Surgery To Implant The Deep Brain Stimulation Device
Deep brain stimulation requires the surgical implantation of an electrical device into the brain. A neurosurgeon uses imaging scans to pinpoint the right spot in the brain for implanting the electrode.
When surgeons have determined the correct location, they create a small opening in the skull and insert a thin, insulated wire, through which they insert the electrode. Surgery to implant the electrode takes about four hours and requires general anesthesia. You may then stay overnight in the hospital for observation.
The next day, doctors perform the second part of the surgery, which involves connecting the insulated wire to a battery-operated pulse generator that is implanted under the skin near the collarbone. Most people can return home after this procedure.
Several days after the surgery, you meet with your neurologist, who programs the pulse generator. Pushing a button on an external remote control sends electrical impulses from the pulse generator to the electrode in the brain.
People who use deep brain stimulation work closely with their neurologist to find the combination of settings that best controls their symptoms. After several visits, they are able to control the strength of the electrical impulses on their own. Following this adjustment period, most people require only occasional maintenance visits.
Efficacy Of Local Versus General Anesthesia Techniques
A meta-analysis of 145 studies of DBS in PD showed that the mean target error was not significantly different between LA and GA however the mean number of DBS lead passes were significantly less with GA as compared to LA .62 Post DBS complications were significantly lower with GA . The two techniques did not differ significantly in UPDRS II scores off medication, UPDRS III scores off and on medication or LED. UPDRS IV off medication score decreased more significantly in awake DBS versus sleep DBS cohorts .62 Hence, most DBS procedures should ideally be carried out under LA due to the lower side effect profile.
Deep Brain Stimulation Surgery
A team of experts, including a movement disorder specialist and a brain surgeon, conducts an extensive assessment when considering DBS for someone. They review your medications and symptoms, examine you when you’re on and off Parkinson’s medication, and take brain imaging scans. They also may do detailed memory/thinking testing to detect any problems that could worsen with DBS. If your doctors do recommend you for DBS and you are considering the surgery, discuss with your care team the potential benefits as each person’s experience is unique. It’s also critical to discuss the potential surgical risks, including bleeding, stroke and infection.
In DBS surgery, the surgeon places thin wires called electrodes into one or both sides of the brain, in specific areas that control movement. Usually you remain awake during surgery so you can answer questions and perform certain tasks to make sure the electrodes are positioned correctly. Some medical centers now use brain imaging to guide the electrodes to the right spot while a person is asleep. Each method has its pros and cons and may not be suitable for everyone or available everywhere.
Once the electrodes are in place, the surgeon connects them to a battery-operated device , which usually is placed under the skin below the collarbone. This device, called a neurostimulator, delivers continuous electrical pulses through the electrodes.
You May Like: Is Parkinson’s Disease An Autoimmune Disorder
Deep Brain Stimulation At Michigan Medicine
For carefully selected patients with Parkinsons disease, Essential Tremor, and Dystonia, deep brain stimulation offers a therapeutic surgical option that can reduce or eliminate movement-related problems and greatly improve quality of life. At the University of Michigan Health System, our STIM program brings together a team of medical experts who are leaders in their respective fields and on the cutting-edge of the latest research.
If The Mechanism Of Dbs Is Not Known Why Should I Consider It
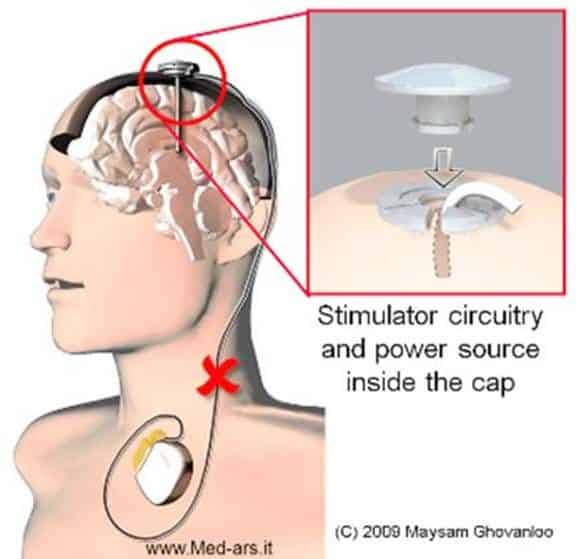
Because it works.
