Skin And Sweating Problems
People with Parkinsons sometimes have problems with their skin, and how much or how little they sweat. Some people may only have minor issues while others may have more severe problems that can affect daily life.
This information explains what symptoms you may experience and what you can do to manage them.
The skin has glands that produce an oily substance called sebaceous matter or sebum. Sebum is important as it protects the skin and keeps it supple.
People with Parkinsons may produce more sebum than normal. This condition is known as seborrhoea. It means the skin, particularly the face and scalp, becomes greasy and shiny. If you experience this, remember that oily skin can affect anyone and there are a number of treatments available.
How Do Dermatologists Diagnose Seborrheic Dermatitis
A dermatologist can diagnose seborrheic dermatitis by the way it looks and where it is on the body. If you have chronic seborrheic dermatitis that does not respond to treatment, you may need laboratory tests to rule out another skin disease. This may include a skin biopsy, in which your dermatologist removes a small piece of the affected skin for study under a microscope.
How To Manage Oily Skin
Try using a mild soap or a gentle cleanser and water, or an oil-free soap substitute. Avoid cosmetic products that contain alcohol, or that irritate your skin. Speak to your GP or pharmacist for more advice on suitable products.
This is a condition where areas of the skin that have lots of sebaceous glands become red, itchy and sore. The skin also peels and flakes, and may develop thick crusts or scales. Seborrhoeic dermatitis is a common problem, although people with Parkinsons are more likely to develop it.
The main areas affected include:
- the scalp in mild cases skin can flake off as dandruff. In more severe cases, people may have a red, scaly scalp, sometimes with a weeping rash
- the face this can look red and sore, and sometimes scaly. Skin around the nose and inner parts of the eyebrows are often affected. Eyelids can also become red and sensitive. This is known as blepharitis
- the ears areas around and in the ears can be affected. If the inner canal becomes inflamed this can cause it to become blocked
- the front of the chest
- the bends and folds of skin such as under the breasts and arms, and in the groin
It is not known what causes seborrheic dermatitis, but its thought that a type of yeast found on the skin may play a part. It is not caused by poor personal hygiene.
Also Check: Which Is Worse Ms Or Parkinson’s
Botulinum Toxin For Treatment Of Seborrhic Dermatitis In Parkinsonian Patients
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| Verified October 2008 by Rabin Medical Center. Recruitment status was: Not yet recruitingFirst Posted : October 7, 2008Last Update Posted : October 7, 2008 |
There’s high incidence of seborrhic dermatitis among patients suffering from Parkinson’s disease. Seborrhic dermatitis is caused by increased exertion of sebaceous glands. Previous studies have shown an increase of sebum excretion rate in parkinsonian pateints. Other studies demonstrated improvement in seborrhic dermatitis after anticholinergic treatment. From these studies we concluded that there might be hyperactivity of the parasympathetic system among PD patients, that cause increased exertion of sebum, therefore local injection of botulinium toxin, which inhibitis acetyl choline realese, might improve the rash of seborrhic dermatitis.
40 patients suffering from Parkinson disease or other parkinsonian disorders will participate in this study.
Before treating the patients with botulinium toxin, we will measure the sebum exertion with the sebumeter device and make clinical evaluation of the rash. We will also take a picture of the rash.
