Neural Mechanisms Underlying Parkinsonian Resting Tremor
Parkinsonian tremor is caused mainly by central, rather than peripheral mechanisms . Evidence for this view comes from work showing that peripheral deafferentation , peripheral anaesthesia of tremulous muscles and mechanical perturbations have little effect on Parkinson’s disease tremor although peripheral reflexes may interact with central oscillations .
Neuronal correlates of Parkinson’s disease tremor. Simultaneous recording of thalamic posterior VL single-unit activity and peripheral EMG during tremor in a parkinsonian patient. These data show continuous synchronization between internal globus pallidus activity and peripheral EMG. Reprinted from , with permission from the Society for Neuroscience. Simultaneous recording of internal globus pallidus multi-unit activity and peripheral EMG during tremor in a patient with Parkinson’s disease . The two plots illustrate the raw signals of two epochs of data sampled 5min apart. Note that in the left trace the peaks in the spike density function coincide with the EMG bursts, whereas in the right trace the oscillations in the spike density function occur at a lower frequency than the EMG. These data show that synchronization between neuronal activity in internal globus pallidus and peripheral EMG is transient in nature. Reprinted from . Copyright National Academy of Sciences, USA.
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Characteristics Of Pd Tremors
The tremors of PD characteristically occur at rest, stop with voluntary action, and recur again after you hold your new position for a few minutes. PD tremors can affect the hands, arms, face, jaw, legs, and/or feet, and are often slightly more prominent on one side than the other.
The tremor almost always begins in the hand before affecting other parts of the body, and it usually looks like you are rolling a pill between your thumb and index finger. Thats why its called a pill-rolling tremor.
A pill-rolling tremor is the most common type of PD tremor, but shaking tremorswhich may involve the hands or other areas of the bodycan also occur.
What Causes Parkinson Disease
Parkinson disease arises from decreased dopamine production in the brain. The absence of dopamine makes it hard for the brain to coordinate muscle movements. Low dopamine also contributes to mood and cognitive problems later in the course of the disease. Experts don’t know what triggers the development of Parkinson disease most of the time. Early onset Parkinson disease is often inherited and is the result of certain gene defects.
What Medications Are Used To Treat Parkinsons Disease

Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal; and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Is Parkinsons Disease Inherited
Scientists have discovered gene mutations that are associated with Parkinsons disease.
There is some belief that some cases of early-onset Parkinsons disease disease starting before age 50 may be inherited. Scientists identified a gene mutation in people with Parkinsons disease whose brains contain Lewy bodies, which are clumps of the protein alpha-synuclein. Scientists are trying to understand the function of this protein and its relationship to genetic mutations that are sometimes seen in Parkinsons disease and in people with a type of dementia called Lewy body dementia.
Several other gene mutations have been found to play a role in Parkinsons disease. Mutations in these genes cause abnormal cell functioning, which affects the nerve cells ability to release dopamine and causes nerve cell death. Researchers are still trying to discover what causes these genes to mutate in order to understand how gene mutations influence the development of Parkinsons disease.
Scientists think that about 10% to 15% of persons with Parkinsons disease may have a genetic mutation that predisposes them to development of the disease. There are also environmental factors involved that are not fully understood.
What Treatments Are Available
Many Parkinson’s patients enjoy an active lifestyle and a normal life expectancy. Maintaining a healthy lifestyle by eating a balanced diet and staying physically active contributes to overall health and well-being. Parkinson’s disease can be managed with self-care, medication, and surgery.
Self careExercise is as important as medication in the treatment of PD. It helps maintain flexibility and improves balance and range of motion. Patients may want to join a support group and continue enjoyable activities to improve their quality of life. Equally important is the health and well being of the family and caregivers who are also coping with PD. For additional pointers, see Coping With Parkinsons Disease.
These are some practical tips patients can use:
Medications There are several types of medications used to manage Parkinson’s. These medications may be used alone or in combination with each other, depending if your symptoms are mild or advanced.
