A High Rate Of Genetic Parkinsons Makes Israel A Perfect Lab For Finding Ways To Prevent Stop And Even Cure This Fast

Parkinson’s disease is a complex, progressive neurological disorder affecting up to 10 million people. And it is fast growing in prevalence worldwide.
April 11, the birthday of James Parkinson — who first described this syndrome in 1817 — kicks off World Parkinson’s Awareness Week.
The disease is most often diagnosed in people over 60, more often males. Classic symptoms include tremor in about 60 percent of cases, rigidity, poor posture and slow movement.
But several decades before diagnosis, subtler symptoms like sleep disturbances and loss of smell often appear together with constipation and erectile dysfunction.
This happens because clumps of alpha-synuclein protein are aggregating in the brain and autonomic nervous system, damaging dopaminergic cells governing motor control, among other functions. Loss of dopaminergic cells eventually causes the classic Parkinson’s symptoms.
Alpha-synuclein clumping can be triggered by aging, genetic mutations, conditions such as diabetes and hypertension, environmental toxins like pesticides and lifestyle factors like smoking, exercise, diet and mood.
Worldwide, about 10% of cases have a genetic basis. While Israel’s rate of Parkinson’s is no different than in other countries, the percentage caused by genetic mutations is much higher.
“Israel’s high rate of genetic Parkinson’s provides an opportunity to make Israel a global hub for research and development,” he says.
The dope on dopamine
Predicting Parkinson’s
Mental imagery
Parkinsons Disease Diagnoses Could Skyrocket Over Next 25 Years Due To Carcinogen Thats Common In Groundwater: Report
Trichloroethylene can be found in at least 30% of the U.S.’ groundwater, studies indicate.
Douglas Perry | The Oregonian/OregonLive
Parkinson’s disease diagnoses are dramatically on the rise in the U.S., and a neurologist who studies the degenerative condition says the increasing rates are “the tip of a very, very large iceberg.”
Dr. Ray Dorsey of the University of Rochester Medical Center told The Guardian newspaper that the number of Parkinson’s disease patients likely “will double” over the next 25 years.
The cause of Parkinson’s disease, which can impact a person’s motor function and cognitive ability, is often impossible to nail down, in part because onset can occur decades after related environmental exposure. But one of the common triggers is suspected to be exposure to the carcinogen trichloroethylene, which is used in dry-cleaning processes, pesticides, household cleaning wipes and paint removers, among other products.
“Pesticides have long been connected to incidence; however, it has become increasingly apparent that other industrial byproducts likely influence neurodegeneration,” states a new peer-reviewed article in the journal Neurobiology of Disease. “For example, organic solvents, which are used in chemical, machining, and dry-cleaning industries, are of growing concern, as decades of solvent use and their effluence into the environment has contaminated much of the world’s groundwater and soil.”
— Douglas Perry
Early Onset Dementia Is On The Rise: Heres Why And How To Protect Your Brain With Alzheimers Support
Most of us accept forgetfulness and memory loss as parts of the normal aging process. Although, you or a loved one may need Alzheimer’s support. What happens when changes in mood and memory begin to happen as early as your 30s or 40s?
Early onset dementia is a decline in cognitive function beginning early in life.It is becoming a reality for an increasing amount of younger people.
Today you’ll learn what early onset dementia is, what causes it, and what steps you can take today to protect the health of your brain.
Preventing Early Onset Dementia: Alzheimers Support Through Integrative Medicine
Cognitive health is driven by a diverse set of genetic, environmental, dietary, and lifestyle factors. Even though getting older is inevitable, the cognitive decline associated with aging is not.
Integrative medicine can help people living with a variety of conditions. We provide the tools to identify and address your risk factors for early onset dementia, and help you become proactive about Alzheimer’s and dementia prevention. For more information, visit our medical and wellness blog. Think of it as a virtual community of dementia care services.
If this article makes you think twice about your recent bouts of forgetfulness, learn about what we can do for you.
Schedule an appointment with CentreSpringMD to evaluate your cognitive risk, and optimize brain health. You can get home health care with our virtual visits. Get the Alzheimer’s support you deserve.
