Signs And Symptoms Of Pdd
Common signs and symptoms of Parkinsons disease dementia include:
- Poor memory and concentration
- Visual hallucinations
If youve noticed some of the above signs and symptoms in yourself or a loved one, its important to get them checked out. But dont jump to conclusions. People with Parkinsons often experience cognitive changes such as anxiety, lack of motivation, and slowed thinking. These symptoms do not automatically mean dementia.
Also Check: Atypical Parkinsons Disease Life Expectancy
This Simple Remedy Changed My Life
Simple lifestyle improvements transformed my entire life. Its done exactly the same for thousands of other very ordinary people who thought theyd suffer their illness for life.
It requires a small initial effort. Not much. But a little more than unscrewing the lid on a jar of chemicals.
For the millions who see drugs as their only hope there are thousands like me who know for an absolute fact that theyre not.
Which is why we dont suffer those nasty symptoms anymore while they still do.
What Is Parkinsons Disease
Parkinsons disease is a nervous system disorder where a part of the brain degenerates over time. Tremors, slow speech and movement, and an altered or festinating gate are common symptoms.
I have worked with many patients who had resting tremors and also patients who truly had Parkinsons disease. Resting tremors are when your hands shake without doing anything.
Some people who have resting tremors will be told that they might have Parkinsons disease. Of course, many of them do but some of them dont.
I have seen a strong correlation with over activation of the Sympathetic Autonomic Nervous System and tremors.
The Parasympathetic Autonomic Nervous System is the Rest and Digest side of the nervous system. It is what keeps us calm. When you eat a large meal, it is what gets activated and causes you to want to rest.
When the two sides of the Autonomic Nervous System are out of balance, it can create health problems.
The best way that I can explain it is when you have a car accident, a physical altercation or a really bad argument, what tends to happen? Your blood pressure will rise and for about 10-20 minutes or so, your hands shake.
Some people can get stuck in a chronic Sympathetic state where the Sympathetic nervous system overpowers the Parasympathetic.
For some people, this can cause them to have resting tremors or the shakes while others will experience anxiety, depression, night sweats, excessive sweating during the day, poor digestion, hot flashes, etc
You May Like: Is Cervical Dystonia Related To Parkinson’s
New Diagnostic Standards For Parkinsons
Until recently, the gold-standard checklist for diagnosis came from the U.K.s Parkinsons Disease Society Brain Bank. It was a checklist that doctors followed to determine if the symptoms they saw fit the disease. But thats now considered outdated. Recently, new criteria from the International Parkinson and Movement Disorder Society have come into use. This list reflects the most current understanding of the condition. It allows doctors to reach a more accurate diagnosis so patients can begin treatment at earlier stages.
Tips For Better Sleep With Thyroid Issues
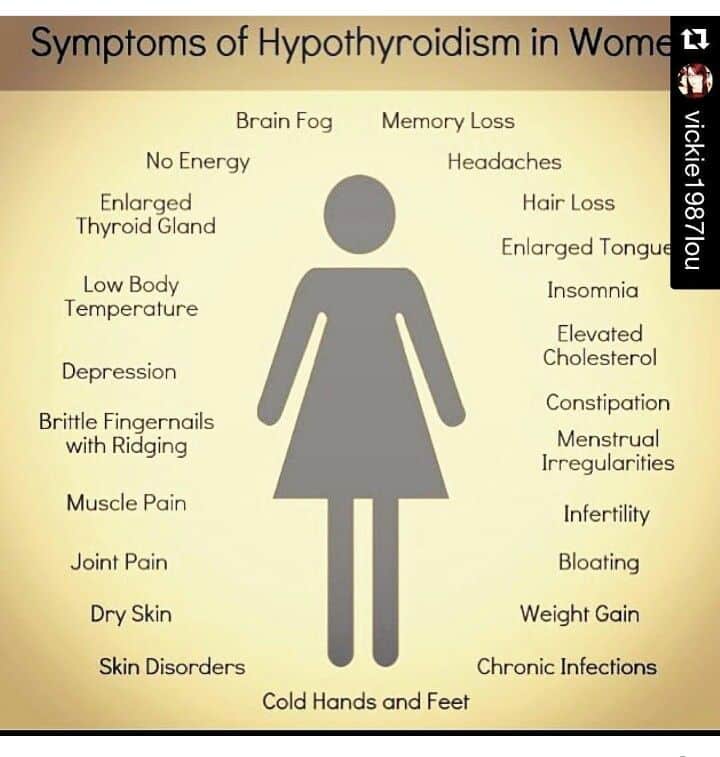
People with thyroid disease who experience sleep loss or disturbances may find relief by taking certain measures.
