Pool Therapy For Multiple Sclerosis Patients
Multiple Sclerosis is a condition that weakens muscles and movements over time. Thus, strength training early and often is one of the key ways to keeping the muscles from weakening. However, this can be understandably difficult for someone who has difficulty walking, picking up a fork to eat or simply waving hello. For Multiple Sclerosis sufferers, the HydroWorx therapy pool can be a place for them to more easily build lean muscle mass than would ever be possible on land. Even if they cannot walk down the street comfortably or safely, they can walk on a treadmill in the water without fear. Not only are they protected by the innate buoyancy of the water, but they are given a psychological boost because they arent afraid to fall.
In a case study that was recently done in Great Britain, a woman with Multiple Sclerosis was treated in the HydroWorx pool. She had complained of progressive weakness in her upper and lower left limbs during a two-year period. She had to walk with a cane, and tended to favor one of her legs over the other. This was causing serious gait problems.
Limitations For Further Research
The level of research is only preliminary, but studies are suggesting great potential for Ibogaine in the treatment of neuroinflammatory and neurodegenerative disorders, including Parkinsons
Unfortunately, there are multiple limitations for future research on Ibogaine and its effect on these debilitating conditions. In the US, Ibogaine is classified as a Schedule I substance, which makes it illegal for use or possession. It is also banned in Australia and many European countries.
That is mainly because of the safety concerns with high dose Ibogaine use. The use of Ibogaine without medical supervision can be dangerous for people with preexisting cardiovascular conditions or those taking prescription medications.
However, Ibogaine can be used safely by patients who dont have cardiovascular problems, prepare for the therapy and taper off their medications properly. All of these factors should be carefully evaluated and overseen by a team of experienced medical professionals. Ibogaine therapy is legal in Canada, Mexico, and New Zealand and currently, it is used successfully for the treatment of patients with addictions.
Clinical Features And Autoimmunity In Pd
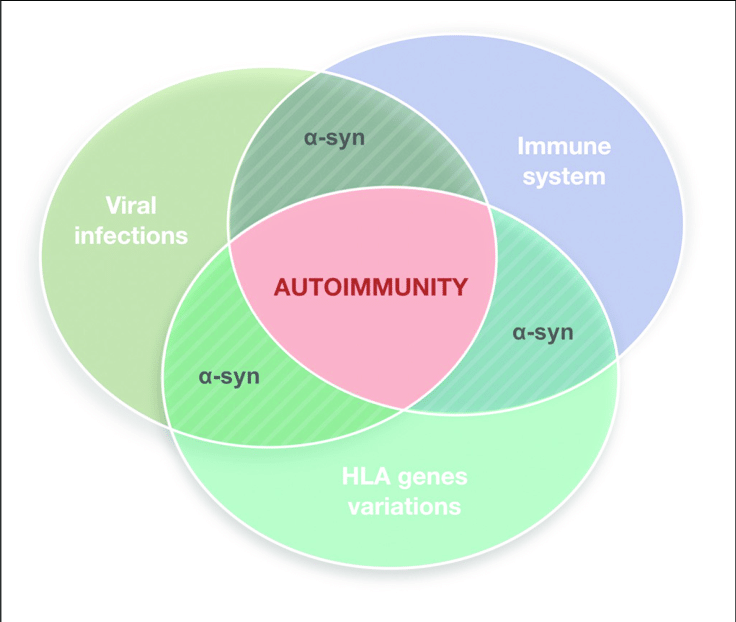
-Synuclein participates in autoimmunity and is involved in the pathological progression of PD. -Syn, as the main disease-causing protein, first appears in the gut and is related to gut dysbiosis, which disturbs the intestinal immune system, leading to one of the main non-motor symptoms of PD: constipation. Then, this protein transmits to the dorsal motor nucleus through the vagus nerve and acts as a self-antigen targeted by effector T cells, B cells, and microglia. This autoimmunity attack finally results in the damage and death of DNs. SIBO, small intestinal bacterial overgrowth.
Also Check: Parkinson’s Disease Awareness Color
Investigating Parkinsons As An Autoimmune Disease
At the University of Montreal, Professor Louis-Eric Trudeau investigates the earliest potential causes of Parkinsons disease, at the cellular level. His project is funded by the Saucier-van Berkom Parkinson Quebec Research Fund with contributions from Parkinson Newfoundland & Labrador, in the amount of $49,748.00 for 1 year. He is exploring the possibility that Parkinsons is a form of autoimmune disease, caused when the immune system attacks the axon terminals in our brain cells. Those extremities release the chemical messengers that communicate with other cells, and damage to such terminals may disrupt the dopamine-producing brain cells that are key to Parkinsons.;
The death of the brain cells that produce dopamine, the chemical messenger that signals other cells involved in motor control, triggers the symptoms of Parkinsons disease. But researchers still dont know exactly what causes those dopamine-producing cells to die.
