Whats The Difference Between Lewy Body Dementia Parkinsons Disease And Alzheimers Disease
Lewy body dementia is an umbrella term for two related clinical diagnoses: dementia with Lewy bodies and Parkinsons disease dementia. These disorders share the same underlying changes in the brain and very similar symptoms, but the symptoms appear in a different order depending on where the Lewy bodies first form.
Dementia with Lewy bodies is a type of dementia that causes problems with memory and thinking abilities that are severe enough to interfere with everyday activities. It specifically affects a persons ability to plan and solve problems, called executive function, and their ability to understand visual information. Dementia always appears first in DLB. The motor symptoms of Parkinsons such as tremor, slowness, stiffness and walking/balance/gait problems usually become more evident as the disease progresses. Visual hallucinations, REM sleep behavior disorder, fluctuating levels of alertness and attention, mood changes and autonomic dysfunction are also characteristic of DLB.
Finally, Alzheimers is characterized by different abnormal clumps called amyloid plaques, and jumbled fiber bundles called tau tangles. These microscopic structural changes in the brain were discovered by Dr. Alois Alzheimer in 1906. These plaques and tangles, together with loss of connections between nerve cells, contribute to loss of coherence and memory, as well as a progressive impairment in conducting normal activities of daily living.
Building A Lewy Body Dementia Care Team
After receiving a diagnosis, a person with LBD may benefit from seeing a neurologist who specializes in dementia and/or movement disorders. Your primary doctor can work with other professionals to follow your treatment plan. Depending on an individual’s particular symptoms, physical, speech, and occupational therapists, as well as mental health and palliative care specialists, can be helpful.
Support groups are another valuable resource for people with LBD and their caregivers. Sharing experiences and tips with others in the same situation can help people find practical solutions to day-to-day challenges and get emotional and social support.
Comparing Parkinsons Disease And Als Causes
When certain nerve cells in the brain begin to die or break down that is what causes Parkinsons disease, but why this occurs is unclear. Some factors that contribute to nerve cell death include genetics as specific gene mutations have been identified to contribute to Parkinsons disease, environmental factors such as exposure to certain toxins, the presence of Lewy bodies in the brain, as well as alpha-synuclein found in Lewy bodies.
There are many unanswered questions about ALS, including the root cause. What we do know is that nerve cells that control the movement of muscles gradually die in ALS patients.
Researchers around the world continue to investigate the possible causes of ALS, including whether the immune system plays a role in attacking the body cells, potentially killing nerve cells. Scientists are examining chemical imbalance and trying to determine if proteins in people with ALS are being incorrectly processed by nerve cells.
Environmental factors are also being put under the scrutiny. One study has stated that members of the military personnel in the Gulf region during the 1991 war were more likely to develop Lou Gehrigs disease than military personnel stationed anywhere else. The question is, could mechanical or electrical trauma, exposure to high levels of exercise, exposure to high levels of agricultural chemicals, or heavy metals play a role?
You May Like: Insomnia And Parkinsons Disease
Recommended Reading: How To Care For Someone With Parkinson’s Disease
Exploring The Connection Between Alzheimers And Parkinsons Disease
While the exact interplay of the clinical and pathological features between the two diseases is not fully established, there is a definite connection between Alzheimers and Parkinsons disease. Similar cognitive and functional impairments are observable in both diseases. However, different proportions, varying manifestations along the disease continuums, and different rates of occurrence set the two apart.
Typically, Parkinsons patients will show early signs of functional impairment and in later stages may experience cognitive impairment, such as memory issues, if they develop dementia. According to the National Parkinsons Foundation, recent studies that followed Parkinsons patients over the course of the disease estimate that 50-80% of people with the disease may eventually develop dementia. Conversely, earlier symptoms of Alzheimers patients may be more biased towards cognitive impairment, with functional impairments observed in later stages of the disease.
