Stage : Age Associated Memory Impairment
This stage features occasional lapses of memory most frequently seen in:
- Forgetting where one has placed an object
- Forgetting names that were once very familiar
Oftentimes, this mild decline in memory is merely normal age-related cognitive decline, but it can also be one of the earliest signs of degenerative dementia. At this stage, signs are still virtually undetectable through clinical testing. Concern for early onset of dementia should arise with respect to other symptoms.
Does Parkinsons Run In Families
Genetics cause about 10% to 15% of all Parkinsons cases. Studies reveal that the appearance of Parkinsons disease is a mix of genetics and environmental factors that induce the development of the disease.
In some families, changes in specific genes are passed down from generation to generation. Yes, Parkinsons disease can run in families, but it is rare. Despite that, if someone is positive for gene mutations directly correlated to Parkinsons disease, that does not mean that the patient will surely develop Parkinsons.
It is possible for people who inherit these genes not to develop the disease if there is no environmental factor that triggers it and a healthy lifestyle.
There are ongoing clinical trials testing therapies to treat people with Parkinsons that carry specific gene mutations. For doctors, it is essential to know which gene mutation does the patient carries.
Are There Medicines To Treat Pdd
Though there is no cure for PDD yet, there are medications that help manage the symptoms. These medications are called cholinesterase inhibitors, and they can help if a person with PDD is having memory problems. Some examples of these medicines are donepezil, rivastigmine and galantamine. Sleep problems may be managed by sleep medications such as melatonin.
Because people with PDD are usually very sensitive to medications, any new medication, even one that is not being used for the brain, needs to be reviewed with the persons provider to avoid potential contraindication.
Read Also: What Is Dyskinesia In Parkinson’s Disease
How Can We Manage Hallucinations
It may not be necessary to treat all hallucinations of a person with PDD. Hallucinations are often harmless, and it is okay to allow them to happen, as long as they are not disruptive or upsetting to the person or surroundings. Sometimes, recognizing the hallucination and then switching the topic might be an efficient way of handling frustrations that occur because of a hallucination. If hallucinations need medical treatment, your provider may be able to discuss and suggest some options. However, many of the medications used to treat hallucinations may make movement symptoms worse.
Can Anaesthesia Cause Dementia In Dogs
Although the toxic substance within grapes and raisins is unknown, these fruits can cause kidney failure. Until more information is known about the toxic substance, it is best to avoid feeding grapes and raisins to dogs. Macadamia nuts can cause weakness, depression, vomiting, tremors and hyperthermia in dogs.
Also Check: End Stage Parkinson Disease What To Expect
What Is The Best Way To Communicate With A Person With Pdd
PD-related mood and motor changes can impact communication cognitive changes and Parkinsons disease dementia can further these difficulties.
- It is not usually helpful to try to reason or argue with someone experiencing a hallucination or delusion. Stay calm and be patient. If the person is frightened by the hallucination or delusion, try to redirect their attention to something else.
- You may find acknowledging what the person is seeing, even if you do not see it, can reduce stress.
- Speak slowly and at eye level. Communicate in simple sentences.
- Ask one question at a time and wait for an answer.
- Limit distractions. Turn off the TV or radio before asking a person with PDD to do something.
- Consider causes behind disruptive behavior: the person may be hungry, thirsty, tired, in pain, frustrated, lonely or bored.
- If the person is stuck on an idea, try agreeing with them, then changing the subject.
- Its OK to use humor to diffuse stressful situations but avoid negative humor or sarcasm these can be misunderstood.
Page reviewed by Dr. Jori Fleisher, MSCE, Assistant Professor, Department of Neurological Sciences at Rush University Medical Center, a Parkinsons Foundation Center of Excellence.
What Is Needed For A Parkinson’s Disease Dementia Diagnosis
There is no definitive medical test that confirms cognitive decline or dementia in Parkinson’s disease. The most accurate way to measure cognitive decline is through neuropsychological testing.
- The testing involves answering questions and performing tasks that have been carefully designed for this purpose. It is carried out by a specialist in this kind of testing.
- Neuropsychological testing addresses the individual’s appearance, mood, anxiety level, and experience of delusions or hallucinations.
