What Are The Symptoms
Symptoms of PD vary from person to person, as does the rate of progression. A person who has Parkinson’s may experience some of these more common “hallmark” symptoms:
- Bradykinesia – slowness of movement, impaired dexterity, decreased blinking, drooling, expressionless face.
- Tremor at rest – involuntary shaking that decreases with purposeful movement. Typically starts on one side of the body, usually the hand.
- Rigidity – stiffness caused by involuntary increase in muscle tone.
- Postural instability – sense of imbalance. Patients often compensate by lowering their center of gravity, which results in a stooped posture.
Other symptoms that may or may not occur:
Freezing or being stuck in place Shuffling gait or dragging of one foot Stooped posture Cognitive impairment
New Research Puts Serotonin At The Heart Of Parkinsons
In a seminal research paper, published in Lancet Neurology, researchers from King’s College London have used brain scans to uncover early changes in the brain that may happen years before the symptoms of Parkinson’s appear.
The study looked at serotonin signalling in the brains of people with extremely rare genetic mutations that meant they had a very high risk of developing Parkinson’s in the future.
They showed that changes in serotonin signalling may happen in the earliest stages of Parkinson’s – before significant loss of dopamine-producing cells. The changes could also be found ahead of dopamine cell loss in other areas of the brain, as the condition progressed.
Comparisons Of Urinary Metabolite Levels Between Pd And Control Groups
Figures 2AC show the levels of urinary HVA, VMA, and 5-HIAA and the HPLC chromatograms of the control and PD groups, respectively. The urinary HVA level was significantly higher in PD patients than in control subjects . The urinary VMA level was not significantly different between the PD and control groups . On the other hand, the urinary 5-HIAA level was significantly lower in PD patients than in control subjects .
Figure 2. Comparisons of urinary HVA , VMA , and 5-HIAA levels and HPLC chromatograms between control subjects and PD patients . Data are presented as mean ± SEM .
Read Also: What Are Early Warning Signs Of Parkinson’s Disease
What Is A Receptor And What Is Its Role In Serotonin Deficiency
There are two types of receptors: presynaptic and postsynaptic. Presynaptic receptors are designed to regulate the release of neurotransmitters from the synaptic cleft. The synaptic cleft is the space between neurons that allows the exchange of information to occur.
Postsynaptic receptors are designed to receive the signal from the presynaptic receptor. In the event that these receptors are not functioning properly or there are not enough of them, low serotonin levels can result.
Serotonin And Parkinsons Disease

PD patients and PD animal models showed serotonergic neuronal loss and Lewy bodies within serotonergic neurons . Moreover, serotonin levels and SERT expression are reduced in several nuclei in PD . However, several findings indicate that the loss of SERT is not correlated with the disease duration and disability . In the basal ganglia, changes in receptor expression were also observed, such as the increase in 5-HT2C levels and a decrease in 5-HT1A expression . Nevertheless, the differential expression of these receptors between regions and discrepancies between different studies using PD models have also been published . Serotonin signaling modulates the RhoA/Rho kinase pathway , which is involved in neuroinflammation and neurodegenerative disorders such as PD . In PD, serotonin dysfunction, together with the noradrenergic dysfunction , are involved in non-motor symptoms such as depression, weight loss, fatigue, and sleep disturbances. Recent studies have shown that administration of the serotonin precursor 5-hydroxytryptophan improves depressive symptoms in PD patients . Furthermore, serotonin dysregulation leads to motor alterations such as tremor, L-DOPA-induced dyskinesia , and graft-induced dyskinesias .
Don’t Miss: Can Parkinson’s Run In The Family
Outside The Nervous System
In the digestive tract
Serotonin regulates gastrointestinal function. The gut is surrounded by enterochromaffin cells, which release serotonin in response to food in the lumen. This makes the gut contract around the food. Platelets in the veins draining the gut collect excess serotonin. There are often serotonin abnormalities in gastrointestinal disorders such as constipation and irritable bowel syndrome.
