The Critical Difference Between Sleepiness And Fatigue
Fatigue is a physical or psychological feeling where people feel weary and exhausted and lacking energy. EDS is about needing and having the urge to sleep.
Fatigue is something that people can experience along with EDS however, people who experience fatigue on its ownthe feeling of being tired and out of energy do not also necessarily fall asleep when sedentary, as people who experience EDS often do.
It is estimated that EDS affects up to 50% to 75% of people living with Parkinsons and fatigue is estimated to affect 40% to 60%. Fatigue, however, is more likely to go undiagnosed.
Because the terms fatigue and sleepiness are so heavily linked, and sometimes used interchangeably, research has concluded that fatigue and EDS should be assessed separately in people with Parkinsons so that we can improve our understanding of their overlapping physiology.
With that knowledge, researchers from the University Hospital of Zurich, Switzerland designed a study to determine the overlap between fatigue and EDS and then associate them with other motor and non-motor symptoms as well as dopaminergic medication.
In their study of 88 outpatients, the researchers found that 72% experienced fatigue or EDS and just under half experienced both. Some of the key findings of the study include:
Unified Parkinsons Disease Rating Scale
The Unified Parkinsons Disease Rating Scale has four parts. Each part has multiple points that are individually scored, using zero for normal or no problems, 1 for minimal problems, 2 for mild problems, 3 for moderate problems, and 4 for severe problems.
These scores are tallied to indicate the severity of the disease, with 199 points being the worst and total disability and 0 meaning no disability.3
In 2001, the Movement Disorder Society updated the rating scale with involvement from patients and caregivers. The updated scale is referred to as the UPDRS-MDS, and it was published in 2008. It now includes the following sections:3
Disabilities Secondary To Parkinsons Disease
While most people tend to think of Parkinsons disorder as a neurological movement disorder, and it most certainly is, many people do not realize that other systems in the body can also be severely affected by Parkinsons. Often, the same chemical exposure can also cause other disorders, such asischemic heart disease. However, often it is the Parkinsons itself, or the medication used to treat it that is the causal factor in the development of a new disorder. Whether a veterans Parkinsons was caused by exposure to the TCDD in agent orange, pesticides, trichloroethylene, or its origins are unknown, Parkinsons cause many secondary health effects and disabilities.
Read Also: What Happens With Parkinson’s
Progression Of Fatigue In Early Parkinsons Disease: A 3
- Laboratory of Neurodegenerative Disorders, Department of Neurology, National Clinical Research Center for Geriatrics, West China Hospital, Sichuan University, Chengdu, China
Objective: To explore the frequency, evolution, associated factors, and risk factors of fatigue over 3-year of prospective follow-up in a cohort of patients with early Parkinsons disease .
Methods: A total of 174 PD patients in the early stage were enrolled and quantitively assessed motor and non-motor symptoms using comprehensive scales including the Fatigue Severity Scale annually. Each subject was categorized as PD with and without fatigue based on a cut-off mean value of 4 using FSS. The generalized estimating equation was utilized to investigate the associated factors, and the stepwise binary logistic regression model was performed to explore the predictors.
Results: The frequency of fatigue was slightly changed during the 3-year follow-up. The changed pattern of the frequency of fatigue was similar to that of anxiety. Fatigue was significantly associated with nocturnal sleep disorders , high Hamilton Anxiety Rating Scale score , and high Unified PD Rating Scale III score over time. High UPDRS III score at baseline increased the risk of developing fatigue after 1-year high LEDD increased the risk of developing fatigue after 2-year and high LEDD and high HAMA score increased the risk of developing fatigue after 3-year.
Insights Into Fatigue From Other Disorders
Although perceived fatigue is probably similar among different illnesses, there may be disease-specific differences. Both similarities and differences may provide insights into fatigue pathophysiology. Similarities in fatigue would be compatible with a hypothesis of shared mechanisms, and thus the possibility of similar interventions. The high prevalence of fatigue in medical and psychiatric disorders points either to some very generalized mechanisms or a limitation in the brains ability to distinguish perceptions. We limited our review of other disorders with prominent fatigue, but excluded chronic fatigue syndrome because of its frequent association with psychiatric disorders such as personality disorders and post-traumatic stress disorder that might confound physiological interpretations.