Key Difference Parkinsons Vs Huntingtons Disease
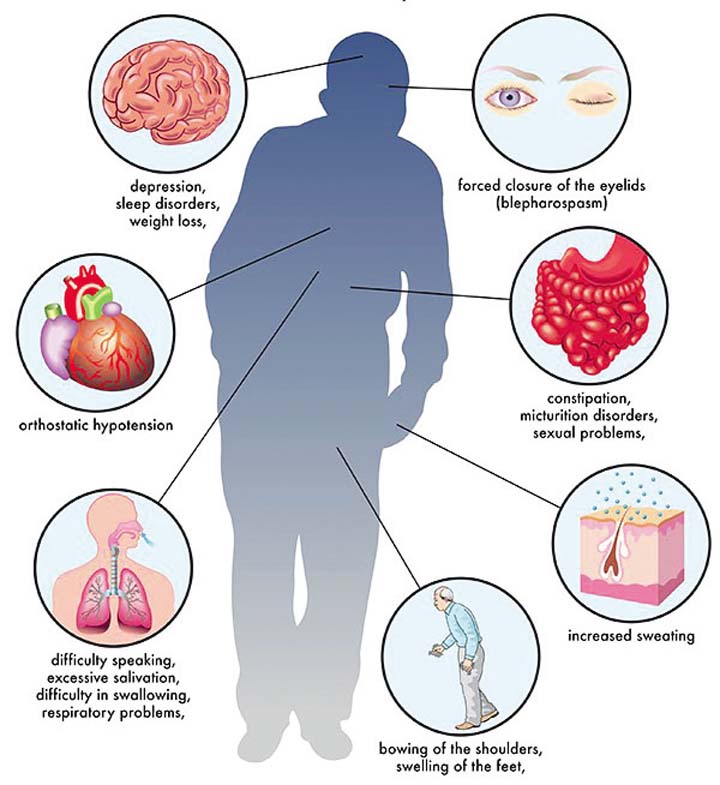
The key difference between Parkinsons and Huntingtons disease is that Parkinson diseaseis a disorder with rigidity, tremors, slowing of movements, postural instability and gait disturbances usually occurring in old age due to degeneration of the substantia nigra of the midbrain while Huntingtons disease is a familial neurodegenerative disorder usually occurring in a younger population, characterized by emotional problems, loss of thinking ability and abnormal choreiform movements .
Also Check: Is Parkinson’s Disease A Disability
Are Parkinson’s And Alzheimers Related
Alzheimers disease and Parkinsons disease are both neurodegenerative diseases that are classified under the general term of dementia. Because of the vagueness of dementia as a medical label, many experts refer to it as a syndrome rather than a specific disease. Within the umbrella of dementia, these neurological disorders are often confused because of overlapping characteristics but Alzheimers and Parkinsons have unique symptoms, treatments and prognoses.
Alzheimers disease is the most common form of dementia. While many cases are diagnosed in patients over 65, individuals younger than 65 can be diagnosed with early-onset Alzheimers. Signs of Alzheimers can be mild at first and include subtle forgetfulness or confusion, but symptoms will worsen over time and eventually interfere with daily tasks and activities.
Theres no cure for Alzheimers, but ongoing research has resulted in treatment options that may temporarily improve symptoms. Current treatment options include medications and physical exercise.
Prognoses vary depending on many factors, but a person with Alzheimer’s usually lives four to eight years after diagnosis. Although, some patients have lived as long as 20 years after finding out they have Alzheimer’s.
While Alzheimers and Parkinsons are both progressive neurological diseases, Parkinsons disease has more of an effect on physical function compared to the decline in cognitive function experienced by Alzheimers patients.
Behavioral And Mood Symptoms Of Lewy Body Dementia
Changes in behavior and mood are possible in LBD and may worsen as the persons thinking abilities decline. These changes may include:
- Apathy, or a lack of interest in normal daily activities or events and less social interaction
- Anxiety and related behaviors, such as asking the same questions over and over or being angry or fearful when a loved one is not present
- Agitation, or restlessness, and related behaviors, such as pacing, hand wringing, an inability to get settled, constant repeating of words or phrases, or irritability
- Delusions, or strongly held false beliefs or opinions not based on evidence. For example, a person may think his or her spouse is having an affair or that relatives long dead are still living.
