How Is Parkinson’s Disease Diagnosed
Diagnosis is difficult at every stage of the disease, but particularly in the early stages. No single test can provide a diagnosis. A diagnosis will likely involve physical and neurological examinations, conducted over time to assess changes in reflexes, coordination, muscle strength, and mental function. Your doctor might also see how you respond to medicine.
You may need to have brain imaging tests to rule out other conditions that might be causing your symptoms. Such tests could include MRI and CT scans and possibly some other types of scans. Blood tests may also be done to exclude other illnesses.
What Is Essential Tremor And How Is It Different To A Parkinsons Tremor
A tremor is a rhythmical, involuntary movement that affects a part of the body, such as the hand.
Essential tremor is the most common type of tremor. Its most noticeable when your hands are doing something and it usually affects both the right and left sides of the body equally. Essential tremors often lessen when your body is resting.
Unlike an essential tremor, a Parkinsons tremor is most obvious when the affected body part is resting and tends to be less noticeable with movement. It usually starts on one side of the body and may progress to the other side as Parkinsons develops.
The time it takes to get a diagnosis can vary from person to person. Some people may receive a diagnosis of Parkinsons quite quickly, but for others it may be a long process. This can be due to a number of things, including your medical history, your age and what symptoms you have.
Your specialist may wish to rule out other causes of your symptoms first and see how you respond to treatment. This may take some time, and, as already mentioned, there is currently no definitive test for Parkinsons.
How you respond to treatment may help your specialist make a diagnosis. Keeping a diary or record of your symptoms will give the specialist more information to guide their decision.
Because the symptoms of Parkinsons are sometimes similar to other forms of parkinsonism, people can sometimes be misdiagnosed.
How Is Parkinson’s Disease Managed
Your doctors will tailor your treatment based on your individual circumstances. You will manage your condition best if you have the support of a team, which may include a general practitioner, neurologist, physiotherapist, occupational therapist, psychologist, specialist nurse and dietitian.
While there is no cure for Parkinson’s disease, symptoms can be treated with a combination of the following.
You May Like: Life Expectancy With Parkinson’s
What Are The Symptoms Of Parkinson’s Disease
The main symptoms of Parkinson’s disease are:
- tremor or shaking, often when resting or tired. It usually begins in one arm or hand
- muscle rigidity or stiffness, which can limit movement and may be painful
- slowing of movement, which may lead to periods of freezing and small shuffling steps
- stooped posture and balance problems
The symptoms of Parkinson’s disease vary from person to person as well as over time. Some people also experience:
- loss of unconscious movements, such as blinking and smiling
- difficulties with handwriting
- drop in blood pressure leading to dizziness
- difficulty swallowing
- sweating
Many of the symptoms of Parkinson’s disease could be caused by other conditions. For example, stooped posture could be caused by osteoporosis. But if you are worried by your symptoms, it is a good idea to see your doctor.
Do Symptoms Get Worse
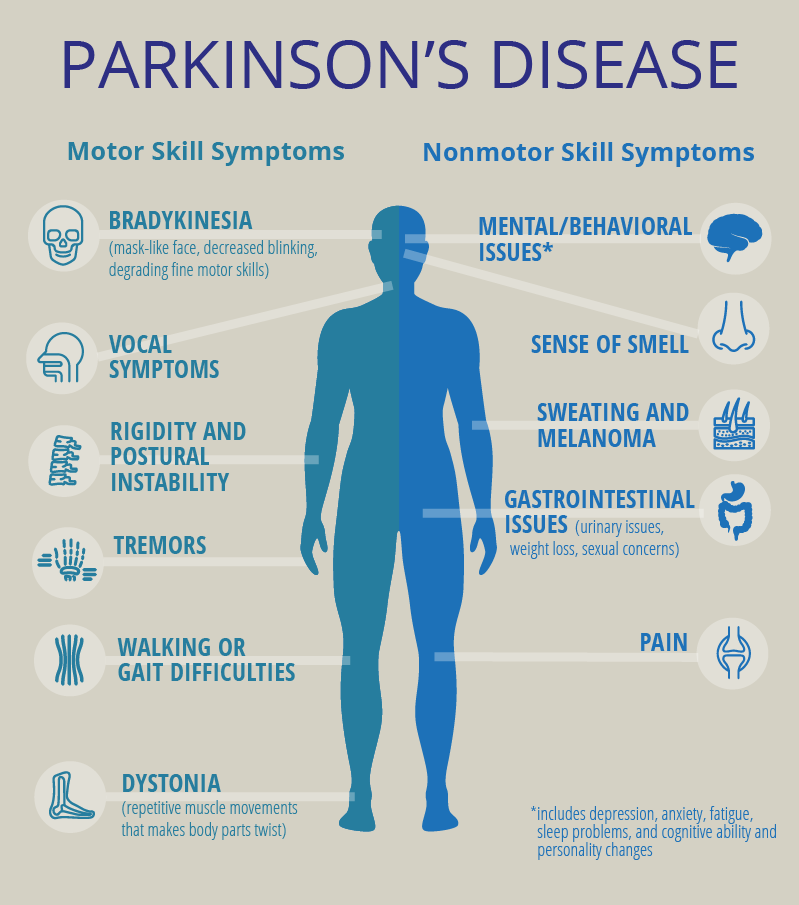
PD does not affect everyone the same way. The rate of progression and the particular symptoms differ among individuals.