For many, finding the right bedroom temperature is key. Many experts agree that 65 degrees Fahrenheit is the optimal sleep temperature for most people. However, those with thyroid disease may feel differently, as hyperthyroidism can cause night sweats and hypothyroidism can decrease your tolerance to the cold. The range of 60-67 degrees Fahrenheit is considered reasonable, and you may find your preferred temperature falls outside this range if you live with thyroid disease.
Practicing good sleep hygiene can also improve your sleep quality whether or not you have a thyroid condition. Sleep hygiene refers to practices and habits that promote consistent, uninterrupted and restorative sleep. These include going to bed and waking up at the same times , avoiding electronic devices for up to an hour before bed, and winding down in the evening with soft music, light stretching, and other relaxing activities.
A healthy diet is also crucial for sleep hygiene. Heavy meals leading up to bedtime can be disruptive to sleep, so its better to opt for light snacks instead. People with thyroid issues should pay particular attention to their iodine intake, as too much or too little iodine in ones diet can affect thyroid activity. You may also want to avoid caffeine and alcohol in the hours before bed, as both of these substances can disrupt sleep.
- Was this article helpful?
You May Like: How To Tell The Difference Between Essential Tremor And Parkinson’s
Inborn Errors Of Metabolism
Inborn errors of metabolism are common causes of hyperkinetic and hypokinetic movement disorders in children. A single error of metabolism can cause multiple movement disorders. Diagnosis of these disorders requires screening for specific metabolites in urine, serum or cerebrospinal fluid, the results of which can direct further biochemical or genetic analyses. Movement disorders in these children can cause life-long disability. Chorea is not an uncommon symtptom of inborn errors of metabolism , and is a predominant characteristic of glutaric aciduria type 1, glucose transporter type 1 deficiency, and Lesch-Nyhan disease. A recent report described that Niemann Pick type C in the adult-onset can mimic HD phenocopies and should be considered in the diagnostic approach of patients with a choreic phenotype .
Table 2
Characteristics of inborn errors of metabolism and mitochondrial cytopathies where chorea is the predominant movement disorder.
Mov Dis: Movement Disorders Sx: Symptoms DD: Developmental delay I: Imaging L: Laboratory AR: Autosomal recessive AD: Autosomal dominant CSF: cerebrospinal fluid WM: white matter FP: frontoparietal.
* Only the disorders of metabolism where chorea is the predominant movement disorder are included.
* Wilsons disease is described under autosomal recessive hereditary choreas.
Thankfully None Of This Is Going To Happen
Which is what I want to tell you about now. So let me start by reassuring you of this:
I feel fine. Absolutely fine.
In some ways, Im happier and more positive than I was before I got that initial shocking diagnosis.
My hands no longer shake. I sleep like a lamb. And I recall all the important details about my life or what I did this morning! with ease.
Second, theres a reason I feel this way. And its to do with how Ive actively worked on my condition.
Also Check: What Effect Does R Dopa Have On Parkinson’s Disease
B Appropriate Prophylaxis And Other Measures To Prevent Readmission
Ensure adequate nutrition and safe swallowing.
