Signs Of Parkinsons Disease
In 1817, Dr. James Parkinson published An Essay on the Shaking Palsy describing non-motor, as well as, motor symptoms of the illness that bears his name. Parkinsons is not just a movement disorder, explained Dr. Shprecher. Constipation, impaired sense of smell, and dream enactment can occur years before motor symptoms of Parkinsons. The latter, caused by a condition called REM sleep behavior disorder, is a very strong risk factor for both Parkinsons and dementia . This has prompted us to join a consortium of centers studying REM sleep behavior disorder.
Stage Two Of Parkinsons Disease
Stage two is still considered early disease in PD, and it is characterized by symptoms on both sides of the body or at the midline without impairment to balance. Stage two may develop months or years after stage one.
Symptoms of PD in stage two may include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities, soft voice, monotone voice, fading volume after starting to speak loudly, slurring speech, stiffness or rigidity of the muscles in the trunk that may result in neck or back pain, stooped posture, and general slowness in all activities of daily living. However, at this stage the individual is still able to perform tasks of daily living.
Diagnosis may be easy at this stage if the patient has a tremor however, if stage one was missed and the only symptoms of stage two are slowness or lack of spontaneous movement, PD could be misinterpreted as only advancing age.
What Are The Symptoms Of End
Stage four for Parkinsons disease is often called advanced Parkinsons disease because people in this stage experience severe and incapacitating symptoms. This is when medication doesnt help as much and serious disabilities set in.
Theres an increased severity in:
- How you speak a softer voice that trails off.
- Falling and trouble with balance and coordination.
- Freezing a sudden, but temporary inability to move, when you start to walk or change direction.
- Moving without assistance or a wheelchair.
- Other symptoms such as constipation, depression, loss of smell, low blood pressure when going to stand up, pain, and sleep issues.
Many times someone with advanced PD cant live on their own and needs help with daily tasks.
Stage five is the final stage of Parkinsons, and assistance will be needed in all areas of daily life as motor skills are seriously impaired. You may:
- Experience stiffness in your legs. It may make it impossible to walk or stand without help.
- Need a wheelchair at all times or are bedridden.
- Need round-the-clock nursing care for all activities.
- Experience hallucinations and delusions.
As Parkinsons disease progresses into these advanced stages, its symptoms can often become increasingly difficult to manage. Whether you or your loved one with end-stage Parkinsons lives at home, in an assisted living facility or a nursing home, hospice services can optimize your quality of life and that of your family members as well.
Also Check: Freddie Roach Medical Condition
Treatment For Atypical Parkinsonism Symptoms
Because PD medication response is poor in these syndromes, treatment focuses on symptom management e.g. physical therapy for fall prevention, speech therapy to maximize communication, swallow therapy to prevent aspiration.
Other symptoms that can be addressed include dystonia, myoclonus, blood pressure dysfunction and urinary dysfunction.
Tips and takeaways:
- Atypical parkinsonism is a very complicated group of diseases that are hard to diagnose. Sometimes a neurologist will change the diagnosis as new symptoms develop or become more apparent.
- Despite the fact that these conditions typically do not respond well to medications for PD, many of the presenting symptoms can be addressed, so make sure to raise all of your concerns with your neurologist.
Do you have a question or issue that you would like Dr. Gilbert to explore? Suggest a Topic
Dr. Rebecca Gilbert
APDA Vice President and Chief Scientific Officer
Stage Four Of Parkinsons Disease
In stage four, PD has progressed to a severely disabling disease. Patients with stage four PD may be able to walk and stand unassisted, but they are noticeably incapacitated. Many use a walker to help them.
At this stage, the patient is unable to live an independent life and needs assistance with some activities of daily living. The necessity for help with daily living defines this stage. If the patient is still able to live alone, it is still defined as stage three.