PD symptoms typically begin on one side of the body. However, the disease eventually affects both sides, although symptoms are often less severe on one side than on the other.
Early symptoms of PD may be subtle and occur gradually. Affected people may feel mild tremors or have difficulty getting out of a chair. Activities may take longer to complete than in the past. Muscles stiffen and movement may be slower. The persons face may lack expression and animation . People may notice that they speak too softly or with hesitation, or that their handwriting is slow and looks cramped or small. This very early period may last a long time before the more classical and obvious motor symptoms appear.
As the disease progresses, symptoms may begin to interfere with daily activities. Affected individuals may not be able to hold utensils steady or they may find that the shaking makes reading a newspaper difficult.
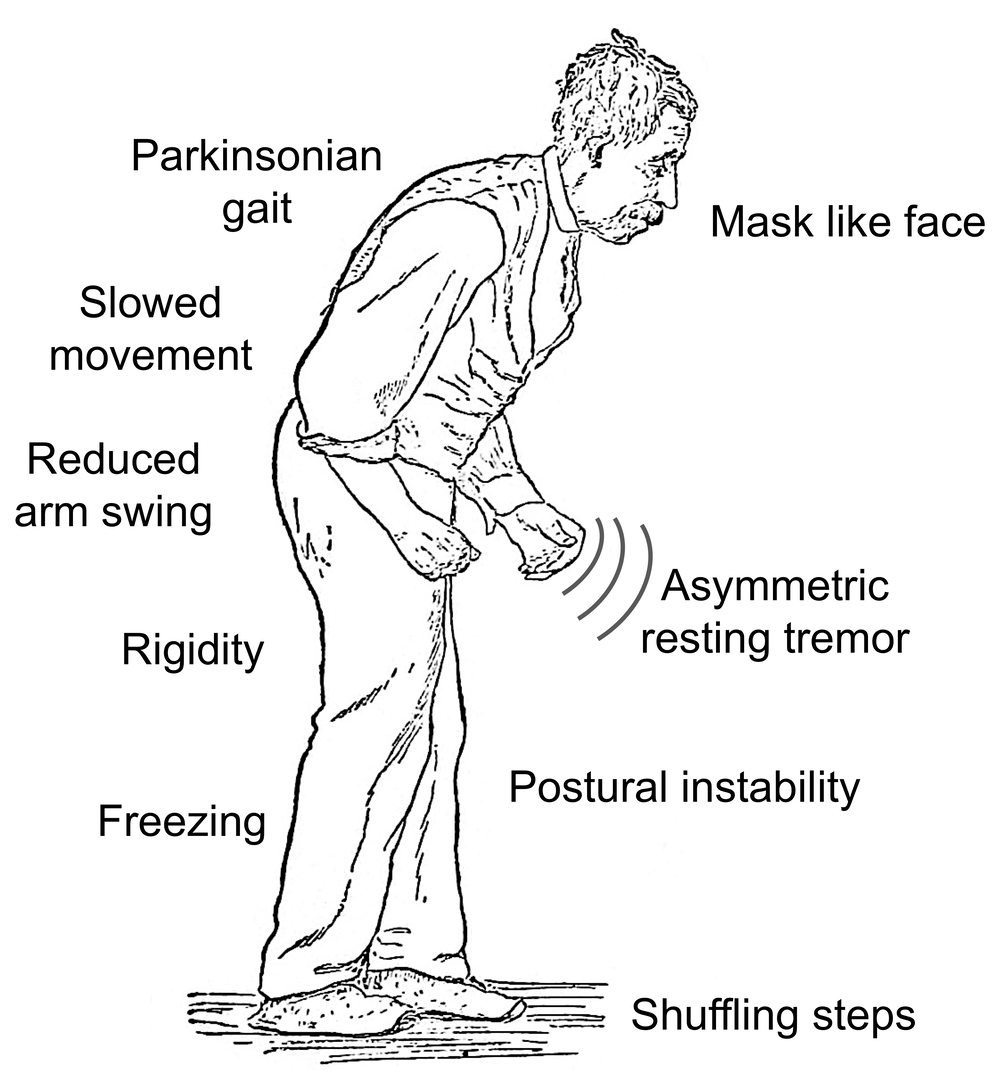
People with PD often develop a so-called parkinsonian gait that includes a tendency to lean forward, taking small quick steps as if hurrying , and reduced swinging in one or both arms. They may have trouble initiating movement , and they may stop suddenly as they walk .
