Medicines For Parkinson’s Disease
Medicines prescribed for Parkinson’s include:
- Drugs that increase the level of dopamine in the brain
- Drugs that affect other brain chemicals in the body
- Drugs that help control nonmotor symptoms
The main therapy for Parkinson’s is levodopa, also called L-dopa. Nerve cells use levodopa to make dopamine to replenish the brain’s dwindling supply. Usually, people take levodopa along with another medication called carbidopa. Carbidopa prevents or reduces some of the side effects of levodopa therapysuch as nausea, vomiting, low blood pressure, and restlessnessand reduces the amount of levodopa needed to improve symptoms.
People with Parkinson’s should never stop taking levodopa without telling their doctor. Suddenly stopping the drug may have serious side effects, such as being unable to move or having difficulty breathing.
Other medicines used to treat Parkinsons symptoms include:
- Dopamine agonists to mimic the role of dopamine in the brain
- MAO-B inhibitors to slow down an enzyme that breaks down dopamine in the brain
- COMT inhibitors to help break down dopamine
- Amantadine, an old antiviral drug, to reduce involuntary movements
- Anticholinergic drugs to reduce tremors and muscle rigidity
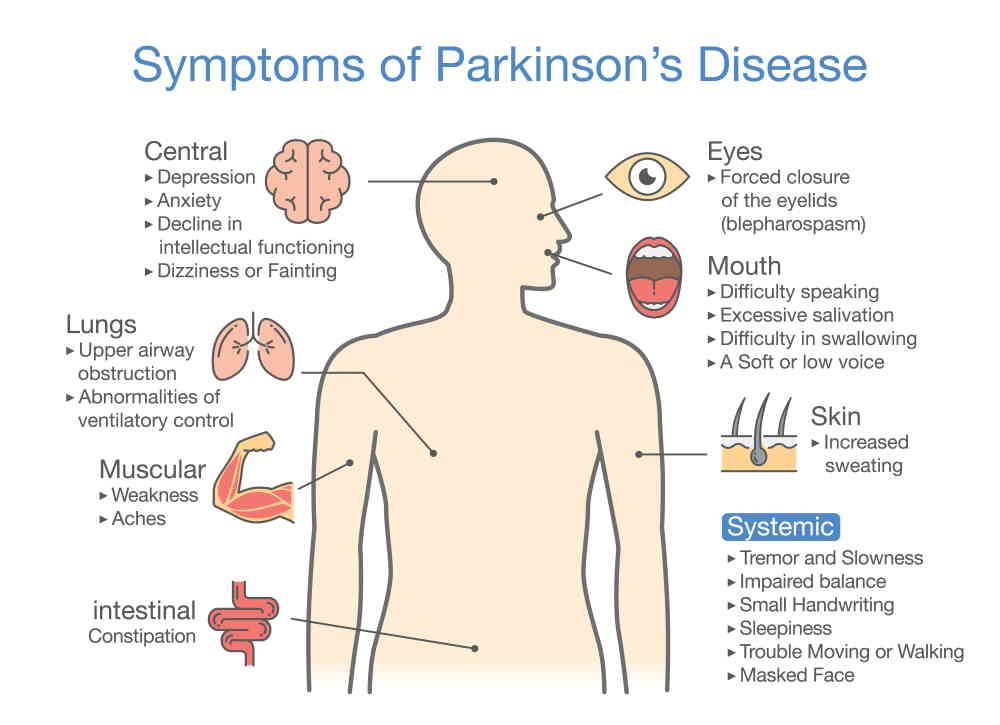
What Are The Symptoms That May Be Clues To The Onset Of Parkinsons Disease
There are many potential symptoms and/or signs that may herald the earliest features and/or evidence supporting a diagnosis of Parkinsons disease. It is estimated that a person must lose approximately 60% of the dopamine producing cells in the brain , before noticeable changes will be detected. This cell loss always occurs befor the symptoms that set off the suspicion in patients, family members, or even doctors . This situation of a threshold of cell loss that must be eclipsed for appearance of symptoms can be compared to what may occur in patients who experience kidney failure. When a kidney begins to malfunction, approximately 75% or more of its cells are lost, and those cells are unrecoverable. Frustratingly, for kidney failure failure patients, the routine laboratory tests are almost never abnormal, and only hint abnormality when the failure process has already begun. In Parkinsons disease, as in kidney failure, a threshold of cells must be lost before one manifests symptoms.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Also Check: What To Expect With Parkinson’s Disease
What Causes Parkinson’s Disease
Parkinson’s disease occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. Normally, these neurons produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinson’s. Scientists still do not know what causes cells that produce dopamine to die.
