Can The Parkinsons Disease Kill A Patient
Parkinsons disease is not really fatal in nature. However, the symptoms associated with Parkinsons disease is actually life threatening that may lead to fatal accidents. Injuries are quite common in Parkinsons disease due to inability to move around effortlessly. This is actually dangerous. Thus, efforts must be taken in order to create a safe environment for patients with Parkinsons disease.
Dont Miss: Light Therapy For Parkinsons
What Causes On/off Episodes In Parkinson’s Disease
On/off episodes, also known as off time, typically happen more often as Parkinson’s disease progresses, and levodopa becomes less effective.
Carbidopa/levodopa is considered the gold standard in Parkinson’s disease treatment, meaning it’s the most effective for treating motor symptoms, such as tremor, rigidity, and bradykinesia . Levodopa works by crossing the blood-brain barrier and converting into dopamine, low levels of which are believed to be the cause of Parkinson’s symptoms. Adding carbidopa to levodopa helps prevent levodopa from breaking down before it crosses into the brain, which helps reduce side effects like nausea and vomiting.
Some people who have Parkinsons start taking levodopa at around three doses per day. If you start experiencing off episodes, your doctor may increase your dose to four or more times per day.
Off time is common: According to patient surveys, around half of patients who take levodopa report experiencing wearing off periods. Of those patients, 25% experience it 3 to 6 hours per day, and 52% have symptoms for 1 to 3 hours a day.
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
Don’t Miss: Parkinson’s Disease Future Treatments
Patient Demographics Personal Circumstances Clinical Characteristics And Current Treatment
A total of 130 neurologists provided data for 722 patients who were receiving carbidopa/levodopa and had all data available required for the analyses. Patients ranged in age from 26 to 90years, and most were male , retired , and living with their spouse or partner . Slightly over half of the patients had a Hoehn and Yahr score of < 3, indicating mild PD, and only 13% had a Hoehn and Yahr score of 4 or 5, indicative of PD symptoms resulting in significant disability. Mean age at diagnosis was just over 60years, and the mean duration of PD was slightly over 4years but ranged to over 20years . In addition to carbidopa/levodopa, patients were also prescribed antiparkinsonian treatments from other pharmacologic classes, including dopamine agonists , catechol-O-methyl transferase inhibitors , monoamine oxidase type B inhibitors , and N-methyl-D-aspartate antagonists .
Table 1 Patient demographics, personal circumstances, clinical characteristics, and current treatment
Also Check: Gender Differences In Parkinsons Disease
Progression Of Parkinsons Disease

The disease progression of PD from diagnosis has been conceptualised into four stages . It is also important to recognise a prodromal phase in which non-motor symptoms, such as anosmia, constipation and rapid-eye-movement sleep behaviour disorder may predict the development of motor PD. Motor complications are more common as PD progresses, and typify transition to the complex phase. Many so-called axial symptoms of later stage PD, such as dysphagia, gait disturbance and falls, do not respond to levodopa, but may be helped by multidisciplinary team input. Dementia occurs in up to 80% of people with PD after 20 years disease duration. The rate of PD progression is heterogeneous and is generally more rapid in those with older age and more severe motor impairment at onset.
Stages of Parkinsons disease. RBD = rapid eye movement sleep behaviour disorder.
Recommended Reading: Can Alcohol Cause Parkinson’s
The Parkinsons Disease On
In Parkinsons disease, the ON-OFF phenomenon occurs when levodopa medication stops working effectively. As Parkinsons disease progresses, the brains levodopa plasma concentration decreases, causing levodopa medications to wear off temporarily and symptoms to return. OFF episodes are most common in patients who have been taking oral levodopa for 3-5 years.
OFF episodes are defined as a returning of Parkinsons symptoms such as tremor, rigidity, slow movement and memory problems. ON periods refer to the times when medicine works and your symptoms are well-controlled, typically just after a dose.
