Falls Can Be Prevented With Appropriately Prescribed Exercise In People With Mild To Moderate Pd
Physiotherapy aimed at preventing falls in people with PD should consider the individuals risk of falls and their fall risk factors. A systematic review showed that exercise reduces the frequency of falls in PD by 60 per cent . However, detailed investigation of randomised controlled trials indicates that when exercise is semi-supervised , falls are reduced in people with milder disease , but are increased in those with more advanced disease .
It is recommended that physiotherapists use the three-step clinical prediction tool to quickly and accurately predict an individuals probability of falling in the next six months as low , moderate or high . People with a low to moderate risk are suitable for group or semi-supervised physiotherapy that targets their remediable fall risk factors commencing as soon as possible after diagnosis.
Evidence is scant regarding intervention for people with high fall risk. However, a carefully monitored multidisciplinary approach, including medical review and higher levels of exercise supervision, along with environmental and behavioural modifications, is suggested.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Dont Miss: Stabilizing Spoon For Parkinsons
What Future Medications May Be Available For Parkinsons
There are numerous studies investigating new treatments for Parkinsons disease.
There has been new information about the role of autoimmunity and T-cells in the development of Parkinsons disease, possibly opening the door to a role for biologics.
Stem cells are also being investigated as a treatment option for Parkinsons disease.
Also Check: Do Parkinson’s Patients Have Tremors During Sleep
Anticholinergics In Clinical Trials For Parkinsons Disease
Several studies have shown that anticholinergics are useful in reducing tremors. Two studies, one published in Movement Disorders and the other in Archives of Neurology, found that anticholinergics, as well as dopamine agonists , are effective at reducing tremors in Parkinsons disease. Some patients responded better to one treatment than the other.
Studies have also shown, however, that anticholinergics may be associated with greater cognitive decline in Parkinsons patients. A meta-analysis study showed that anticholinergics lead to a definite improvement in motor symptoms but are also associated with side effects including cognitive decline and hallucinations. The study analyzed six anticholinergics but did not have enough evidence to compare their efficacy.
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Recommended Reading: Lyme Disease And Parkinson’s
Avoid Anticholinergics In Parkinsons Say Researchers Despite Study Findings
Researchers say there are good reasons why study did not confirm deleterious effects on cognition in Parkinsons disease patients.
Adverse drug events
BSIP, Cavalini James / Science Photo Library
Use of anticholinergic drugs by patients with newly diagnosed Parkinsons disease is not associated with cognitive decline, according to new research, but the study authors say there may be good reasons why these findings contradict previous studies.
The study, led by Alison Yarnall, a research fellow at Newcastle University, used data from the ICICLE-PD study a twin-centre, longitudinal, observational study exploring the development of dementia in Parkinsons disease .
The researchers studied the medication history of 219 patients with incident PD and 99 healthy controls to calculate each participants anticholinergic burden using the anticholinergic drug scale . Each drug was given a score from 0 to 3 according to its level of anticholinergic activity and these were summed at baseline and 18 months for each participant.
Comparing patients who had an ADS score of 0 at 18 months with those with an ADS score of one or more at both time points , the researchers found no difference in global cognition or in assessments of attention, memory or executive function. The proportion of patients with mild cognitive impairment was also similar between the two groups, at 49.4% in PD+ADS and 45.5% in PD-ADS .
Also Check: Wolff Parkinson White Syndrome Drugs To Avoid
Parkinsons Disease Nurse Specialist Interventions
care has been pioneered in the UK over the last 10 years supported by the UK . A PDNSs role is defined as a practitioner with essential skills in:
- providing ongoing support and advice
- referral to other therapists
A recent report from the UK identified the key roles and responsibilities of the in the UK as:
- making and receiving referrals directly to create an integrated and responsive service for people with
- admitting and discharging people for specified conditions and within agreed protocols
- managing caseloads
- providing information, education and support to people in their homes, in clinics and in hospitals
- prescribing medicines and treatment and monitoring the effectiveness of changes in medication and treatment
- using the latest information technology to triage people with to the most appropriate health professional
- using IT to identify people at risk and speed up responses to crises.
