The Kensington Falls Church Memory Care Community
The Kensington Falls Church is an enhanced assisted living, Alzheimers care, dementia care, and memory care community located in Falls Church, Virginia.
Our Enhanced Assisted Living Residence license enables us to provide a higher continuum of healthcare thats not normally seen in other assisted living communities.
This includes employing a staff of registered nurses 24 hours a day who can administer medications and injections. This allows all of our residents to age in place, meaning they can stay in our community as long as theyd like, even as their healthcare needs change.
Our community is also uniquely capable of providing world-class care for people experiencing memory loss due to Alzheimers, Parkinsons, and Lewy body dementia.
We have two distinct memory care communities that provide care for people experiencing early to middle and late stages of dementia Haven and Connections.
Both our Haven and Connections neighborhoods are fully-secured environments that provide a higher level of care and supervision for our residents with memory loss.
Each community is specially designed to cater to the needs of our residents with memory loss, and feature wander technology to keep track of our residents, and also feature lots of sunlight in a homelife setting that fosters calm and comfort.
At the Kensington Falls Church, we extend Our Promise to you to love and take care of your family as we would our own.
What Causes Lewy Body Dementia
The causes of LBD are not yet well understood, but research is ongoing in this area. There are probably multiple factors involved, including genetic and environmental risk factors that combine with natural aging processes to make someone susceptible to LBD.
For more information, visit www.lbda.org.
Modified with permission from the Lewy Body Dementia Association
To learn more about motor symptoms related to Parkinsons, visit here.
To learn more about non-motor symptoms related to Parkinsons, visit here.
Dementia With Lewy Bodies And Neuroleptics
Neuroleptics, or antipsychotics, are strong tranquillizers sometimes prescribed for people with dementia to treat hallucinations or other behavior problems. However, if taken by people with LBD, neuroleptics may be particularly dangerous. This class of drugs can induce Parkinson-like side-effects, including rigidity, immobility, and an inability to perform tasks or to communicate.
If you or your loved one with Lewy body dementia is not unduly distressed by the hallucinations, it may be better to tolerate them rather than endure the side effects of the medication. If, however, you and your doctor decide to use a neuroleptic, this should be done with the utmost care and monitored carefully and regularly.
According to Lewy Body Dementia Association:
Up to 50% of patients with LBD who are treated with any antipsychotic medication may experience severe neuroleptic sensitivity, such as worsening cognition, heavy sedation, increased or possibly irreversible Parkinsonism, or symptoms resembling neuroleptic malignant syndrome , which can be fatal. .
Recommended Reading: Specialist Parkinson’s Nursing Homes
Lewy Body Dementia: A Common Yet Underdiagnosed Dementia
While its not a household word yet, Lewy body dementia is not a rare disease. It affects an estimated 1.4 million individuals and their families in the United States. Because LBD symptoms can closely resemble other more commonly known disorders like Alzheimers disease and Parkinsons, it is often underdiagnosed or misdiagnosed. In fact, many doctors or other medical professionals still are not familiar with LBD.
Causes Of Dementia With Lewy Bodies
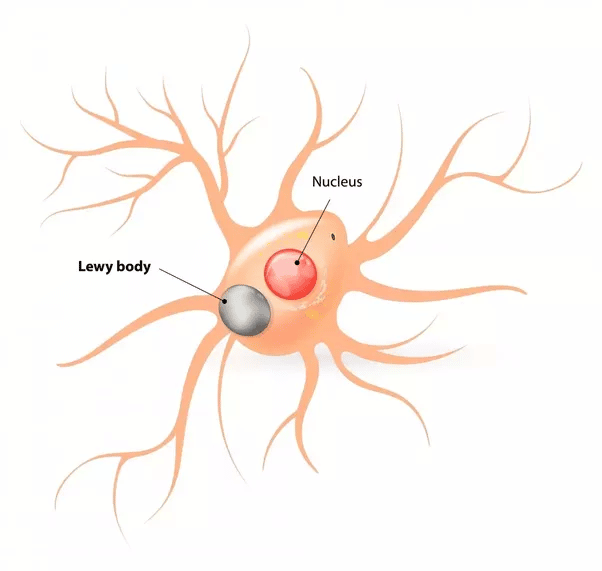
Dementia with Lewy bodies is caused by clumps of protein forming inside brain cells. These abnormal deposits are called Lewy bodies.