Not all OFF episodes are the same most people have fluctuating responses to levodopa. Whats more, everyone experiences Parkinsonian symptoms differently due to the bespoke nature of the disease.
Dont Miss: Pfnca Wellness Programs
What Causes Parkinsons Disease
Parkinsons disease occurs when nerve cells in an area of the brain called the substantia nigra become impaired or die. These cells normally produce dopamine, a chemical that helps the cells of the brain communicate . When these nerve cells become impaired or die, they produce less dopamine. Dopamine is especially important for the operation of another area of the brain called the basal ganglia. This area of the brain is responsible for organizing the brains commands for body movement. The loss of dopamine causes the movement symptoms seen in people with Parkinsons disease.
People with Parkinsons disease also lose another neurotransmitter called norepinephrine. This chemical is needed for proper functioning of the sympathetic nervous system. This system controls some of the bodys autonomic functions such as digestion, heart rate, blood pressure and breathing. Loss of norepinephrine causes some of the non-movement-related symptoms of Parkinsons disease.
Scientists arent sure what causes the neurons that produce these neurotransmitter chemicals to die.
Also Check: Service Dogs For Parkinsons
Recommended Reading: How Is Parkinson’s Tested
What Are The Early Warning Signs Of Parkinson’s Disease
Parkinsons warning signs can be motor symptoms like slow movements, tremors or stiffness. However, they can also be non-motor symptoms. Many of the possible non-motor symptoms can appear years or even decades ahead of motor symptoms. However, non-motor symptoms can also be vague, making it difficult to connect them to Parkinson’s disease.
Non-motor symptoms that might be early warning signs include:
Icipant Disposition And Baseline Characteristics
Of the 198 randomized participants across both double-blind trials,, 196 were included in the mITT population and their OFF time was analyzed. Of these, 102 participants had 2.5h of OFF time at baseline and 94 participants had < 2.5h of OFF time at baseline, 23 of whom had 0h OFF . Overall, 145 participants included in the mITT population of the pooled pivotal trial dataset transitioned to the extension trial and were included in the open-label analyses. Of these, 80 completed the open-label extension trial.
Fig. 1: Patient disposition.
*Completed double-blind trial or were active in EASE LID which was stopped early by the sponsor to accelerate data submission to the US Food and Drug Administration. All randomized patients had the opportunity to complete their week 12 trial visit . **An additional 78 patients were enrolled, n=17 who participated in a phase II dose-finding trial and later enrolled in EASE LID 2 after a gap in amantadine-DR/ER therapy, and n=61 who had DBS and did not participate in double-blind trials. *** Seven participants (n=3 who received placebo and n=4 who received amantadine-DR/ER in double-blind pivotal trials experienced a gap in treatment before entering the open-label trial. For purposes of these analyses we have included them with their original double-blind treatment groups.
Table 1 Baseline characteristics.
Recommended Reading: Does Parkinson’s Make You Shake
How To Manage Parkinsons Disease After It Is Diagnosed
Along with the medication so prescribed by the doctor, it is extremely important to bring some form of lifestyle changes in order to manage Parkinsons disease. They include-
Activity: As mentioned earlier Parkinsons disease affects the patients motor abilities, it is thus important to keep the body fit by indulging into exercise regularly. The patient may do any form of exercise which he may like every day to keep the body moving. This does not let the body parts to be stiff and also slows down the progression of the disease.
Additional Help: The caregivers and well-wishers should make attempts to make the environment safe for the patient with Parkinsons disease. Modifying the environment like installing grab bars in washroom and removing obstacles which may hamper movement of the patient is important.
Diet: Having nutritious food is important for patients with Parkinsons disease. It is seen to be beneficial to have right amount of nutrients in order to manage the symptoms of Parkinsons disease. The patient should also discuss with the doctor the food to avoid so that they do not interfere with the working of the medicines, especially levodopa.