Study Examines Connection Between Diabetes Medication And Parkinsons Disease
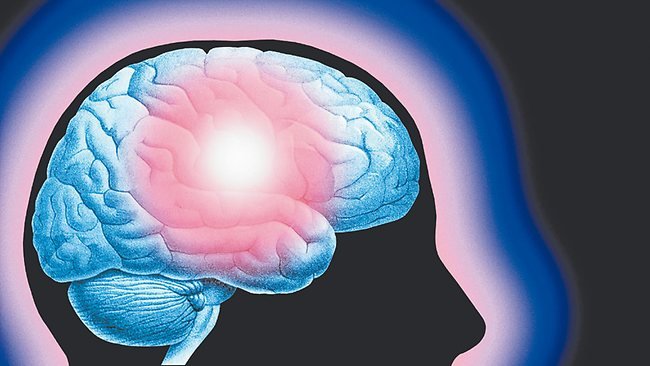
It was first suggested in the 1960’s that people with type-2 diabetes are at increased risk for developing Parkinson’s disease – and when they do develop PD, its progression is faster and often more severe. This may be due, in part, to an apparent relationship in the brain between dopamine, insulin resistance, and glucose control. Insulin is not only made in the pancreas, it’s also present in the brain – where it has been shown to impact dopamine levels.
Parkinson’s is generally believed by scientists to be caused by the loss of dopamine-producing neurons. Parkinson’s symptoms, such as slowness, rigidity, and tremor, typically develop after approximately 40-80% of these dopamine-producing neurons die.
Why does this matter? Currently, more than 30 million people in the United States have type-2 diabetes, and that number is growing. The lifetime risk of developing Parkinson’s is also on the rise. In light of these trends, it would be valuable to know whether any specific type-2 diabetes medications might be associated with an increased or decreased risk for developing PD.
1) Thiazolidinediones , like pioglitazone or rosiglitazone , which specifically target insulin resistance
2) Drugs, like albiglutide or dulaglutide , that mimick glucagon-like peptide-1 a hormone that promotes insulin secretion, and
3) Dipeptidyl peptidase 4 inhibitors, which increase GLP-1 levels, and lead to insulin secretion and lowering of blood sugar levels
Results
What Does This Mean?
Learn More
Rates Of Parkinsons Disease Are Exploding A Common Chemical May Be To Blame Adrienne Matei
Researchers believe a factor is a chemical used in drycleaning and household products such as shoe polishes and carpet cleaners in the US
Last modified on Thu 8 Apr 2021 14.06 BST
Asked about the future of Parkinson’s disease in the US, Dr Ray Dorsey says, “We’re on the tip of a very, very large iceberg.”
Dorsey, a neurologist at the University of Rochester Medical Center and author of Ending Parkinson’s Disease, believes a Parkinson’s epidemic is on the horizon. Parkinson’s is already the fastest-growing neurological disorder in the world; in the US, the number of people with Parkinson’s has increased 35% the last 10 years, says Dorsey, and “We think over the next 25 years it will double again.”
Most cases of Parkinson’s disease are considered idiopathic – they lack a clear cause. Yet researchers increasingly believe that one factor is environmental exposure to trichloroethylene , a chemical compound used in industrial degreasing, dry-cleaning and household products such as some shoe polishes and carpet cleaners.
To date, the clearest evidence around the risk of TCE to human health is derived from workers who are exposed to the chemical in the work-place. A 2008 peer-reviewed study in the Annals of Neurology, for example, found that TCE is “a risk factor for parkinsonism.” And a 2011 study echoed those results, finding “a six-fold increase in the risk of developing Parkinson’s in individuals exposed in the workplace to trichloroethylene .”
Parkinsons Disease On The Rise: The Fastest Growing Neurological Disorder
Parkinson’s Disease is one of the fastest growing conditions on the planet – to the extent that it’s been suggested that it will soon become a pandemic.
It’s reported that the number of people with the condition has doubled in the last 25 years, making it the world’s fastest growing neurological disorder.
Globally there are approximately 6.9 million people with Parkinson’s disease. It’s been predicted that by 2040, that number will increase to 14.2 million.
According to Parkinson’s Australia, 110,000 people may be living with Parkinson’s in Australia, with 32 new cases diagnosed every day.
Parkinson’s disease is even increasing at a faster rate than dementia and Alzheimer’s disease.
Professor Ray Dorsey, of the University of Rochester explained that “pandemics are usually equated with infectious diseases like Zika, influenza and HIV”.
“But neurological disorders are now the leading cause of disability in the world, and the fastest growing is Parkinson’s disease”.
Professor Dorsey co-authored the Global Burden of Disease study which found that neurological disorders are now the leading source of disability globally – and they show no signs of slowing down.