Trudeau, a neuroscientist, investigates the possibility that an autoimmune attack on those dopamine cells is the culprit.
Trudeau and his immunologist colleague, Michel Desjardins, are studying the role of the portion of cells called axon terminals. These terminalsthe root-like extremities of cellsrelease the chemical messengers that send communication signals. Trudeau believes the death of these terminals, before the death of the dopamine cells themselves, is where the trouble starts.
How Can People Manage Parkinsons
When it comes to managing dyskinesia and tremors, its important to strike a balance between too much medication and too little. You can have too much dopamine medication , which can make dyskinesias occur earlier and can make them worse once they start, says Herrington. Then theres the effect of not enough dopamine medication, which can leave people with this off, slow, stiff feeling.
The person and the caregiver and loved ones need to be aware of the necessary trade-offs that are involved, he continues. Only then can you make an informed decision on how best to move forward.
The more people know about the treatment options for Parkinsons, the better off they tend to feel. There may be a situation where a patient feels very uncomfortable in the off state but the spouse is bothered by dyskinesias, Herrington says. I share with that we cant necessarily find the perfect dose that gives your partner relief from the slow, stiff, off symptoms and causes no dyskinesias. For some patients, finding that middle ground is very difficult.
Dont Miss: Can Epilepsy Cause Parkinsons Disease
You May Like: Life Expectancy Of Someone With Parkinson’s
Is Parkinsons An Autoimmune Disease
Parkinsons disease is a neurological condition resulting from an imbalance of dopamine and acetylcholine, two chemical messengers in the brain that help control movement.; Too little dopamine leads to problems with gross and fine motor coordination.; It is thought to be caused by a combination of genetic and environmental factors, in conjunction with increasing age. ;More recently an immunological cause has been under investigation.; Below we examine the possibility of a connection between Parkinsons and autoimmune disease.
What are the signs and symptoms of Parkinsons disease?
Aside from those above, Parkinsons patients may present with a fairly wide range of other signs and symptoms, which are alternately present or absent depending on the individual.; They may experience psychological issues such as depression or anxiety, which is likely the result of biochemical changes within the brain, coupled with the considerable burden of living with Parkinsons.; And some patients will exhibit varying degrees of autonomic dysfunction, where the automatic/involuntary functions of the body, such as urination or sweating, are disrupted.; Still others have trouble maintaining their balance during normal activities.
Have there been studies linking Parkinsons to an autoimmune trigger?
Does the research indicate that, similar to hypothyroidism, Parkinsons has an autoimmune and non-autoimmune root cause?
Questions for your doctor:
The Connection Between The Immune System & Parkinson’s
In the recent study, researchers from Columbia University Medical Center and the La Jolla Institute for Allergy and Immunology collected blood samples from 67 people with PD and 36 age-matched healthy control subjects. The blood was then exposed to fragments of alpha-synuclein and other proteins that are found in neurons.
In the healthy controls, there was little immune activity detected, but in the blood samples from people with PD, there was a significant response. Researchers believe that the T-cells in people with PD have been primed to recognize alpha-synuclein from past exposure the exposure being the presence of Lewy bodies in the brain. The immune response seen in the study subjects with PD was associated with a common gene variant that is known to affect the immune system, a gene variant that is common in people with PD.
Researchers hypothesize that autoimmunity in people with PD may develop when the neurons are no longer able to rid themselves of the abnormal accumulations of alpha-synuclein. In normal, healthy cells, old or damaged proteins are broken down and eliminated, but this process is not functioning properly in PD. When alpha-synuclein begins to form clumps, the immune system may mistakenly see it as a pathogen that needs to be attacked.1,2
Don’t Miss: Do People Die From Parkinson’s Disease
Key Brain Changes Are Different
The key brain changes linked to Parkinsons disease and Parkinsons-related dementia are abnormal deposits of common brain proteins, called alpha-synuclein. These deposits are known as Lewy bodies, named after the doctor who discovered them. As more of these proteins clump in the brain, normal brain cells begin to die off.1
In Alzheimers disease, the key brain changes include the buildup of different brain proteins, called amyloid and tau. When amyloid proteins clump together, they form abnormal structures known as plaques. Abnormal groups of tau proteins form tangles.3 Over time, the buildup of these proteins causes normal brain cells to die, and affected parts of the brain may shrink.5
You May Like: Sleep And Parkinsons
Attack By Own Immune System May Kill Neurons In Parkinsons
The cause of neuronal death in Parkinsons disease is still unknown, but a new study proposes that neurons may be mistaken for foreign invaders and killed by the persons own immune system, similar to the way autoimmune diseases like type I diabetes, celiac disease, and multiple sclerosis attack the bodys cells. The study was published April 16, 2014, in Nature Communications.
