A Cure Means Different Things To Different People But What We Can Be Certain Of Is That We Dont Yet Have One For Parkinsons
Charities these days are all promising their research will lead to a cure, but while humanity has eradicated, or is on the way towards eradicating, some infectious diseases — such as small pox, measles and polio — it is unlikely that we will ever see a day when humans do not get cancer, heart disease or neurological conditions like Parkinson’s.
As A Person Explains Their Off Period It’s More Of A Sad Testimony Because You’re Sharing What You’re Missing In Life
Steven D., Living with Parkinson’s Since 2005
Co-Chair of the PwP Advisory Board & Founder and CEO of the Connecticut Advocates for Parkinson’s
In a 2014 survey conducted by the Michael J. Fox Foundation, 64% of approximately 3,000 people living with Parkinson’s reported that they spent two or more hours per day in OFF periods15
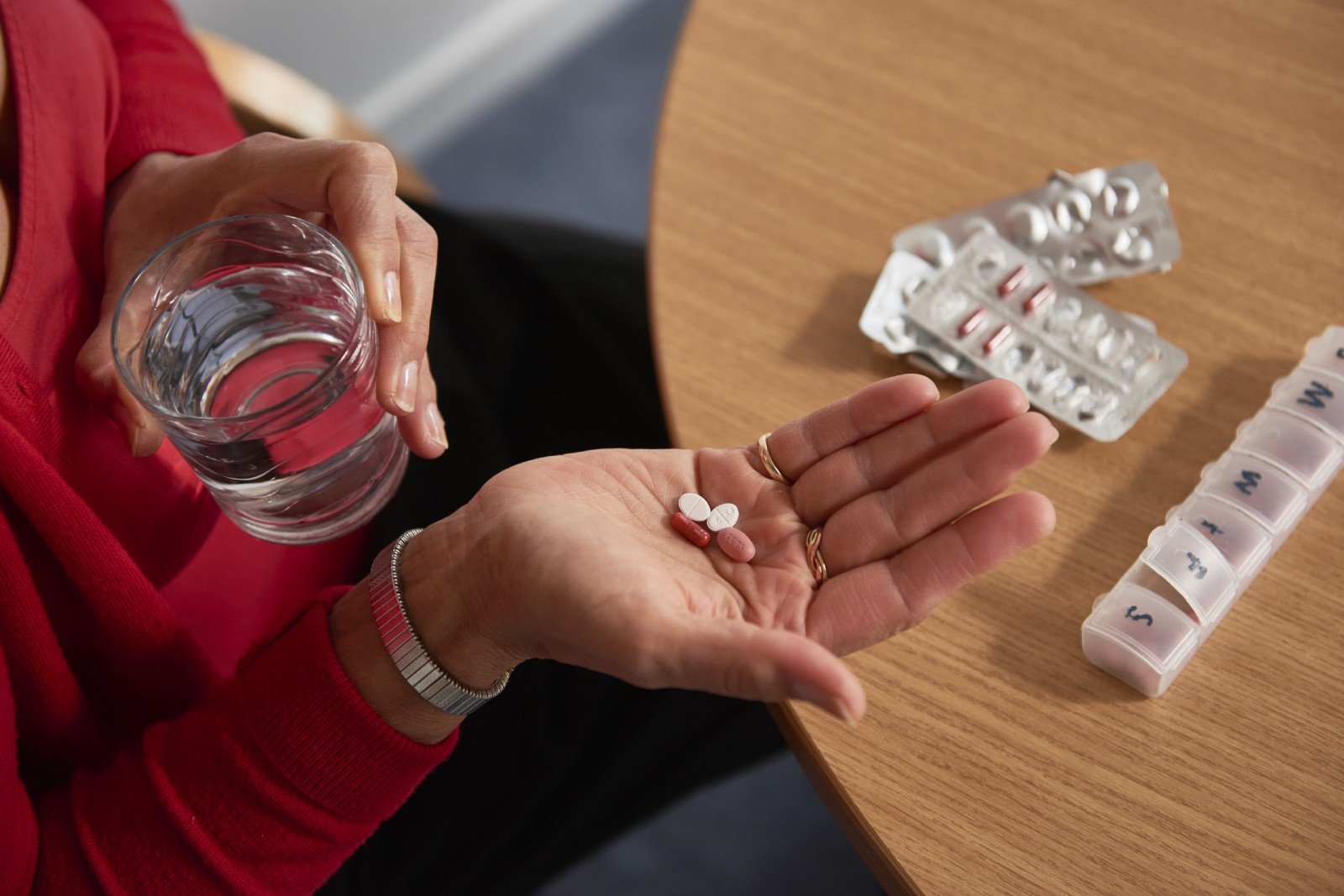
Have You Ever Thought How Challenging Drinking A Glass Of Water Can Be For Someone Suffering From Parkinsons Disease
On World Health Day, you’ll likely read about how healthy habits like exercising or drinking more water, can improve your health. While these are helpful tips and important topics to cover, we decided to take things a step further. What if you couldn’t drink that glass of water by yourself? It can be daunting to consider, but this scenario can become all-too-real for a person suffering from Parkinson’s disease. There are 10 million people in the world suffering from this disorder; which is why, today, we decided to share with you how Parkinson’s Disease can affect mobility and balance, and what can be done when the disorder is detected in its early stages. That is why raising awareness for this degenerative disease is important, and, while there is still much research to be done, we have high hopes that researchers will find a way to reduce the symptoms of Parkinson’s disease, and eventually find a cure. This is becoming more and more urgent, given the fact that life expectancy is rising and the number of individuals with Parkinson’s disease will only increase in the future. But is there another solution in sight?