People with Parkinson’s also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinson’s, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying-down position.
Many brain cells of people with Parkinson’s contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons disease and Lewy body dementia.
Confusion With Essential Tremor
The tremor of Parkinsons disease is often confused with the tremor of a condition called Essential Tremor, or Benign Familial Tremor . Katherine Hepburn had Essential Tremor, and was originally misdiagnosed with Parkinsons. Ronald Reagan also had Essential Tremor. Both had a head tremor and a vocal tremor. In Essential Tremor, the hands are most commonly involved, followed by the head and then the voice. Essential Tremor can also cause the jaw to tremor, and it may be difficult to figure out if a jaw tremor is from Essential Tremor or Parkinsons. Unfortunately, some people may have both disorders. Some authorities believe that there is, in fact, an increased association between the two conditions, so that more people with Parkinsons disease have Essential Tremor than would be expected by chance alone, but this has not been established.
Also Check: Is Parkinson’s Disease Terminal
What Is The History Of Parkinsons Disease
Parkinsons disease, sometimes erroneously termed paralysis agitans, was described in the Indian medical system of Ayurveda , and also by Galen who referred to it as the shaking palsy. Perhaps the most interesting reference came from Shakespeare who wrote in Henry VI why dost thou quiver man. The character in the story responds by saying the palsy and not the fear provokes me. The use of the term Parkinsons disease was largely credited to the highly influential 19th century French Neurologist Jean-Martin Charcot, although it should be noted that many people prior to Parkinson himself described the disease. James Parkinson a Londoner and son of an apothecary and surgeon is credited with the eponym for his 1817 essay on the shaking palsy. His descriptions included six cases only three of which were actually examined .
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
You May Like: Does Parkinson’s Cause Fatigue
What Is The History Of The Discovery Of Levodopa
There were several seminal discoveries that led to the development of levodopa as a therapy for Parkinsons disease:
- 1911 First synthesis of its D,L racemate and the isolation of its L-isomer from the seedling of Vicia faba beans
- 1913 Isolation from legumes
- 1930 L-Dopa was shown to have an effect on Rabbit glucose metabolism
- 1938 L-dopa decarboxylase described and enzymatic conversion to dopamine demonstrated
- 1940 Studies on the effects of L-Dopa on blood vessels
- 1950 Studies began to consider the use of dopamine on the brain
- 1960 Consideration was given to Parkinsons disease treatment which was found to be related to dopamine
- 1967 High dose levodopa was verified for treatment of patients suffering with Parkinsons disease
- 1970s Dopamine decarboxylase was added to the regimen to improve the side effect profile and absorption
Many scientists have worked on the development of levodopa and levodopa therapy and the list of their names is too long for a short book such as this. Arvid Carlsson from Sweden won the Nobel Prize in 2000 for his work on the administration of levodopa to animals , and Oliver Sacks .
Signs Of Parkinsons Disease
In 1817, Dr. James Parkinson published An Essay on the Shaking Palsy describing non-motor, as well as, motor symptoms of the illness that bears his name. Parkinsons is not just a movement disorder, explained Dr. Shprecher. Constipation, impaired sense of smell, and dream enactment can occur years before motor symptoms of Parkinsons. The latter, caused by a condition called REM sleep behavior disorder, is a very strong risk factor for both Parkinsons and dementia . This has prompted us to join a consortium of centers studying REM sleep behavior disorder.