If irritants are present in the food, the enterochromaffin cells release more serotonin to make the gut move faster, i.e., to cause diarrhea, so the gut is emptied of the noxious substance. If serotonin is released in the blood faster than the platelets can absorb it, the level of free serotonin in the blood is increased. This activates 5-HT3 receptors in the chemoreceptor trigger zone that stimulate vomiting. Thus, drugs and toxins stimulate serotonin release from enterochromaffin cells in the gut wall. The enterochromaffin cells not only react to bad food but are also very sensitive to irradiation and cancer chemotherapy. Drugs that block 5HT3 are very effective in controlling the nausea and vomiting produced by cancer treatment, and are considered the gold standard for this purpose.
Bone metabolism
Organ development
Cardiovascular growth factor
Several classes of drugs target the 5-HT system, including some antidepressants, antipsychotics, anxiolytics, antiemetics, and antimigraine drugs, as well as, the psychedelic drugs and empathogens.
Which Conditions Have Links To Dopamine And Serotonin
Having abnormal levels of either dopamine or serotonin can lead to several different medical conditions.
Both neurotransmitters can affect mood disorders such as depression. Imbalances can also result in distinct conditions that affect different bodily functions.
In the sections below, we cover these conditions in more detail:
You May Like: Parkinson Awareness Ribbon
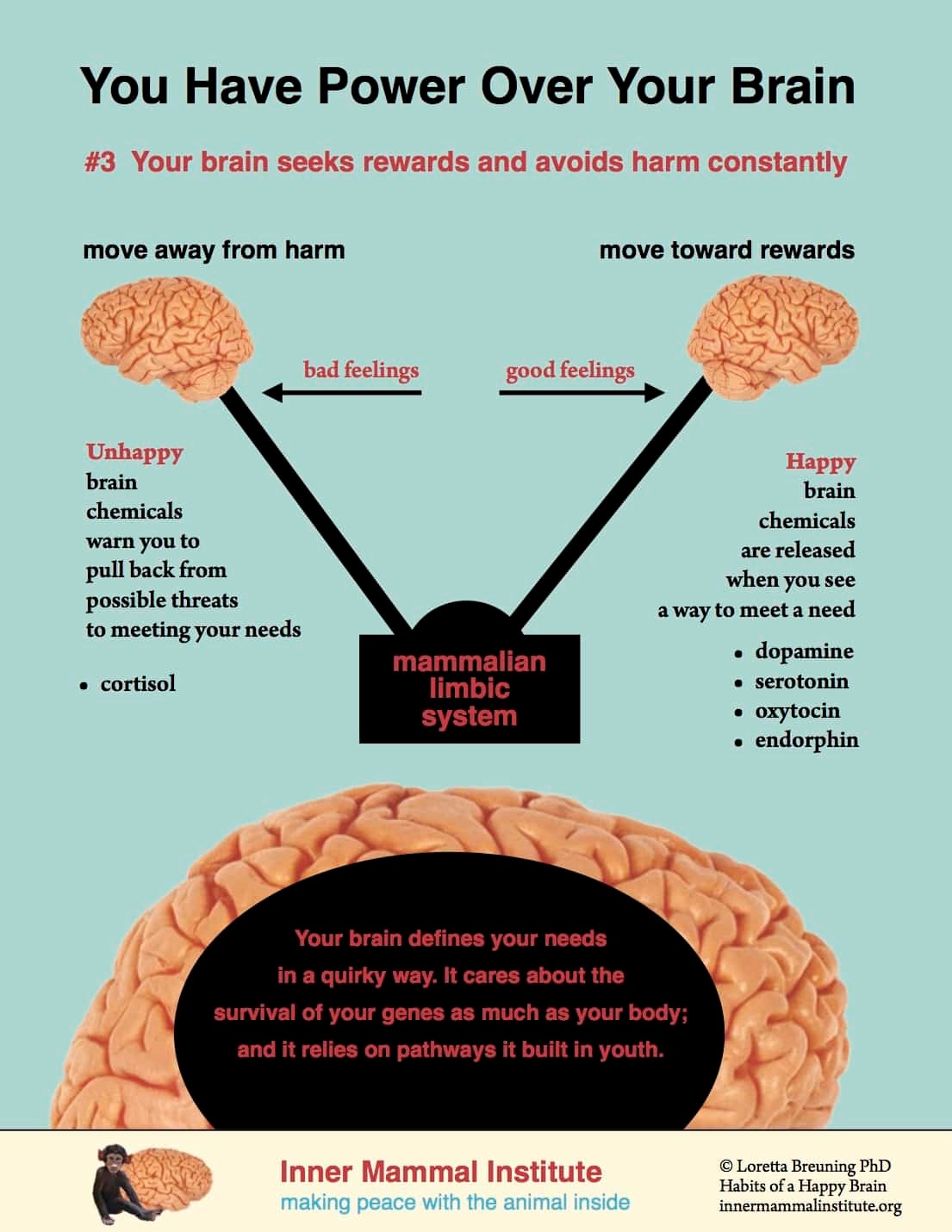
Chemical Messengers In Parkinson’s
There are a number of neurotransmitters that the brain uses to communicate. Dopamine is most commonly associated with Parkinson’s, with the condition causing the gradual loss of dopamine-producing cells.
