Patients Who Start To Experience Dysphagia Should Always Inform Their Prescriber And Pharmacist So They Can Obtain The Best Advice On Their Medicines
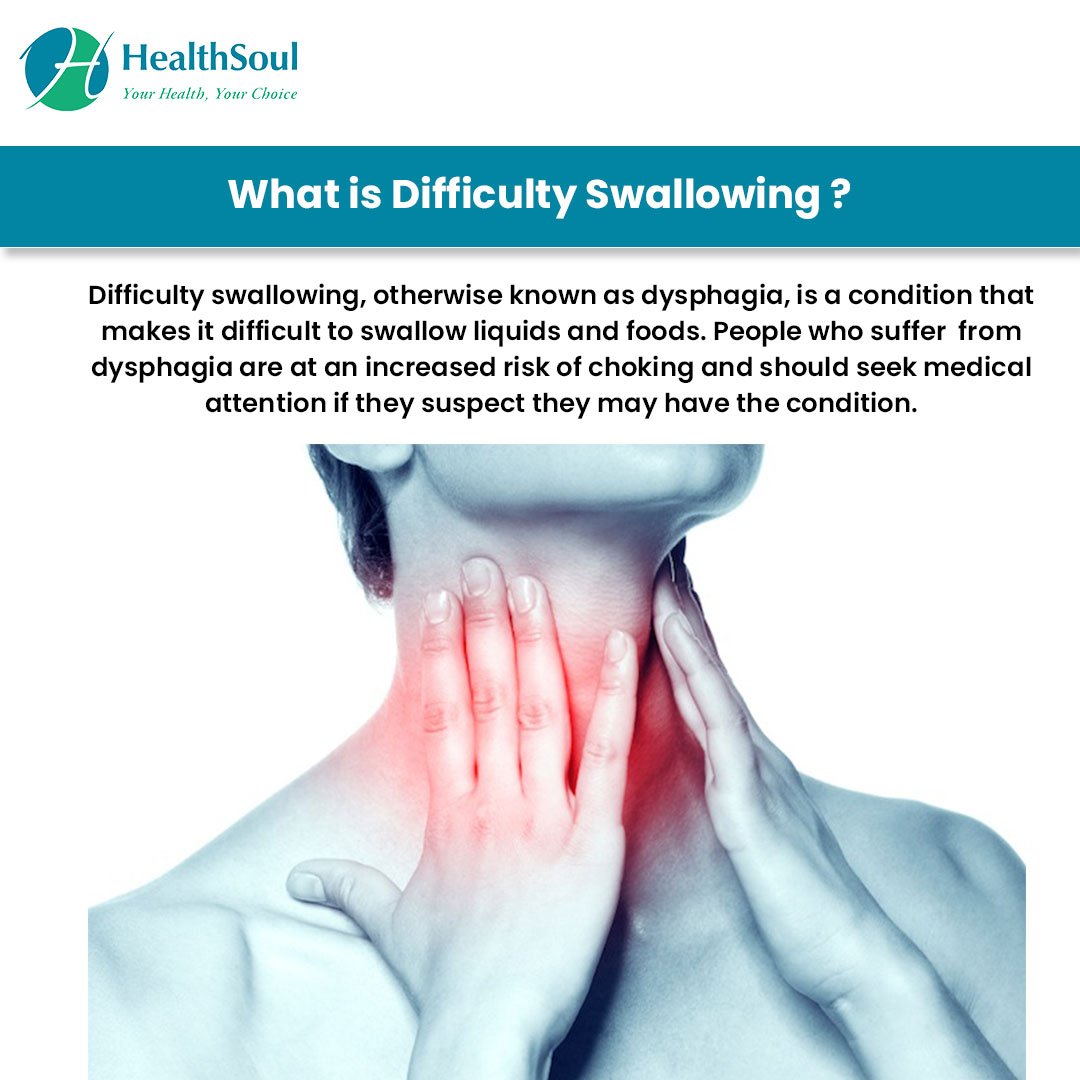
Many medicines are now available as dispersible tablets, patches or liquid medicines. It is therefore frequently not necessary to manipulate tablets or capsules when a patient has dysphagia. Although the pharmacist is the best person to ask about what is available, there is a website where you can type in the name of your drug to find alternatives – visit www.swallowingdifficulties.com for more information. For example, Madopar is available as a dispersible tablet.