Also Check: How To Manage Adrenal Fatigue
Recommended Reading: Which Part Of The Brain Is Affected By Parkinson’s Disease
Physiology And Biomarkers For Fatigue In Pd
The physiology underlying fatigue symptoms in PD is unknown, whereas much is known about the mechanisms of motor fatigability. The only published study of physiological differences between fatigued and nonfatigued PD patients found no measurable differences in oxygen utilization during exercise, but some studies have suggested that exercising improves fatigue.,,, Whether fatigue fluctuates with motor fluctuations was looked at in one study. Subjects were assessed during their off, whereas all other studies used the subjects experience over a preceding time interval of weeks. Eighty-eight percent of their subjects were fatigued, and fatigue increased with motor ”off.” Too few subjects were nonfatigued to determine how often fatigue occurred only during motor ”off.” The physiological implications are unclear, as many other nonmotor symptoms also increased during the ”off” period.
Diagnosis And Treatment Of Parkinsons Sleep Problems
Parkinsons disease is chronic and progressive, meaning it tends to get worse over time. However, there are treatment options that can help manage symptoms and allow patients to get more restful sleep.
The simplest way to start sleeping better with Parkinsons disease is by adopting healthy sleep habits. Sleep hygiene tips for Parkinsons disease sufferers include:
- Sticking to regular bedtimes
- Following a consistent bedtime routine with soothing activities such as listening to music or reading a calming book
- Getting regular exercise, preferably early in the day
- Getting adequate exposure to light, whether outdoors or through light therapy
- Avoiding long naps and naps late in the day
- Creating a cool, dark, and comfortable sleeping environment
- Restricting bedtime activities to sex and sleep only
- Turning off screens an hour before bedtime
- Reducing liquid intake before bedtime
- Avoiding caffeine, alcohol, and tobacco
- Eating a healthy diet and avoiding large meals at night
Light therapy, exercise, and deep brain stimulation have been successfully used to improve overall sleep quality and to treat specific conditions, such as REM sleep behavior disorder, in patients with Parkinsons disease. Cognitive behavioral therapy for insomnia has proven effective at reducing insomnia in healthy adults, although further research is needed on the effects of CBT in patients with Parkinsons disease.
- Was this article helpful?
Also Check: How Many Stages Of Parkinson’s Are There
The Parkinsons Disease News Today Forums Are A Place To Connect With Other Patients Share Tips And Talk About The Latest Research Check Them Out Today
The study involved 22 Parkinsons patients , and 15 age-matched individuals , who were, in most cases, the spouses or caregivers of the Parkinsons patients.