But we now know that, while changes in dopamine account for many of the motor symptoms of Parkinson’s, changes in other neurotransmitters like serotonin may play more of a role in symptoms such as sleep problems, fatigue and anxiety. And we know that some people with Parkinson’s experience symptoms like these many months and even years before being diagnosed with the condition.
Research has previously shown associations between Parkinson’s and serotonin, often thought of as the happy hormone, but this is the first study to show that changes in serotonin signalling may be an early consequence of Parkinson’s, challenging the traditional view of what causes the condition.
Dr Beckie Port, Research Communications Manager, says:
“This is one of the first studies to suggest that changes in serotonin signalling may be an early consequence of Parkinson’s.
“Detecting changes that are happening in the brain in these early stages is a crucial gap in Parkinson’s research at the moment. Picking up on the condition earlier and being able to monitor its progression would aid the discovery of new and better treatments that could slow the loss of brain cells in Parkinson’s.
Comparisons Of Plasma Monoamine Levels Between Pd And Control Groups
Figures 1AD show the levels of plasma monoamine and represent their HPLC chromatograms of the control and PD groups. The plasma DA level was not significantly different between PD patients and control subjects . The plasma NE level was significantly higher in PD patients than in control subjects . Compared to control subjects, PD patients had a significantly lower plasma EPI and 5-HT levels .
Figure 1. Comparisons of plasma DA , NE , EPI , and 5-HT levels and HPLC chromatograms between control subjects and PD patients . Data are presented as mean ± SEM .
Don’t Miss: What Kind Of Effect Does R-dopa Have On Parkinson’s Disease
Serotonin Hypothesis Of Depression
Serotonin is mainly produced in the dorsal raphe nucleus . Serotonin transporters take up released serotonin from the synaptic cleft into serotonergic neurons in a manner that helps to modulate various functions in the brain including mood and emotion . The striatum, the amygdala, and the prefrontal cortex are regions of the brain that are innervated by serotonergic neurons . These brain regions including the dorsal raphe nucleus which is part of the brains serotonergic system, are activated during early maternal stress . Abnormal 5-HT levels in these brain areas have been associated with depression . Pre-clinical and clinical studies have demonstrated that early life stress affects 5-HT levels in the brain and this may lead to depression . Selective serotonin re-uptake inhibitors are a class of antidepressant drugs commonly used to treat depression . SSRIs work by blocking 5-HT re-uptake thus increasing the availability of 5-HT in the synaptic cleft as well as its chance to bind to receptors in the post-synaptic membrane . Therefore, by restoring the levels of monoamines and their transporters in the brain, SSRIs drugs are appropriate treatments to address early life stress dysfunction that predisposes to depression later in life.
Differences Between Serotonin And Dopamine
Although both dopamine and serotonin have positive associations, as serotonin stabilizes mood and dopamine signals rewards, they have other distinct functions in the body as well.
Their core functions are quite different. Dopamine brings feelings of pleasure and provides a happiness boost, while serotonin is more of a stabilizer than a booster.
-
Enhances impulsive behavior
Read Also: Parkinson’s Mayo
Testing For Low Levels
Serotonin levels vary over time. Sometimes, a person will have no symptoms of depression, or any other serotonin-associated health condition, despite having low levels of serotonin.
If a doctor suspects that serotonin may be the cause of an underlying health condition, they may conduct a range of tests, such as depression surveys or memory tests.