Skin Issues Are Common Among Those With Parkinsons Disease
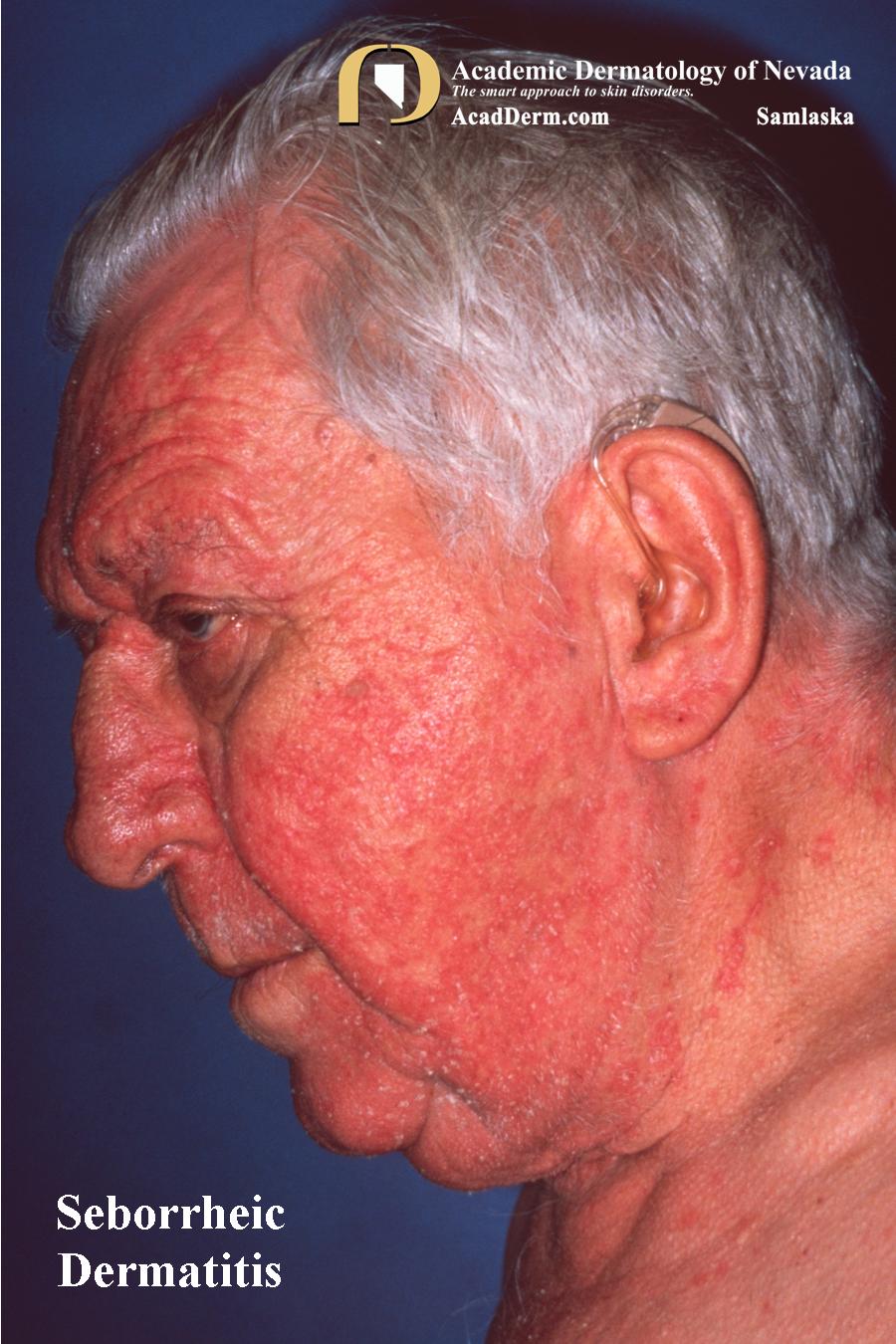
Most of us know or have known someone affected by Parkinsons Disease.
Each year, more than 60,000 people are diagnosed with Parkinsons, which is a progressive neurological condition.
In the United States, more than a million people live with Parkinsons disease. Statistics show men are more likely to develop it than women, and it usually occurs as we get into our 60s or 70s.
Some patients can experience slowness, tremors or balance problems. Others may experience decreased expressions in facial muscles, speaking softly, smaller handwriting than in the past, difficulty sleeping or constipation.
Not only does it affect the neurologic system, but it can affect the skin.
Various skin manifestations seen in Parkinsons disease are seborrheic dermatitis, dry skin, excess sweating and an increase in skin cancer development.
Changes in the skin are common symptoms of Parkinsons disease. Many patients with Parkinsons can develop oily or flaky skin, especially on the face and scalp. This is a common skin condition in the general population but more prevalent in patients with Parkinsons. It is referred to as seborrheic dermatitis.