Fall prevention and physical therapy to strengthen the patient.
If the patient is to return home on discharge, make sure the primary caregiver has adequate support systems and community resources available to assist in care.
No sponsor or advertiser has participated in, approved or paid for the content provided by Decision Support in Medicine LLC. The Licensed Content is the property of and copyrighted by DSM.
Im Not A Medical Rebel
Now I should point out here that I am not the kind of person who second-guesses his doctor!
I trust professionals and experts. They studied for years. They do the research. They know plenty.
But their most effective meds came with unpleasant side-effects.
And those meds would become less effective as time wore on.
They would work for a while and then theyd start failing.
And as they failed my health would fail even more.
What kind of future is that?
Also Check: How Close Is A Cure For Parkinson’s
F Prognosis And Patient Counseling
Parkinsons is a progressive disease, although the rate and degree of progression is variable. Treatments such as levodopa that initially provide great improvement in motor skills, tend to lose their effect or longevity with time.
There are many Parkinsons support groups that patients and their families can benefit from. There is currently no genetic testing recommended for family members.
Clinical And Demographic Features
Table compares the demographic characteristics of the 38 patients with PD and 16 patients with other forms of parkinsonism that completed our work-up. Patients with PD were older than patients with parkinsonism . However, age of onset, disease duration and gender distribution were similar in both groups, despite a trend for higher percentage of women in the parkinsonism group and for older age of onset and longer disease course in the PD group. Mean Hoehn and Yahr scores in the PD group were 2.6±0.1 . Most of the PD patients were treated with levodopa and 68.8 % of the parkinsonism group were taking levodopa. A third of the PD patients and 31 % of the parkinsonism group were treated with pramipexol while 38.9 % of the PD and none from the parkinsonism group were treated with amantadine and only 8.3 and 18.8 were treated with biperiden.
Table 1 Demographic characteristics and risk factors for neuropathy in patients with Parkinsons disease and Parkinsonism
Also Check: What Type Of Doctor Diagnosis Parkinson’s Disease
Thyroid Dysfunction And Risk Of Parkinsons Disease: A Systematic Review And Meta
- 1Department of Medicine, Mount Auburn Hospital, Harvard Medical School, Cambridge, MA, United States
- 2Department of Medicine, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
- 3Harvard T.H. Chan School of Public Health, Boston, MA, United States
- 4Department of Pharmacology, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
- 5Department of Medicine, MetroWest Medical Center, Framingham, MA, United States
Objective: Studies have suggested that patients with thyroid dysfunction may have an increased risk of developing Parkinsons disease . However, the results from existing studies are inconsistent. Therefore, we aimed to investigate the association of hypothyroidism and hyperthyroidism with risk of PD using the method of systematic review and meta-analysis.
Results: A total of 3,147 articles were identified. After two rounds of independent review by three investigators, 3 cohort studies and 6 case-control studies met the eligibility criteria and were included into the meta-analysis. Pooled analysis showed an increased likelihood of PD in both patients with hypothyroidism and patients with hyperthyroidism . Funnel plots for both meta-analyses were fairly symmetric, which did not indicate presence of publication bias.
This systematic review and meta-analysis found a significant association of both hypothyroidism and hyperthyroidism with an increased risk of PD.