What is the effectiveness of care versus standard medical care in the management of people with ?
Read Also: What Kills A Person With Parkinsons Disease
You May Like: How Long One Can Live With Parkinson’s Disease
Icipating In Clinical Trials
Clinical trials and their participants have revolutionized Parkinsons treatment, and have changed the lives dramatically of those affected. They have helped make available many new treatments in addition to improving the delivery methods of medications and new deep brain stimulation techniques.
Clinical trials are essential to the future of Parkinsons research, and APDA is committed to this vital effort.
Mindfulness Context Mechanism Outcome Configurations
From the two included mindfulness studies, we generated nine CMO configurations focused on explaining what mindfulness interventions, worked for whom, under what circumstances, and why . The Parkinsons active living program reduced apathy in persons with PD . The PAL program focuses on behavioural activation therapy. The PAL program uses program coaches that are paraprofessional and trained as interventionists, and encourages the involvement of caregivers . The program focuses on providing foundational skills in activity planning, scheduling, and monitoring to encourage self-management and independence. Further mechanisms that may lead to the improvements in apathy include providing treatment by telephone, to prevent transportation barriers. Semantics may also play an important role in the success of the PAL program, as the use of the term program instead of intervention has a more positive connotation . Personality may also play a role in the success of mindfulness interventions at improving apathy, given some persons may dislike scheduling or persons may be too concerned with disappointing program coaches to focus on the intervention . The other included mindfulness study found a mindfulness-based stress reduction program yielded non-statistically significant improvements in apathy among persons with PD and no cognitive impairment . Mindfulness interventions may not be completed by persons that prioritize physical components of PD over emotional and cognitive symptoms .
You May Like: Is Tardive Dyskinesia Related To Parkinson’s
Anticholinergic Drugs Can Improve Movement Symptoms Of Parkinson’s Disease But With Adverse Mental Effects And There Is Not Enough Evidence To Compare The Different Drugs
Anticholinergics were the first drugs available for Parkinson´s disease and they are still widely used. They are believed to work by counteracting an imbalance which exists in Parkinson´s disease between two chemicals in the brain which transmit messages between nerve cells. However, anticholinergic drugs have been associated with unfavourable side effects. They are used alone, or with other anti-Parkinson’s drugs. The review of trials found that anticholinergics can improve movement problems in people with Parkinson’s disease, but also cause adverse mental effects . There is not enough evidence to compare the different anticholinergic drugs.
As monotherapy or as an adjunct to other antiparkinsonian drugs, anticholinergics are more effective than placebo in improving motor function in Parkinson´s disease. Neuropsychiatric and cognitive adverse events occur more frequently on anticholinergics than on placebo and are a more common reason for withdrawal than lack of efficacy.Results regarding a potentially better effect of the anticholinergic drug on tremor than on other outcome measures are conflicting and data do not strongly support a differential clinical effect on individual parkinsonian features.Data is insufficient to allow comparisons in efficacy or tolerability between individual anticholinergic drugs.
To determine the efficacy and tolerability of anticholinergics in the symptomatic treatment of Parkinson´s disease compared to placebo or no treatment.
Is Parkinsons Disease Treated By A Neurologist
People with Parkinsons disease will usually require a team of healthcare professionals to help them manage the condition.
A neurologist, a doctor specializing in conditions of the brain and nervous system, will be one of the main people involved in treating Parkinsons.
Other healthcare professionals who may help treat Parkinsons can include:
- a persons regular doctor
- a speech or occupational therapist
- mental health professional
- other specialists, such as a gastroenterologist, if people experience other symptoms of Parkinsons such as digestive issues
Recommended Reading: What Areas Of The Brain Are Affected By Parkinson’s Disease
What Is An Anticholinergic
Anticholinergics are a type of medication that blocks the action of a neurotransmitter called acetylcholine. Acetylcholine transfers signals between cells that affect specific bodily functions.