Also Check: Computer Mouse For Parkinsons
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinsons disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable reducing symptoms during on periods and no longer controlling symptoms during off periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they cant. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
Recommended Reading: Cleveland Clinic Parkinsons Bicycle Study 2017
Recommended Reading: Is There Any Treatment For Parkinson’s Disease
Understanding Of Off Periods
Two studies addressed the understanding of off periods .1). A questionnairebased study of patients and their carepartners found that a large proportion of patients and carepartners indicated that they understood the concept of wearing off. On further questioning, however, 53% of patients and 36% of carepartners did not answer the question about the meaning of wearing off and 17% of patients and 47% of carepartners gave incorrect answers . In interviews conducted in Dutch nursing homes, lack of staff knowledge regarding motor fluctuations in PD, including the importance of timely administration of levodopa and avoidance of proteinrich meals at the time of ldopa intake to minimize off time was one of residents and caregivers main complaints. This lack of understanding was felt to contribute to a lack of empathy. We identified no studies investigating physician understanding.
What Are The Symptoms
The best-known symptoms of Parkinson’s disease involve loss of muscle control. However, experts now know that muscle control-related issues aren’t the only possible symptoms of Parkinson’s disease.
Motor-related symptoms
Motor symptoms which means movement-related symptoms of Parkinsons disease include the following:
Additional motor symptoms can include:
- Blinking less often than usual. This is also a symptom of reduced control of facial muscles.
- Cramped or small handwriting. Known as micrographia, this happens because of muscle control problems.
- Drooling. Another symptom that happens because of loss of facial muscle control.
- Mask-like facial expression. Known as hypomimia, this means facial expressions change very little or not at all.
- Trouble swallowing . This happens with reduced throat muscle control. It increases the risk of problems like pneumonia or choking.
- Unusually soft speaking voice . This happens because of reduced muscle control in the throat and chest.
Non-motor symptoms
Several symptoms are possible that aren’t connected to movement and muscle control. In years past, experts believed non-motor symptoms were risk factors for this disease when seen before motor symptoms. However, theres a growing amount of evidence that these symptoms can appear in the earliest stages of the disease. That means these symptoms might be warning signs that start years or even decades before motor symptoms.
Non-motor symptoms include:
Stages of Parkinsons disease
Also Check: Team Fox For Parkinson’s Research
Making The Most Of On Time
Although there are many approaches to managing off time, it often becomes harder to control motor fluctuations over time. Once you get a sense of when your off times are likely to occur possibly with the help of a motor symptom journal you can better plan your day. Take advantage of on times when symptoms are well-controlled to be active, and try to make sure “off” times happen at times when it matters less.
Each persons daily schedule will look different based on when off time occurs which may be as a dose of Parkinsons medication wears off, in the morning before the first dose, or while waiting for a dose to take effect. It may also depend on other medications you take, whether for Parkinsons or another medical condition.
As you make your schedule, take into account:
- Timing meals for best medication effectiveness
- Getting sunlight and physical activity early in the day if possible
- Minimizing drinking before bedtime to avoid needing to get up to urinate
- Taking any sedating medication later in the day, closer to bedtime
For some MyParkinsonsTeam members, the morning is peak on time. Best time for me is early in the morning, wrote one member. I clean house, do yoga, then have a big breakfast at about 6:30. Another shared, Walked three miles this morning. If I dont walk in the morning, by the afternoon Im spent! No energy!
What Are The Symptoms Of Wearing Off
Wearing off is very individual. In some people, motor symptoms such as tremor may be the first sign, whilst for others it might be stiffness and difficulty initiating movement. But wearing off symptoms may not be related to movement at all and may be experienced in the form of increased anxiety, fatigue, a change in mood, difficulty thinking, restlessness and sweating .
If you notice a change in your usual symptom pattern, you should discuss this with your doctor because you may be experiencing wearing off. Your doctor will then be able to adjust your medication regime to provide better symptom control, possibly by reducing the interval between the levodopa doses and increasing the number of daily doses.