It’s been reported that up to 40 per cent of people with Parkinson’s disease in both the US and Europe don’t see a neurologist – highlighting the need for more awareness and accessible support.
Mayo Clinic Study Shows Increase In Parkinsons Disease Over 30 Years
ROCHESTER, Minn. — The incidence of Parkinson’s disease and parkinsonism increased significantly in 30 years from 1976 to 2005, Mayo Clinic researchers reported today in a study in JAMA Neurology. This trend was noted in particular for men age 70 and older. According to the researchers, this is the first study to suggest such an increasing trend.
The study shows that men of all ages had a 17 percent higher risk of developing parkinsonism and 24 percent higher risk of developing Parkinson’s disease for every 10 calendar years. The study also showed that men 70 and older had an even greater increase — a 24 percent higher risk of developing parkinsonism and 35 percent higher risk of developing Parkinson’s disease for every 10 calendar years.
Using the Rochester Epidemiology Project, Mayo Clinic researchers were able to look at the complete medical records — from birth to death — of anyone in Olmsted County, Minnesota, who received at least one of the diagnoses related to parkinsonism. The records were reviewed by a movement disorders specialist to confirm the diagnosis and to classify different types of parkinsonism, including the most common type, Parkinson’s disease.
The researchers point to environmental and lifestyle changes as potential causes for the increase.
MEDIA CONTACTSusan Barber Lindquist, Mayo Clinic Public Affairs, 507-284-5005, newsbureau@mayo.edu
Increase In Parkinsons Disease Cases Looming; What Pcps Need To Know

We were unable to process your request. Please try again later. If you continue to have this issue please contact customerservice@slackinc.com.Kelly Mills
The number of patients with Parkinson’s disease worldwide was 2.5 million in 1990 and jumped more than 100% in the 25 years since to an estimated 6.1 million in 2016, according to findings published in Lancet Neurology.
Some data suggest that number could top 12 million by 2040, and one model predicts as many as 17 million by 2040.
“By 2040, we can truly talk about a pandemic that will result in increased human suffering, as well as rocketing societal and medical costs,”PatrikBrundin, MD, PhD, of the Van Andel Research Institute in Grand Rapids, Michigan, said in a press release.
The toll the disease would take would not just be felt by patients, Ray Dorsey, MD, of the department of neurology and Center for Health and Technology, University of Rochester Medical Center, Rochester, N.Y., added.
“The strain of caregiving has adverse health consequences of its own. The economic costs of are also substantial, poised to grow,” Dorsey said.
While neurologists will be responsible for much of the diagnosis and initial management of the condition, much of the health care burden of long-term care and understanding how the condition affects a patient’s overall health will fall to primary care, and data suggest more education is needed.
“There are many other diseases related to Parkinson’s disease that can mimic it,” Mills agreed.
Parkinsons Disease Still On The Rise What This Means For Canadians Global News
The number of people affected by Parkinson’s disease has doubled in the last 25 years and is on track to double again by 2040, making it the fastest-growing neurological disorder in the world. More than 100,000 Canadians live with Parkinson’s and 25 more are diagnosed every day.
Parkinson’s is a brain disorder that causes difficulty in movement. People affected experience a decrease in dopamine, causing tremors, slow and rigid movements and a loss of balance.
Ray Dorsey, a professor of neurology at the University of Rochester and author of Ending Parkinson’s Disease, recently joined The Morning Show to discuss how Canadians can best protect themselves.
Read more: Larry Gifford — Parkinson’s disease is no barrier to joy in life
Dorsey says Parkinson’s is so prevalent that he considers it a pandemic.
The Mayo Clinic says that the exact cause of Parkinson’s disease is unknown, but several factors appear to play a role, including genes and environmental triggers — but the latter is a relatively small risk. Still, over the last decade, several studies have found a connection between Parkinson’s disease and pesticide/chemical exposure.
In this country, Parkinson’s affects one in every 500 people, and Canada has the highest rate of Parkinson’s in the world.
Dorsey says the reasons for the disease’s rapid growth are unknown.
“But if you look at the environmental risk factors that are tied to Parkinson’s disease, they are common in Canada.”
Studies Show Rise In Anxiety For People Battling Parkinsons Disease
Research shows increase in anxiety for those with PD amid pandemic.
RENO, Nev. – April is Parkinson’s Disease awareness month and its been challenging for those living with the disease. According to the American Parkinson Disease Association studies have shown the coronavirus pandemic has been tough for people with PD.