Different types of modified release tablets and capsules
Liquid medicines, which are available for many medications, are designed to be palatable and provide a consistent dose. In many cases, they have a thick consistency to reduce the likelihood of aspiration. However, when there is no suitable alternative, the only option may be to tamper with the tablet or capsule before swallowing.
Tablet casings and coats
Tablets and capsules are very carefully designed to ensure that they are not only acceptable to patients but that the drug is released at the correct speed and in the best location. They each contain a number of different ingredients that are selected to ensure they don’t interfere with the drug. It is important, therefore, that different crushed or dispersed tablets should not be mixed together.
C Follow These Tips To Decrease Swallowing Difficulty & Aspiration Risk:
Although these tips are not a substitute for evaluation and training by a speech-swallow therapist, I think following these instructions will be very helpful for you.
How Do You Know If You Or Your Loved One Has A Problem With Swallowing
Swallowing difficulties can start very subtly and initially not be obvious to either the person with PD or their loved ones. There are signs to look out for before swallowing difficulty becomes overt . Some of the signs you should pay attention to include:
- Slow rate of eating – people with difficulty swallowing may slow down their eating in order to avoid coughing or choking
- Fatigue during eating or decreased enjoyment of food
- A sensation that food is “sticking” in the throat
- Coughing or excessive throat clearing during eating
- Difficulty in swallowing pills
- Unexplained weight loss– people with difficulty swallowing may reduce their consumption in an attempt to eat without coughing or choking
- Change in dietary habits – people with difficult swallowing may alter their diet in order to avoid foods that cause difficulty. This may not be a choice made consciously
- Diagnosis of a pneumonia – this could be caused by aspiration, or entry of a foreign substance into the airway
If you think there might be a swallowing issue, it is important to speak with your doctor about it. There are steps you can take to properly assess the situation and improve your swallowing function. This can in turn reduce your risk of choking, make eating more enjoyable, and lessen the chances of unwanted weight loss and/or other discomforts.
Swallowing Exercises Can Be Very Helpful To Improve Your Swallowing
After a formal swallow assessment, swallowing therapy sessions can be designed for you, involving exercises tailored to the specific parts of your mouth and throat that are causing the swallowing problem. Sessions may involve practicing compensatory swallowing strategies with various types of foods in order to maximize safety and efficiency while swallowing.
During swallow therapy, recommendations may include:
- Best feeding techniques
- Exercises to strengthen oral and throat muscles
- Compensatory techniques to assist in safe swallowing
- Oral and mouth care techniques
- Appropriate food selection and ways to modify food texture
- Safe positioning strategies
Clinical Features And Diagnosis Of Dysphagia In Parkinsons Disease
Oropharyngeal dysphagia in PD may limit or preclude safe oral feeding, reducing the patient’s full capacity in society and resulting in social, psychological, and economic problems for the individual .
One of the first reports of parkinsonian dysphagia was in 1817 by James Parkinson, who described a typical case of PD with weight loss, difficulty in swallowing solids and liquids, sialorrhea, and reduced tongue movements .
In 1983, Longemann proposed the videofluoroscopic swallowing study as a means of assessing the dynamics of swallowing. Parkinsonian VFSS can show specific impairments, such as those in the oral pharyngeal and esophageal phases. In the oral phase, these include orofacial tremor, difficulty forming a cohesive food bolus, prolonged swallowing time, limited tongue and mandibular excursion during mastication, and the presence of repetitive anteroposterior movements of the tongue during bolus propulsion . Pharyngeal phase impairments include delayed pharyngeal response with consequent stasis in the valleculae and piriform sinuses, with the risk of laryngeal penetration and aspiration, and impairment of pharyngeal muscle contraction and cricopharyngeal function . Impairments in the esophageal phase of swallowing include reduced peristalsis and reduced transit time. All of these disturbances occur together with the traditional motor symptoms of PD as a result of degeneration of the autonomic nerve system and voluntary muscle system .
Oral Dysfunction In Parkinsons: Swallowing Problems And Drooling
Two common and distressing problems that can develop in Parkinson’s disease are swallowing dysfunction and drooling. I want to help you better understand these issues and learn what you can do to improve them – so read on!
Thank you to Christine Sapienza, PhD, CCC-SLP and Bari Hoffman Ruddy, PhD, CCC-SLP for providing some of the material below.
Management Of Dysphagia In Patients With Parkinson’s Disease
Treatment of PD has traditionally been pharmacologic and was revolutionized by the discovery that levodopa is able to penetrate the blood–brain barrier and be converted to dopamine in the central nervous system. However, the effect of pharmacologic treatment on oral communication and swallowing is still controversial.