What Causes Thyroid Problems
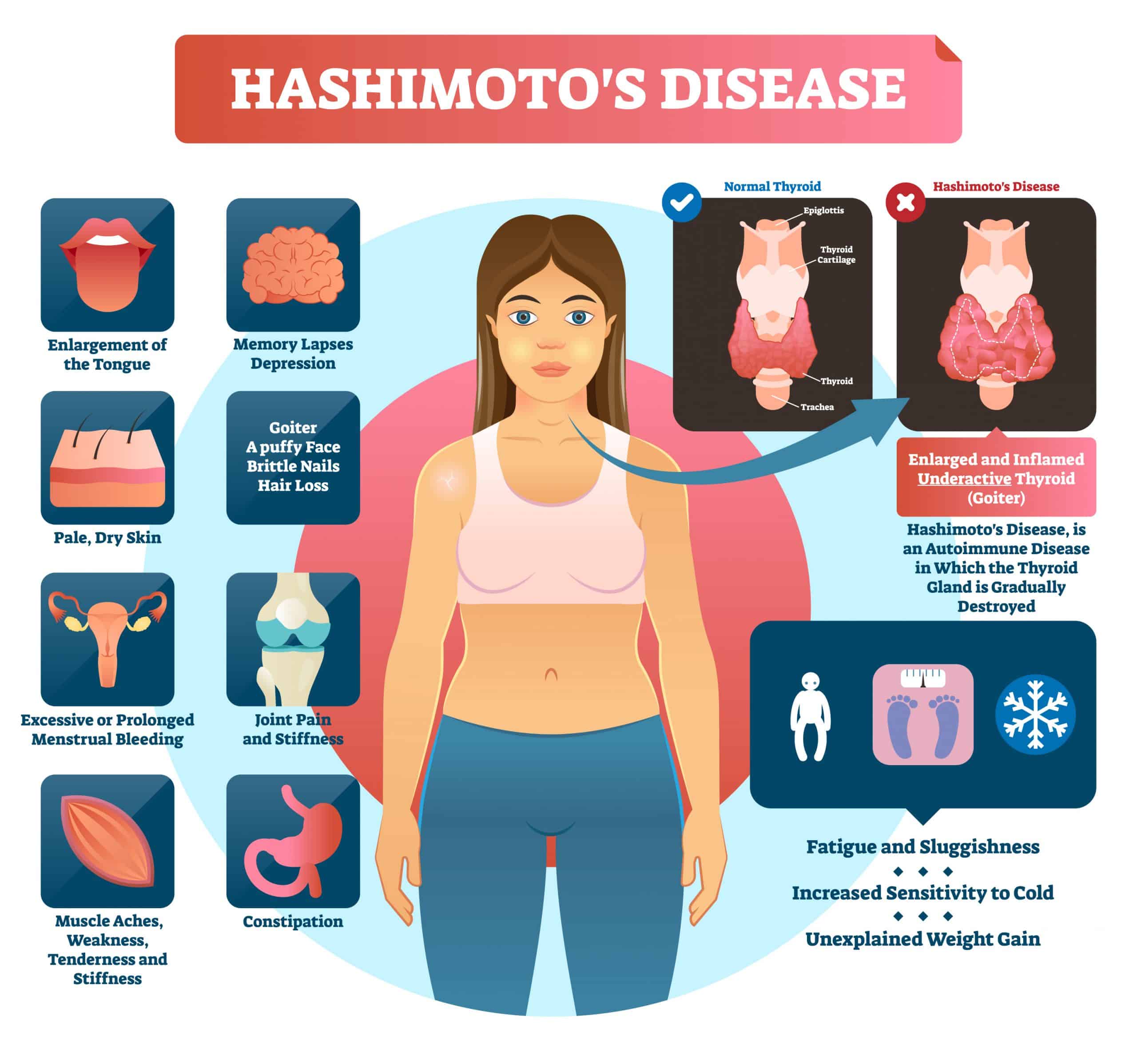
Several different problems can arise when your thyroid produces too much hormone or not enough .
Your thyroid is a small, butterfly-shaped gland located at the base of your neck just below the center of your throat. Its part of an intricate network of glands called the endocrine system. Your endocrine system is responsible for coordinating many of your bodys activities. Your thyroid gland manufactures hormones that regulate your bodys metabolism.
When your thyroid is underproducing or overproducing, it can cause bothersome symptoms such as irritability, fatigue, weight loss, weight gain, and more.