Because it is quite safe.
There are many things for which we dont understand the exact reason. For example, we are still finding out more about the myriad benefits of exercise.
For example How does exercise improve Mood? We dont understand that too well. But it is easy to grasp that exercise is good for you.
This what-you-see-is-true evidence is called Empiric Evidence.
Don’t Miss: How Much Coq10 Should I Take For Parkinson’s
What Risks Come Along With Doing Deep Brain Stimulation
DBS is a surgical procedure. As with any surgery there are some risks associated with it. Some of the risks of DBS include infection and bleeding. Your neurosurgeon may discuss some additional risks with you. Studies have shown that any risks are relatively small, but they should be kept in mind when considering DBS.
Living With A Dbs Device
Batteries most often last three to five years, but this can vary. Rechargeable batteries may last up to 15 years.
There are several precautions related to electrical/magnetic devices that are important, but usually easy to accommodate. Items such as cell phones, computers, and home appliances do not generally interfere with the stimulator. Keep your stimulator identification card handy when you are out and about, in your wallet or purse.
Theft Detectors
Be aware that some devices may cause your transmitter to turn on or off. This includes security monitors that might be found at the library and retail shops.
If this occurs accidentally, it is not usually serious, but may be uncomfortable or result in your symptoms worsening if the stimulator is turned off. When you visit stores with these devices, you can ask to bypass the device by presenting your stimulator identification card.
Home Electronics
Keep the magnet used to activate and deactivate the stimulator at least 12 inches away from televisions, computer disks, and credit cards, as the magnet could potentially damage these items.
Air Travel/Metal Detectors
Talk to TSA personnel when traveling by plane, as the metal in the stimulator may set off the detector. If you are asked to go through additional screening with a detector wand, its important to talk to the person screening you about your stimulator.
Medical Diagnosis and Treatment
Occupational Electromagnetic Concerns
You May Like: Can Sleep Apnea Cause Parkinson’s Disease
Will I Still Need To Take Medications After Deep Brain Stimulation
Depending on the disease, it may be possible to reduce medications. However, DBS is most helpful when used along with medications and other treatments. That’s because using it and other treatments at the same time means it may be possible to lower medication doses, have fewer side effects and still get the same benefits.
Who Is Not A Good Candidate For Dbs
You are not a good candidate for DBS if:
- You do not have a clear diagnosis of Parkinson’s disease.
- You have Parkinsons plus or an atypical form of the disease. Parkinsons plus disorders include multiple system atrophy, progressive supranuclear palsy and vascular parkinsonism. DBS might make these disorders worse.
- You have certain brain conditions, such as ischemic brain disease, demyelinating brain disease or brain tumors.
- You are not healthy enough for surgery.
If you are evaluated for DBS and not a candidate, your OHSU movement disorders neurologist will recommend other options.
Read Also: Occupational Therapy And Parkinson’s Disease
Top Patient Complaint About Dbs Device: Ineffective Stimulation
Now, researchers at Vanderbilt University Medical Center, in Tennessee, where the trial took place, reported five-year results regarding medication costs. They also projected such costs through 15 years to reflect the mean time for Parkinsons to progress from early to advanced stages the time when a typical patient may be offered DBS.
Data from motor symptom-targeting medications, collected at each visit, were used to calculate and project medication costs.
The analysis included 28 participants who completed at least one follow-up visit. They had a mean age of 61.1 and had lived with the disease for a mean of 2.1 years at study entry.
The results showed that the mean annual Parkinsons medication cost had increased from $4,941 at the studys start to $14,177 after five years for patients receiving standard medication alone. For the DBS group, the costs increased from $4,507 to $6,636.
This represented a 2.4 times lower annual medication cost and a five-year cumulative cost reduction of $28,246 for patients receiving both DBS and standard medication relative to the control group.
Patients originally assigned to medication alone also were five times more likely to have higher medication costs than those in the DBS group.
In addition, annual medication costs at 15 years using 10% annual cost increases to account for disease progression were projected to reach $30,371 for the control group and $14,216 for the DBS group.
How Dbs Is Advancing Parkinson’s Treatment
Deep brain stimulation can improve the lives of people with movement disorders.