Drug treatment appears to have little effect on speech and swallowing disturbances compared with the major effect it has on motor symptoms in the trunk and limbs. In a study on voice and swallowing, when patients were asked about the effects of medication, all reported clear improvements in general physical symptoms, but only three out of twenty-four patients reported improvements in oral communication and swallowing symptoms. This suggests that both dysarthrophonia and dysphagia are related to dysfunction of nondopaminergic neuronal pathways .
Although the subject of much controversy in the past, the value of speech therapy has been confirmed in several objective studies . The effects of speech therapy on voice and swallowing were analyzed in a study, which showed that there was a 100% improvement in symptoms after therapy, particularly increased sphincteric action of the larynx .
The Preponderance Of Injury In The Past Of People With Pd
Neck issues or damage can be caused by injuries, but the injury site doesn’t have to be local to the neck itself, since it is an integral part of the kinetic chain of the human body – problems anywhere else which affect posture can, in turn, profoundly affect how we tense our necks and cause strains on it by the way we are holding up the head. I’ve frequently asked people with Parkinson’s Disease to think carefully about any pains and injuries which they might have incurred either before or concurrent with their PD diagnosis. I’ve found that the overwhelming majority of us have suffered a prior accident or physical trauma. Injuries to jaw, neck, shoulders, back, hips, knees or feet predominate. All these severely affect posture and hence the kinetic chain and are liable to make our necks prone to permanent strains and stiffness. So in my view, even if chemical “cures” were invented tomorrow, people with PD would still present with the postural problems, still suffer from the old injuries which have been masked by the narratives of neurology, and would probably quickly decline into pain and problems again, unless these past injuries are properly attended to.
Why Do Parkinsons Patients Cough While Swallowing Food
When a small particle of food goes into the wind-pipe, we gag & start coughing vigorously to throw the particles out. These are called the “Gag” and “Cough” reflexes.
Food can go into the wrong pipe often in Parkinson’s patients . Therefore they frequently cough while swallowing food.
But the condition becomes even more problematic in advanced Parkinson’s disease.
In advanced Parkinson’s disease, there may be no coughing even when particles are entering the windpipe. This is dangerous!
Thus, particles of food may repeatedly go into the lungs of Parkinson’s patients without them noticing it. This is called “Silent Aspiration”.
Is Difficulty Swallowing Common In Parkinsons Disease
Yes.
Many patients with Parkinson’s disease may complain of difficulty swallowing. The medical term for swallowing difficulty is “Dysphagia”.
In milder cases, you may just have the feeling that food gets “stuck” in your throat. Some patients may report that they have a feeling of their “throat closing” when they try to swallow.
In more severe cases, you may tend to choke on your food if you try to swallow it too quickly.
What Else Can Help With Swallowing And Saliva Control
Speech and language therapy
If you need more advice on swallowing and saliva control, a speech and language therapist can help. Speak to your GP about getting a referral.
A speech and language therapist can give you tips to help you swallow more easily and teach you how to use any equipment for controlling saliva.
The Swallow Prompt app
Swallow Prompt is an app that delivers regular and discreet prompts that remind you to swallow. It’s available for iPhone, iPad and Android devices.
What Can You Do About Weight Loss Associated With Pd
If you do find yourself unable to maintain a healthy weight, discuss this with your doctor. The good news is that after a medical workup, he or she may suggest one or more of the following steps that can help you:
Tips and takeaways
- Despite a diagnosis of PD, weight loss should prompt a full medical workup.
- Weight loss that is attributed to PD can be caused by a variety of reasons including decreased appetite, increased energy expenditure, swallowing difficulties, and poor gut motility.
- Weight loss has been linked to a poorer quality of life in PD and may contribute to increasing frailty.
- There are steps you can take that may help. Depending on the causes contributing to weight loss, efforts to counteract weight loss could include consultation with a dietician, swallow evaluation and PD medication adjustment.
- As with all symptoms, discuss your concerns about weight loss with your doctor.
Do you have a question or issue that you would like Dr. Gilbert to explore?
Dr. Rebecca Gilbert
APDA Vice President and Chief Scientific Officer
Definition And Classification Of Parkinsonism And Pd

PD is a progressive parkinsonism of undetermined cause without features suggestive of an alternative diagnosis. It responds to dopaminergic treatment and is associated with depletion of dopaminergic neurons and the presence of Lewy body inclusions in some of the remaining nerve cells .