Request Brochure
Production Of Dopamine Neurons From Stem Cells: Could We Be One Step Closer To The Cure
As the disease progresses, people may experience reduced quality of life, if normal functions such as swallowing, start to be affected. Currently, there is no known cure for Parkinson’s disease. Once Parkinson’s is diagnosed, the symptoms can often be treated with medications and therapies, especially in the early stages. However, the scientific community is making every effort to find a way to cure or at the very least find more effective ways to lessen the symptoms of this physically impairing disease.
As we mentioned before, the disease primarily affects dopamine-producing brain cells or neurons. The good news is, scientists in Sweden have identified some insights and a set of markers that should help control the quality of stem cells engineered for clinical use to treat Parkinson’s disease. As the disease progresses and dopamine-producing brain cells malfunction and die, it leads to lower levels of dopamine, which is a chemical messenger essential for controlling movement. These findings should help fine-tune stem cell engineering to produce pure populations of high-quality dopamine neurons. Then, a pool of progenitor cells can be transplanted into the brains of patients, so they can make new supplies of dopamine cells.
But while this exciting new research is still in the lab, what else can we hope for to delay the symptoms of Parkinson’s and improve the quality of life of those suffering from the disease?
How Can I Support Someone With Parkinson’s At The Advanced Or Palliative Stage

In the advanced stages of Parkinson’s, your patient’s care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the ‘whole person’ to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinson’s may be supported by a number of professionals, including a Parkinson’s nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinson’s also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinson’s should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the person’s wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesn’t want to have in the future – this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
Parkinsons Disease Is A Progressive Neurodegenerative Multisystem Disease1
Parkinson’s disease is a multisystem disorder typically defined by a progressive loss of dopaminergic neurons in the substantia nigra.1,2 By the time of diagnosis, individuals have lost a significant number of dopaminergic neurons—evidence suggests 60-80% of dopaminergic neurons degenerate before clinical features emerge.23 As PD progresses, neurodegeneration continues, with further loss of dopaminergic neurons and dopamine.2 The progression of disease reduces the brain’s ability to store and release dopamine when it is needed.2,3
The characteristic motor symptoms of Parkinson’s disease are bradykinesia, tremor and rigidity, all of which are related to the degeneration of dopaminergic neurons in the substantia nigra. However, these symptoms are only one aspect of this multifaceted and complex disorder. It is now suggested that Parkinson’s related degeneration is widespread in both the central and peripheral nervous systems.1
Evidence is mounting that many non-nigral sites produce a number of clinical signs and symptoms of Parkinson’s disease.1
Off Periods For Me Are Best Defined As Not Knowingwhat Is Going To Happen
Israel R., Living with Parkinson’s Since 2007
Lynn H., Living with Parkinson’s Since 2010
Michael B., Living with Parkinson’s Since 2011
Brenda V., Living with Parkinson’s Since 2012
Steven D., Living with Parkinson’s Since 2005
Gary R., Living with Parkinson’s Since 2008
Steven D., Living with Parkinson’s Since 2005
Israel R., Living with Parkinson’s Since 2007
How Can We Reduce Mobility Constraints In People With Parkinsons Disease
Over the last few decades, neuroscience has been providing us with exciting new findings regarding the effects of physical exercise on neuroplasticity , neuroprotection and slowing of neural degeneration. In fact, it has been proven that physical exercise can improve brain function in people with neurological disorders.