After a time on medication, patients may notice that each dose wears off before the next dose can be taken or erratic fluctuations in dose effect . Anti-Parkinsons drugs can cause dyskinesia, which are involuntary jerking or swaying movements that typically occur at peak dosage and are caused by an overload of dopamine medication. Sometimes dyskinesia can be more troublesome than the Parkinsons symptoms.
The Tremors Of Parkinson’s Disease
The distinction between these different tremors is not always visible to the naked eye. For example, resting tremor can re-emerge during postural holding, making it difficult to clinically distinguish it from essential tremor. This distinction can be made by focusing on the delay between adopting a posture and the emergence of tremor: in essential tremor there is no delay, while Parkinson’s disease resting tremor re-emerges after a few seconds . Since the frequency of re-emergent and resting tremor can be similar, it has been hypothesized that both tremors share a similar pathophysiological mechanism. One interesting patient with Parkinson’s disease had no resting tremor, but a marked 36Hz postural tremor that occurred after a delay of 24s following postural holding , thus resembling re-emergent tremor. Such observations point to heterogeneity in the circumstances under which the classical Parkinson’s disease resting tremor occurs.
In the following sections, we will mainly focus on the classic resting tremor in Parkinson’s disease. We will first describe the clinical and cerebral differences between patients with tremor-dominant and non-tremor Parkinson’s disease. Then we will detail how these differences may inform us about the causes and consequences of Parkinson’s disease resting tremor.
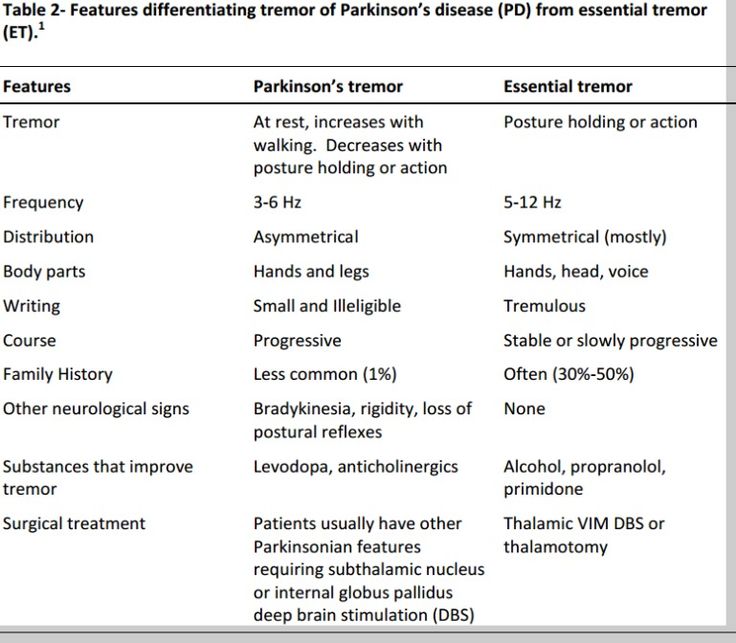
Confusion With Essential Tremor
The tremor of Parkinsons disease is often confused with the tremor of a condition called Essential Tremor, or Benign Familial Tremor . Katherine Hepburn had Essential Tremor, and was originally misdiagnosed with Parkinsons. Ronald Reagan also had Essential Tremor. Both had a head tremor and a vocal tremor. In Essential Tremor, the hands are most commonly involved, followed by the head and then the voice. Essential Tremor can also cause the jaw to tremor, and it may be difficult to figure out if a jaw tremor is from Essential Tremor or Parkinsons. Unfortunately, some people may have both disorders. Some authorities believe that there is, in fact, an increased association between the two conditions, so that more people with Parkinsons disease have Essential Tremor than would be expected by chance alone, but this has not been established.
Tremors Not Associated With Parkinsons Disease
There are different types of tremors, of which not all are associated with Parkinsons disease, and they vary slightly in terms of how, when and where they manifest in the body. They include essential tremor and dystonic tremor and may be associated with other conditions and genetic mutations, although a specific gene has not been identified.