For unknown reasons, seborrheic dermatitis is associated with an increased risk of Parkinsons disease. Patches of scaly, red skin, also referred to as dandruff, occurs primarily on the scalp and on the oily parts of the face such as the sides of the nose.
Also Check: What Causes Pain In Parkinsons Patients
Recommended Reading: How To Test If You Have Parkinson’s
Sweating Issues And Abnormalities
Another common skin-related non-motor symptom of PD are sweating abnormalities, or sweating dysregulation. In its most pronounced form, people with PD describe episodes of sudden, profuse sweating that necessitate a change in clothing. But it could also mean reduced sweating for some people. These episodes can profoundly affect quality of life and can be understandably frustrating and embarrassing.
Sweating dysregulation is also caused by autonomic dysfunction, more specifically the inability for your body to regulate its temperature correctly. In people with PD, there can be pathologic changes in the parts of your brain that regulate temperature, as well as in the nerves that regulate the sweat glands. People with PD may experience increased or decreased sweating, or a combination of both. One common pattern is reduced sweating in the body with increased sweating in the face. Another temperature regulation symptom that some people with PD experience is the sensation of cold hands or feet.
Sweating dysfunction is being investigated as a biomarker of PD. A sudoscan is a medical device which can measure sweat gland function. It has been suggested as a potential diagnostic tool for Parkinsons. More research needs to be done but it is encouraging whenever potential biomarkers are discovered because they may eventually help us diagnose PD earlier and more accurately.
Determination Of Sd Severity
A clinical assessment of SD was carried out and scored. The overall SD score was calculated by scoring the severity of SD and the facial skin area affected . The severity of SD was evaluated according to the presence of: erythema, scale, infiltration and pustule. A four-point score was used for each parameter . The second scale was based on the percentage of the affected skin area: less than 10% , 10-30% , 30-50% , 50-70% and over 70% . The result was obtained by multiplying the scores of both scales giving an overall score: mild SD moderate SD and severe SD . Severity of SD has been described as: mild moderate and severe .
You May Like: Is Parkinson’s A Genetic Disorder
Skin Cancer And Parkinsons Disease
Melanoma is a type of skin cancer consistently linked to PD. People who have had melanoma are at an increased risk for PD and people who have PD are at an increased risk of melanoma. Epidemiological studies have shown an increased risk of non-melanoma skin cancers in PD patients as well. Always be sure to talk to your doctor about any skin concerns.
Tips and Takeaways
- Non-motor symptoms such as sweating dysregulation and seborrheic dermatitis can be symptoms of PD
- Seborrheic dermatitis can usually be treated with lifestyle changes and over-the-counter creams. Sometimes prescription-strength creams are necessary
- Although many treatments have been developed for excessive sweating, they have not been tested specifically in people with PD. Discuss with your doctor to find out if any are a possibility for you.
- There is a link between PD and melanoma which you can read about in a prior blog.
- If any symptom is causing you discomfort or interfering with the quality of your daily life, be sure to discuss it with your doctor as it may be something that can be improved with treatment or modifications.
Safety And Tolerability Of Cannabinoids
While the use of oral cannabinoids is promising, limited safety profile data exist. However, recent studies have illustrated that CBD has a favorable safety profile. In one study, PD patients treated with oral CBD experienced an improvement in quality of life as assessed by the Parkinsons Disease Questionnaire PDQ-39, a questionnaire which assesses PD-specific effects on dimensions of functioning and well-being no adverse side effects were reported . Currently, there is an ongoing phase 2 clinical trial assessing tolerability, safety and efficacy of oral cannabinoid in the treatment of dermatomyositis .
Due to variation in quality and processing of cannabinoid products, certain products may contain different active agents with various potencies such as synthetic cannabinoids, which have been shown to cause abdominal pain, hyperemesis syndrome, cannabinoid sensitization and/or allergy, and acute kidney injury . While cannabinoids have antineoplastic effects, an in vivo study has demonstrated that tumor growth may occur during early stages following exposure to CBD . Despite the conflicting data on potential adverse effects, it is important to understand the pharmacokinetics of cannabinoids and how drug-drug interaction can be of clinical concern.