“There has been increases in anxiety, depression, and generally in isolation, and so there’s been a lot of effects of the entire situation with people with PD,” said ADPA Chief Scientific Officer Dr. Rebecca Gilbert.
She said in Nevada about 10,000 people have the neurodegenerative disorder. Dr. Gilbert explained that’s when nerves in the brain die which could lead to different symptoms, most commonly tremors.
ADPA said the study “Incidence of Anxiety in Parkinson’s Disease During the Coronavirus Disease Pandemic” shows 20% of patients polled felt the pandemic has exacerbated their symptoms. It also shows 12% increased their medication use during the pandemic.
According to ADPA another study of the impact of the COVID-19 lockdown on PD patients was conducted. Patients from the movement disorders clinic were assessed over the phone. The study demonstrated, compared to controls, PD patients had significantly increased levels of stress, depression and anxiety along with decreased measures of quality of life, as compared to controls. It also shows PD patients also reported a significant decline in physical activity as compared to pre-lockdown.
Most Read
Parkinsons Disease Is On The Rise In Every Region Of The Planet
The global burden of Parkinson’s disease is increasing over time due to the increasing numbers of older people.
Neurological disorders are the leading source of disability globally, and ageing in the general population is increasing the burden of neurodegenerative disorders, including Parkinson’s disease .
PD is a progressive chronic neurodegenerative disorder and is characterised by the progressive loss of muscular control leading to resting tremor, rigidity, akinesia and postural reflex impairment.
Why Are Cases Of Early Onset Dementia And Alzheimers Increasing

In the U.S., it’s estimated that about 200,000 people have early onset dementia, either early-, middle- or late-stage dementia. Alzheimer’s diagnosis rates increased 200% between 2013 and 2017 in people aged 30 to 64. This resulted in the average age of 49 in someone living with the early onset of this neurodegenerative condition .
Early onset dementia is a difficult road because many patients often have families to provide for, and are frequently caregivers themselves to someone living with chronic illness. Alzheimer’s and dementia also disproportionately impact women more so than men. It’s clear that proper Alzheimer’s support can help anyone cope with these difficulties.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinson’s disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didn’t exercise or didn’t start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinson’s, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments — whether medicines or deep brain stimulation — are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Improve the quality of your sleep.
Alzheimers Incidence Is Rising Not Falling A Researcher Says
11 Apr 2018
In the last few years, numerous studies have reported that dementia incidence is falling in the developed world. The drop in new cases has been attributed to better public health, in particular improved blood pressure control, but this conclusion may not tell the whole story. At the first Advances in Alzheimer’s and Parkinson’s Therapies Focus Meeting , held March 15–18 in Turin, Italy, Walter Rocca of the Mayo Clinic in Rochester, Minnesota, summarized recent research from his group and others that suggests the incidence of neurodegenerative diseases such as Parkinson’s, amyotrophic lateral sclerosis, and early onset Alzheimer’s is going up, not down. The reasons are unclear but could be environmental factors. Rocca argued this trend may extend to late-onset AD as well. He attributed the drop in all-cause dementia in recent decades to fewer cases of vascular dementia and stroke, which he thinks could be masking an increase in pure AD pathology.
- The incidence of PD, ALS, and early onset AD appears to be rising.
- The incidence of late-onset AD may be rising too.
- The drop in all-cause dementia is due to vascular health improvements.
“The dementia developing de novo in this group is very different in causes and manifestations from dementias with earlier onset,” Rocca noted. “This important work supports the hypothesis that improvements in cardiovascular health may be a major hope for the prevention of dementia.”
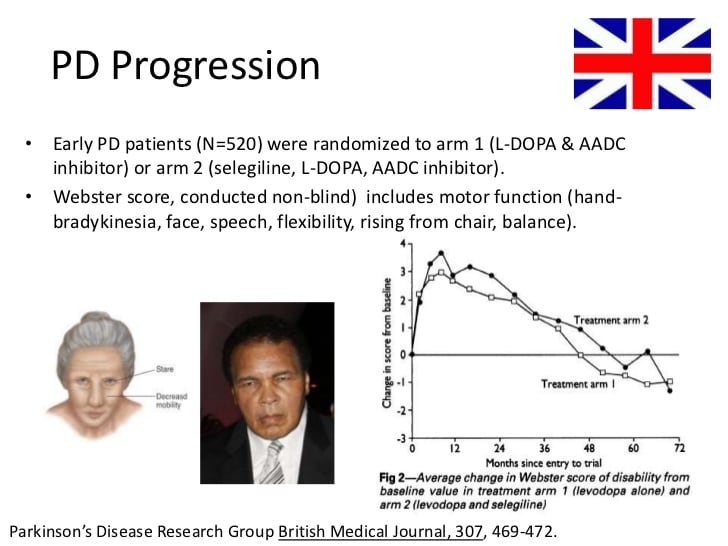
Parkinson’s Diagnoses Set To Increase By A Fifth By 2025
The number of people diagnosed and living with Parkinson’s is increasing, according to our latest research.