A patient with a Parkinsons tremor typically will find that their symptoms worsen and spread to other parts of the body over time. Generally, the tremor starts in one hand and can progress to the arm and foot on the same side of the body, and then eventually to the other side of the body. In severe cases, tremors also can affect the jaw or lips.
Psychological And Physiological Anxiety Measures
Repeated measures ANOVA indicated a significant effect on phase and group × phase interaction for VAMS anxiety factor . However, no difference was found between the groups . With regard to other VAMS factors, there was a significant effect of phase on mental sedation , physical sedation , and other feelings . However, there were no significant effects of these parameters on group × phase interaction and the groups.
Figure 1
Repeated measures ANOVA showed a significant effect of phase on heart rate without differences between the groups or group × phase interaction. Moreover, there were no differences in systolic or diastolic blood pressure between the phases, groups, or group × phase interaction.
Sleep Disturbances In Parkinson’s Disease
In general, research seems to indicate that people with Parkinson’s disease have more sleep disruptions than similarly aged people without the disease. The most commonly reported sleep-related problems are the inability to sleep through the night and difficulty returning to sleep after awakening, generally referred to as maintenance insomnia. Unlike many older adults, patients with Parkinsons disease often find that they have no trouble initiating sleep, but often wake up within a few hours and find sleeping through the rest of the night to be difficult. People with Parkinson’s disease also report daytime sleepiness, nightmares, vivid dreams, nighttime vocalizations, leg movements/jerking while asleep, restless legs syndrome, inability to or difficulty turning over in bed, and awakenings to go to the bathroom.
Although all the reasons for these sleep changes are unknown, potential explanations include reactions to/side effects of medications and awakening due to symptoms such as pain, stiffness, urinary frequency, tremor, dyskinesia, depression and/or disease effects on the internal clock.
How Is A Diagnosis Made
Because other conditions and medications mimic the symptoms of PD, getting an accurate diagnosis from a physician is important. No single test can confirm a diagnosis of PD, because the symptoms vary from person to person. A thorough history and physical exam should be enough for a diagnosis to be made. Other conditions that have Parkinsons-like symptoms include Parkinsons plus, essential tremor, progressive supranuclear palsy, multi-system atrophy, dystonia, and normal pressure hydrocephalus.
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as or scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
What Is The Difference Between Hdl And Ldl Cholesterol
LDL cholesterol is short for Low Density Lipoprotein. Most people are aware that HDL cholesterol is considered the good cholesterol and that LDL is the bad cholesterol.
Consider this: LDL cholesterol is considered bad because it has a higher content of fat than HDL cholesterol. Both, HDL and LDL cholesterol are antioxidants though. They help heal and protect tissues.
Even the bad LDL cholesterol helps repair damaged tissues. The problem with LDL cholesterol is that it repairs the damaged tissues with cholesterol that has more fat in it than what is considered healthy.
However, it is still repairing tissue. This is another example of the body healing itself. Ideally, LDL cholesterol levels will be low and HDL cholesterol levels will be high so that if a part of your body gets inflamed, it will repair with the good HDL cholesterol.
This is especially important for someone with high levels of homocysteine like Janice. Homocysteine damages the inner lining of the arteries . When this damage occurs, LDL will create foam cells or fibrous plaques in the arteries.
This creation of plaques is what can lead to arteriosclerosis and atherosclerosis and that is exactly how high levels of homocysteine is considered a significant risk factor for a stroke or heart attack.
Im especially proud of Janice. I call her my rock star. She took ownership of her health and through my guidance, got herself healthy and has stayed that way.
Health is Happiness,
Dr. Keith Currie
How Is Tremor Treated
Although there is no cure for most forms of tremor, treatment options are available to help manage symptoms. In some cases, a persons symptoms may be mild enough that they do not require treatment.
Finding an appropriate treatment depends on an accurate diagnosis of the cause. Tremor caused by underlying health problems can sometimes be improved or eliminated entirely with treatment. For example, tremor due to thyroid hyperactivity will improve or even resolve with treatment of thyroid malfunction. Also, if tremor is caused by medication, discontinuing the tremor-causing drug may reduce or eliminate this tremor.