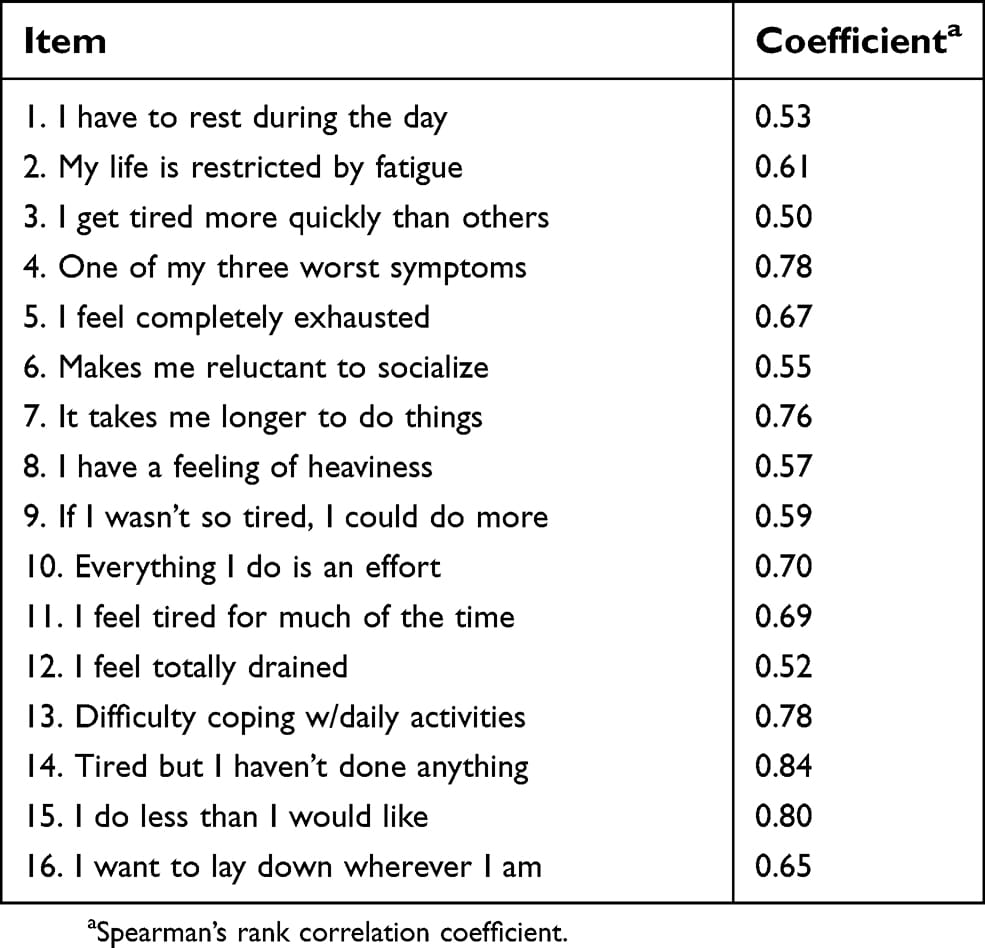
All participants completed four scales: the Fatigue Severity Scale , the Functional Assessment of Chronic Illness Therapy-Fatigue Scale , the Parkinson Fatigue Scale , and the Fatigue Visual Analog Scale .
Parkinsons patients were also asked to list their top three most bothersome Parkinsons symptoms, and to complete 13 quality of life-related measures, including cognition, sleep, depression, life orientation, physical activity, and Parkinsons symptoms.
The scores from the four scales showed that Parkinsons patients experienced much more fatigue than their spouses/caregivers. Many of the patients had excessive and unusual fatigue, and six included fatigue in their top three most bothersome symptoms.
The results of the Fatigue Severity Scale, Parkinson Fatigue Scale, and Visual Analogue Fatigue Scale were highly consistent, and could predict with elevated certainty if the results were from Parkinsons patients or from spouses/caregivers.
Among them, the Visual Analogue Fatigue Scale was the most reliable tool, and patients who rated their fatigue as lower than5.5 were found to be three times more likely to have excessive fatigue.
Measurement Of Fatigue And Balance
A randomized crossover design examined each participant twice, once in a fatigued condition and once in a non-fatigued condition. The Visual Analog Scale of Fatigue measured subjective fatigue. The VASF is a quick self-report measure used to quantify subjective perceptions of fatigue during a particular task by marking a 100mm line with 0mm representing no fatigue and 100mm representing maximum fatigue. One can calculate immediate effect of a task on subjective fatigue by subtracting the immediate pre-test measure from the immediate post-test measure designated by each research participant. This ability to measure immediate effects of a task makes the VASF a better option than other self-report measures like the PFS-16 which measure the generalized state of fatigue specifically with persons with PD. Although it has not been studied in PD, the VASF has been found to be more sensitive than other self-report fatigue measures for measuring fatigue in other neurodegenerative diseases .
Balance was measured with MBT, a 14-item test that measures balance in 4 domains: anticipatory balance, reactive postural control, sensory orientation, and dynamic gait. Its validity and reliability in PD has been established .