Don’t Miss: Is Parkinson’s Disease Terminal
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
The Role Of Levodopa In Pd Gait Progression
Although the precise mechanisms of non-dopaminergic gait control are unclear, emerging evidence suggests the importance of the cholinergic system . Cholinergic neurons in the pedunculopontine nucleus influence gait and postural control , and slower walking speed in PD is associated with increases in short-latency afferent inhibition and cholinergic denervation . Also, deep brain stimulation within the PPN may improve step velocity suggesting interventions that target brain regions not primarily dependent on dopamine may therefore help to mitigate gait impairment in PD. The benefits of drugs targeting the cholinergic system on PD gait are also being explored . Overall, interpretation of the relationship between dopamine and gait progression is limited as gait was not assessed off medication, nor were biomarkers of dopaminergic activity such as DAT imaging used. Nevertheless, our findings indicate that discrete gait characteristics progress irrespective of levodopa, suggesting the importance of non-dopaminergic mechanisms in gait impairment.
Recommended Reading: Does Restore Gold Work For Parkinson’s
Symptoms Of Atypical Parkinsonism
PD symptoms vary from person to person. Some people have a tremor, usually on one side of the body. Others with PD have muscle freezing or balance difficulties. You might have PD symptoms that are mild for years. Someone else may have symptoms that worsen quickly.
Atypical Parkinsonian syndromes each have their own set of symptoms:
- VP: Gait and balance problems are common symptoms. Dementia, incontinence, and palsy also develop.
- LBD: Thinking and memory decline. Hallucinations, delusions, and difficulty staying alert are also symptoms.
- MSA: Walking and balance problems are common with this condition. You may also have symptoms related to autonomic dysfunction. This is when the autonomic nervous system doesnt function as it should. The ANS controls automatic bodily functions like breathing, digestion, and circulation. These symptoms might include:
- incontinence
- a sudden drop in blood pressure when you stand up
Associations Between Gait Changes And Change In Levodopa Dose Over Time
LEDD increased by 106 mg/day each year. Ninety-three percent of people with PD had increased LEDD compared to baseline assessment . Only one gait characteristic was related to LEDD change larger increases in step width variability related to greater increases in LEDD over time . Inclusion of the LEDD × Time interaction resulted in no significant change in step width variability , indicating that step width variability change is at least partially explained by a change in LEDD. All other gait characteristics meeting criteria 1 and 3 did not show associations between gait change and LEDD change and therefore exhibited disease-specific change that was not related to levodopa adjustments .
Recommended Reading: Can You Die From Parkinson’s Disease
Study Participants And Baseline Assessments
One-hundred and thirty control and 109 PD participants completed at least two assessments, so were included in this analysis . At baseline, PD participants had similar age, height, mass, and NART scores to controls . The PD group had proportionately more males, poorer global cognition , lower mood , poorer balance confidence , and were slower performing the sit-to-stand test . The mean time to baseline assessment from PD diagnosis was 6 months, and from the first subjective motor symptom was 27 months. Motor score severity at baseline was low 10% had already experienced FOG and most were taking dopaminergic medication, in keeping with clinical practice. Thirty-one percent of people with PD were taking medication with an anticholinergic burden although the overall burden was low, with a mean score of 0.7, which may reflect increased clinician awareness of the adverse outcomes associated with anticholinergic in PD. For both groups, participants who completed the 72-month assessment were younger and had better baseline performance on the MoCA compared to non-completers who did not attend a 72-month assessment . Additionally, PD completers had better balance and less severe motor disease at baseline than non-completers.
If You Live In South Jersey And Have Questions About The Final Stages Of Parkinsons Disease Or Hospice Care For Your Loved One Please Call Samaritan At 229
Samaritan is a member of the National Partnership for Healthcare and Hospice Innovation, a network of not-for-profit hospice and palliative providers across the country. If you know someone outside of our service area who is living with advanced illness and can benefit from hospice or palliative care, please call 1 -GET-NPHI for a referral to a not-for-profit provider in your area.