Parkinsonian disorders can be classified into four categories: primary parkinsonism, secondary parkinsonism, heredodegenerative parkinsonism, and multiple system degeneration . A number of features, including tremor, early gait abnormality , postural instability, pyramidal tract signs, and response to levodopa, can be used to distinguish PD from other parkinsonian disorders. While differences in the density of postsynaptic dopamine receptors in PD patients or patients with atypical parkinsonian disorders have been used to account for the poor response to levodopa therapy in the latter group, other explanations may also be possible .
| UK Parkinson’s Disease Society Brain Bank |
| Step 1 |
Diagnostic criteria for Parkinson’s disease
If You Have Swallowing Difficulty What Can Be Done
In some cases, swallowing function varies in response to dopamine medication doses, much like other aspects of motor function. Therefore, if swallowing becomes problematic, an increase in dopaminergic medications can be tried. In addition, make sure you undergo a swallow evaluation when you are in the ON state.
Even before a formal swallow study, you can take steps to increase the efficiency of your swallow. These include:
- Sit upright during all eating and drinking, even when taking pills
- Tilt the head slightly forward, not backward, as you swallow
- Take small bites of food, chew thoroughly, and do not add any more food until everything from the first bite has been swallowed
- Take small sips of liquid
- Concentrate while moving the food backward in the mouth with the tongue
- “Double swallow” if the food did not go down completely with the first swallow
- Sometimes taking a sip of liquid between bites of food can help to wash the food down
- If eating is very tiring, try several smaller meals spaced out during the day instead of three large meals.
How Do I Know If I Have A Speech Or Voice Problem
- My voice makes it difficult for people to hear me.
- People have difficulty understanding me in a noisy room.
- My voice issues limit my personal and social life.
- I feel left out of conversations because of my voice.
- My voice problem causes me to lose income.
- I have to strain to produce voice.
- My voice clarity is unpredictable.
- My voice problem upsets me.
- My voice makes me feel handicapped.
- People ask, “What’s wrong with your voice?”
Swallowing Difficulties And Parkinsons Medication
If swallowing tablets or capsules becomes difficult, it may be tempting to crush tablets or open capsules, but this should never be done, as it can cause serious side effects and/or prevent the medication working properly. Always ask your pharmacist or doctor, or check the patient information leaflet before tampering with medicines in any way. Swallowing medications with jelly, yoghurt or apple sauce may help you swallow medication more comfortably.
Many Parkinson’s medicines are prepared or designed to work in a particular way that will be harmed by crushing or opening capsules. For example, some medicines have:
- Sugar or film coating: This is usually to make them taste better, but crushing may make them taste unpleasant.
- Enteric coating: This coating is designed to keep the tablet whole in the stomach, in some cases to protect the stomach or to protect the medicine from stomach acid so that it is released after passing through the stomach, for example in the intestine. This type of tablet should never be crushed.
- Modified or controlled release: These medications have been designed to release slowly and act over a longer period, so they can be taken less often. Crushing this type of tablet would lead to a rapid release of the medicine which could be harmful.
If you experience any problems you should talk to your doctor, so that he or she can prescribe medication in a form that is easier to take. Some medicines are available in liquid form.
A Exercises To Improve Swallowing Difficulty :
A speech-swallow therapist evaluates how your muscles move while swallowing. They can teach you important exercises to improve swallowing difficulty and prevent Aspiration.
Speech therapists specially trained in Parkinson’s can teach you exercises such as Expiratory Muscle Strength Training or Lee Silverman Speech Therapy or LOUD therapy.
These specialized training sessions are tremendously helpful in improving voice. But these exercises also make swallowing easier.
Why Worry About Weight Loss Associated With Pd
Weight loss has been linked to a poorer quality of life and more rapid progression of PD. The reasons for this are two-fold. On the one hand, as outlined in the list above, weight loss can be a hallmark of advancing disease – as it could be a consequence of more swallowing difficulties, worsened mobility, more impaired gut function etc.
On the other hand, having weight loss can further lead to poorer health. Inadequate food intake can contribute to malnutrition and vitamin deficiencies. Malnutrition can subsequently be the cause of increased susceptibility to infection, increased fatigue and increased frailty. The situation can spiral with more fatigue and frailty causing a further decrease in activity and function.
