live in a rural location are more likely to develop Parkinsons.
Peripheral Neuropathy And Parkinsons Disease
A number of studies have tried to determine if PN is more common among people with PD as opposed to people without PD. PN is a relatively common condition in the general population, which makes it difficult to ascertain whether or not it is even more common among people with PD.
The available studies have varying results and are difficult to compare with each other as they:
- Include different types of populations of people with PD
- Assess peripheral neuropathy differently
- Assess for causes of peripheral neuropathy differently
A recent review looked at all the available data and determined that large fiber neuropathy was present in 16% of patients with PD, about double the prevalence of this condition in the general population. Skin biopsy-proven small fiber neuropathy was present in over 50% of people with PD, although this result was based on a small sample of patients.