Don’t Miss: Early Warning Signs Of Parkinson’s Disease
Pd Vs Atypical Parkinsonism
Symptoms of PD come on gradually as neurons in a part of the brain called the substantia nigra begin to die.
Doctors arent sure exactly what causes the cells to die. Theyve linked it to a misfolding of certain proteins in the brain. This could set off a reaction among other proteins, which start to form clumps and damage the brain. Over time, this leads to the loss of muscle control and dementia that characterize Parkinsons.
Symptoms of PD and atypical Parkinsonism are often similar. For this reason, Parkinsonism is sometimes initially misdiagnosed as PD. This is why testing and imaging are so important in making an accurate diagnosis.
Researchers are working on ways to take images inside the living human brain of proteins associated with PD and Parkinsonism. Live brain imaging of these proteins would greatly boost doctors ability to diagnose and monitor these disorders.
One main difference between the two conditions is that atypical Parkinsonism symptoms tend to come on earlier than they do in typical PD. Symptoms such as falling, dementia, and hallucinations occur earlier in atypical Parkinsonism disorders.
PD symptoms often appear first on one side of the body. With atypical Parkinsonism, signs are often present on both sides at the beginning.
Another key difference between PD and atypical Parkinsonism is whats happening in the brain.
Progression Of Gait Impairment Over 72 Months

In both groups, gait characteristics from all five domains significantly progressed over 72 months. Progression was more extensive in the PD cohort. In basic change models, ten of sixteen characteristics significantly changed in PD compared to seven characteristics in controls . In PD, gait became significantly slower, with a shorter step length, greater variability , reduced asymmetry , wider step width, and faster steps . Gait also became significantly slower in controls, with shorter steps, greater variability , greater asymmetry , wider step width, and faster swing time. Variation was considerable between individuals in the trajectories of change for each gait characteristic . The overall severity of PD-related motor symptoms also worsened as shown by a 3.0 point increase per year in the UPDRS III .
Figure 2. Change in gait over 6 years for control and Parkinsons disease participants for gait characteristics that demonstrated a significant change in PD related to disease progression. Panel shows gait characteristics that significantly changed in PD but not controls so demonstrated change related to disease progression only. Panel shows gait characteristics that significantly changed in PD and control groups, but the rate of change was greater in PD, so demonstrated change related to both aging and disease progression. Bold lines show overall change within each group faint lines show change for individuals.
Read Also: Is Parkinson’s Disease Fatal
Are There Any Factors That Slow Or Increase The Pace Of Parkinsons
Though there is currently no drug to halt the progression of the Parkinsons, there are some factors that can alter how quickly it develops. There is a growing body of evidence to suggest that regular exercise and healthy eating can slow the progression of Parkinsons, says Dr Stott.
For example, researchers in the Netherlands have recently demonstrated in a randomised clinical trial that six months of exercising slowed the progression of 65 people with Parkinsons .
Inactivity and social isolation also appear to be associated with faster progression, hence the need to encourage affected individuals to partake in regular exercise ideally in a social environment, he adds.
An investigation into the genetics of Parkinsons shows some promise as to explaining the difference in progression among patients. Dr Stott explains: There is evidence indicating that some genetic variations can influence the speed of progression some variations are associated with increased rate of progression, while others result in a slower rate. We are not sure why these genetic variations are having these effects, but the biology is currently being explored.
What Causes Parkinsons Disease
Parkinsons disease occurs when nerve cells in an area of the brain called the substantia nigra become impaired or die. These cells normally produce dopamine, a chemical that helps the cells of the brain communicate . When these nerve cells become impaired or die, they produce less dopamine. Dopamine is especially important for the operation of another area of the brain called the basal ganglia. This area of the brain is responsible for organizing the brains commands for body movement. The loss of dopamine causes the movement symptoms seen in people with Parkinsons disease.