- Paranoia, or an extreme, irrational distrust of others, such as suspicion that people are taking or hiding things
Don’t Miss: Do Women Get Parkinson’s
What Is Alzheimer’s Disease
Alzheimer’s disease , the most common form of dementia among older adults, is an irreversible degeneration of the brain that causes disruptions in memory, cognition, personality, and other functions that eventually lead to death from complete brain failure. Genetic and environmental factors including diet, activity, smoking, traumatic brain injury, diabetes, and other medical diseases contribute to the risk of developing this form of the disease. The hallmarks of Alzheimer’s disease are the accumulation of beta-amyloid plaques between nerve cells in the brain and neurofibrillary tangles, which are twisted fibers found inside the brain’s cells). These tangles consist primarily of a protein called tau.
Alzheimers And Parkinsons Disease: Similarities And Differences
James M. Ellison, MD, MPH
Swank Center for Memory Care and Geriatric Consultation, ChristianaCare Configure
Explore the similarities and differences between two common degenerative brain disorders.
Ron brings his 78-year-old wife, Sara, to the Memory Clinic, with a pressing concern. Sara is forgetting things more often even though her Parkinsons disease symptoms appear to be under good control with standard medications, healthy diet, and plenty of physical activity. She is losing her train of thought mid-sentence and she became very confused about where she was while driving the well-traveled route to her daughters home. Is she developing dementia? Is that a part of Parkinsons disease? Or is she developing Alzheimers disease? And what are the differences between Alzheimers and Parkinsons?
Recommended Reading: Video Of Parkinson’s Tremor
Chronic Traumatic Encephalopathy/brain Injury
Initial symptoms: Symptoms of brain injury include loss of consciousness, memory loss, personality and behavior changes, and slow, slurred speech.
Progression: While symptoms from a single concussion are often temporary and resolve with appropriate treatment, chronic traumatic encephalopathy typically develops over time from repeated head injuries and is generally not reversible. Later symptoms include poor decision-making ability, aggression, impaired motor function and inability to communicate effectively.
Prognosis: Life expectancy varies according to the severity of injuries.
Parkinsons Disease Is Actually 50% More Common In The Us Than Current Estimates
Current estimates put the number of Parkinsons disease diagnoses at 60,000 annually. However, new research reveals that the actual incidence rate is nearly 90,000 diagnoses each year, which is 50% higher.
New Parkinsons disease incidence rate totals nearly 90,000 diagnoses each year, compared to previous estimates of 60,000 diagnoses annually.
Parkinsons disease is the second most common neurodegenerative disease after Alzheimers disease. It is much more common in older age, with a population prevalence of 4% at age 80 compared to 1% at age 60. It is a brain disorder that causes unintended or uncontrollable movements, such as shaking, rigidity, and difficulty with balance and coordination. Symptoms usually begin gradually and worsen over time, with cognitive decline common at later stages. As the disease progresses, people may have difficulty walking and talking.
New research reveals that the annual incidence of Parkinsons disease among older adults is actually 50% higher than current estimates of 60,000 diagnoses annually. Published today in the scientific journal npj Parkinsons disease, the peer-reviewed study measured new cases of Parkinsons disease, or the number of people diagnosed with PD per year.
The key findings include:
The study was supported by the Parkinsons Foundation and The Michael J. Fox Foundation for Parkinsons Research , as well as the Institute for Clinical Evaluative Sciences .
Read Also: Is Cbd Good For Parkinson’s
What Causes Parkinsons Disease
Parkinsons disease occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. Normally, these neurons produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinsons. Scientists still do not know what causes cells that produce dopamine to die.
People with Parkinsons also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying-down position.