If there is no underlying cause for tremor that can be modified, available treatment options include:
Medication
Focused Ultrasound
A new treatment for essential tremor uses magnetic resonance images to deliver focused ultrasound to create a lesion in tiny areas of the brains thalamus thought to be responsible for causing the tremors. The treatment is approved only for those individuals with essential tremor who do not respond well to anticonvulsant or beta-blocking drugs.
Surgery
When people do not respond to drug therapies or have a severe tremor that significantly impacts their daily life, a doctor may recommend surgical interventions such as deep brain stimulation or very rarely, thalamotomy. While DBS is usually well tolerated, the most common side effects of tremor surgery include dysarthria and balance problems.
Lifestyle changes
Models Explaining The Occurrence Of Parkinsonian Resting Tremor
Several hypotheses have been put forward to explain the occurrence of resting tremor in Parkinson’s disease. As outlined above, there is evidence that both the basal ganglia and the cerebello-thalamo-cortical circuit are implicated in tremor. However, most models are based on detailed recordings in a limited set of neurons or a limited set of structures . Therefore, most models focus on a node in a single circuit and interpret the changes in other circuits as secondary. Here we will place concurrent changes in two separate circuits into perspective. This section also updates and elaborates on earlier reviews about the pathophysiology of parkinsonian tremor .
What Are The Symptoms Of Tremor
Symptoms of tremor may include:
- a rhythmic shaking in the hands, arms, head, legs, or torso
- shaky voice
- difficulty writing or drawing
- problems holding and controlling utensils, such as a spoon.
Some tremor may be triggered by or become worse during times of stress or strong emotion, when an individual is physically exhausted, or when a person is in certain postures or makes certain movements.
Types Of Parkinsons Tremors
Quivering in these parts of the body can be signs of Parkinson’s:
- Finger Twitching Commonly seen among patients in the early stages of the disease, this symptom is also called a pill-rolling tremor because the fingers and hand appear to be rolling a pill-sized object.
- Jaw Tremors This movement in the jaw may resemble a slow shivering and disappear while eating or talking. In some cases, the teeth chatter. Patients may chew gum to stop the trembling.
- Foot Tremors This shakiness may appear while resting, lying down, or dangling the feet. It stops when standing and walking. It can also extend beyond the feet and cause the whole leg to vibrate.
- Tongue Tremors Although far less reported than other types of tremor, quivering in tongue can be a revealing manifestation of Parkinsons, according to an article published in December 2015 in the journal Movement Disorders Clinical Practice. The shaking can also appear in the chin, lips, and face.
While these types of tremors can help doctor identify Parkinsons, about 30 percent of patients do not have these movements, per prior research. Those people who do not have a resting tremor may not get a diagnosis immediately, says Gilbert. If doctors dont see it, they wont necessarily think a person has Parkinsons.
What Are The Complications Of Parkinson Disease
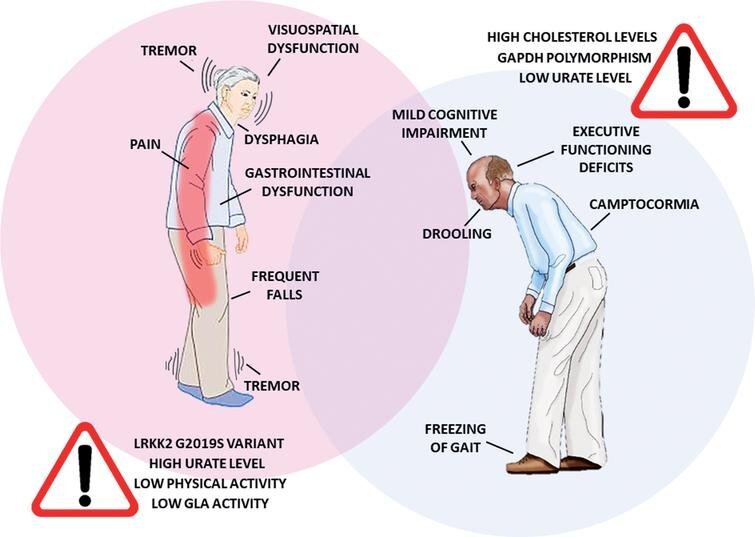
Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may arise later. As the disease gets worse with time, many people develop dementia. This can cause profound memory loss and makes it hard to maintain relationships.