We estimate that in 2018 around 145,000 people in the UK are diagnosed with the condition – that’s around 1 in 350 adults in the UK. And Parkinson’s diagnoses are set to rise by nearly a fifth by 2025.
What Are The Surgical Treatments For Parkinsons Disease

Most patients with Parkinson’s disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable – reducing symptoms during “on” periods and no longer controlling symptoms during “off” periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they can’t. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinson’s disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare team’s efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinson’s disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein – glial cell-line derived neurotrophic factor, GDNF – to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Is Paraquat To Blame For The Rise In Parkinsons Disease
08/12/2021
What is Parkinson’s disease?
Parkinson’s disease is a chronic and progressive neurodegenerative disorder impacting approximately one million Americans. The nervous system disease affects predominately dopamine-producing neurons in a specific area of the brain, disturbing movement. There is no single test or scan to detect PD. Although the disease exposes itself in five common stages, and with each stage that develops, the progression of the disease is more evident.
Stage One: The individual has mild symptoms that typically does not interfere with their day-to-day life. Tremor and other movement difficulties are present on one side of the body and may be accompanied with changes in posture, walking and facial expressions.
Stage Two: Symptoms begin to progress as tremor, rigidity and other movement struggles arise on both sides of the body. Walking problems and poor posture may also be present.
Stage Three: Loss of balance, slowness of movements, and a higher fall-risk mark the mid-stage of PD progression. Although the affected person is fully independent, they may have difficulties with everyday activities like changing and eating.
Stage Four: At this stage, the individual is limited by the severity of their symptoms such as inability to walk without assistance and necessary help with daily living.
Financial and Emotional Cost of Parkinson’s Disease
How Does Paraquat Cause Parkinson’s Disease?
Rise in Parkinson’s Disease and Paraquat Use
The Link Between Parkinsons Disease And Toxic Chemicals
A new book calls the increasing prominence of Parkinson’s “a man-made pandemic.”
Michael Richard Clifford, a 66-year-old retired astronaut living in Cary, N.C., learned before his third spaceflight that he had Parkinson’s disease. He was only 44 and in excellent health at the time, and had no family history of this disabling neurological disorder.
What he did have was years of exposure to numerous toxic chemicals, several of which have since been shown in animal studies to cause the kind of brain damage and symptoms that afflict people with Parkinson’s.
As a youngster, Mr. Clifford said, he worked in a gas station using degreasers to clean car engines. He also worked on a farm where he used pesticides and in fields where DDT was sprayed. Then, as an aviator, he cleaned engines readying them for test flights. But at none of these jobs was he protected from exposure to hazardous chemicals that are readily inhaled or absorbed through the skin.
Now Mr. Clifford, a lifelong nonsmoker, believes that his close contact with these various substances explains why he developed Parkinson’s disease at such a young age. Several of the chemicals have strong links to Parkinson’s, and a growing body of evidence suggests that exposure to them may very well account for the dramatic rise in the diagnosis of Parkinson’s in recent decades.
Sometimes, though, the links are so strong and the evidence so compelling that there can be little doubt that one causes the other.