Aerobic exercise, such as treadmill training and walking programs, have been tested on individuals with Parkinson’s Disease and has been shown to improve gait and quality of life in general. However, the type of exercise chosen should take into account a specific program provided by a specialist. The exercise shouldn’t, by any means, put the patient’s physical integrity at risk, especially if the patient is a senior. In order to address complex mobility issues in people with Parkinson’s Disease, a therapist could incorporate tasks such as balance training into the patient’s rehabilitation. These are exercises that challenge sensorimotor control of dynamic balance and gait to improve mobility.
According to a study by Dr. Ergun Y. Uc, of the University of Iowa, the results suggest that
“walking may provide a safe and easily accessible way of improving the symptoms of Parkinson’s disease and quality of life.”
Signs It Might Be Multiple System Atrophy Instead Of Parkinsons Disease
Here are some clues as to whether it is multiple system atrophy or Parkinson’s disease. One of the easier distinctions is between PD and MSA-C .If the patient presents with unsteadiness while walking, uncoordinated arms and legs, bladder disturbance and/or dizziness when standing the diagnosis is more likely to be MSA-C. On the other hand, if a person looks Parkinsonian the distinction can be harder, but there are clues:
- In the earlier stages of MSA-P , which is often when people have just been told they have Parkinson’s disease, some patients will fall often.Frequent falls also occur in Parkinson’s disease, but it typically occurs 10-15 years after diagnosis.
- In patients with MSA the classic Parkinson’s drug L-Dopa may work initially but will stop working very quickly.It can continue working in PD patients for many years.
- Dementia is not associated with MSA however, it does occur in patients with lewy body Parkinson’s disease.
- Early autonomic nervous system symptoms such as low blood pressure when standing and issues with the bladder are often signs of possible MSA in patient’s diagnosed with Parkinson’s.
- Vocal cord issues are less common but very typical in MSA and much less common in PD.Some examples include difficulty getting words out, odd sighs and even falling asleep during a conversation.
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage
Parkinson’s progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinson’s about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinson’s may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more ‘off’ periods – when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinson’s symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinson’s most often die because of an infection or another condition, usually caused by Parkinson’s.
Help Your Patients Uncover The Troublesome Symptoms Of Off Periods9
Both physicians and patients agree: OFF periods can be one of the most difficult aspects of Parkinson’s disease. It’s understood that recognizing the symptoms of OFF periods is challenging because of a variety of reasons, including interpatient symptom variability and reliance on patient reporting.9
People with OFF periods may not discuss their symptoms or communicate the impact of the symptoms to their healthcare provider as they may be unaware that the changes they are experiencing are a result of OFF periods. Because patients may not recognize the more subtle changes they are experiencing as symptoms of OFF periods, enhancing communication around the full spectrum of symptoms is important.9
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Its Not Just One Condition There Are Multiple Types Of Parkinsons

Like cancer, we are starting to understand the importance of subtyping Parkinson’s and developing tailored treatments that will be more successful than a one size fits all approach. Better understanding is coming from large scale studies that follow vast numbers of people with the condition over time. And we are starting to see how the subtypes of Parkinson’s have different symptoms, progression rates and even different responses to medication.
To effectively treat Parkinson’s, we probably need to tackle each of these subtypes differently, providing the right treatments and support to suit the individual and their form of Parkinson’s. And this starts with understanding more about how we classify and identify these different types.
You can read more about research into personalised treatments in our recent blog ‘Precision medicine for Parkinson’s, how close are we?’
How Can Parkinsons Disease Affect Mobility And Sense Of Balance
The neurophysiology of Parkinson’s Disease proves that it affects balance, gait, movement and can actually cause constraints on mobility. But what do we mean by mobility?
Mobility is a person’s ability to move safely in a variety of environments in order to accomplish functional tasks.
Functional tasks like drinking a glass of water or eating can become a problem. And if we think about it, mobility is something we take for granted most of the time. We don’t expect to lose it, and we don’t expect to get a degenerative disease, such as Parkinson’s. Therefore, being able to maintain good mobility is something of utmost importance as we age, and we must take preventive measures to delay mobility impairment as much as possible.
Mobility requires dynamic neural control, a sense of balance, and enough agility to be able to adapt to postural transitions as quickly as possible. What also concerns us today is the several types of mobility deficits caused by the progression of Parkinson’s Disease. We need to understand what preventive exercises and preventative measures can be taken to minimize the risk of falls and injury.