Read Also: Freddie Roach Brain Damage
Why Has My Neurologist Prescribed Levodopa To Confirm My Diagnosis
Depending on your symptoms, your neurologist may ask you to take levodopa for a period of time.
Parkinsons disease is characterized by a deficiency of dopamine in the brain and mainly in the substantia nigra.Taking levodopa, a precursor to dopamine, can reverse the symptoms of Parkinsons disease. One dose is not enough. You will need to take several weeks of treatment with increasing doses until you get a result that will confirm your diagnosis.This test, when negative, can also invalidate the trail of other diseases related to Parkinsons disease
Establishing Pd Research Priorities
The NINDS-organized Parkinsons Disease 2014: Advancing Research, Improving Lives conference brought together researchers, clinicians, patients, caregivers, and nonprofit organizations to develop 31 prioritized recommendations for research on PD. These recommendations are being implemented through investigator-initiated grants and several NINDS programs. NINDS and the NIHs National Institute of Environmental Health Sciences held the Parkinsons Disease: Understanding the Environment and Gene Connection workshop to identify priorities for advancing research on environmental contributors to PD.
Research recommendations for Lewy Body Dementia, including Parkinsons disease dementia, were updated during the NIH Alzheimers Disease-Related Dementias Summit 2019 .
Also Check: How Long Do Parkinson’s Patients Live
Highlights From The Canadian Chronic Disease Surveillance System
Parkinsonism, including Parkinsons disease, can have significant impacts for those affected, their caregivers, and society. With a growing and aging population, it is estimated that the number of Canadians living with parkinsonism will double between 2011 and 2031 and that the incidence will increase by 50%.Footnote 1
The Public Health Agency of Canada , in collaboration with all Canadian provinces and territories, conducts national surveillance of parkinsonism to support the planning and evaluation of related policies, programs, and services. This fact sheet presents an overview of the data on diagnosed parkinsonism, including Parkinsons disease, from the Canadian Chronic Disease Surveillance System .
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
You May Like: Is Gabapentin Used For Parkinson’s Disease
Are There Additional Tests To Help Diagnose Parkinson’s Disease
Imaging tests cannot confirm the diagnosis of Parkinsons disease. On the other hand, they allow the exclusion or investigation of other possible causes for the symptoms observed.
The most widely used technique is used to visualize the integrity of the dopaminergic system by injecting, intravenously, a radioactive product that binds to dopaminergic neurons. In those affected, these neurons are less numerous, which then becomes apparent during the assessment. This technique mainly distinguishes Parkinsons disease from essential tremor.
Is Parkinsons Disease Inherited
Scientists have discovered gene mutations that are associated with Parkinsons disease.
There is some belief that some cases of early-onset Parkinsons disease disease starting before age 50 may be inherited. Scientists identified a gene mutation in people with Parkinsons disease whose brains contain Lewy bodies, which are clumps of the protein alpha-synuclein. Scientists are trying to understand the function of this protein and its relationship to genetic mutations that are sometimes seen in Parkinsons disease and in people with a type of dementia called Lewy body dementia.