What Medications Are Used To Treat Parkinsons Disease
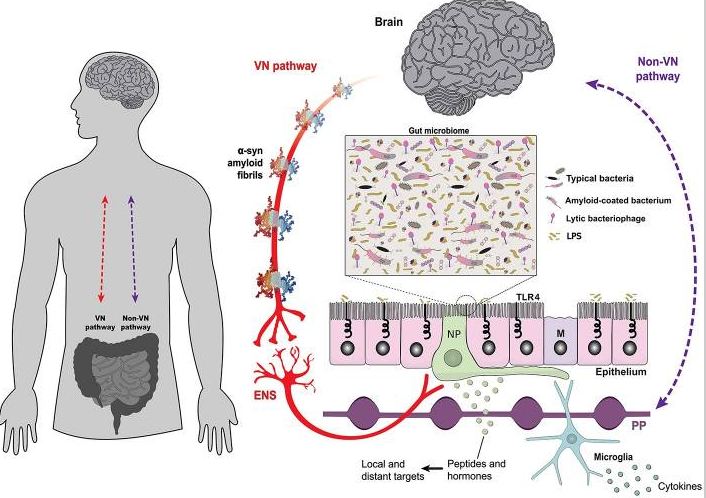
Medications are the main treatment method for patients with Parkinson’s disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinson’s disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinson’s disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinson’s disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinson’s disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinson’s disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinson’s disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms; others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinson’s disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
The Impact Of Parkinsons Disease On Overall Health
Based on the Blue Cross Blue Shield Health Index, the overall health of those affected by Parkinson’s is significantly lower than the general population. In 2017, the average BCBS Health Index for someone aged 30-64 with Parkinson’s was 57, compared to 88 for the entire commercially insured population in this age range. This translates to an average of 10.7 years of healthy life lost for those with the condition compared to 3.4 years for the 30-64 population as a whole.4
Caring for someone with Parkinson’s Disease
The majority of Parkinson’s patients are cared for by informal caregivers, such as a family member. The physical, mental and emotional work this requires can be significant. The Impact of Caregiving on Mental and Physical Health found that caregivers have 26% poorer health compared to a benchmark population, as measured by the BCBS Health Index. In addition, a national survey conducted by the Blue Cross Blue Shield Association found that 1 in 4 unpaid caregivers are feeling more stress trying to balance work and family due to COVID-19.5
Diagnosis And Management Of Parkinsons Disease
There are no diagnostic tests for Parkinson’s. X-rays, scans and blood tests may be used to rule out other conditions. For this reason, getting a diagnosis of Parkinson’s may take some time.
No two people with Parkinson’s disease will have exactly the same symptoms or treatment. Your doctor or neurologist can help you decide which treatments to use.
People can manage their Parkinson’s disease symptoms through:
- seeing a Doctor who specialises in Parkinson’s
- medication
- multidisciplinary therapy provided for example, by nurses, allied health professionals and counsellors
- deep brain stimulation surgery .
Medications For People With Parkinsons Disease
Symptoms of Parkinson’s disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinson’s medications fit into one of the following broad categories:
- levodopa – dopamine replacement therapy
- dopamine agonists – mimic the action of dopamine
- COMT inhibitors – used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics – block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine – has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors – prevent the metabolism of dopamine within the brain.
How Many People Does Parkinsons Disease Affect
Parkinson’s disease affects 1 in every 500 people in Canada. Over 100,000 Canadians are living with Parkinson’s today and approximately 6,600 new cases of PD are diagnosed each year in Canada . Most are diagnosed over the age of 60; however, at least 10% of the Parkinson’s population develops symptoms before the age of 50. Approximately four million people worldwide are living with the condition.
The Hidden Link Between Parkinsons And Autism
The Hidden Link Between Parkinson’s and Autism
Nieske Zabriskie, ND
Autism and Parkinson’s disease are two seemingly unrelated conditions. Yet, they are tied together by a common denominator—glutathione deficiency.
Glutathione deficiency has been associated with several neurological and degenerative diseases. Glutathione is a potent antioxidant that has been shown to decrease with age, and these diminished levels manifest in increased oxidative stress associated with neurological conditions such as Alzheimer’s disease, Parkinson’s disease, autism and Lou Gehrig’s disease .1
Glutathione is a molecule synthesized by the liver comprised of the amino acids glycine, cysteine and glutamate. Glutathione provides antioxidant activity protecting DNA and cell membranes from free radical damage, detoxifies external substances such as pharmaceuticals and environmental pollutants, and enhances immune function. Glutathione exists in the body in 2 forms: the reduced state and the oxidized, disulfide forms. Reduced glutathione reacts with and neutralizes free radicals, and in the process is converted into the oxidized form, which is no longer functional. Thus, sufficient levels of reduced glutathione are imperative to inhibit free radical damage.
Autism
Parkinson’s Disease
Liposomal Glutathione
References
1. Bains JS, Shaw CA. Neurodegenerative disorders in humans: the role of glutathione in oxidative stress-mediated neuronal death. Brain Res Brain Res Rev. 1997 Dec;25:335-58.