People with Parkinsons disease also lose another neurotransmitter called norepinephrine. This chemical is needed for proper functioning of the sympathetic nervous system. This system controls some of the bodys autonomic functions such as digestion, heart rate, blood pressure and breathing. Loss of norepinephrine causes some of the non-movement-related symptoms of Parkinsons disease.
Scientists arent sure what causes the neurons that produce these neurotransmitter chemicals to die.
Recommended Reading: What Are Early Warning Signs Of Parkinson’s Disease
Predicting Rates And Patterns Of Progression In Parkinson Disease
Predicting progression in patients with Parkinson disease continues to be an elusive clinical goal. Overlapping etiologies with a variety of other Parkinsonian disorders such as progressive supranuclear palsy and multiple system atrophy, which have more rapid progression patterns, makes initial diagnosis more challenging. In addition, the tools to accurately measure rates of disease progression, including peripheral biomarkers, have not yet been identified.
According to David K. Simon, MD, PhD, director of the Parkinsons Disease & Movement Disorders Center at Beth Israel Deaconess Medical Center in Boston, Massachusetts, numerous factors likely contribute to the rate of progression, with different combinations of factors showing relevance for individual patients. Dr Simon told Neurology Advisor that the possibilities include genetic factors , physical exercise, diet, exposure to pesticides, perhaps exposure to certain medications or metabolic factors such as whether or not a person has diabetes or metabolic syndrome, or levels of uric acid. But an important related problem is that we dont know for sure if these factors truly do have any impact on rate of progression. And if they do, that relationship to progression is likely to be complex with interactions between different mechanisms, he said.
Known Predictive Features
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Also Check: What Color Is The Ribbon For Parkinson’s
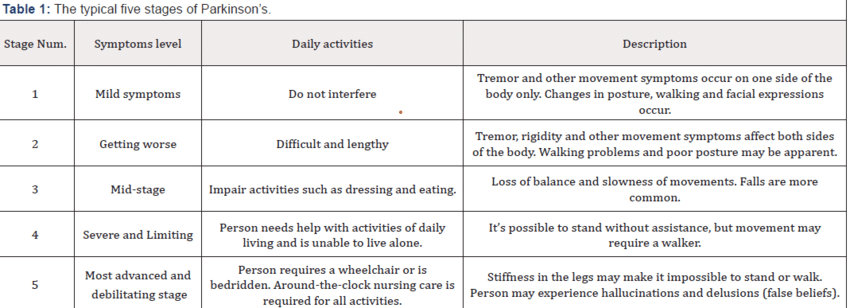
The 5 Stages Of Parkinsons Disease
Getting older is underrated by most. Its a joyful experience to sit back, relax and watch the people in your life grow up, have kids of their own and flourish. Age can be a beautiful thing, even as our bodies begin to slow down. We spoke with David Shprecher, DO, movement disorders director at Banner Sun Health Research Institute about a well-known illness which afflicts as many as 2% of people older than 65, Parkinsons Disease.
What Are The Stages Of Parkinsons
Doctors sometimes use five stages to describe the progress of Parkinsons disease. Each stage presents changing or new symptoms that a person is likely to encounter.
It is worth noting that not everyone will reach the advanced stages. For some people, the symptoms remain mild, and they can continue to live independently and be mobile.
Dividing the condition into stages helps doctors and caregivers understand and address some of the challenges a person is experiencing as it progresses.
Recommended Reading: Parkinsons Genetic Link
Stages Of Parkinsons Disease
Experts have identified a general Parkinsons progression and created a set of Parkinsons stages, which can help determine where you are at in the disease and what your prognosis might be. However, not everybody progresses through Parkinsons disease in the same way or on the same time frame. Some people skip stages or rapidly progress to later stages. Others live for many years with mild or moderate Parkinsons and never reach the more advanced stage of the illness.
Here are five commonly recognized stages of Parkinsons, including what symptoms you might expect. Treatment also can occur during these stages to help prevent or delay later stages of the illness. This can include medication, , and lifestyle changes, such as a healthy diet and exercise program.