Read Also: What Are The Initial Symptoms Of Parkinsons Disease
Read Also: When Was Billy Graham Diagnosed With Parkinson’s
Who Are We Who Sees Your Information
We are an independent, venture-capital backed startup based in San Francisco, working hard on a mission we love. All of the features on the site are designed with one goal in mind to connect you with others who have been in your shoes. Today with millions of members, millions of conversations, and a presence in eight countries, MyHealthTeam has become the fastest growing and most engaging set of social networks for web and mobile apps in healthcare.
MyParkinsonsTeam should not only provide you emotional support through the social network, but also be a resource for practical tips, personal experiences, and even referrals to other great doctors from the community. Information shared on the site can be seen by everyone who signs up for an account. You can share as much or as little as you like.
If you ever have any concerns or questions, we can always be reached at support@myparkinsonsteam.com.
Predictors Of Fatigue In Parkinsons Disease
The predictors for fatigue in PD are presented in Table 3. In the three multivariate models, all the VIF for each variable was less than 5. High UPDRS III score increased the risk of developing fatigue after 1-year high LEDD increased the risk of developing fatigue after 2-year and high LEDD and high HAMA score increased the risk of developing fatigue after 3-year.
Table 3. Predicted factors for the development of fatigue in patients with PD.
You May Like: How To Increase Dopamine In Parkinson’s
Why Does Pd Lead To Fatigue
PD damages certain areas throughout the brain. The nerve cells in the heavily damaged area make dopamine, which is a chemical messenger . Dopamine sends signals to parts of the brain that help make the muscles and nerves work together for smooth movement.3
Doctors have found that low levels of dopamine in PD lead to fatigue. However, many different things can lead to fatigue. When talking to your doctor, they will first work to find out the cause of the problem. It is often PD itself. However, other things besides your disease could be causing your symptoms. Treatment for fatigue will depend on the underlying cause.3,4
Figuring Out Causes Of Fatigue
The first step in easing the fatigue associated with Parkinsons disease is to rule out other causes of tiredness, says Liana Rosenthal, M.D., assistant professor of neurology at the Johns Hopkins University School of Medicine and director of clinical core at the Morris K. Udall Center Parkinsons Disease Research Center of Excellence. We evaluate patients to see if there are other things contributing to the fatigue besides their disease, she says.
Sometimes patients may be referred to a sleep specialist for an evaluation. That can help identify causes of tiredness, like sleep apnea. Rosenthal says: Our aim is to first treat any sleep issues, like insomnia, sleep apnea or other causes of poor sleep. Once we treat and address those issues, we can see if fatigue still persists.
You May Like: New Diagnostic Test For Parkinson Disease
Causes Of Fatigue In Parkinsons Disease
Many of the symptoms of PD, including slow movement, muscle stiffness, depression, and changes to sleep quality can cause or worsen the symptom of fatigue.
- Akinesia Fatigue may be caused by akinesia . People experiencing akinesia find it challenging to accomplish simple tasks, requiring significantly more energy to get through the daily activities.
- Muscle fatigue Many of the symptoms of PD that affect the muscles, like stiffness, cramping, tremor, and difficulty starting movement, put extra stress on the muscles, causing fatigue. In addition, some people with PD experience muscle atrophy, in which the muscles shrink and weaken due to lack of use. Muscle atrophy decreases a persons stamina and endurance, contributing to the sense of fatigue.
- Depression Depression is another common non-motor symptom of PD, occurring in approximately 40% of people with PD. Depression can cause fatigue, adding to a sense of low energy or lack of motivation.
- Sleep disturbance PD often causes changes in sleep cycles, which can add to a sense of fatigue during the day.
- Medications Some of the medications used to treat PD, including dopamine agonists, can cause fatigue as a side effect. Others may cause insomnia as a side effect, leading to daytime fatigue.1,2
Recommended Reading: High Blood Pressure Back Pain Fatigue
Managing Fatigue And Parkinsons Disease
If you are living with Parkinsons disease , you might often feel run down, out of energy, or even a bone-deep kind of tired that isnt relieved with rest. Those feelings of intense tiredness are known as fatigue a symptom that affects at least 50 percent of those with Parkinsons.