The medication blocks acetylcholine from causing involuntary muscle movements in the lungs, gastrointestinal tract, urinary tract, and other areas of the body.
As anticholinergics can affect a variety of functions, including digestion, urination, salivation, and movement, they can help treat many conditions.
Anticholinergic drugs work by blocking the activity of acetylcholine, a neurotransmitter, in the cholinergic system. The cholinergic system plays a role in:
Symptomatic And Neuroprotective Therapy

Pharmacologic treatment of Parkinson disease can be divided into symptomatic and neuroprotective therapy. At this time, there is no proven neuroprotective or disease-modifying therapy.
Levodopa, coupled with carbidopa, a peripheral decarboxylase inhibitor , remains the gold standard of symptomatic treatment for Parkinson disease. Carbidopa inhibits the decarboxylation of levodopa to dopamine in the systemic circulation, allowing for greater levodopa distribution into the central nervous system. Levodopa provides the greatest antiparkinsonian benefit for motor signs and symptoms, with the fewest adverse effects in the short term however, its long-term use is associated with the development of motor fluctuations and dyskinesias. Once fluctuations and dyskinesias become problematic, they are difficult to resolve.
Monoamine oxidase -B inhibitors can be considered for initial treatment of early disease. These drugs provide mild symptomatic benefit, have excellent adverse effect profiles, and, according to a Cochrane review, have improved long-term outcomes in quality-of-life indicators by 20-25%.
Neuroprotective therapy aims to slow, block, or reverse disease progression such therapies are defined as those that slow underlying loss of dopamine neurons. Although no therapy has been proven to be neuroprotective, there remains interest in the long-term effects of MAO-B inhibitors. Other agents currently under investigation include creatine and isradipine.
Recommended Reading: Is Coffee Good For Parkinson’s
What You Should Know About Your Parkinsons Medication
Each medication has its own particular properties and important considerations to be aware of. Below are some key aspects to think about before you start taking your medication. Detailed information regarding these can be found in the Patient Information Leaflet :
- what is it and what is it used for?
- special warnings and precautions
- what to do if you forget to take a dose
- what to do if you take more than you should
- possible effects on your ability to drive or use machinery
- safety in pregnancy and breast-feeding
The active ingredient in Disipal® Tablets belongs to the group of medicines called anticholinergic agents. Disipal® Tablets are used in the treatment of all forms of Parkinsons, a condition which can cause uncontrollable trembling of the hands, and other difficulties of movement, for example in standing or walking. Anticholinergic agents are also used when other medicines have caused these problems.
Procyclidine belongs to a group of medicines called anticholinergics. Anticholinergics stop a substance called acetylcholine working in your body.
Procyclidine is predominantly used in Parkinsons to help with muscle control and reducing stiffness.
Patient Information Leaflet and Summary of Product Characteristics
The PIL is the leaflet that is included with a medicine and is a patient-friendly version of the Summary of Product Characteristics. It gives information about taking or using a medicine.
Dont Miss: Treatment Of Dyskinesia In Parkinsons Disease
How Well Do The Outcomes Of The Intervention Provided To Mr Jennings Match Those Suggested By The Systematic Review
The interventions provided for Mr Jennings were most similar to those in the general physical therapy and exercise trials. Tomlinson et al reported significant improvements in the FRT with data from the exercise and cuing groups and in the TUG with data from the exercise, cuing, dance, and martial arts groups. Mr Jennings improvements in balance, as evidenced by the FRT and TUG results , were at the high end of the changes reported by Tomlinson et al.
Only limited data for the minimal clinically important difference of measures in people with PD are available they are predominantly from one study to date. The data reported may have been from people with much greater impairments, as indicated by the changes noted they would have been improbable for Mr Jennings, given his baseline status. Mr Jennings 6-minute walk test change score met the criterion of 50 m as the minimal clinically important difference reported for a variety of people with a variety of cardiopulmonary diagnoses.