Many brain cells of people with Parkinsons contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons disease and Lewy body dementia.
You May Like: Parkinsons Donations In Memory Of
Types Of Lewy Body Dementia And Diagnosis
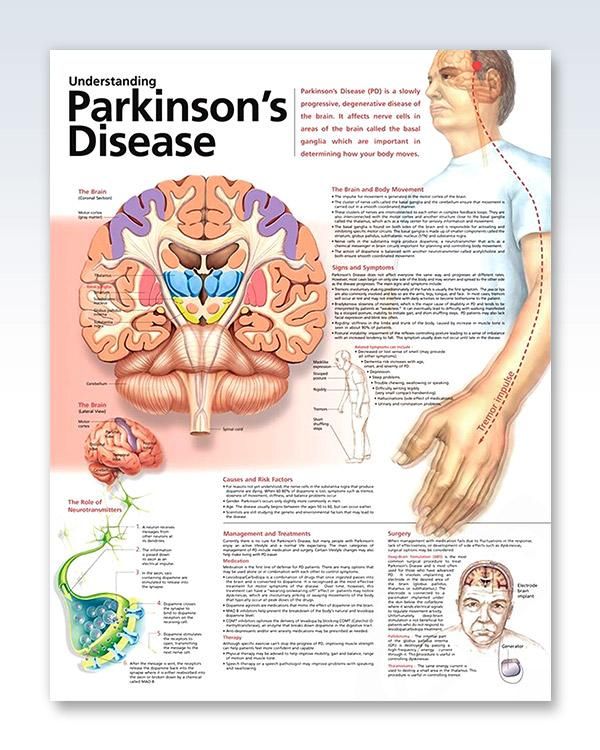
LBD refers to either of two related diagnoses dementia with Lewy bodies and Parkinson’s disease dementia. Both diagnoses have the same underlying changes in the brain and, over time, people with either diagnosis develop similar symptoms. The difference lies largely in the timing of cognitive and movement symptoms.
In DLB, cognitive symptoms develop within a year of movement symptoms. People with DLB have a decline in thinking ability that may look somewhat like Alzheimer’s disease. But over time, they also develop movement and other distinctive symptoms of LBD.
In Parkinson’s disease dementia, cognitive symptoms develop more than a year after the onset of movement symptoms . Parkinson’s disease dementia starts as a movement disorder, with symptoms such as slowed movement, muscle stiffness, tremor, and a shuffling walk. These symptoms are consistent with a diagnosis of Parkinson’s disease. Later on, cognitive symptoms of dementia and changes in mood and behavior may arise.
Not all people with Parkinson’s disease develop dementia, and it is difficult to predict who will. Many older people with Parkinson’s develop some degree of dementia.
Caregivers may be reluctant to talk about a person’s symptoms when that person is present. Ask to speak with the doctor privately if necessary. The more information a doctor has, the more accurate a diagnosis can be.
You May Like: Is Parkinson’s More Common In Males
Movement Disorders Similar To Parkinsons
Conditions causing excess movement or decreased movement that are sometimes associated with Parkinsons disease-like symptoms include:
What Movement Disorder Could I Have?
When making a Parkinsons diagnosis, your doctor will review your medical history and symptoms, perform a careful neurological exam, and, if necessary, carry out further tests to rule out other movement disorders.
Your symptoms may be caused by a movement disorder other than Parkinsons disease if:
- You display Parkinsons disease symptoms and features that are characteristic of an additional movement disorder.
- The results of a brain imaging study or laboratory test, such as a blood test, confirm the presence of another movement disorder.
- Your symptoms do not respond to Parkinsons disease medication.
Because movement disorders are not all treated the same way, it is important to get a proper diagnosis as early as possible so you can formulate the right treatment plan with your doctor.