Several other gene mutations have been found to play a role in Parkinsons disease. Mutations in these genes cause abnormal cell functioning, which affects the nerve cells ability to release dopamine and causes nerve cell death. Researchers are still trying to discover what causes these genes to mutate in order to understand how gene mutations influence the development of Parkinsons disease.
Scientists think that about 10% to 15% of persons with Parkinsons disease may have a genetic mutation that predisposes them to development of the disease. There are also environmental factors involved that are not fully understood.
Don’t Miss: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Referral To A Specialist
If your GP suspects Parkinson’s disease, you’ll be referred to a specialist.
This will usually be:
- a neurologist, a specialist in conditions affecting the brain and nervous system
- a geriatrician, a specialist in problems affecting elderly people
The specialist will most likely ask you to perform a number of physical exercises so they can assess whether you have any problems with movement.
A diagnosis of Parkinson’s disease is likely if you have at least 2 of the 3 following symptoms:
- shaking or tremor in a part of your body that usually only occurs at rest
- slowness of movement
- muscle stiffness
If your symptoms improve after taking a medication called levodopa, it’s more likely you have Parkinson’s disease.
Special brain scans, such as a single photon emission computed tomography scan, may also be carried out in some cases to try to rule out other causes of your symptoms.
How Is Parkinsons Disease Diagnosed
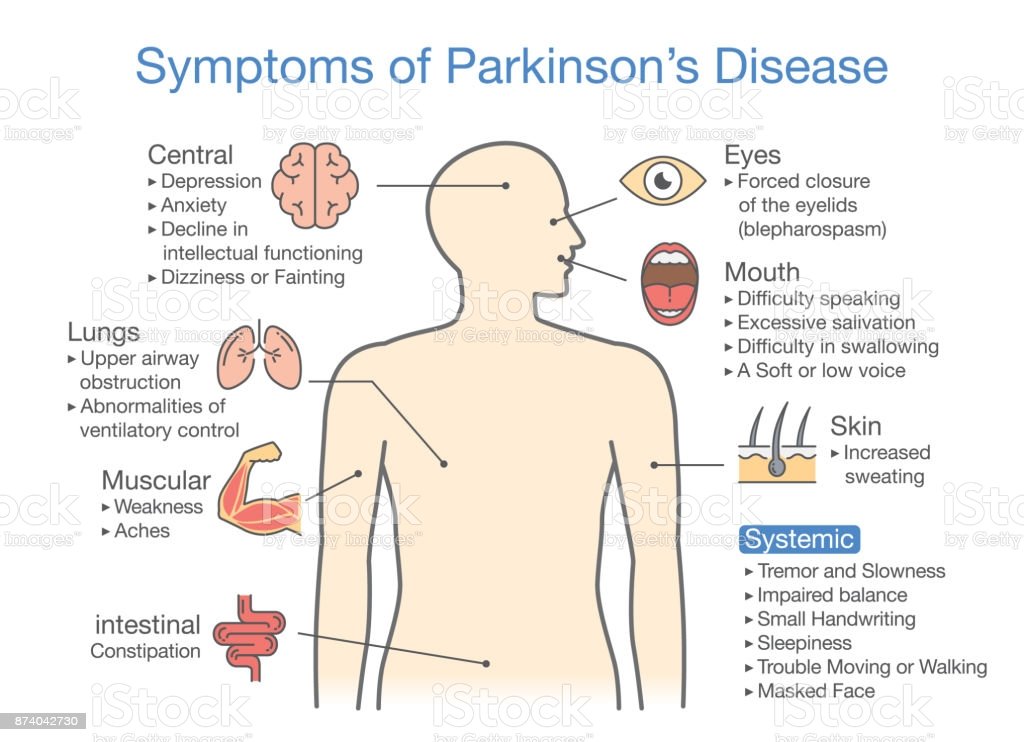
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Read Also: Amy Klobuchar Tremor
Passive Manipulation Of Limbs
To test for the presence of rigidity, we need to passively manipulate the limbs of the patient. However, If the disease is in its early stage or the symptoms are well controlled with medications, we may not be able to see rigidity. We will need to use some activation maneuvers, that basically consist in performing repetitive movements with the limb contralateral to the one that is being tested.