These deposits are also found in people with Parkinsons disease, and they build up in areas of the brain responsible for functions such as thinking, visual perception and muscle movement.
Its not clear why the deposits develop and how exactly they damage the brain. Its thought that part of the problem is the proteins affecting the brains normal functions by interfering with signals sent between brain cells.
Dementia with Lewy bodies usually occurs in people with no family history of the condition, although there have been very rare cases that seem to run in families.
Don’t Miss: Lab Test For Parkinson’s Disease
Pathophysiology Of Cognitive Impairment
The neurobiological basis for cognitive impairment in DLB and PDD is multifocal, related to a synergistic effect of both Syn/LB and AD pathologies and dysfunction of dopaminergic, noradrenalinergic, serotonergic, and cholinergic systems . The emergence of PDD and DLB occurs on the background of severe dopamine deficits and correlates with a marked loss of limbic and cortically projecting dopamine, noradreanaline, serotonin, and ACh neurons. The relationship between these lesions is not yet fully understood.
Severe pathology also involves the noradrenergic locus ceruleus and the serotonergic dorsal raphe nucleus as well as the ventral tegmental area not always associated with coincidental AD lesions . LC neuronal loss and the accompanying norepinephrinergic deficiency are an important cause and pharmacological target for the treatment of PD/PDD/DLB . The prominent role of serotonergic degeneration also involving the anterior caudate nucleus, the orbitofrontal and cingulate cortex for neuropsychiatric symptoms in PD , emphasizes its important role in both PDD and DLB, and stimulates new insight into novel treatments by modulating 5-HT receptors .
Read Also: Meds For Parkinsons Psychosis
Tests For Dementia With Lewy Bodies
There’s no single test for dementia with Lewy bodies.
The following may be needed to make a diagnosis:
- an assessment of symptoms for example, whether there are typical symptoms of dementia with Lewy bodies
- an assessment of mental abilities this will usually involve a number of tasks and questions
- blood tests to rule out conditions with similar symptoms
- brain scans, such as an MRI scan, CT scan or a SPECT scan these can detect signs of dementia or other problems with the brain
You May Like: Thc For Parkinson’s Disease
Role Of Genetic Factors
In contrast to PD in which numerous disease-related gene loci have been described, it has long appeared in DLB that genetic factors play here virtually no role. Only in the last decade, some variants have been identified in DLB. One of the first hints that genetics plays the same role in PD and DLB came from the studies of glucocerebrosidase . Homozygous GBA mutations are known to cause a lysosomal storage disorder , while heterozygous mutations are considered a risk factor for PD. In DLB, a similar effect of these mutations was identified suggesting that there is an identical underlying lysosomal dysfunction present in both diseases.
The genetic differences between PDD and DLB have, so far, not been studied in detail. Some factors predisposing to the development of earlier dementia in PDD cases have a genetic basis. For example, rapid eye movement sleep behaviour disorder, which is predictive of cognitive involvement when it occurs in patients with PD, is more common in patients carrying GBA and SNCA mutations and less common in patients carrying LRRK2 mutations.
What Are The Causes Of Lewy Body Dementia
The precise cause of LBD is unknown, but scientists are learning more about its biology and genetics. For example, we know that an accumulation of Lewy bodies is associated with a loss of certain neurons in the brain that produce two important chemicals that act as messengers between brain cells . One of these messengers, acetylcholine, is important for memory and learning. The other, dopamine, plays an important role in behavior, cognition, movement, motivation, sleep, and mood.
Scientists are also learning about risk factors for LBD. A risk factor is something that may increase the chance of developing a disease. Some risk factors can be controlled while others cannot. Age is considered the greatest risk factor. No specific lifestyle factor has been proven to increase one’s risk for LBD.
Other known risk factors for LBD include certain diseases and health conditions, particularly Parkinson’s disease and REM sleep behavior disorder, which have been linked to a higher risk of LBD.
Having a family member with LBD also may increase a person’s risk, though LBD is not considered a genetic disease. Variants in three genes APOE, SNCA, and GBA have been associated with an increased risk, but in most cases, the cause is unknown.