Osteoporosis, or porous and fragile bones, is more common in under-weight people since bone structure is dependent on weight-bearing. Since osteoporotic bones are more prone to fracture during a fall, this too can be a contributor to more disability and frailty. Bottom line is that it is important for your health to maintain a healthy weight.
Swallowing Difficulties In Parkinsons Disease
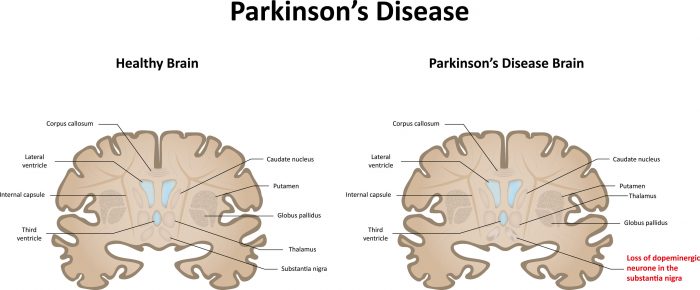
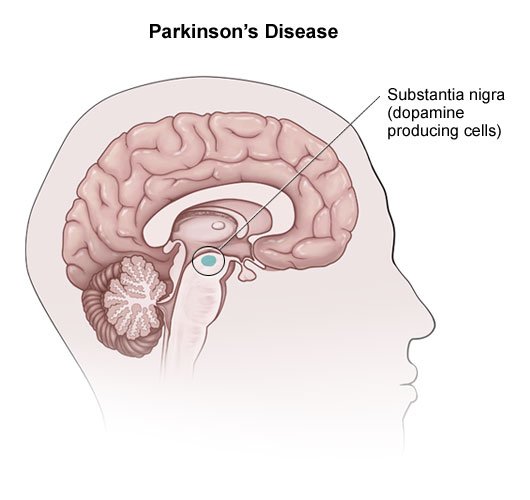
The act of swallowing involves a complex series of activities that begin in the mouth, continue in the pharynx and end in the esophagus. These include chewing, using the tongue to move the bolus of food to the back of the throat and then coordinating the muscles that both propel the food into the esophagus and protect the airway or trachea from food penetration. Swallowing dysfunction can be considered both a motor and a non-motor symptom of PD. Loss of dopamine neurons in the substantia nigra area of the brain can cause the motor dysfunction that impairs swallowing. However, loss of neurons in other areas of the brain, such as the cortex and lower brain stem can also affect the overall control and coordination of swallowing, and can be thought of as a non-motor symptom of PD. Swallowing issues are very important to diagnose. Impacts on your daily life and your health can range from difficulties with meals to more extreme cases where it could lead to choking and aspiration which can be very serious or even fatal.
How Parkinson’s May Make Swallowing Difficult
This morning I woke up with a sore throat. A mild sore throat caused by a viral infection is uncomfortable when swallowing, making you aware how often you swallow through the day. But it does not limit the efficiency or safety of swallowing food and liquid as in swallowing disorders. Parkinson’s disease is one of the well-known causes of swallowing disorders also called ‘dysphagia’. Dysphagia can lead to less eating and drinking or aspiration of food and liquid resulting in coughing or near choking. That is why some researchers and clinicians advocate early screening of dysphagia in people with Parkinson’s disease . But how frequently does dysphagia occur in Parkinson’s disease and what are typical signs of dysphagia in PD?
Then is early screening for dysphagia in PD needed? There are several points of view depending on the disease severity and availability of services. Routinely asking about difficulties with swallowing is a good start, in particular in advanced PD, but more detailed questioning may uncover possible dysphagia more reliably than a single question. Most importantly, PwP should be aware that also difficulty with chewing or swallowing is usually caused by their Parkinson’s, but can be treated or compensated quite well .
Links:
Eating Swallowing Problems And Saliva Control
Page contents
Eating and swallowing problems, known as dysphagia, occur in many medical conditions and become more common as we get older.
The main risks associated with swallowing problems are:
- Choking or asphyxiation: When food blocks the airway, preventing breathing. Also, when food or liquid enter the airway below the level of the vocal cords.
- Aspiration pneumonia: When food or liquid enter the lungs, this may cause a lung infection.
- Increased secretion: As a reaction to food or liquid entering the lungs.
- Dehydration: Lack of fluids can lead to problems such as constipation.
- Malnutrition: Lack of nourishment leads to poor health and harms the body’s ability to fight infection.
- Drooling: decrease in mouth sensitivity and / or a reduction in the frequence of swallowing saliva can cause drooling.