Parkinson disease dementia can cause problems with:
- Speaking and communicating with others
- Problem solving
- Forgetfulness
- Paying attention
If you have Parkinson disease and dementia, in time, you likely won’t be able to live by yourself. Dementia affects your ability to care of yourself, even if you can still physically do daily tasks.
Experts don’t understand how or why dementia often occurs with Parkinson disease. Its clear, though, that dementia and problems with cognitive function are linked to changes in the brain that cause problems with movement. As with Parkinson disease, dementia occurs when nerve cells degenerate, leading to chemical changes in the brain. Parkinson disease dementia may be treated with medicines also used to treat Alzheimer’s disease, another type of dementia.
Which Body Parts Do Parkinsons Tremors Affect
There are five main places youâll have Parkinsonâs tremors:
1. Hands. Parkinsonâs disease tremors often start in the fingers or hands with whatâs called a pill-rolling motion. Imagine holding a pill between your thumb and index finger and rolling it back and forth.
2. Foot. A Parkinsonâs foot tremor is more likely to happen while youâre sitting or lying down with your feet at rest. If the tremor moves into your thigh muscles. It could look like your whole leg is shaking.
Foot tremors disappear when you stand or walk because those are active movements. A foot or leg tremor while youâre standing may be another condition.
3. Jaw. This is common in people with Parkinsonâs. It may look like youâre shivering. It can become bothersome if the tremor makes your teeth chatter. If you wear dentures, it could make them shift or fall out.
Chewing eases the tremor, so gum might help.
4. Tongue. Itâs rare, but a tongue tremor can cause your entire head to shake.
5. Internal. Some people with Parkinsonâs say they can feel a shaking sensation in their chest or abdomen. But canât be seen from the outside.
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, it’s called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. It’s also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesn’t go away and continues to get worse over time.
Other Tremors And How It Differs
A Parkinsonian tremor has a few distinct characteristics, though it may be easy to confuse with other types of tremors depending on the other symptoms a person shows. Doctors will look for and rule out other types of tremors to confirm their diagnosis.
The National Institute of Neurological Disorders and Stroke notes that some common tremors include:
Dopamine is an important neurotransmitter that plays a critical role in a number of bodily functions, such as movement and coordination. People with Parkinsons disease produce less dopamine, which may cause them to experience movement-related problems, such as rigidity, slowness of movement, poor balance, and tremors.
Low levels of dopamine may disrupt the way the brain processes movement, which can result in movement problems. Evidence suggests that many people with Parkinsons disease lose 6080% of dopamine-producing cells in the brain by the time they present symptoms.
Other causes of tremors unrelated to Parkinsons disease can include:
- certain medications
Movementtremor Interactions In The Cerebello
A beat of tremor preceding movement in Parkinson’s disease. Fast flexion patterns in patients with Parkinson’s disease. In many patients with Parkinson’s disease , although resting tremor was not continuously present, a single beat of tremor occasionally occurred before the pattern that moved the limb. This is illustrated for one patient. Adapted from with permission from BMJ Publishing Group Ltd.
Tremor Is An Independent Symptom
Tremor may have a pathophysiology different from most other Parkinson’s disease symptoms. First, tremor does not progress at the same rate as bradykinesia, rigidity, gait and balance . Second, tremor severity does not correlate with other motor symptoms . Third, tremor can occur on the body side contralaterally to the otherwise most affected side, i.e. where bradykinesia and rigidity are most prominent. This so-called wrong-sided tremor is seen in 4% of patients with Parkinson’s disease . Finally, tremor responds less well to dopaminergic treatment than bradykinesia and rigidity .