Also, there are two types of rigidity:
– Lead-pipe rigidity: where the tone is uniformly and smoothly increased throughout the entire range of movement
– Cogwheel rigidity: where a tremor is superimposed on the hypertonia, making the movement irregular due to intermittent increase and reduction of tone
Upper Extremity Testing
For the upper extremity the most sensitive joint where to check for rigidity is the wrist. To uncover rigidity, passively rotate the wrist and feel for a resistance to the movement. It is very important that the arm of the patient is fully relaxed when rotating the wrist. To do this, place your proximal hand under the patients forearm, while your distal hand grabs and rotates the wrist of the patient. When rigidity is present, the range of motion will be preserved but you will feel a resistance in performing the movement.
Wrist rotation with activation maneuver.
It is also possible to test for rigidity in the elbow by passively flexing and extending the forearm.
Elbow flexion-extension with activation maneuver.
Lower Extremity Testing
Medications For People With Parkinsons Disease
Symptoms of Parkinsons disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinsons medications fit into one of the following broad categories:
- levodopa dopamine replacement therapy
- dopamine agonists mimic the action of dopamine
- COMT inhibitors used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors prevent the metabolism of dopamine within the brain.
Read Also: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How Can People Cope With Parkinson’s Disease
While PD usually progresses slowly, eventually daily routines may be affectedfrom socializing with friends to earning a living and taking care of a home. These changes can be difficult to accept. Support groups can help people cope with the diseases emotional impact. These groups also can provide valuable information, advice, and experience to help people with PD, their families, and their caregivers deal with a wide range of issues, including locating doctors familiar with the disease and coping with physical limitations. A list of national organizations that can help people locate support groups in their communities appears at the end of this information. Individual or family counseling may also help people find ways to cope with PD.
People with PD may also benefit from being proactive and finding out as much as possible about the disease in order to alleviate fear of the unknown and to take a positive role in maintaining their health. Many people with PD continue to work either full- or part-time, although they may need to adjust their schedule and working environment to accommodate their symptoms.
How Will I Manage The Changes Caused By The Disease
You likely had plans, dream vacations or other things you wanted to accomplish in your future. You must now incorporate your condition into these projects. Although Parkinsons is a progressive disease, it progresses slowly and differently from person to person.
Take advantage of everyday that passes and continue the hobbies and activities you enjoyed. For some, the diagnosis can be the opportunity to strengthen character and discover passions and qualities they would not have found otherwise.
Turn your fear into curiosity and learn all you can about the disease. Parkinson Québec has many resources to help you better understand the disease and live with it on a daily basis. Ask your loved ones for help or reach out to available resources for support.
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
How It All Fits Together
Diagnosing Parkinsons disease can be tricky. The process relies heavily on your doctors judgment. In addition, the causes and risk factors of Parkinsons are not entirely clear yet, which contributes to the difficulty in diagnosing this condition.
However, there have been efforts to try and detect this disease earlier. For instance, clinicians have started focusing more on prodromal symptoms, which are early symptoms that appear before movement-related difficulties begin.
These symptoms include:
- Loss of smell, which can sometimes occur years before other symptoms
- Chronic constipation, without any other explanation
- Rapid eye movement behavior disorder, which causes sleep disturbances
Defining Populations At Risk For Parkinsons Disease
One of the areas of research that aims to aid in the early detection and treatment of PD is seeking to identify biomarkersprotein or chemicals in the blood, urine, or cerebrospinal fluid that reliably help diagnose PD, particularly at the early stage. For example, a recent study detected aggregates of alpha-synuclein in the cerebrospinal fluid. These aggregates were found in PD patients but not patients with other neurologic disorders. Many research studies are attempting to identify new biomarkers, particularly those that may even predict whether someone will develop PD over time.5
Also Check: What Kind Of Effect Does R-dopa Have On Parkinson’s Disease
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Parkinsons Disease Risk Factors
There are a variety of risk factors for Parkinsons, including those related to your age and environment.
Your risk of developing Parkinsons disease increases with age, and about 1% of people over 60 years old have Parkinsons disease. Although it more commonly affects older people, about 10% of cases are considered early onset, meaning symptoms begin before age 50.
Parkinsons affects more men than women, and having a relative with Parkinsons disease might mean you may have a slightly higher risk of developing it. However, your risk is still low unless you have many relatives with the disease. Environmental toxins, such as ongoing exposure to pesticides and herbicides, may also be a risk factor.
Recommended Reading: Is Parkinsons Fatal