You May Like: Alternative Treatment For Parkinsons Disease
Managing Sleep Disorders In Lewy Body Dementia
Sleep problems may increase confusion and behavioral problems in people with LBD and add to a caregiver’s burden. A physician can order a sleep study to identify any underlying sleep disorders such as sleep apnea, restless leg syndrome, and REM sleep behavior disorder.
REM sleep behavior disorder, a common LBD symptom, involves acting out one’s dreams, leading to lost sleep and even injuries to individuals and their sleep partners. Clonazepam, a drug used to control seizures and relieve panic attacks, is often effective for the disorder at very low dosages. However, it can have side effects such as dizziness, unsteadiness, and problems with thinking. Melatonin, a naturally occurring hormone used to treat insomnia, may also offer some benefit when taken alone or with clonazepam.
Excessive daytime sleepiness is also common in LBD. If it is severe, a sleep specialist may prescribe a stimulant to help the person stay awake during the day.
Some people with LBD have difficulty falling asleep. If trouble sleeping at night persists, a physician may recommend a prescription medication. It is important to note that treating insomnia and other sleep problems in people with LBD has not been extensively studied, and that treatments may worsen daytime sleepiness and should be used with caution. Sleep problems can also be addressed by avoiding lengthy naps, increasing daytime exercise, and avoiding caffeine, alcohol, and chocolate late in the day.
Also Check: How To Reverse Parkinson’s Naturally
Discovery Raises Possibility Of New Medication For Alzheimers Parkinsons
Researchers from Oregon Health & Science University have for the first time demonstrated its possible to use a synthetic thyroid hormone to regulate a gene implicated in neurodegenerative diseases like Alzheimers, Parkinsons and multiple sclerosis.
The findings from tests in cells and mice, published today in the journal Cell Chemical Biology, raise the possibility of development of new medication to treat debilitating diseases.
This is the first example reported that shows its possible to increase the expression of the TREM2 gene in a way that will lead to healing in certain diseases, said senior author Tom Scanlan, Ph.D., professor of physiology and pharmacology in the OHSU School of Medicine. This will generate a lot of excitement.
The papers first author is Skylar J. Ferrara, Ph.D., a postdoctoral fellow in the OHSU School of Medicines chemical physiology and biochemistry department.
The discovery builds on a 2013 publication linking genetic variants of TREM2 to risk of Alzheimers disease.
The new research from OHSU builds on that work by showing that its possible to turn on TREM2 expression and the TREM2 pathway using a compound originally developed more than two decades ago to lower cholesterol.
The pathway activated by the TREM2 gene is also implicated in neurodegenerative diseases, including Alzheimers and Parkinsons.
The possibility of doing clinical trials is not millions of miles away, Scanlan said. It would be an achievable thing.
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinsons disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
You May Like: Is Lewy Body Dementia Present In All Parkinson’s Residents
Symptoms Related To Brain Function Are Different
There is some overlap, but in general, the overall cognitive symptoms that people experience with Parkinson’s disease, dementia, and Alzheimer’s are different. Alzheimer’s mainly affects language and memory at the outset, whereas Parkinson’s affects problem-solving, speed of thinking, memory, and mood.6
Unlike Alzheimer’s disease, people with Parkinson’s-related dementia often experience hallucinations, delusions, and paranoid thoughts. Both conditions can lead to depression, anxiety, and sleep disturbances.4,6
What Is Alzheimers Disease
Alzheimers disease , the most common form of dementia among older adults, is an irreversible degeneration of the brain that causes disruptions in memory, cognition, personality, and other functions that eventually lead to death from complete brain failure. Genetic and environmental factors including diet, activity, smoking, traumatic brain injury, diabetes, and other medical diseases contribute to the risk of developing this form of the disease. The hallmarks of Alzheimers disease are the accumulation of beta-amyloid plaques between nerve cells in the brain and neurofibrillary tangles, which are twisted fibers found inside the brains cells). These tangles consist primarily of a protein called tau.
You May Like: Using Cbd For Parkinsons Disease
Also Check: Tremors Associated With Parkinson’s