- It assesses cognitive abilities such as memory, attention, orientation to time and place, use of language, and abilities to carry out various tasks and follow instructions.
- Reasoning, abstract thinking, and problem solving are tested.
- Neuropsychological testing gives a more accurate diagnosis of the problems and thus can help in treatment planning.
- The tests are repeated periodically to see how well treatment is working and check for new problems.
Imaging studies: Generally, brain scans such as CT scan and MRI are of little use in diagnosing dementia in people with Parkinson’s disease. Positron emission tomographic scan may help distinguish dementia from depression and similar conditions in Parkinson’s disease.
Read Also: Is Parkinson’s Disease Fatal
Coping With Dietary Problems
Many people with Parkinsons experience various eating and dietary problems, such as constipation, chewing and swallowing difficulties, and upset stomach. The following tips can help you minimize the symptoms.
If you suffer from constipation Drink lots of water and eat fiber-rich foods, including beans, brown rice, whole grains, and fruit.
If you have trouble chewing or swallowing food Cut foods into smaller portions to avoid choking and to encourage digestion, and remain upright for 30 minutes after eating.
If youre struggling with fatigueLimit the amount of sugar youre eating. Also avoid alcohol and caffeine, especially before bed, as they can reduce the quality of your sleep.
If you take levodopa Dont eat meat or other protein-rich foods for at least 30-60 minutes after taking levodopa, as protein blocks your bodys ability to absorb the medication.
If your medication gives you an upset stomach Take your medication with a full glass of water and a small non-protein based snack, such as a piece of toast or fruit.
Some Parkinsons disease medications need to be taken promptly at specified times before or after eating, so it can also help to establish a regular routine for meal and medication times.
Coping With A Parkinsons Diagnosis
A diagnosis of Parkinsons can be a frightening experience for both you and your loved ones. While there is currently no cure, there are treatments available for Parkinsons symptoms and lifestyle changes you can make to slow the progression of the disease and delay the onset of more debilitating symptoms, including Parkinsons disease dementia. Early diagnosis can prolong independence and help you to live life fully for much longer.
If youve been diagnosed with Parkinsons you may feel anger, deep sadness, or fear about what the future will bring. These feelings are all normal. Its also normal to grieve as you deal with this enormous adjustment.
Give yourself some time to adjust. As with any major change in life, dont expect that you will smoothly snap into this new transition. You may feel alright for a while, and then suddenly feel stressed and overwhelmed again. Take time to adjust to this new transition.
Learn all you can about Parkinsons disease and Parkinsons disease dementia. Educating yourself and making important decisions early can help you feel more in control during this difficult time.
Reach out for support. Living with Parkinsons presents many challenges, but there is help available for this journey. The more you reach out to others and get support, the more youll be able to cope with symptoms while continuing to enrich and find meaning in your life.
Don’t Miss: Parkinson’s Disease Charity Donations
What Are The Signs And Symptoms Of Parkinson’s Disease Dementia
Parkinson’s disease dementia can’t be diagnosed conclusively by a single test. Instead, doctors may use multiple tests and consider a range of Parkinson’s disease dementia criteria, including symptoms like:
- Feelings of disorientation or confusion
- Agitation or irritability
RELATED: 7 Warning Signs of Dementia to Look For in Loved Ones
Not all cases of cognitive impairment are severesome people with Parkinson’s disease can still manage their work and personal life just fine. But once a person has Parkinson’s disease dementia, it usually means that they can no longer go about their daily life as they once did.
Who Gets Parkinson’s Disease Dementia
No two cases of Parkinson’s are exactly alike, so it’s hard to say for sure who will develop Parkinson’s disease dementia and who will not. However, researchers have identified several factors that may increase a person’s risk for Parkinson’s disease dementia, including:
- Older age, especially at the time Parkinson’s symptoms began
- Being a man
- Advancing to late-stage Parkinson’s disease
- Experiencing visual hallucinations
Read Also: Parkinson Diet Plan
Stage : Mild Cognitive Impairment
Clear cognitive problems begin to manifest in stage 3. A few signs of stage 3 dementia include:
- Getting lost easily
- Noticeably poor performance at work
- Forgetting the names of family members and close friends
- Difficulty retaining information read in a book or passage
- Losing or misplacing important objects
- Difficulty concentrating
Patients often start to experience mild to moderate anxiety as these symptoms increasingly interfere with day to day life. Patients who may be in this stage of dementia are encouraged to have a clinical interview with a clinician for proper diagnosis.