Four common issues associated with the thyroid include Hashimotos thyroiditis, Graves disease, goiter , and thyroid nodules. Keep reading to learn about common thyroid disorders and diseases as well as their symptoms and treatment.
In hyperthyroidism, your thyroid gland is overactive. It produces too much thyroid hormone. This can cause many of your bodys functions to speed up.
Hyperthyroidism affects between 1 and 3 percent of people in the United States and is more common in women.
Graves disease is the most common cause of hyperthyroidism, affecting about 70 percent of people with an overactive thyroid. Nodules on your thyroid a condition called toxic nodular goiter or multinodular goiter can also cause the gland to overproduce its hormones.
Hyperthyroidism can also be caused by:
- thyroid gland inflammation
Don’t Miss: Parkinson’s Sleeping All The Time
What Are The More Serious Complications Of Hyperthyroidism
People with advanced and extreme hyperthyroidism face a ramshackle of problems, some of them life-threatening. The good news, though, is many patients do not reach this level of severity. Complications can include:
- Graves ophthalmopathy or Thyroid Eye Disease , which may soon be treatable using a new drug called Teprotumumab
- Irregular heartbeat, which can lead to:
Bottom line: The longer you have an overactive thyroid and go without treatment, the greater the risk of lifelong complications, even after treatment. As over 60 percent of people with thyroid disease go undiagnosed, its important to listen to your body before reversible symptoms like weight loss and insomnia become life-threatening issues such as irregular heartbeat , bone loss , and infertility .
Do One Thing Right Now
Relax! Slowing things down is keyeven if it feels counterintuitive with all the sped up effects of the condition. The GDATF recommends practicing yoga, Tai Chi, self-hypnosis, and meditation.
Dementia Case Finding Procedures
Dementia and its subtypes were identified in a multi-step case-finding procedure, described in detail elsewhere . In brief, all participants underwent neuropsychological screening with the 100-point Cognitive Abilities Screening Instrument , a measure of global function that has been validated in English and Japanese . Diagnosis was based on neuropsychologic testing using the Consortium to Establish a Registry for Alzheimer Disease battery, a neurologic exam and an informant interview. Those with dementia received a work-up with neuroimaging and blood tests. All recognized subtypes of dementia were considered in the diagnostic consensus conference that included a neurologist and at least two other study investigators. Dementia was diagnosed according to DSM-III-R criteria , probable and possible AD according to National Institute of Neurological and Communicative Disorders and Stroke-Alzheimer Disease and related Disorders Association criteria , and vascular dementia according to California Alzheimer Disease and Treatment Centers criteria . The remaining subtypes included subdural hematoma, Parkinson disease, cortical Lewy body disease, Pick disease, and cause not determined. Among participants who received autopsy evaluation, approximately two-thirds of the clinical Alzheimer cases met CERAD neuropathologic criteria for AD .
Recommended Reading: 5 Signs You Ll Get Parkinsons
You May Like: Tremor-dominant Parkinson’s Disease
Can Parkinsons Symptoms Come And Go
Over time, the bodys ability to convert levodopa into dopamine decreases, meaning the helpful effects of the medication will wear off more quickly and off episodes will arrive more quickly. The symptoms can come and go with suddenness, prompting some to compare it to turning a light switch on and off.
A Critical Reappraisal Of The Worst Drugs In Parkinsons Disease
What are the worst drugs for Parkinsons disease patients? Couldnt a simple list be assembled and disseminated to the Parkinson community? Recently Ed Steinmetz, an experienced neurologist in Ft. Meyers, FL pointed out to me, a list approach published in the Public Citizen Newsletter . The approach was to list every drug associated with a single confirmed or unconfirmed symptom of Parkinsons disease or parkinsonism. Parkinsons disease is defined as a neurodegenerative syndrome , whereas parkinsonism encompasses a wider net of drug induced and other potential causes. In parkinsonism symptoms are similar to Parkinsons disease, but patients do not have Parkinsons disease. Patients and family members confronted with a simple drug list approach may falsely conclude that most medicines are bad for Parkinsons disease, and that any medicine may cause parkinsonism. This concept is in general, incorrect. Although the approach is well-meaning, it is in need of a major revision, as Parkinsons disease and parkinsonism are too complex to summarize by simple lists. In this months column I will try to summarize the key information that patients and family members need to know about the worst pills, for Parkinsons disease and parkinsonism.