Don’t Miss: Psoriatic Arthritis And Parkinson’s Disease
An Insufficient Mainstay For The Formulation Of Pdd Criteria
PDD as a novel subtype of the LBD has been gradually recognized in the nineties of the last century. The principal reason which led to its identification waswithout any doubtthe introduction of novel drugs into the PD treatment armamentarium, hand-in-hand with the introduction of the treatment of late, advanced, and complicated PD, i.e. deep brain stimulation and subcutaneous apomorphine infusions. Both these approaches led to substantially longer survival of PD patients, so the cases with manifest dementia appeared. In other words, dementia related to PD was unmasked.
When Emre in 2003 discussed the concept of PDD on a more extensive basis, he introduced two most important risk factors: older age as such, and older age at the moment of motor symptoms manifestation. The detailed description of typical PDD phenotype together with the first suggestion of clinical diagnostic criteria was published in 2007. International experts, led by Emre, indeed performed a critical meta-analysis of published studies. They particularly extracted the neuropsychological manifestations of the typical PDD cognitive disorder, i.e. the progressive executive dysfunction, only later accompanied by the general cognitive dysfunction. They also summarized the results of 24 clinicalpathological studies, published in 19792005.
Treating Parkinsons Disease Dementia
A treatment plan for PDD typically includes medications that boost the brains level of certain neurotransmitters and help improve memory and processing speed, Dr. Petrossian says. Exercise is also an important part of the treatment planDr. Petrossian recommends skill-based activities like boxing or dance to boost cognitive function as well as fitness. PDD symptoms should be monitored long-term by a neurologist, and in some cases a psychiatrist, says Dr. Okun. In many cases, physical, occupational, speech, and social work therapy can also be useful since PPD affects all aspects of life.
You May Like: Is There A Blood Test To Check For Parkinson’s
Is Lewy Body Dementia Hereditary & What Is The Life Expectancy Of A Person With Lewy Body Dementia
Most patients suffering from Lewy Body Dementia prefer visiting a primary care physician at the initial stage. Diagnosing the disorder can be a real problem if the symptoms grow severe.
There are many families that have been affected by Lewy Body Dementia . However, it has been seen that very few individuals and even medical professionals are aware of the diagnostic criteria and symptoms. Some even dont have the idea whether or not the disease exists. Therefore, you should know about Lewy Body Dementia not only to save yourself but also your loved ones, families and friends. Lewy body dementia is a type of progressive dementia that comes only after Alzheimers disease dementia.
Recommended Reading: How Does Deep Brain Stimulation Work In Parkinsons Disease
Lewy Bodies: More Than Lbd
LBD is characterized by the presence of Lewy bodies in the nerve cells of the brain, meaning that LBD patients have Lewy bodies in the brain.2 However, Lewy bodies are also common with other conditions, such as Alzheimers and Parkinsons disease. In fact, most people with PD also have Lewy bodies in their brain. However, even if they have Lewy bodies, not all Parkinsons patients will also develop LBD.2
You May Like: Can Thyroid Problems Cause Parkinsons
Don’t Miss: How To Help With Parkinson Disease
Slowing The Progression Of Symptoms
The same healthy lifestyle changes that are used to prevent dementia can also be useful in slowing the advancement of LBD symptoms.
To learn more about putting these strategies into action, see Preventing Alzheimers Disease.
How Is Lewy Body Disease Diagnosed
There is no specific test for Lewy body disease. A person with symptoms of Lewy body disease will usually be examined and assessed to see what mix of symptoms they have and the timing of the appearance of the symptoms. This can help make a diagnosis of Parkinsons disease, Parkinsons disease with dementia, or dementia with Lewy bodies.
To make a diagnosis, a neurologist, geriatrician or psychiatrist will assess a persons thinking and alertness, whether they have hallucinations, Parkinsons symptoms and how they sleep.
They may want to ask the person and their family members about symptoms. They may ask a person to do a Mini-Mental State Examination a short test to check for problems with thinking and memory.
The doctor may also look at blood pressure, heart rate, body temperature and sweating. They may do blood tests to rule out other conditions.
Scans can show degeneration in the brain, but there is no particular appearance that can diagnose Lewy bodies. However, doctors may suggest an MRI or CT scan of the brain to rule out other causes of dementia.
A SPECT or PET scan may help to support a diagnosis of dementia with Lewy bodies, but at the moment Lewy bodies can only be confirmed by examining brain tissue after death.
A diagnosis of dementia with Lewy bodies is likely if, alongside dementia, a person has the characteristic symptoms of:
In Parkinsons disease dementia, the muscle and movement symptoms are often more severe than the mental problems.