- Difficulties in swallowing medications.
Eating And Swallowing Problems And Parkinsons
Research suggests that eating and swallowing difficulties affect about a 90% of all people with Parkinson’s. The true figure may be even higher as some people do not report the problem to their health care team.
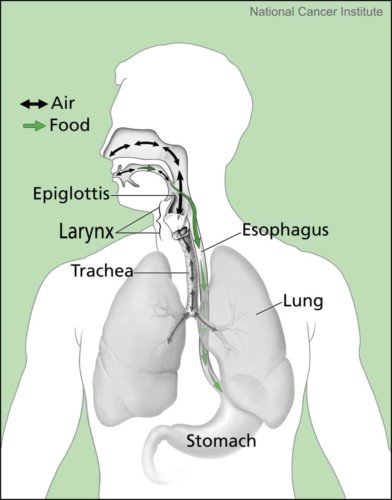
Swallowing is a motor function that includes three stages.
- The first stage is the oral phase: food is chewed and mixed with saliva to form a soft ball called bolus. The tongue then pushes the bolus to the back of the mouth, triggering the swallow reflex.
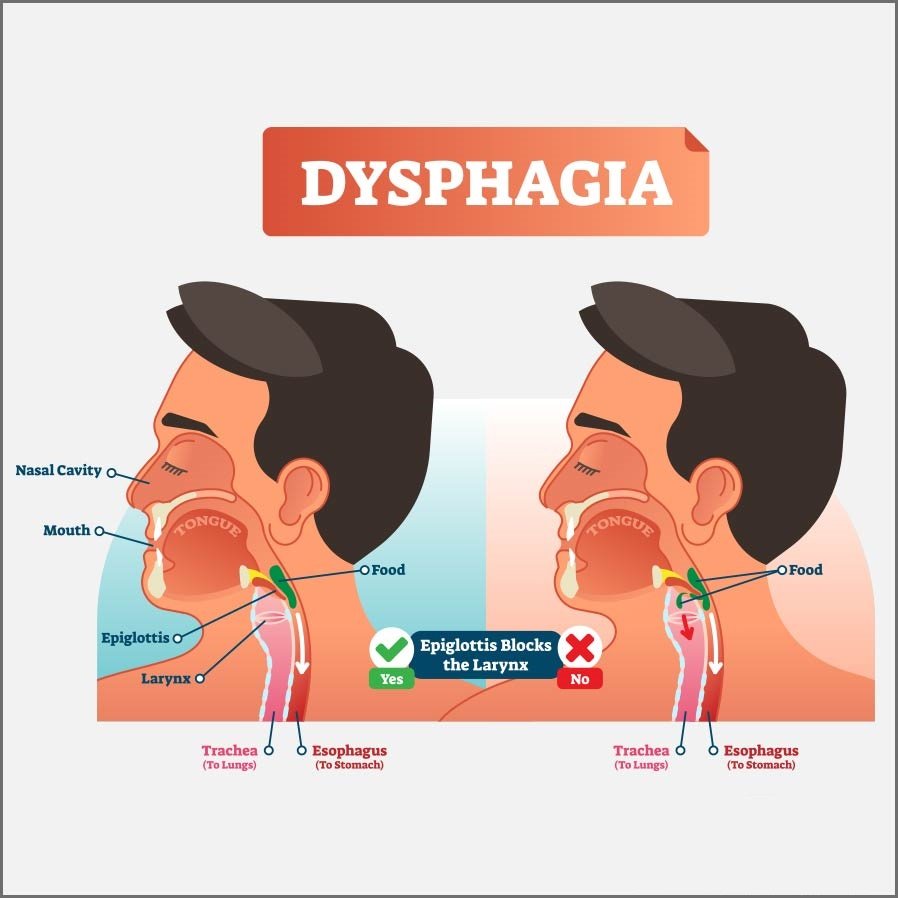
- The second stage is the pharyngeal phase: it is the involuntary closure of the larynx by the epiglottis and vocal cords, which temporarily inhibites breathing. These actions prevent food from going ‘down the wrong pipe’ into the trachea .
- The third stage is the esophageal phase: the bolus moves into the esophagus, the muscular tube that contracts to push the bolus into the stomach.
Unfortunately, many people with Parkinson’s experience swallowing problems due to reduced control and muscle tone of the jaw, lips, tongue and throat muscles, especially in later stages of the condition. Eating and swallowing becomes slower and requires more effort.