Movement disorders, like Parkinson’s Disease or Essential Tremor, can have a significant impact on the quality of someone’s everyday life.
These neurological disorders are characterized by symptoms such as the loss of muscle control, tremors, balance issues, trouble with coordination and involuntary movements.
The number of people living with movement disorders continues to grow. For example, 60,000 Americans are diagnosed with Parkinson’s every year and an estimated 10 million people have the condition worldwide. That’s why innovations in Parkinson’s treatment are critical.
Deep brain stimulation provides targeted therapy for people with Parkinson’s Disease or essential tremor. It’s care that can be tailored to their unique needs as precision and personalization become integral to the way healthcare providers deliver care.
Advancing Parkinson’s Treatment
The typical course of treatment for people with Parkinson’s involves medication that increases levels of dopamine, which helps control movement and emotions, in the brain. However, these medications become less effective at providing reliable symptom control over time.
Though DBS is used in combination with medications prescribed for Parkinson’s, this treatment is typically recommended when medication alone no longer controls symptoms adequately.
How DBS Does It
Managing Treatment with the Touch of a Button
References
You May Like: What Time Of Day Are Parkinson’s Symptoms Worse
What Happens Before Deep Brain Stimulation
Before this procedure, your healthcare provider will discuss the advantages and disadvantages of having a DBS device implanted. Theyll also explain the possible risks that come with this surgery. Theyll also verify that you can have this surgery, which can involve other imaging scans or lab tests to look for any reasons you may not be able to have the procedure.
If you still decide you want to have the DBS implanted, your provider will then have you get detailed magnetic resonance imaging and computed tomography scans of your brain. These scans will help your provider decide which location is the best place to place the wires for the DBS.
Before the procedure, your provider will also talk to you about the following:
Maximizing Therapy Minimizing Side Effects
The directional DBS works with Medtronics Percept PC neurostimulator to capture a patients brain signals and provide objective data to better understand how medication or stimulation changes affect the patient. The technology enhances the detection of local field potentials small electrical signals generated by the brain that are 1 million times smaller than DBS stimulation pulses.
The ability to record and identify the patients brain activities, along with directional capabilities to steer the currents of the electrodes, allows us to maximize the therapeutic benefits and minimize the side effects for our patients, says Brian Dalm, MD, a neurosurgeon in the Ohio State Wexner Medical Center Department of Neurological Surgery.
At the Ohio State Wexner Medical Center, patients receive DBS treatment at the Center for Neuromodulation.
With a combined neurology and neurosurgery team, we work together to identify patients, prepare them for surgery, and handle all of their postoperative programming needs, Dr. Dalm says.
During a DBS procedure, electrodes are implanted into the brain and connected to a small, pacemaker-like device placed under the skin of the chest. The device sends electrical pulses to specific points in the brain to calm abnormal signals that control movement. This can reduce disabling symptoms and restore physical function.
Recommended Reading: How To Care For A Person With Parkinson’s Disease
What Are The Results
Successful DBS is related to 1) appropriate patient selection, 2) appropriate selection of the brain area for stimulation, 3) precise positioning of the electrode during surgery, and 4) experienced programming and medication management.
For Parkinson’s disease, DBS of the subthalamic nucleus improves the symptoms of slowness, tremor, and rigidity in about 70% of patients . Most people are able to reduce their medications and lessen their side effects, including dyskinesias. It has also been shown to be superior in long term management of symptoms than medications .
For essential tremor, DBS of the thalamus may significantly reduce hand tremor in 60 to 90% of patients and may improve head and voice tremor.
DBS of the globus pallidus is most useful in treatment of dyskinesias , dystonias, as well as other tremors. For dystonia, DBS of the GPi may be the only effective treatment for debilitating symptoms. Though recent studies show little difference between GPi-DBS and STN-DBS.
Patients report other benefits of DBS. For example, better sleep, more involvement in physical activity, and improved quality of life .
Research suggests that DBS may “protect” or slow the Parkinson’s disease process .
What Happens After Surgery
After surgery, you may take your regular dose of Parkinson’s medication immediately. You are kept overnight for monitoring and observation. Most patients are discharged home the next day.
During the recovery time after implanting the electrodes, you may feel better than normal. Brain swelling around the electrode tip causes a lesion effect that lasts a couple days to weeks. This temporary effect is a good predictor of your outcome once the stimulator is implanted and programmed.