What Other Conditions Have Similar Symptoms And Signs Of Parkinsons Disease
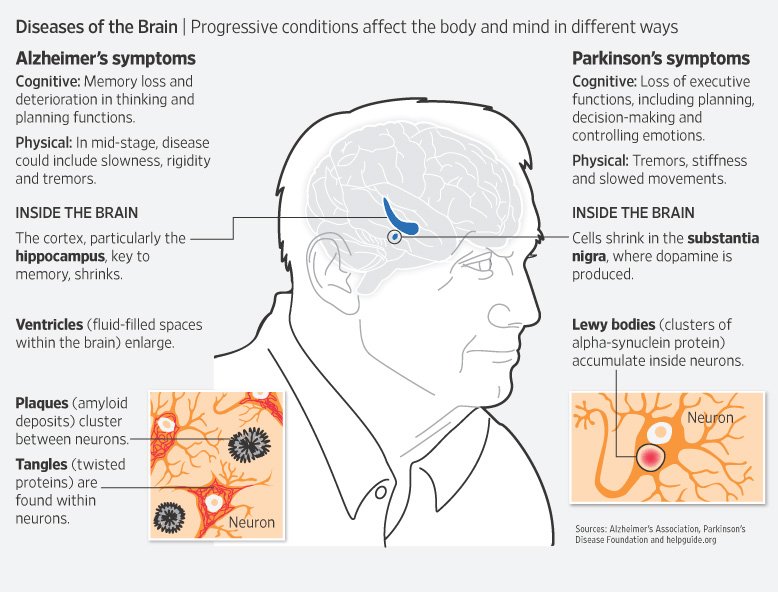
Other neurological diseases may cause symptoms similar to Parkinsons disease. The term Parkinsonism refers to a patient that has symptoms similar to Parkinsons.
Early in the disease process, it can be tough to make an assertive diagnosis and difference between Parkinsons and Parkinson-like diseases.
Often the correct diagnosis is made after further symptoms develop, and the physician can monitor the course of the disease.
The development of additional symptoms and the course of the illness generally points towards the correct diagnosis. These are the most common neurological diseases that can produce Parkinson-like symptoms.
- Progressive Supranuclear Palsy
- Lewy Body disease or Dementia with Lewy bodies
- Corticobasal degeneration or corticobasal ganglionic degeneration
Nonetheless, doctors should think of other causes rather than Parkinsons disease when events like this happen.
- Poor response to dopamine
- Early loss of balance or vision problems
- Prominent intellectual decline dementia
- Rapid onset or progression of the disease
Actually, though it is a disease that is not clearly understood, there are specific organizations like Parkinsons UK that dedicate themselves to doing research.
These organizations look forward to following the natural course of the disease and developing clinical trials for patients in an attempt to find a cure.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Organs Does Parkinson Disease Affect
Parkinsons disease is a degenerative, progressive disorder that affects nerve cells in deep parts of the brain called the basal ganglia and the substantia nigra. Nerve cells in the substantia nigra produce the neurotransmitter dopamine and are responsible for relaying messages that plan and control body movement.
How Is Parkinsons Disease Dementia Diagnosed
No single test can diagnose Parkinsons disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinsons and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinsons dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
You May Like: Parkinson’s Stage 5 Life Expectancy
Do All Parkinsons Patients Develop Dementia
It would be untrue to say that all Parkinsons patients develop dementia. Nevertheless, according to the statistics an estimated 50 to 80 percent of patients having Parkinsons disease eventually develop dementia as the disease progresses. The onset of dementia on an average starts in about 10 years after developing Parkinsons disease.
Certain patients with Parkinsons disease are at higher risk of developing dementia than others. Some of the vital risk factors for developing dementia after Parkinsons disease may include older age, severity of symptoms and presence of mild cognitive impairment. Other additional symptoms which act as risk factor for developing into full fledged dementia include-
- Excessive sleepiness in the daytime.