This is a new, and likely controversial, idea in Parkinsons disease; but if true, it could lead to new ways to prevent neuronal death in Parkinsons that resemble treatments for autoimmune diseases, said the studys senior author, David Sulzer, PhD, professor of neurobiology in the departments of psychiatry, neurology, and pharmacology at Columbia University College of Physicians & Surgeons.
The new hypothesis about Parkinsons emerges from other findings in the study that overturn a deep-seated assumption about neurons and the immune system.
For decades, neurobiologists have thought that neurons are protected from attacks from the immune system, in part, because they do not display antigens on their cell surfaces. Most cells, if infected by virus or bacteria, will display bits of the microbe on their outer surface. When the immune system recognizes the foreign antigens, T cells attack and kill the cells. Because scientists thought that neurons did not display antigens, they also thought that the neurons were exempt from T-cell attacks.
Also Check: Which Is Worse Parkinson’s Or Parkinsonism
Potential New Treatment Strategies For Parkinson’s
This new finding provides additional knowledge and understanding of the disease processes that are present in PD and opens the door for using immunotherapies, drugs that suppress the abnormal immune response seen in autoimmune disorders. Additional research is needed to understand the molecular steps that occur in PD and the immune response, but researchers are hopeful that an immunotherapy strategy could help to prevent or lessen worsening symptoms in people with PD.1,2
What Are Atypical Parkinsonian Disorders
Atypical Parkinsonian disorders are progressive diseases that present with some of the signs and symptoms of Parkinsons disease, but that generally do not respond well to drug treatment with levodopa. They are associated with abnormal protein buildup within brain cells.
The term refers to several conditions, each affecting particular parts of the brain and showing a characteristic course:
- Dementia with Lewy bodies, characterized by an abnormal accumulation of alpha-synuclein protein in brain cells
- Progressive supranuclear palsy,; involving tau protein buildup affecting the frontal lobes, brainstem, cerebellum and substantia nigra
- Multiple system atrophy, another synucleinopathy that affects the autonomic nervous system , substantia nigra and at times the cerebellum
- Corticobasal syndrome, a rare tauopathy that typically affects one side of the body more than the other and makes it difficult for patients to see and navigate through space
Recommended Reading: Is Tardive Dyskinesia A Symptom Of Parkinson’s
In Vitro Studies Of Ipsc
A recent in vitro study using induced-pluripotent stem cells -derived midbrain neurons and T cells from PD patients was the first to show that PD patient-derived T cells can kill dopamine neurons directly. Sommer et al. determined that PD patients contain significantly higher Th17 cells than healthy controls . The PD patient-derived Th17 cells exerted cytotoxic effects on neurons by releasing IL-17A, a cytokine detected by IL-17R expressed on neurons . The iPSC in vitro cultures lacked glia, which express MHC-II and can potentially interact with Th17 cells. In addition, T cells were activated non-specifically, and so the antigen specificity of Th17 cells remains unclear . While the study indicates that PD-derived T cells can directly kill dopaminergic neurons, the omission of professional antigen presenting cells, antigenicity, and neuronal specificity in the cultures in this initial study overlooks the role of multiple relevant in vivo factors important for disease progression. Moreover, the mode of action that garners specific vulnerability of dopaminergic neurons and avoids unaffected neurons was not resolved in this study. Nevertheless, the study indicates Th17 cells may participate in PD-related neuronal death.
Potential For Ibogaine In The Treatment Of Parkinsons And Autoimmune Diseases
Ibogaine is an alkaloid derived from the African shrub Tabernanthe iboga. Aside from its psychoactive and anti-addiction properties, it has beneficial effects on certain neurotrophic factors and receptors in the brain. Targeting them has shown great potential for the future therapy of neurodegenerative and neuroinflammatory conditions such as Parkinsons.
Parkinsons disease is a crippling neurological disorder that affects more than 1 million people in the US. The number of people with the condition is expected to increase by more than 60% in the next 20 years . Currently, its cause is unknown but new evidence suggests that its main pathogenetic mechanism might be related to an autoimmune reaction that is present even before the onset of the first symptoms.;
Autoimmune diseases are debilitating conditions that affect about 5% of the population. Currently, there is no cure for Parkinsons or other autoimmune disorders. The treatment options aim at reducing symptoms, preventing complications, and prolonging life.