Don’t Miss: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Living With Parkinsons Disease
Depending on severity, life can look very different for a person coping with Parkinsons Disease. As a loved one, your top priority will be their comfort, peace of mind and safety. Dr. Shprecher offered some advice, regardless of the diseases progression. Besides movement issues Parkinsons Disease can cause a wide variety of symptoms including drooling, constipation, low blood pressure when standing up, voice problems, depression, anxiety, sleep problems, hallucinations and dementia. Therefore, regular visits with a neurologist experienced with Parkinsons are important to make sure the diagnosis is on target, and the symptoms are monitored and addressed. Because changes in your other medications can affect your Parkinsons symptoms, you should remind each member of your healthcare team to send a copy of your clinic note after every appointment.
Dr. Shprecher also added that maintaining a healthy diet and getting regular exercise can help improve quality of life. Physical and speech therapists are welcome additions to any caregiving team.
How Parkinsons Disease Affects The Autonomic Nervous System And The Heart
In PD, there are two major reasons why the automatic control of the cardiac system is impaired. First, areas of the brain that control this system often contain Lewy bodies and have undergone neurodegeneration. In addition, the autonomic nervous system itself is directly affected by Lewy body-like accumulations and neurodegeneration. This means, when the baroreceptors in the heart and carotid artery sense a drop in blood pressure and try to generate a signal to the heart and blood vessels to increase the blood pressure, the message may not get through. This results in neurogenic orthostatic hypotension , or drops in blood pressure upon standing due to autonomic nervous system dysfunction. There are no medications that can cure nOH by restoring the autonomic nervous system in PD. nOH however, can be treated. Read more about nOH and its treatments here.
Structural problems of the heart such as coronary artery disease or cardiomyopathy are not thought to be part of the pathology of PD, although of course, could co-exist with PD.
You May Like: Early Signs Of Parkinson’s In Males
How Does Parkinsons Progress
Parkinsons is a chronic and slowly progressive disorder. This means that symptoms normally appear slowly and develop gradually over time. The stage at which symptoms appear, speed at which they progress and the severity of those symptoms will vary from person to person. The most important point is that Parkinsons affects everyone differently.
There are a wide range of symptoms, but it is highly unlikely that you will experience every possible symptom. Some of the early symptoms of Parkinsons include handwriting changes, reduced sense of smell, tiredness and constipation. As Parkinsons progresses symptoms will change over time, and new symptoms will emerge. It can take many years for symptoms to progress to a point where they cause problems.
Ultimately symptoms will begin to impact on your day to day life. Many symptoms are related to physical movement, so you may find that walking becomes difficult. You may also experience non-movement symptoms such as mood changes, disrupted sleep or difficulty communicating. As these symptoms worsen it may become difficult to manage all of your daily activities.
Currently, there is no known way to slow the progression of Parkinsons. However, medications and other treatments can help to effectively manage your symptoms. To ensure the effectiveness of medications, they will need to be reviewed regularly by your specialist or doctor.
The Nervous System & Dopamine
To understand Parkinson’s, it is helpful to understand how neurons work and how PD affects the brain .
Nerve cells, or neurons, are responsible for sending and receiving nerve impulses or messages between the body and the brain. Try to picture electrical wiring in your home. An electrical circuit is made up of numerous wires connected in such a way that when a light switch is turned on, a light bulb will beam. Similarly, a neuron that is excited will transmit its energy to neurons that are next to it.
Neurons have a cell body with branching arms, called dendrites, which act like antennae and pick up messages. Axons carry messages away from the cell body. Impulses travel from neuron to neuron, from the axon of one cell to the dendrites of another, by crossing over a tiny gap between the two nerve cells called a synapse. Chemical messengers called neurotransmitters allow the electrical impulse to cross the gap.
Neurons talk to each other in the following manner :
You May Like: Mannitol Parkinson’s
Stiffness And Slow Movement
Parkinsons disease mainly affects adults older than 60. You may feel stiff and a little slow to get going in the morning at this stage of your life. This is a completely normal development in many healthy people. The difference with PD is that the stiffness and slowness it causes dont go away as you get up and start your day.
Stiffness of the limbs and slow movement appear early on with PD. These symptoms are caused by the impairment of the neurons that control movement. A person with PD will notice jerkier motions and move in a more uncoordinated pattern than before. Eventually, a person may develop the characteristic shuffling gait.