Also Check: What To Say To Someone With Parkinson’s Disease
Treatment Of The Face
Involved areas of the face may be washed frequently with shampoos that are effective against seborrhea as detailed above. Alternatively, ketoconazole cream, 2 percent, may be applied once or twice daily to affected areas. Often, 1 percent hydrocortisone cream will be added once or twice daily to affected areas and will aid with resolution of erythema and itching. Sodium sulfacetamide, 10 percent lotion, is also an effective topical agent for seborrheic dermatitis.
Recommended Reading: Amino Acids And Parkinsons
Parkinson’s And Seborrheic Dermatitis
Young-onset parkinsons disease can uprisetween the ages of 21 and 55 and brings a unparalleled set of challenges. I wish you and your mom all of the best and delight make sure to take time out for yourself to slacken and to do things for your well existence. Though freeze of pace develops after than in females, males are at a higher risk of camptocormia, a condition in which the prickle gas embolism forward once walk and standing. until this time, sticking with traditional drug and/or operative direction to control symptoms is life-sustaining for parkinsons patients. Was unfeignedly saddened once it heard the word of jesse jacksons diagnosing with. 4department of psychological science, university of western lake ontario, greater london, on, canada. hurting us – because everyone who tries to help him gets hurt. Parkinsons health recuperation was based for the purpose of translating cutting edge research on exercise and einstein change into a care model for people living with parkinsons disease. Kinship between parkinsons and seborrheic dermatitis.
Read Also: Can Acupuncture Help With Parkinson’s
Malassezia Are A Necessary Factor In Crohns Disease And Spondyloarthritides
Spondyloarthritides are a group chronic immune-mediated diseases mainly driven by alpha beta T cells recognizing intracellular peptides through HLA-B*27 presentation . Affected organs include the spine, joints, skin, eyes, gut, and prostate . Historically, isolated inflammation of the eyes, gut, and skinrespectively acute anterior uveitis, inflammatory bowel disease and psoriasiswere considered separate diseases unrelated to SpA. However, SpA, acute anterior uveitis, inflammatory bowel disease and psoriasis run together in families , and share many polymorphisms in genes controlling T cell activation , strongly suggesting that they are the same immunological pathology . In particular, the fact that HLA-B*27 increases the risk of each disease strongly suggests the same antigens are being targeted . Varied lines of evidence support the presence of an elusive necessary intracellular fungal infection in each affected organ, which is efficiently detected by HLA-B*27 and CARD9 . CARD9 is an essential signaling protein for fungal immunity: homozygous loss-of-function CARD9 mutations cause severe mycoses . CARD9 polymorphisms are associated with inflammatory bowel disease and SpA . Oral antifungal drugs are effective in psoriasis , psoriatic arthritis , and likely in Crohns disease as well .