A Florida Parkinsons Treatment Blog by Michael S. Okun, M.D.
UF Center for Movement Disorders & Neurorestoration, Gainesville FL
Recommended Reading: Loud Program For Parkinson’s
What Are The Causes Of Pseudoparkinsonism
Pseudoparkinsonism is a drug reaction. Its often caused by medications that block dopamine receptors in the brain. Dopamine is the brain chemical your body needs to make smooth motions and to move with purpose and intent.
An interruption to the dopamine flow is similar to what causes Parkinsons disease in this case, the nerve cells stop making enough dopamine. When someone has pseudoparkinsonism, their body is still making enough dopamine, but a drug reaction keeps their body from using it properly.
There are a wide variety of medications that can sometimes cause pseudoparkinsonism. Medications for mental health conditions, digestive conditions, arrhythmias, and seizures, along with some blood pressure medications, can lead to pseudoparkinsonism.
Medications most likely to cause pseudoparkinsonism include:
I Feel Wonderful And Theres A Reason Why
Actually, there are three fantastic reasons:
First and foremost: I have tackled the loss of dopamine by working on the underlying cause of that loss.
We know that cell loss in the substantia nigra is the direct cause of dopamine loss. I address that cell loss in gentle but powerful ways and so protect dopamine levels.
Second, I increase dopamine production in my brain using non-drug methods. Increasing dopamine fights this condition head-on leading to wonderfully quick improvements.
Third, I have taken each of the symptoms of my illness stiffness, shaking, anxiety and so on and addressed them directly. Ive enacted specific daily habits that make those symptoms reduce to almost nothing.
Read Also: Is There A Blood Test To Check For Parkinson’s Disease
Parkinsons Misdiagnosis: Depression Or Anxiety