Recommended Reading: Treatment Of Dysphagia In Parkinson’s Disease
Many Dont Manage Off Time Well
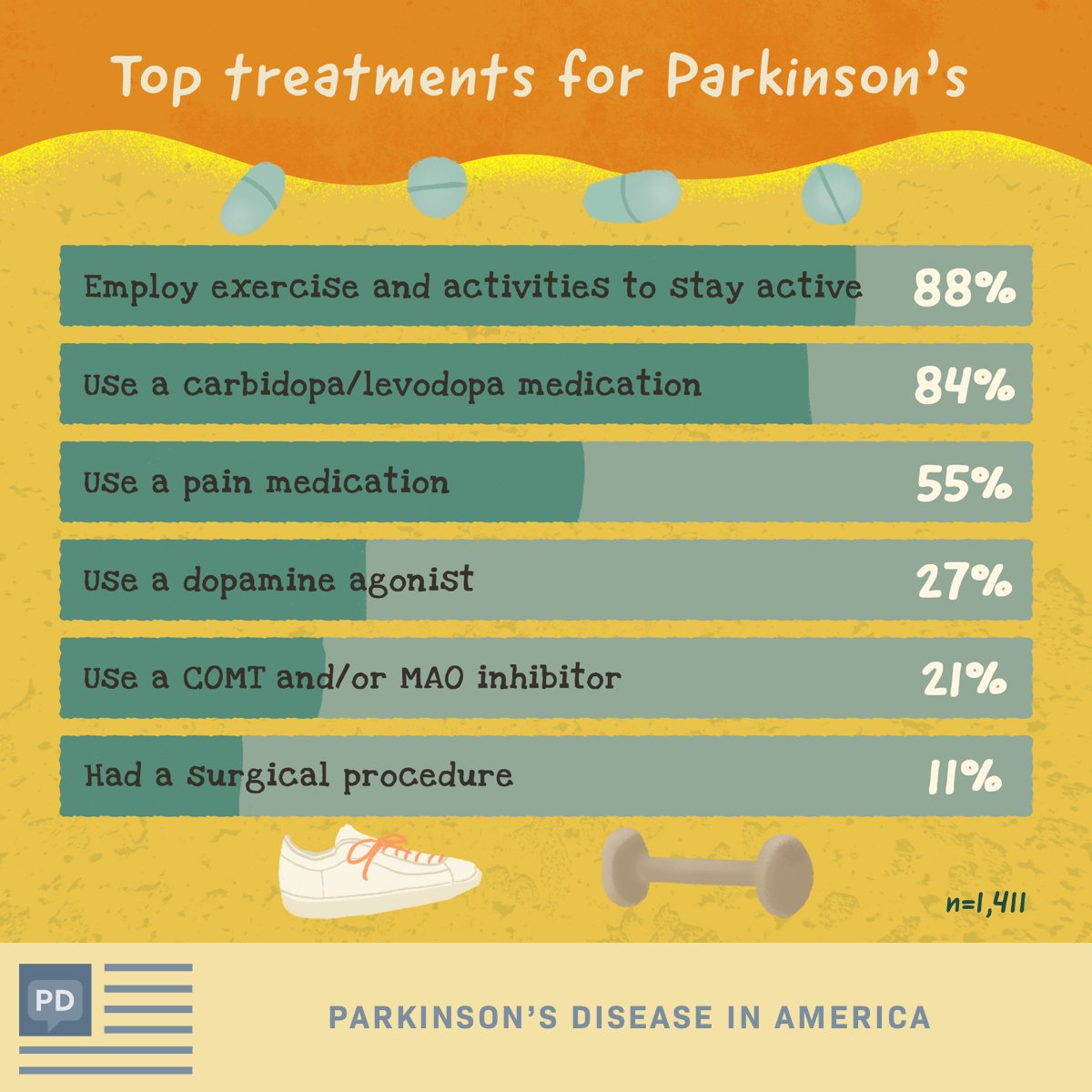
In the Parkinsons Disease in America 2017 survey, 80% of people with PD reported they currently use a carbidopa/levodopa therapy to treat their symptoms. Carbidopa/levodopa treatment is the most effective treatment available for the management of motor symptoms of PD.