Don’t Miss: What Drugs Induce Parkinson’s Disease
Treatments For Dementia With Lewy Bodies
There’s currently no cure for dementia with Lewy bodies or any treatment that will slow it down.
But there are treatments that can help control some of the symptoms, possibly for several years.
Treatments include:
- medicines to reduce hallucinations, confusion, drowsiness, movement problems and disturbed sleep
- therapies such as physiotherapy, occupational therapy and speech and language therapy for problems with movement, everyday tasks, and communication
- psychological therapies, such as cognitive stimulation
- dementia activities, such as memory cafes
Building A Lewy Body Dementia Care Team
After receiving a diagnosis, a person with LBD may benefit from seeing a neurologist who specializes in dementia and/or movement disorders. Your primary doctor can work with other professionals to follow your treatment plan. Depending on an individual’s particular symptoms, physical, speech, and occupational therapists, as well as mental health and palliative care specialists, can be helpful.
Support groups are another valuable resource for people with LBD and their caregivers. Sharing experiences and tips with others in the same situation can help people find practical solutions to day-to-day challenges and get emotional and social support.
You May Like: How Bad Does Parkinson’s Get
Lewy Bodies And Parkinsons Disease
A person with Parkinsons disease may develop dementia and have problems with reasoning and thinking. Lewy bodies are a feature of several brain disorders, including Parkinsons disease and Alzheimers disease, and they may cause rigid muscles and problems with movement and posture.
Research suggests that the similarity of the symptoms of Parkinsons disease and Lewy body dementia may be indicative of a shared link to how the brain processes alpha-synuclein.
It is not possible to test for the presence of Lewy bodies, so researchers must try to determine their effects by carrying out postmortem studies.
There is currently no cure for dementia. However, medication can alleviate the symptoms, while a team of medical professionals and therapists may help a person develop strategies to manage their daily activities.
Diagnosing Lewy Body Dementia: For Professionals
Lewy body dementia can be difficult to diagnose. Talking to both patients and caregivers helps doctors make a diagnosis. It is important to ask the patient and their care partners about any symptoms involving thinking, movement, sleep, behavior, or mood. Certain medications can worsen LBD symptoms be aware of all current medications and supplements the patient is taking.
Dementia with Lewy bodies is often hard to diagnose because its early symptoms may resemble those of Alzheimers disease or a psychiatric illness. As a result, it is often misdiagnosed or missed altogether. As additional symptoms appear, making an accurate diagnosis may become easier.
The good news is that doctors are increasingly able to diagnose LBD earlier and more accurately, as researchers identify which symptoms and biomarkers help distinguish it from similar disorders.
Visiting a family doctor is often the first step for people who are experiencing changes in thinking, movement, or behavior. If a persons primary doctor is not familiar with LBD, they may have patients seek second opinions from specialists, like a geriatric psychiatrist, neuropsychologist, or a geriatrician to help diagnose LBD. If a specialist cannot be found in your community, ask the neurology department at a nearby medical school for a referral. Neurologists generally have the expertise needed to diagnose LBD.
Difficult as it is, getting an accurate diagnosis of LBD early on is important so that a person:
Read Also: Parkinson’s Disease Stem Cell
Advice For People Living With Lewy Body Dementia
Coping with a diagnosis of LBD and all that follows can be challenging. Getting support from family, friends, and professionals is critical to ensuring the best possible quality of life. Creating a safe environment and preparing for the future are important, too. Take time to focus on your strengths, enjoy each day, and make the most of your time with family and friends. Here are some ways to live with LBD day to day.
Getting Help
Your family and close friends are likely aware of changes in your thinking, movement, or behavior. You may want to tell others about your diagnosis so they can better understand the reason for these changes and learn more about LBD. For example, you could say that you have been diagnosed with a brain disorder called Lewy body dementia, which can affect thinking, movement, and behavior. You can say that you will need more help over time. By sharing your diagnosis with those closest to you, you can build a support team to help you manage LBD.
As LBD progresses, you will likely have more trouble managing everyday tasks such as taking medication, paying bills, and driving. You will gradually need more assistance from family members, friends, and perhaps professional caregivers. Although you may be reluctant to get help, try to let others partner with you so you can manage responsibilities together. Remember, LBD affects your loved ones, too. You can help reduce their stress when you accept their assistance.
Consider Safety
Plan for Your Future