People with Parkinson’s are at particular risk of aspiration due to a delay in the triggering of their swallow reflex. This compromises the effectiveness of the airway protection while swallowing. This can lead to aspiration pneumonia due to a lack of coughing if food enters the windpipe, allowing food to reach the lungs unchecked.
How Can I Make Chewing And Swallowing Easier
The way you sit, the foods you eat, and how you eat can affect your ability to swallow. To use your posture to make chewing and swallowing easier, you can:
- Sit upright at a 90-degree angle.
- Tilt your head slightly forward.
- Stay seated or standing for 15-20 minutes after you eat a meal.
When you eat:
How Do I Know If I Have A Swallowing Problem
- I have recently lost weight without trying.
- I tend to avoid drinking liquids.
- I get the sensation of food being stuck in my throat.
- I tend to drool.
- I notice food collecting around my gum line.
- I tend to cough or choke before, during or after eating or drinking.
- I often have heartburn or a sore throat.
- I have trouble keeping food or liquid in my mouth.
*Please note that not all content is available in both languages. If you are interested in receiving Spanish communications, we recommend selecting “both” to stay best informed on the Foundation’s work and the latest in PD news.
Excessive Saliva And Drooling In Parkinsons
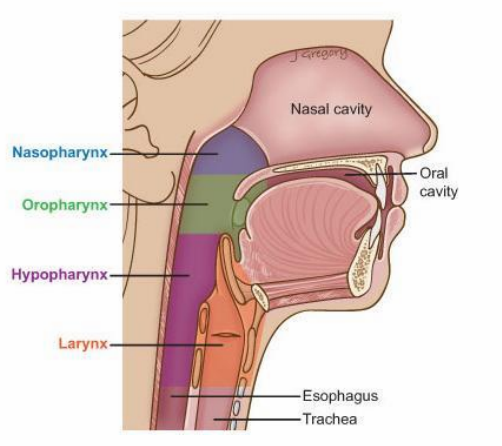
Saliva is needed for the first stages of digestion, including chewing and swallowing. This watery substance contains enzymes that start to digest our food.
Many people with Parkinson’s experience poor saliva control, which may result in excessive saliva and drooling, or alternatively, in a dry mouth and other eating problems.
Treating Eating And Swallowing Difficulties
If you or someone you care for is experiencing difficulties with eating, swallowing or saliva control, the first step is to consult your doctor, who may refer you on to an SLT / SLP.
Your doctor may be able to adjust the timing and dose of medicines so that these are working well at mealtimes and so swallowing problems are better managed when eating. However, for some patients, medications do not affect the swallowing function.
Your doctor may also adjust your medications, or may prescribe new ones to reduce production of saliva. Some Parkinson’s medicines, including levodopa, improve muscle movement and may help to reduce drooling. However, some medications, such as clozapine, which is prescribed for mental health problems, can actually increase saliva production.
Anticholinergic medications may help to reduce the amount of saliva you produce but are not suitable for everyone. For more information see Managing medication.
Botulinum toxin can be injected into the salivary glands to reduce saliva production. This treatment will not work for everyone and injections may need to be repeated every three to six months. However, for some patients, Botox injections are not recommended and may be dangerous.
In severe cases when other treatments are not effective, radiotherapy to the salivary glands can restrict saliva production. In extreme cases the salivary glands can be surgically removed as a last resort.
Slow Muscles Carrying Food To Your Stomach
Parkinson’s may also slow down the muscles carrying food down into your stomach. Food moving slowly down your food pipe to your stomach can make you feel full up. But once it arrives at your stomach you realise you’re still hungry. By this time the food on your plate may have gone cold and be unappealing.