Changes in FAR were not reported in the systematic review, but it is noteworthy that the change in FAR for Mr Jennings was at the high end of the improvements reported by Schenkman et al. No comparison data were found for the other 2 outcomes.
Dont Miss: How Long Does A Parkinsons Patient Live
Also Check: Parkinson’s And Exercise Research
What Are The Possible Side Effects Of Anticholinergics
Side effects can vary depending on the specific drug you are taking. The most common side effects of anticholinergic drugs include:3
- Memory problems
These are not all the possible side effects of anticholinergics. Talk to your doctor about what to expect or if you experience any changes that concern you during treatment with anticholinergics.
How Do Anticholinergic Antiparkinson Agents Work
Anticholinergic antiparkinson agents are a class of medications used to treat the symptoms of Parkinsons disease.
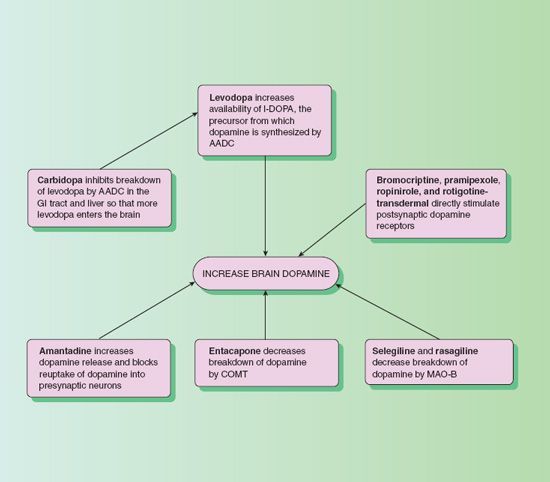
The direct cause of Parkinsons disease or Parkinsonian-like syndrome is the deficiency of the neurotransmitterdopaminein the brain. Antiparkinson medicines aim to prolong the action of dopamine in the brain by:
- Replacing dopamine
- Inhibiting dopamine breakdown
- Sensitizing dopamine receptors to stimulate dopamine release
Anticholinergic antiparkinson agents prolong dopamine action in the brain by inhibiting the reabsorption and storage of neurotransmitters. Reabsorption is a normal mechanism by which the body controls how long a nerve signal lasts. However, reabsorption can be an issue when there is a low level of dopamine. Hence, by limiting the reuptake of dopamine, anticholinergics increase dopamine concentration in the brain.
Also Check: Is There A Link Between Prostate Cancer And Parkinson’s Disease
How Do Anticholinergics Work
The motor symptoms of PD are caused by the reduction in dopamine. This is a neurotransmitter that sends signals in the brain to produce smooth, purposeful movement. As PD damages and destroys the nerve cells that make dopamine, the motor symptoms of PD appear.1,2
The primary treatments for PD directly affect dopamine. However, anticholinergics work in a different way to treat the symptoms of PD. They block the action of acetylcholine. This is another neurotransmitter involved in messages from the brain to the muscles. Anticholinergics work on correcting an imbalance between acetylcholine and dopamine in an area of the brain. Anticholinergics are often used in along with other treatments for PD.1,2
Speech And Language Therapy
Deterioration in speech is a common manifestation of that increases in frequency and intensity with the progress of the disease.
The specific resulting from is known as hypokinetic dysarthria and it is characterised by:
- monotony with reduced loudness and pitch range
- difficulties in initiating speech
- imprecise consonant
- breathy or harsh voice.
Treatment programmes have focused on specific components of the such as respiratory exercise and prosodic exercises. These treatments can be used with individuals or in groups.
is a speech therapy programme developed specifically for individuals with . It focuses on improving voice loudness with immediate carry over into daily communication. The intensive nature of the programme helps individuals with PD to recognise that their voice is too soft, convince them that a louder voice is within normal limits and makes them comfortable using the new louder voice. It is now provided by certified clinicians in England.
Some people with may benefit from use of augmentative and alternative communication devices, which can include the use of:
- alphabet boards
Read Also: Patron Saint For Parkinson’s Disease