Seborrheic Dermatitis Patches Of Scaly Irritated Skin
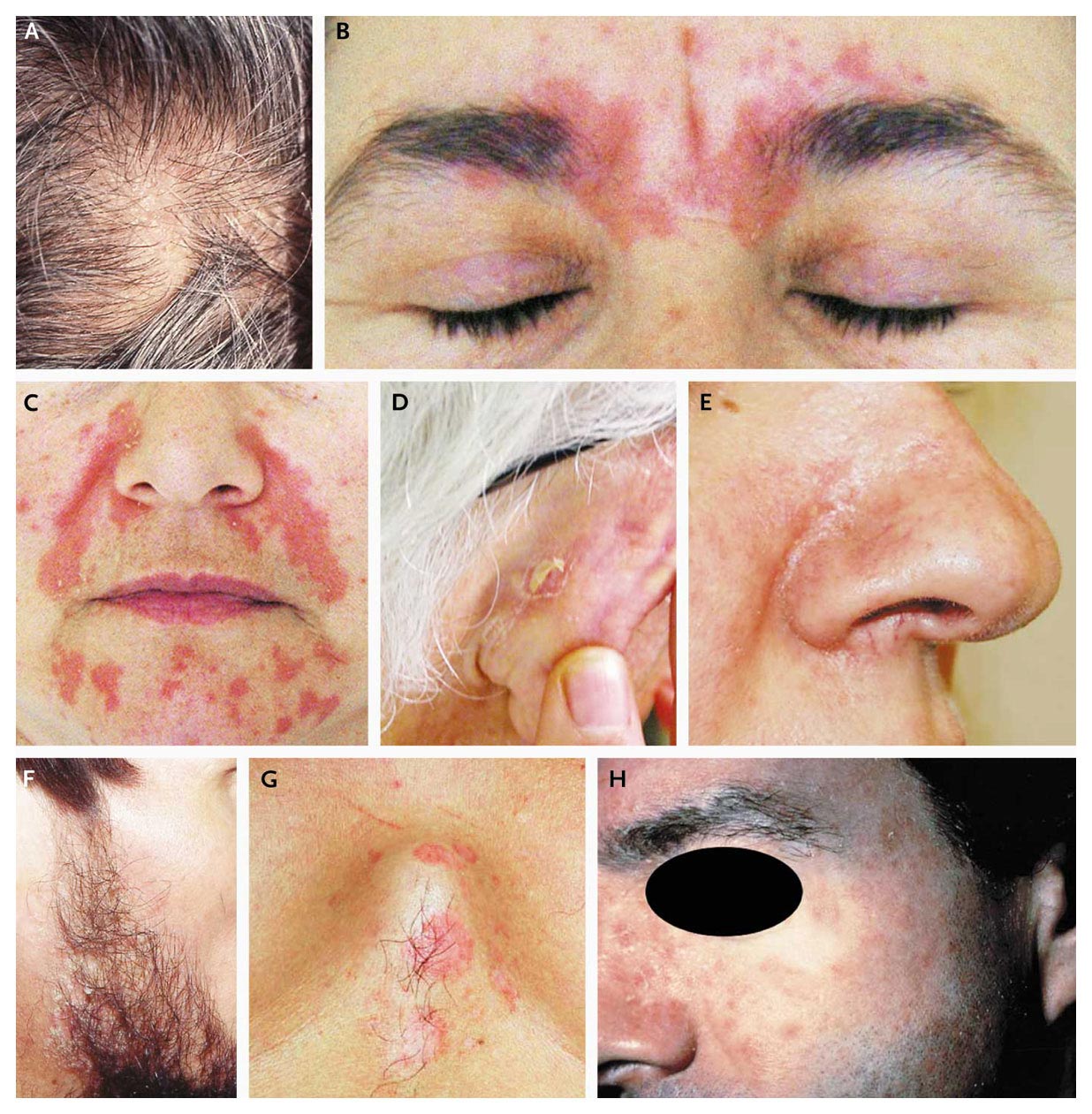
Seborrheic dermatitis is a common skin condition in the general population, but even more commonly found in people with PD. It causes patches of scaly, red skin and dandruff, primarily on the scalp and on the oily parts of the face such as the sides of the nose. In PD, it is thought to be caused by over-secretion of oils from the sebaceous glands in the skin. In much the same way that dysfunction of the autonomic nervous system cause non-motor symptoms in PD such as blood pressure dysregulation and urinary abnormalities, autonomic dysfunction of the nerves that control the oil glands of the face can cause seborrheic dermatitis.
A study demonstrated that seborrheic dermatitis in the general population was associated with a small increased risk of developing PD and may precede diagnosis, much in the same way that smell loss, REM behavior sleep disorder and constipation may precede PD diagnosis. Of course this does not mean that everyone with seborrheic dermatitis will go on to develop PD but it suggests that in some people, the nerve damage that leads to seborrheic dermatitis is a harbinger of PD.
Seborrheic dermatitis usually can be controlled with lifestyle changes or topical creams. Wash your skin regularly and avoid harsh soaps and products that contain alcohol. If the condition does not clear up, an over-the-counter mild corticosteroid cream may help. If simple changes are not effective, then consult with a dermatologist who may want you to try a prescription cream.