Urinary Difficulties In Parkinsons Disease
The most common urinary difficulty experienced by people with PD is a frequent and urgent need to urinate. Urinary incontinence, the involuntary loss of urine, is also a symptom of PD. This may occur even when the bladder is not full. Recent research studies estimate approximately 27-39% of people with PD experience urinary difficulties, although urinary incontinence only develops in about 15% of those with PD. Bladder issues usually develop in the later stages of PD.2
There are several medications that can help manage urinary difficulties, such as tolterodine, oxybutynin, darifenacin, and solifenacin. These medications work to block or reduce overactivity in the bladder. However, these medications may make the symptoms of PD worse. It is recommended to discuss these treatments with a movement disorders specialist who has been trained to understand the effects of various medications on the disease.2
Why Does Parkinsons Disease Cause Drooling
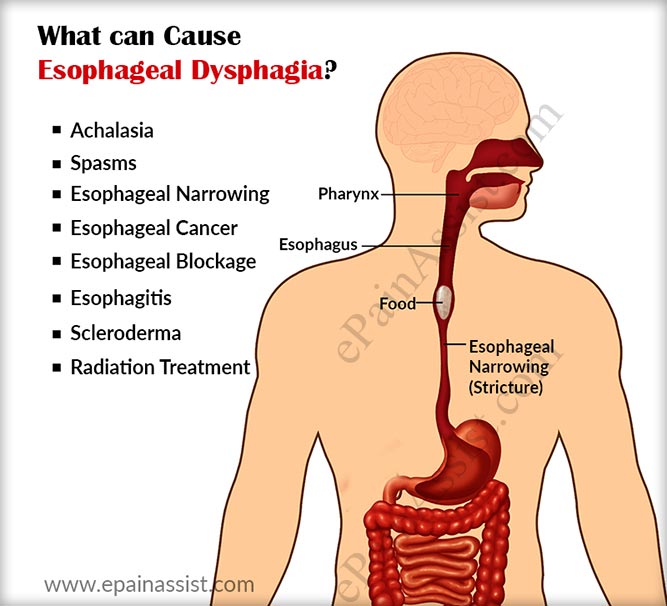
Saliva is produced by small glands around our mouth, called “Salivary glands”.
It is a common misconception that Parkinson’s patients have drooling because they are producing too much saliva. In fact, multiple studies have shown that most Parkinson’s patients produce less saliva.
Our salivary glands continuously produce saliva, even when we are not eating.
Normally, we automatically swallow this saliva, through small gulps that we don’t even notice.
But in Parkinson’s disease, there is a marked decrease in all automatic movements, including automatic swallowing.
Therefore, saliva accumulates in the mouth. When the mouth is full, it drips out. We call this “Drooling”.
Let’s talk about treatment…
A Reducing The Amount Of Saliva Produced:
Saliva can be reduced by a number of medications called “Anticholinergics”. These include medications such as Glycopyrollate, hycosamine etc.
These medications tell our salivary glands to decrease saliva production.
Some of these medications are also available in convenient packages such as skin patches. A “Scopolamine patch” is a small sticky patch applied to the skin. It gradually releases a medication called scopolamine. It needs to be replaced every 3 days.
Actually, I am not a big fan of these medications. Anticholinergics can produce some nasty side-effects such as confusion and urinary retention . Therefore, they need to be used carefully and at the lowest dose possible.
A much better alternative is botox injections into the salivary glands. These injections markedly decrease saliva production, reducing drooling dramatically in many cases.
Here is a link to one of the numerous research studies that have demonstrated the safety and efficacy of botox injections for excessive drooling in Parkinson’s disease .
Botox injection into the salivary glands does not cause severe pain. It can be performed within a few minutes, in the outpatient department. There is no reason to get admitted.
Since such a small dose of botox is used, and very little of the botox goes into the bloodstream, there are usually no side-effects.
The only problems are that the injections are somewhat expensive & wear off after some time. They may need to be repeated every 3-6 months.
Tips For Coping With Speech Difficulties
- Exercise your voice by reading out loud or singing every day.
- Drink enough water, avoiding shouting and rest your voice when it is tired.
- Train your voice like an actor—sit and stand with good posture, do exercises for articulation, breathing and projecting the voice.
- Get feedback from friends and family members about how others perceive your speech —develop a cue or code word you can use in public to make you focus on speaking clearly.
- If you have soft speech, use tools such as a voice amplifier , placed on your shirt, and on the telephone . Ask an occupational therapist about other tools.
- Make eye contact with the person to whom you are speaking.
- Reduce background noise.
- Socialize in small groups or one-on-one.
- If you experience a facial masking, use “feeling” words to communicate your emotions . Use practice physical gestures to help convey emotions.
- Determine which times of day your speech is best. Plan social engagements around those times.
Even in the early stages of PD, many report that their voices are too soft, causing others to ask them to repeat themselves. Other people with PD may have a gruff or hoarse quality to their voice. Try these strategies:
Page reviewed by Dr. Chauncey Spears, Movement Disorders Fellow at the University of Florida, a Parkinson’s Foundation Center of Excellence.
For more insights on this topic, listen to our podcast episode“Importance of Early Detection of Swallowing Disturbances.”