Parkinson’s Disease and fall prevention
While Parkinson’s is not life-threatening, people may experience life-threatening complications, such as choking on food or falling over. We must help our elderly loved ones prevent falls at any cost so that suggested exercise programs can work effectively in combatting the effects of Parkinson’s Disease.
Why It Is Hard To Detect The Progression Of Parkinsons Disease
As we stated above that Parkinson’s disease is not basic, it becomes difficult to detect it in its early stage due to 2 symptoms – it affects motor issues such as the rigid muscles and tremors, and the other is the development of non-motor symptoms such as dementia, pain, and loss of smell.
Although one cannot see that a person suffering from Parkinson’s disease will show all the symptoms, you cannot even tell or predict which symptoms will be present and their severity. For instance, one patient may show severe dementia with slight tremors. Another patient displays a critical condition of tremors but does not have any problem related to memory or thinking. In another case, the patient can show a severe state of all the symptoms. Therefore, it is difficult to predict the progression of the condition.
In addition to this, the medicines that help in treating Parkinson’s disease also make it difficult to predict the results because a few patients show positive results while others do not show any improvement.
So What Is It Is It Parkinsons Disease Or Is It Something Else
The answer is not easy, but many who feel they have more than Parkinson’s may in fact have multiple system atrophy .MSA is a very rare disorder that has similarities and features of Parkinsonism.However, it is so rare that many physicians are unfamiliar with it and so the diagnosis is not considered. As a result, a likely diagnosis of MSA might be delayed by years and even missed all together. What’s more, due to many symptoms that could possibly be attributed to other conditions diagnosing MSA can be challenging, even to the most experienced doctors. This can be very frustrating to those who know it is more than PD.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
Research To Find Msa Biomarkers And An Earlier Msa Diagnosis
An important goal of the Coalition’s MSA Research Program is to fund and encourage the development of biomarkers to distinguish PD from MSA at a much earlier stage.The stakes are high.An accurate biomarker could lead to quicker development of treatments.In fact, a concern in past clinical trials of MSA treatments that failed is that maybe the patients in the trial are too late stage to show effectiveness.Increasing the number of known early stage MSA patients could improve the likelihood of finding treatments and even a cure.
Reasons Your Parkinsons Symptoms May Be Worse After Exercise
You’ve heard all the hype. Every Parkinson’s healthcare professional, researcher and advocate is shouting from the rooftops how wonderful exercise is supposed to be to help you improve your symptoms and slow the progression of the disease.
But you’ve had a different experience.
When you exercise, you feel like your symptoms get worse instead of better.
You’re afraid you’re the only one.
You’re worried that you’re the outlier who can’t reap the benefits of exercise.
Rest assured, it’s not just you.
As a Parkinson’s physical therapist, I regularly talk to people who struggle to get on board with a regular exercise program because the side effects after the fact are frustrating and disruptive.
In this article, I want to walk you through four reasons why your Parkinson’s symptoms may be getting worse after exercise, and how you can adapt your Parkinson’s exercise program to minimize the side effects so you can reap the benefits.
Elements Of A Highly Effective Parkinsons Exercise Program
What Are The Primary Motor Symptoms Of Parkinsons Disease

There are four primary motor symptoms of Parkinson’s disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinson’s.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinson’s disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinson’s disease has a tremor, nor is a tremor proof of Parkinson’s. If you suspect Parkinson’s, see a neurologist or movement disorders specialist.
Tremors
Read more about Parkinson’s tremors
Rigidity
Bradykinesia
mask-like expression of the face
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
How Long Does It Take For Parkinsons Disease To Progress
It is quite common for any individual suffering from Parkinson’s disease to wonder about the unfolding of the condition. If you belong to the group that in search for the answers related to the progression of Parkinson’s disease, then you will try to learn about the symptoms that you can acquire with the condition, when they start, and the changes the disease brings in the body.
The questions are basic, but Parkinson’s disease is not. Like other illnesses, Parkinson’s disease does not have a specific path of progression. Due to this, it is difficult to state or pin down the exact time or the path of the progression.
What Diseases And Conditions Resemble Parkinsons Disease
PD is the most common form of parkinsonism, in which disorders of other causes produce features and symptoms that closely resemble Parkinson’s disease. Many disorders can cause symptoms similar to those of PD, including:
Several diseases, including MSA, CBD, and PSP, are sometimes referred to as “Parkinson’s-plus” diseases because they have the symptoms of PD plus additional features.