They may also test serotonin levels, though they tend to reserve this for when they suspect a serotonin-secreting tumor.
Serotonin helps the body regulate many functions, including mood.
When serotonin is either too low or too high, a person may develop mental health symptoms.
The physical maladies that low serotonin causes, such as erectile dysfunction and movement disorders, can also impact a persons mental health.
Healthcare professionals do not fully understand why some people develop serotonin deficiency.
However, some potential causes
Interactions Between Serotonin And Other Neurotransmitters In The Basal Ganglia
Several studies have highlighted a crucial role for the interactions between serotonergic and other neurotransmitter systems in movement control and pathophysiology of the basal ganglia , and particularly PD .
Figure 1. Schematic representation of the major neuronal neurotransmitter systems acting on striatal projection neurons. Interactions between serotonergic, glutamatergic, and dopaminergic systems control the activity of striatal neurons for correct regulation of movement. Abnormal interactions lead to abnormal movement and neurological disorders such as Parkinsons disease , L-DOPA-induced dyskinesia or graft-induced dyskinesia . Abbreviations: SNc, substantia nigra pars compacta DRN, dorsal raphe nucleus 5-HT, serotonin DA, dopamine, GLUT, glutamate. The figure was produced using Servier Medical Art .
You May Like: What Are Early Warning Signs Of Parkinson’s Disease
The Case Of Fluvoxamine Maleate
The role of serotonergic drugs in PD associated with depression has been receiving considerable attention amongst the research community . As a link between DA and the development of depression in patients with PD has been suggested, the pathophysiological features of both PD and depression have in common DA pathway dysfunction and depletion and/or 5-HT deficit . It has been suggested that an increase in serotonergic tone may indirectly influence DA function and may contribute to increased motor activity which is partially blocked by DA antagonists . Studies have shown that depression may be associated with an abnormal level of DA . As studies have also shown that brain regions affected by abnormal DA processing may also be affected when 5-HT is abnormally processed, we hypothesize that Fluvoxamine maleate treatment may play a role in improving the chemical imbalance caused by low levels of DA in the brain .
How Is It Diagnosed
Its hard to diagnose a serotonin deficiency because theres no way to accurately test the amount in your brain, and there are no specific diagnostic criteria.
While there is a test that measures serotonin in your blood, its generally only used to check for serotonin-producing tumors outside of the brain. Also, blood serotonin levels dont necessarily reflect the levels in your brain.
Steer clear of neurotransmitter urine tests that are available online. A 2010 analysis debunked claims that these tests can help to diagnose serotonin deficiency in the brain.
Your brain is surrounded by a membrane called the blood-brain barrier . This membrane is semi-permeable, meaning it lets some things through but not others. Serotonin is one substance that cant pass through the BBB.
This means that serotonin in your brain generally must be produced in your brainstem, making the levels in your blood and urine an unreliable measurement of the amount in your brain.
If you think you have symptoms of a serotonin deficiency, its best to track your symptoms for a few weeks and work with your doctor to narrow down a diagnosis.
Regardless of whats causing a serotonin deficiency, there are a few proven ways to increase serotonin functioning, both in your brain and the rest of your body.
Don’t Miss: Wehaveparkinsons
Other Complementary Therapies For Anxiety In Pd
Complementary therapies are a growing group of treatments which may improve the symptoms of PD without medication. I have written past blogs on two complementary therapy approaches for several symptoms of PD art therapy and music therapy.
Various complementary therapy modalities have been developed that may lower stress and anxiety in PD. These include yoga, massage, the Alexander technique, neurofeedback and others. Some of these therapies have been studied in small trials with data suggesting that they may be helpful for the anxiety of PD. Others have not yet been studied, although anecdotally, people with PD may feel that they are very useful in combatting anxiety. In general, this group of therapies may be effective for the anxiety of PD but needs to be studied more rigorously.
How Is A Diagnosis Made
Because other conditions and medications mimic the symptoms of PD, getting an accurate diagnosis from a physician is important. No single test can confirm a diagnosis of PD, because the symptoms vary from person to person. A thorough history and physical exam should be enough for a diagnosis to be made. Other conditions that have Parkinsons-like symptoms include Parkinsons plus, essential tremor, progressive supranuclear palsy, multi-system atrophy, dystonia, and normal pressure hydrocephalus.