Causes Of Parkinson’s Disease
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Also Check: Sam Waterston Parkinson’s 2018
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
The Heart Of The Matter: Cardiovascular Effects Of Parkinsons Disease
It has long been understood that Parkinsons disease does not just cause movement symptoms, but also causes a litany of non-motor symptoms with effects throughout the body. One of the organ systems that is affected is the cardiac system, encompassing the heart, as well as the major and minor blood vessels. I received this topic as a suggestion from a blog reader and we will be discussing this important issue today. Please feel free to suggest your own blog topic.
Don’t Miss: Hemp Oil Benefits For Parkinson’s
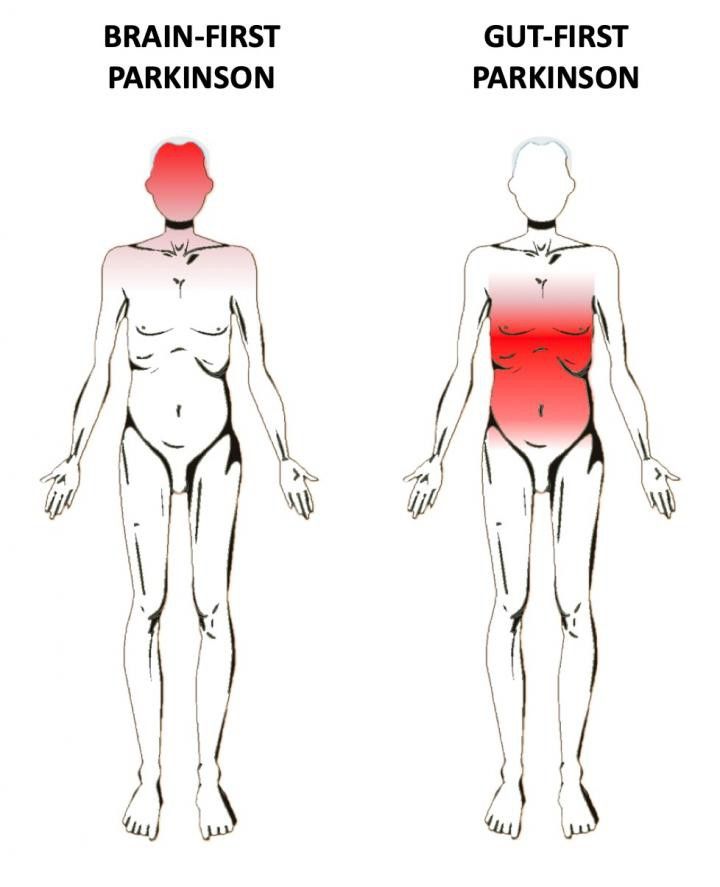
Does Parkinsons Disease Start In The Gut Or In The Brain
During most of the 20th century, Parkinsons disease was thought to be brain disorder – more specifically, a dopamine deficiency disorder leading to the characteristic motor symptoms, which defines the disease. In this millennium, however, our understanding of PD has become much more refined. We know now that many people with Parkinsons display a stereotypical distribution of brain pathology, suggesting that the initial pathology may have arisen in the nerves of the gut and nose.
Animal studies have shown that the prototypical PD pathology, i.e. assemblies of the protein alpha-synuclein, can spread from neuron to neuron. If such pathology is introduced into the gut, either by injecting it in the gut wall or by the animals directly ingesting these proteins, the pathology readily spreads to the brain and involves key structures also known to be affected in the human condition. Alpha-synuclein pathology has been found in the gut of PD patients many years before they became symptomatic. Also, nationwide registry studies have demonstrated that surgical cutting of the vagus nerve, i.e. the most important putative gut-to-brain spreading route, reduces the risk of PD by as much as 50%.
Per Borghammer, MD, PhD, DMSc presented at the 5th World Parkinson Congress in Kyoto, Japan. He is currently a senior consultant and Professor in the Department of Nuclear Medicine & PET at Aarhus University Hospital in Denmark.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Recommended Reading: Does Sam Waterston Have Parkinson