Also Check: What Happens In The Last Stages Of Parkinson’s
Relationship Between Parkinsons And Seborrheic Dermatitis
While the rate of seborrheic dermatitis in general population is estimated at roughly 3%, in individuals suffering from Parkinsons disease this figure rises closer to the 50% mark .
Because of this striking relationship, seborrheic dermatitis is often discussed and mentioned in the literature examining Parkinsons disease. For example, in a 2017 paper, the authors classified seborrheic dermatitis as a premotor feature of Parkinsons disease referable to dysregulation of the autonomic nervous systemâ .
To put this relationship in context it may make sense to first review Parkinsons disease. While an in-depth review is outside the scope of this work, some of the most important features of the condition include:
- A common neurodegenerative disorder
- Can be genetic, but more frequently it is idiopathic
- No definitive treatment exists
- Tremor, stiffness, and loss of balance are the most prevalent symptoms
Possibly a more concise way to summarize the condition is that it is a myriad of symptoms that arise from the bodies inability to properly coordinate nervous system activity.
And two specific features of the Parkinsons appear to be most relevant to the high rate of seborrheic dermatitis seen among those affected:
- Abnormal sebum production
- Abnormal sweat function
A repeating theme that weâve seen in much of the evidence discussed in this chapter so far.
Parkinsons Disease And Autoimmunity
This autoimmune component of PD may only be one piece of a larger puzzle. It has long been suspected that immune alterations are an important part of the development of PD, says Maureen Leehey, MD, professor of neurobiology at the University of Colorado School of Medicine in Aurora, CO. She notes previous research that has linked ibuprofen use in mid-life with lower PD risk. And studies have shown that in the early stages, but not the late stages, there is activation of immune fighting cells in the brains of persons with PD, Dr. Leehey says. I think that immune alterations are an important part of the progression of central nervous system damage in PD.
This isnt the first research being done on Parkinsons and autoimmunity there have been multiple studies in this vein in recent years. In 2017, the same researchers from La Jolla and Columbia University identified a specific protein that drives the T cell response in early Parkinsons disease. Further work has suggested that Parkinsons could be triggered by bacterial infection.
Paredes explains that changes in the gut bacteria population can cause chronic inflammation that might influence Parkinsons symptoms. An April 2020 study in Nature Genetics theorized that Parkinsons may start in the gut, due to evidence that neurons in the gut are directly associated with the onset of disease.
Recommended Reading: How To Delay Parkinson’s Disease
What Is Progressive Supranuclear Palsy
Progressive supranuclear palsy is a rare brain disorder that causes problems with movement, walking and balance, and eye movement. It results from damage to nerve cells in the brain that control thinking and body movement. The disorders long name indicates that the disease worsens and causes weakness by damaging certain parts of the brain above nerve cell clusters called nuclei that control eye movements.
PSP is different than Parkinsons diseaseanother movement disorderalthough they share some symptoms . Currently there is no effective treatment for PSP, but some symptoms can be managed with medication or other interventions.
Dont Miss: Which President Had Parkinsons Disease
New Evidence That The Immune System Can Be Activated In Parkinsons
All Science News articles summarize a research study and are not an official opinion, endorsement or position of the Parkinsons Foundations.
A new study funded in part by the Parkinsons Foundation shows how the loss of brain neurons in Parkinsons disease could, in part, result from an attack by a persons own immune system.; Furthermore, the researchers link this attack to alpha-synuclein the protein that forms toxic clumps in the brain cells of people with PD.; The results appear in the June 21 online edition of;Nature.
In autoimmune diseases like type 1 diabetes and multiple sclerosis, the immune system attacks and kills specific cells in the body that are mistakenly labeled or flagged as foreign.; The cells actually have a molecular flag, indicating that they are foreign. The flag is called an antigen, and the flagpole an MHC.
Results
- About a third of people with PD had immune-related DNA risk factors; previously linked to PD, compared to 15 percent of healthy individuals.
- Scientists identified two specific pieces of the alpha-synuclein protein that caused the immune cells to respond.
- Immune system cells from people with PD more often recognized specific peptides, or pieces, of alpha-synuclein.
What Does it Mean?
Reference
Sulzer D, Alcalay RN, Garretti F, et al. . T Cells from Patients with Parkinsons Disease Recognize -Synuclein Peptides.; Nature doi:10.1038/nature22815
Recommended Reading: Does Parkinson’s Have Remissions And Exacerbations