You May Like: Is Sugar Bad For Parkinson’s Disease
Serotonin And Its Role In Autism Spectrum Disorder
In regards to research for neurotransmitters and effects on patients with Autism Spectrum Disorder , 5-HT has been studied the most in terms of research efforts and investigations. As noted, 5-HT signaling does facilitate many neural processes including that of neurogenesis, cell migration and survival, synaptogenesis, and synaptic plasticity. It was noted that 45% of tested ASD subjects contained high levels of 5-HT in their blood. In addition, investigations performed on ASD-like animal models reported that hyperserotonemia significantly reduced the motivation for social interest through inhibition of separation distress, which could be related in the ASD patients that have social impairments.
Environmental Toxins And Parkinsons Disease
Neuronal cell death in PD may also be triggered by exposure to toxic substances or environmental factors which precipitate the symptoms of the disease as they render the brain vulnerable to subsequent physiological chronic stress . The environmental cause of PD mainly refers to exposure to dopaminergic toxins 6-hydroxydopamine , 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine , paraquat and rotenone as these toxins are known to induce formation of reactive oxygen species and oxidative stress which may result in neuronal cell death .
DA is one of the common neurotransmitters present in most parts of the central nervous system . The mesocortical, mesolimbic, nigrostriatal and tubero-infundibular pathways are the four main pathways that play a key role in dopaminergic signaling . DA cannot cross the blood brain barrier, therefore, it is synthesized from tyrosine which is carried into the brain via amino acid transporters . At the dopaminergic neuron level, tyrosine is then converted into dihydroxyphenylalanine by tyrosine hydroxylase then finally into DA by aromatic L-amino acid decarboxylase . DA is then stored in the vesicle until an action potential allows the vesicle to be discharged into the synapse . Monoamine oxidase is the enzyme that is responsible for breaking down excess DA and is known to similarly act on 6-OHDA inducing oxidative stress resulting in apoptosis .
Read Also: Parkinson Awareness Ribbon Color
Is Serotonin Pathology A Good Biomarker In Vivo For Early Parkinsons Disease
Celia Painous1,2,3,4, Andres Perissinotti5, Maria J. Martí1,2,3,4
1Parkinsons Disease & Movement Disorders Unit, Hospital Clínic Barcelona DIBAPS-Institut d’Investigacions Biomèdiques August Pi i Sunyer , Centro de Investigación Biomédica en Red sobre Enfermedades Neurodegenerativas , Spain 5Nuclear Medicine Department, Hospital Clínic Barcelona & Biomedical Research Networking Center in Bioengineering, Biomaterials and Nanomedicine , Barcelona , Spain
Correspondence to:
Provenance: This is an invited article commissioned by the Section Editor Dr. Zhangyu Zou .
Submitted Aug 30, 2019. Accepted for publication Sep 12, 2019.
doi: 10.21037/atm.2019.09.80
The article shows very interesting results, favoring the use of -DASB PET as an even earlier marker than -F-PCIT SPECT in that subgroup of patients with A53T SNCA mutation and suggesting homologous results in iPD. Finding markers capable of identifying patients with an increased risk of developing PD at a prodromal stage is a paramount. These prodromal tracers could grant earlier diagnosis and treatment not only improving patients quality of life but also allowing enrollment into clinical trials with potential neuroprotective medications.
Neurotransmitter And Metabolite Levels Determination
Specimen Collection
Plasma and urine were obtained to determine the neurotransmitter and metabolite concentrations, respectively. Blood samples were collected from a cubital vein, drawn into an EDTA tube, immediately centrifuged to separate plasma at 3,000 ×g for 10 min, and stored at 80°C until analyzed. Plasma DA, NE, EPI, and 5-HT were measured by HPLC with an electrochemical detector. At the same time, a single urine sample was collected in a container with 10 ml hydrochloric acid per liter of urine and pH was adjusted to 12. In these urine samples, the levels of homovanillic acid , vanillylmandelic acid , and 5-hydroxyindoleacetic acid , metabolites of DA, NE/EPI, and 5-HT, respectively, were quantified.
HPLC Analysis
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