- Presence of hallucination in the absence of other dementia related symptoms.
- Presence of postural instability and gait which include freezing that occurs suddenly, difficulty in initiating movement and problems with balancing and frequent falling.
Diagnosis Of Parkinsons Disease Dementia
Diagnosis of PDD typically requires the initial diagnosis of PD, with the signs of Parkinsons disease of rest tremor, bradykinesia , rigidity , and postural instability.
At Pacific Movement Disorders Center we regularly monitor patients for cognitive changes which could signal the beginning of dementia, utilizing evidence-based screening tests. If concern arises, detailed neuropsychological evaluation with clear delineation of cognitive strengths and weakness can be obtained. On occasion, volumetric MRI scanning or PET scanning may play a role.
Differentiating between PDD and Dementia with Lewy Bodies can be challenging, given both conditions pertain to dementia and parkinsonism .
Lewy Bodies in PD patients predominate in the deep part of the brain called the substantia nigra, whereas in DLB they are widespread from onset.
The main differentiating factor is the clinical history:
In PDD, parkinsonism comes first, typically years prior to onset of dementia, whereas in DLB, cognitive changes either precede or coincide with onset of parkinsonism.In PDD, there tends to be clear improvement with levodopa for the motor symptoms at least.
For more on differentiating between PDD and DLB, see this comparison table.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
What Is Aggressive Parkinsons Disease
As written above, Parkinsons dementia aggression is that form of Parkinsons which makes the patient exhibit aggressive behavior. They vent out their aggression either verbally or physically, in the various forms that have been written above. Besides verbal and physical outbursts, PD Dementia patients are also prone to hallucinating caused by the medication administered. Hallucinations in PD Dementia patients primarily occur because of the effects of dopaminergic agents for motor symptoms.
Loss of dopamine neurons in the ventral tegmental area is one of the likeliest of all neuropathological causes as changes in serotonin and norepinephrine systems are not. For the uninitiated, the ventral tegmental area is the origin of the mesolimbic dopaminergic projection. Plenty of studies have gone into analyzing the cause behind the aggression in PD Dementia patients. Depression in PD Dementia patients has been identified due to changes in the medial frontal cortex and the anterior cingulate. Akinetic-rigid variants have been found in patients showing signs of major depression.
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesn’t go away and continues to get worse over time.
Also Check: Do Dogs Get Parkinson’s
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Differences Between Alzheimers And Parkinsons

We will group the differences between the two diseases in different blocks and explain what each of them consists of. The differences are taken from two reference manuals for psychopathology: Belloch, Sandín and Ramos and DSM-5 .
The first block of differences between Alzheimers and Parkinsons refers to their type of symptoms. Lets look at who they are.
Also Check: Parkinson Risk Factors
What Is End Stage Parkinsons
The final stage of Parkinsons disease is the most severe. You may not be able to perform any physical movements without assistance. For that reason, you must live with a caregiver or in a facility that can provide one-on-one care. Quality of life declines rapidly in the final stages of Parkinsons disease.
Surgery And Deep Brain Stimulation
Deep brain stimulation is a treatment for Parkinsonâs disease that uses an implantable pacemaker-like device to deliver electrical pulses to parts of the brain involved in movement. The DBS system consists of leads precisely inserted into a specific brain target, the neurostimulator implanted in the chest, and extension wires that connect the leads to the neurostimulator. Though implantation of the system requires a neurosurgical procedure, the treatment itself consists of long-term electrical stimulation. Advantages of DBS include its ability to reduce the high doses of medications , its adjustability , and its reversibility DBS was approved by the Food and Drug Administration as a treatment for PD in 2002 and according to Medtronic , more than 80,000 patients have undergone DBS surgery worldwide.
Typical candidates are those who have motor fluctuations or periods of âoffâ time with troublesome symptoms alternating with periods of âonâ time with good symptom control, and also with possible periods of excessive movement .
Not all patients with Parkinsonâs disease are good candidates for treatment with DBS. Approximately 10â20% of patients considered for possible treatment with DBS include those:
Read Also: How To Reverse Parkinson’s Disease Naturally