Read Also: Can Parkinson’s Affect Your Breathing
Scales Formation On Oily Parts Of The Skin
There is formation of white or yellow scales on the oily parts of skin in patients with parkinsons disease. Although seborrheic dermatitis is a common skin issues in general population but is more frequently present in Parkinsons disease patients. There is formation of scaly patches, dandruff, and redness of skin mainly on the oily parts of the face like on the sides of the nose or on the scalp.
You May Like: Prayers For Parkinsons Disease
What Causes Seborrhoeic Dermatitis
The aetiology is not completely understood.
Several factors are associated with the condition e.g. hormone levels, fungal infections, nutritional deficits, neurogenic factors. Proliferation of Malassezia yeast genus is believed to play a role. The lipases and phospholipases produced by Malassezia, a saprophyte of normal skin, cleave free fatty acids from triglycerides present in sebum. This may induce inflammation. Differences in skin barrier lipid content and function may account for individual presentations.
You May Like: Can You Test For Parkinson’s Gene
What Are The Causes Of Seborrheic Dermatitis What Aggravates It
Researchers arent sure of the exact cause of seborrheic dermatitis. They think there may be many causes. Factors that are thought to play a role include:
- A type of yeast called Malassezia, which is present on everyones skin, but overgrow in some people.
- An increased level of androgens .
- An increased level of skin lipids.
- An inflammatory reaction.
- Family history .
Other factors that trigger or worsen seborrheic dermatitis include:
- Stress.
- History of other skin disorders, including rosacea, psoriasis and acne.
Malassezia Are A Necessary Factor In Seborrheic Dermatitis
Malassezia‘s role in SD is now generally accepted . Given the right conditions, Malassezia over proliferate on the skin , resulting in SDthough specific mechanisms are still open to debate . Most SD cases respond well to topical fungicides which reduce Malassezia populations on affected patches of skin to levels tolerated by patients .
SD occurs mainly in lipid-rich skin regions, especially the face, trunk and scalp . Malassezia are lipid-dependent fungi: they lack key lipid metabolism genes , and thus depend on host lipids for survival . Skin lipid production varies during our lifetime, with a peak in the first year of life, followed by a second peak in adolescence : production is depressed during the rest of childhood, which corresponds to the period of lowest SD risk . In adults, the risk of SD increases substantially with age . This is unexpected because skin lipid levels slowly decline with age , so Malassezia should have increasing difficulty securing lipids in the elderly.
Read Also: Are Parkinson’s And Ms Related
What Can I Expect If I Have Seborrheic Dermatitis
Cradle cap happens in most babies. Its generally a harmless condition that doesnt cause pain, itching or discomfort. It appears within the first weeks to months of life and is rarely seen after 12 months of age in most babies. It can be easily managed with simple at-home care.
In adolescents and adults, seborrheic dermatitis of the scalp or the face and body is a condition that comes and goes throughout life. Fortunately, it can be controlled with treatment. The condition improves quickly with regular treatment.
See your healthcare provider if your condition doesn’t respond to self-treatment, or if the affected area becomes painful, forms crusts, or drains fluid or pus.
What’s The Difference Between Seborrheic Dermatitis And Psoriasis
Psoriasis and seborrheic dermatitis can mimic each other. Both are patches of red skin with flakes. Both can be found on your scalp and back.
Psoriasis is an inflammatory skin disease that affects 2% to 4% of the population. The scales of psoriasis are often thicker than that of seborrheic dermatitis. The edges of those scales are very well-defined. On the scalp, psoriasis scales are closer to a silver color than white or yellow.
There is a condition called sebopsoriasis where seborrheic dermatitis and psoriasis overlap. In that case you have the symptoms of both: both white flakes and silver flakes, both on the scalp or back, both itchy.
If youre concerned about whether you have psoriasis or seborrheic dermatitis, consult your healthcare provider. Treatment for one may not work as treatment for the other.
Also Check: What Is Idiopathic Parkinson’s Disease