It is shocking how many times Parkinsons is dismissed as nothing more than anxiety or depression. It is true that physical symptoms can sometimes result from mental conditions. However, reducing PD to a mental condition is usually the result of not enough testing or not taking enough time to talk to a patient.
My husband was diagnosed with anxiety.
My husband was diagnosed with anxiety and low testosterone years before his diagnosis.
Yes they said it was all in my head!
Mental illness.
Thyroid Dysfunction Could Increase Risk Of Parkinson Disease
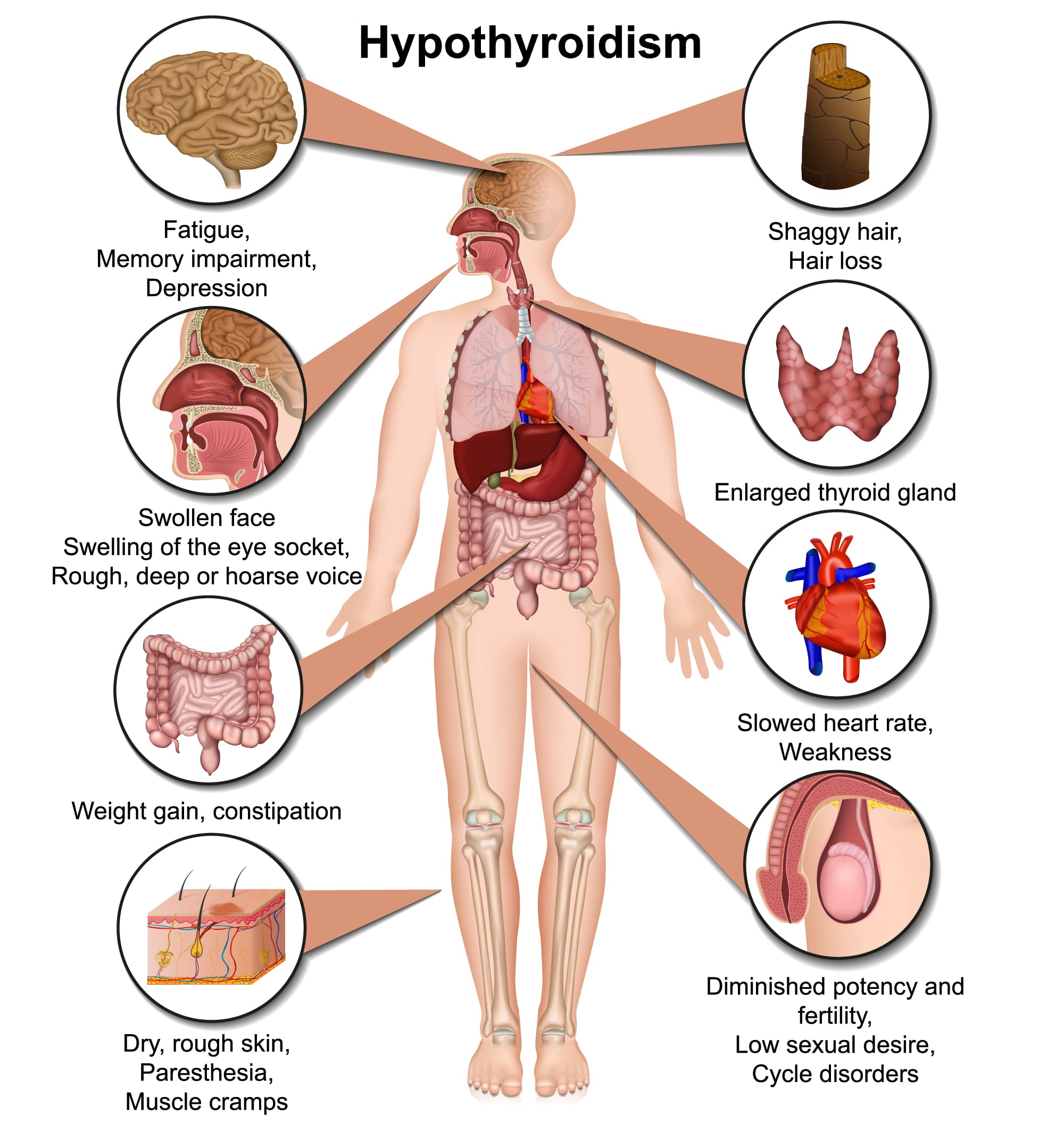
A systematic review and meta-analysis from AACE 2022 provides an overview of the potential associations between thyroid dysfunction, including both hypothyroidism and hyperthyroidism, and risk of Parkinson disease.
Patients with thyroid disorders may be at an increased risk of Parkinson disease, according to the results of a new study.
Presented at the American Academy of Clinical Endocrinology annual meeting, results of the systematic review and meta-analysis indicate patients with hypothyroidism and hyperthyroidism were at a 1.5 times greater risk of developing Parkinson disease.
Studies suggest patients with thyroid dysfunction may have an increased risk of developing Parkinson disease. However, the results from existing studies are inconsistent, said Nipith Charoenngam, MD, a postdoctoral research fellow at Boston Medical Center, during his presentation. Therefore, we aimed to investigate the association between hypo and hyperthyroidism with risk of Parkinson disease using the method of systematic review and meta-analysis.
Upon analysis, results indicated there was an increased likelihood of Parkinson disease was greater among those with hypothyroidism and those with hyperthyroidism . Investigators pointed out funnel plots for both meta-analyses were fairly symmetric, which led them to believe there was little evidence of publication bias.
Related Content:
Also Check: What Chemicals Cause Parkinson’s Disease