However, half of the survey respondents who use carbidopa/levodopa therapy are experiencing off times. Twenty-five percent of those experiencing off times notice their symptoms for 3 to 6 hours a day.
Another 52% report 1 to 3 hours a day when their symptoms are noticeable and affecting their daily activities. Yet 43% of those experiencing an off time report that they dont take any action to manage these episodes.
Read Also: Celebrities With Parkinsons Disease
Do You Have An Off Story To Share
This post is the first in a series about what it means to be OFF. If you have a story about OFF and what youve done on your own and with your doctor that has helped you to minimize or navigate these periods, and youd like to share it with us, please send us an email at .
This post was written by the Davis Phinney Foundation.
This blog series is sponsored by Sunovion Pharmaceuticals Inc.
Also Check: How To Control Parkinson’s Disease
Q& A: Sublingual Apomorphine More Effective Than Levodopa For Parkinsons Off Episodes
Healio Interviews
Disclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact .
Apomorphine sublingual film resulted in greater motor improvement and an increase in responders at earlier time points compared with levodopa, according to results from a study of more than 300 patients with Parkinsons disease.
Researchers presented the findings, which were consistent with previous research and further support the use of apomorphine sublingual film in patients with PD who have a delayed response in on time to levodopa, at the American Academy of Neurology annual meeting, which was held virtually.
Researchers analyzed motor improvements with apomorphine sublingual film vs. levodopa in patients with PD experiencing off episodes, according to the presentation. The trial comprised 384 patients with comparable Movement Disorder Society Unified Parkinsons Disease Rating Scale Part III scores who received apomorphine sublingual film and levodopa.
Healio Neurology spoke with Jennifer S. Hui, MD, clinical associate professor of neurology at the University of Southern Californias Keck School of Medicine and director of the deep brain stimulation program at Keck Hospital, to learn more about the study results.
Healio Neurology: What prompted this research?
Healio Neurology: What does prior research demonstrate about the efficacy of apomorphine sublingual film?
Healio Neurology: What did the study results demonstrate?
What Does Dyskinesia Look Like
Levodopa-induced dyskinesia causes symptoms ranging from writhing or wriggling to dramatic rocking and head bobbing, from minor tics to full-body movements. Dyskinesia can also cause swaying, which can be embarrassing on its own and even more so when youre walking. Some people with dyskinesia fear others will think theyre intoxicated and, combined with other Parkinsons symptoms such as freezing of gait, rigidity, and balance problems, walking around in public can feel too vulnerable to do.
Read Also: Icd 10 Code Parkinson’s Disease
Screening Selection And Data Extraction
Identified publications were initially screened by title to remove duplicates and papers of a type not meeting with the PICOS eligibility criteria. Screening and data extraction were conducted independently by two reviewers . Results were matched between reviewers and discordance was resolved by consensus through a third reviewer .
Data on off-time at all reported timepoints were collected from each selected publication. Other available information that was extracted from the selected publications, where reported and at all reported timepoints, was: study characteristics , change from baseline in motor symptoms , change from baseline in motor complications , change from baseline in dyskinesia duration, change from baseline in motor experiences of daily living , change from baseline in QoL scores, change from baseline in non-motor symptoms and safety outcomes.
These data were extracted independently by both reviewers from selected publications using a standardised Microsoft Excel-based form. Extracted data were verified in the drafting of this manuscript by a third reviewer. As identified studies were not RCTs, the domains to address in a risk of bias assessment, according to the Cochrane Collaboration , were absent in most studies. Therefore, we did not draw a funnel plot or conduct a formal assessment of the risk of bias of included publications.