Many MyParkinsonsTeam members experience fatigue. I didnt know it was caused by PD. I just thought I was getting lazy, said one self-proclaimed chronic napper.
Im getting a better understanding of fatigue reading other PD patients stories and knowing Im more normal than I thought, wrote another member, relieved.
You May Like: When Did Michael J Fox Get Parkinson’s Disease
Common Causes Of Dizziness And Vertigo In Parkinsons And How To Treat Them:
In people with early Parkinsons disease , the dizziness has in many cases linked to a lower Montreal Cognitive Assessment score raising the possibility that dizziness may be a non-movement symptom associated with cognitive decline .
Dizziness or vertigo can be tied to many causes and is not unique to Parkinsons. Symptoms can be caused by medications, low blood pressure, anxiety, cold, flu, dehydration, heart conditions and more. Tell your doctor immediately if you regularly experience dizziness or vertigo.
Page reviewed by Dr. Michael S. Okun, Parkinsons Foundation Medical Director, Professor and Chair, Department of Neurology, Executive Director of the Fixel Institute for Neurological Diseases a Parkinsons Foundation Center of Excellence.
What Causes Fatigue In People Living With Parkinsons Disease
There exists many causes that interact with one another and are responsible for fatigue. Some of these causes can be treated and others cannot:
- The decrease in neurotransmitters associated with Parkinsons disease. The levels of dopamine and serotonin, which usually regulate movement and mood, decrease as neurons disappear.
- Medications to treat conditions such as insomnia, anxiety, muscle pain and spasms, as well as allergies.
- Medications taken to control the motor symptoms of the disease.
- Low blood pressure or orthostatic hypotension which are characteristics of Parkinsons disease and which are aggravated by antiparkinsonian drugs.
- Involuntary muscle contractions , slow movements , muscle stiffness and tremors.
- Lack of exercise which can fuel the vicious cycle of low energy.
Mental fatigue can also be exacerbated by difficulty concentrating, memorizing, or performing cognitive tasks.
People living with Parkinsons disease often use these phrases to describe their fatigue:
- I have no energy
- I am unable to do anything
- I am not able to motivate myself
- I feel overwhelmed
Out of the many medical conditions, lack of sleep and aging can be the cause of fatigue. In general, the fatigue associated with Parkinsons disease improves with antiparkinsonian treatments, but does not go away completely.
Your neurologist can help you determine the cause of your fatigue and eventually find the best treatment.
Read Also: Can Stress Cause Headaches And Fatigue
Also Check: What Are The Non Motor Symptoms Of Parkinson’s Disease
Effects Of Vestibular Rehabilitation On Fatigue And Activities Of Daily Living In People With Parkinsons Disease: A Pilot Randomized Controlled Trial Study
Mohammad-Reza Hadian
Abstract
One of the most disabling nonmotor symptoms in persons with Parkinsons disease is fatigue, which can decrease the quality of life by restricting the function and activities of daily living . Nonetheless, sufficient evidence for treating fatigue, including drug or nondrug treatment, is not available. In this study, we evaluated the probable effects of vestibular rehabilitation on fatigue and ADL in patients with Parkinsons disease. Methods. This was a single-blind clinical trial study in which patients with Parkinsons disease voluntarily participated based on the inclusion and exclusion criteria. The patients were randomly assigned to the case and control groups. The case group received 24 sessions of vestibular rehabilitation protocol, and conventional rehabilitation was performed in the control group . Both groups were also given fatigue management advice. Fatigue was measured by the Parkinson Fatigue Scale and the Modified Fatigue Impact Scale . ADL was measured by the Functional Independence Measure . All changes were measured from the baseline at the completion of the intervention. Results. Both fatigue and ADL improved significantly more in the vestibular intervention group than in the control one. . Vestibular rehabilitation may improve fatigue and ADL and therefore can be used as an effective intervention for patients with Parkinsons disease, which was also found to be well tolerated.
1. Introduction