In very rare cases, parkinsonian symptoms may appear in people before the age of 20. This condition is called juvenile parkinsonism. It often begins with dystonia and bradykinesia, and the symptoms often improve with levodopa medication.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Knowing That It Is Msa And Not Parkinsons Is Important
Over the years MSA Coalition Board Members have heard the frustration about a slow diagnosis after the initial diagnosis of Parkinson’s.While MSA is fatal, knowing the correct diagnosis, is still important.
Multiple system atrophy affects “multiple systems” in the body.As a result, while there are not MSA specific treatments, treating the various symptoms from sleep disorders, urinary and bowel issues, blood pressure control, etc. can vastly improve quality of life. The earlier an MSA patient is diagnosed, the earlier doctors can establish a plan of action to improve symptoms that can be very disabling. Another factor is that Parkinson’s medications typically stop working in MSA patients.
An early diagnosis also allows patients and their families to spend quality time together while they are still able.It also provides time to prepare for end-of-life issues, such as preparing wills and living wills.
What Are The Causes And Symptoms Of Parkinsons Disease
As a neurodegenerative disorder, Parkinson’s Disease leads to the progressive deterioration of motor function due to loss of dopamine-producing brain cells. While the cause of Parkinson’s Disease is unknown, researchers speculate that both genetic and environmental factors are involved. Studies also show that men are 50% more likely to develop the disorder than women.
Primary symptoms of Parkinson’s Disease:
- tremor
- dementia
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinson’s disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinson’s disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinson’s disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinson’s disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinson’s disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
What Are The Different Stages Of Parkinsons Disease

Each person with Parkinson’s disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinson’s disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinson’s disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
What Doctors Look For When Diagnosing Parkinsons
Certain physical signs and symptoms — noticed by the patient or his or her loved ones — are usually what prompt a person to see the doctor. These are the symptoms most often noticed by patients or their families:
-
Shaking or tremor: Called resting tremor, a trembling of a hand or foot that happens when the patient is at rest and typically stops when he or she is active or moving
-
Bradykinesia: Slowness of movement in the limbs, face, walking or overall body
-
Rigidity: Stiffness in the arms, legs or trunk
-
Posture instability: Trouble with balance and possible falls
Once the patient is at the doctor’s office, the physician:
-
Takes a medical history and does a physical examination.
-
Asks about current and past medications. Some medications may cause symptoms that mimic Parkinson’s disease.
-
Performs a neurological examination, testing agility, muscle tone, gait and balance.
What Are The Complications Of Parkinson Disease
Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may arise later. As the disease gets worse with time, many people develop dementia. This can cause profound memory loss and makes it hard to maintain relationships.
Parkinson disease dementia can cause problems with:
- Speaking and communicating with others
- Problem solving
- Forgetfulness
- Paying attention
If you have Parkinson disease and dementia, in time, you likely won’t be able to live by yourself. Dementia affects your ability to care of yourself, even if you can still physically do daily tasks.
Experts don’t understand how or why dementia often occurs with Parkinson disease. It’s clear, though, that dementia and problems with cognitive function are linked to changes in the brain that cause problems with movement. As with Parkinson disease, dementia occurs when nerve cells degenerate, leading to chemical changes in the brain. Parkinson disease dementia may be treated with medicines also used to treat Alzheimer’s disease, another type of dementia.
Signs It Could Be More Than Parkinsons Disease
Feb 9, 2020 | MSA-Blog |
Close to one million people in the US have a diagnosis of Parkinson’s disease .Unfortunately, for a small percentage of these people the diagnosis just doesn’t seem right. They feel like something more is wrong.Their medicines may not be very effective. They might have severe dizziness and even be prone to fainting.They just sense the disease is progressing faster than expected.
Parkinson’s Disease Symptoms: Life Expectancy
Even though Parkinson’s disease is a serious, progressive condition, it is not considered a fatal illness. People who have Parkinson’s disease usually have the same average life expectancy as people without the disease.
But when the disease is in its advanced stages, Parkinson’s symptoms can lead to life-threatening complications, including:
- Falls that lead to fractured bones
- Pneumonia
- Choking
Thinking about the progression of Parkinson’s disease can be frightening. But proper treatments can help you live a full, productive life for years to come. And researchers hope to one day find ways to halt the progression of Parkinson’s and restore lost functioning.