About a week later, you will return to the hospital for outpatient surgery to implant the stimulator in the chest/abdomen. This surgery is performed under general anesthesia and takes about an hour. Patients go home the same day.
Step 7: implant the stimulator You will be taken to the OR and put to sleep with general anesthesia. A portion of the scalp incision is reopened to access the leads. A small incision is made near the collarbone and the neurostimulator is implanted under the skin. The lead is attached to an extension wire that is passed under the skin of the scalp, down the neck, to the stimulator/battery in the chest or abdomen. The device will be visible as a small bulge under the skin, but it is usually not seen under clothes.
You will have lifting and activity restrictions for 6-8 weeks while the incisions heal. Follow all discharge instructions and the neck exercises provided. Incision pain can be managed with medication.
Don’t Miss: Does Parkinson’s Cause Alzheimer’s
Placement Of The Neurostimulator
This procedure takes place under general anesthesia so that the person is asleep. The surgical team inserts the neurostimulator under the outer layers of skin, usually just under the collarbone, but sometimes in the chest or abdomen. The extension wire from the lead is attached to the neurostimulator.
Opening Doors For Treating Other Movement Disorders
Soon, patients with epilepsy and other movement disorders could also receive treatment with the new directional and sensing DBS technology.
There is currently active research going on throughout the world to better understand how sensing the brains activity can be utilized to improve therapeutic outcomes, and this does not have to be limited strictly to essential tremor or Parkinsons disease, Dr. Dalm says.
As advances in personalization continue for DBS, doctors and patients can expect therapy that is eventually more tailored to each individual patients physiology, he says.
Tractography-based targeting and each patients individual brain activity will more accurately set stimulation parameters, he says.
DBS in the future will likely move away from mostly anatomical placement of the lead to a more precise placement that provides the most accurate stimulation for each patient based on the best intensity, rate and stimulation pattern for them.
Recommended Reading: What Are Some Symptoms Of Parkinson’s Disease
Up To Five Additional Hours Of Good Movement Without Dyskinesia
Good movement control means no troubling symptoms like shaking, stiffness, and difficulty moving. DBS therapy can provide up to five additional hours of good movement control without dyskinesia per day, compared with medication alone.*2,3,4 What would you do with five additional hours every day?
*Measured by the UPDRS IV
Open Loop Dbs Or Conventional Dbs
cDBS is the most commonly used strategy in PD with a known efficacy on different targets .6 However, since no sensor is used for feedback control of the electrical stimulation, cDBS is associated with several problems. Programming in cDBS is intricate and time consuming, and therefore needs very skilled staff.6 cDBS needs frequent reprogramming, which adds to the treatment cost of an already costly procedure. Further continuous stimulation is associated with shorter battery life, requiring frequent surgical procedures to change battery.6 Hence, other DBS technologies are continuously being assessed to improve patient experience and reduce treatment cost.
Also Check: What Are The Effects Of Parkinson’s Disease
Dbs Surgery For Parkinsons Disease
Deep brain stimulation is a surgical procedure used to treat a variety of disabling neurological symptomsmost commonly the debilitating symptoms of Parkinsons disease , such as tremor, rigidity, stiffness, slowed movement, and walking problems. The procedure is also used to treat essential tremor, a common neurological movement disorder. At present, the procedure is used only for patients whose symptoms cannot be adequately controlled with medications.
Deep brain stimulation, or DBS, uses tiny electrodes surgically implanted into part of the brain. The electrodes are connected by a wire under the skin to a small electrical device called a pulse generator that is implanted in the chest beneath the collarbone. The pulse generator and electrodes painlessly stimulate the brain in a way that helps to stop many of the symptoms of PD. DBS is stereotactic surgery, meaning it uses a 3D coordinate mapping system to locate tiny areas in our bodies in order to perform surgery accurately.
DBS usually reduces the need for levodopa and related drugs, which in turn decreases dyskinesias. It also helps to relieve on-off fluctuation of symptoms. People who initially responded well to treatment with levodopa tend to respond well to DBS. While the benefits of DBS can be substantial, it usually does not help with speech problems, “freezing,” posture, balance, anxiety, depression, or dementia.
The patient is then taken to the operating room:
