What Is Carbidopa And Levodopa
Carbidopa and levodopa is a combination medicine used to treat symptoms of Parkinsons disease, such as stiffness or tremors.
Carbidopa and levodopa is also used to treat Parkinson symptoms caused by carbon monoxide poisoning or manganese intoxication.
Carbidopa and levodopa may also be used for purposes not listed in this medication guide.
Levodopa In Combination With Carbidopa
Most of the times, neurologists and other doctors recommend intake of Levodopa in combination with Carbidopa. This helps in the entry of more Levodopa within the brain and thereby, allows far better functions. Carbidopa belongs to decarboxylase inhibitors. It thus performs functions by simply preventing the breakage of Levodopa before it goes into the human brain. In this way, it helps in reducing levodopa dosage, which may cause less vomiting and nausea.
An Approach To The Treatment Of Parkinson’s Disease
No treatment can arrest or slow neurodegeneration in Parkinson’s disease. The aim is to relieve symptoms and avoid the complications of therapy.
Early Parkinson’s disease
Many studies have shown that early treatment with dopamine agonists reduces the incidence of dyskinesia.1Fewer motor fluctuations were shown in some but not all of the studies. We recommend a dopamine agonist as the first treatment in younger patients who have mild disease and no cognitive deficit. It is necessary to add levodopa within 1-5 years in most patients. In more severe disease, treatment begins with levodopa but a dopamine agonist may be added to keep the daily dose of levodopa in the lower range if there is no cognitive deficit. Dopamine agonists are used infrequently and with caution in patients more than 70 years old because of the risk of neuropsychiatric adverse effects and postural hypotension. They are contraindicated in the presence of dementia.
Isolated resting tremor is rarely disabling, but if it interferes with function it can usually be managed with levodopa. When this is ineffective at low to moderate doses, the addition of an anticholinergic can sometimes be useful.
Patients with motor fluctuations
Role of physical therapy and surgery
Also Check: What Are The Best Exercises For Parkinson’s Disease
Improving Mobility Strength And Balance
Staying mobile and self-sufficient is top of mind for people living with Parkinson disease. Stiffness is also a known problem with the disease. This rigidity can cause poor posture and pain that leads to other functional problems. A physical therapist can help with these problems. PTs guide people with Parkinson through moves and stretches to increase mobility, strength, and balance.
Why Do I Have To Take Levodopa So Frequently
Short answer: Once levodopa gets into your bloodstream , it doesnt last long most of it is gone after about 2-3 hours, and then you need to take more. The resulting rapid oscillations in blood levels of the drug are responsible for both on-off cycling and dyskinesia.
Longer answer: All drugs get cleared out of your body on some timescale. Thats largely a good thing your body is well-designed to get rid of foreign compounds, through a combination of chemically modifying the drugs and then eliminating them through the urine or the bile, for example. The study of these types of processes is called pharmacokinetics.
The rate at which a drug disappears from your bloodstream can be described in terms of a half-life: the time it takes for half of the drug to disappear. This rate is primarily a property of the drug, but it can vary a bit between patients. Suppose that the half-life is 2 hours, a fairly typical number for levodopa . L-DOPA is absorbed pretty quickly, at least when your stomach is empty, so lets say that you take a pill at 9:30 am, and by 10 am most of it has been absorbed, such that there is a total of 100 mg of levodopa in your blood. Using the half-life of two hours, only 50 mg will be left by noon. And then when another 2 hours pass , only 25 mg left. Theoretically, it never goes to zero, but it does fall pretty darn quickly, and in advanced patients, you can transition to an off state once it falls below some threshold.
Don’t Miss: Does Parkinson’s Cause Muscle Wasting
How Carbidopa/levodopa Is Used To Treat Parkinsons Disease Symptoms
Loss of neurons in the brain that use dopamine to communicate is one of the hallmark features of Parkinsons disease , causing slowness, stiffness, tremor and balance problems. Replacing the brains dopamine is therefore one of the key treatment strategies to help improve the motor symptoms of PD. Dopamine itself does not cross the blood-brain barrier and therefore cant be used to treat PD. Instead, levodopa, a precursor of dopamine, which does cross the blood-brain barrier is used. If levodopa is ingested by itself however, it breaks down in the bloodstream before it crosses into the brain, so levodopa is typically ingested with another medication that stops it from breaking down. In the US, the combination of carbidopa/levodopa is used.
Carbidopa/levodopa is the mainstay of treatment for PD and is the most effective medication currently available for PD. APDA research support played a role in the discovery of levodopa for PD treatment when we funded the work of Dr. George C. Cotzias back in the 1960s.
This previous blog answers common questions regarding carbidopa/levodopa.
While carbidopa/levodopa remains the most effective medication for people with PD, it is available in various strengths and delivery systems which makes understanding all the available levodopa options very confusing. To help you make sense of the many options, I will describe the various levodopa formulations and the rationale for using each one.
What Other Information Should I Know
Keep all appointments with your doctor and the laboratory. Your doctor will order certain lab tests to check your response to levodopa and carbidopa.
Before having any laboratory test, tell your doctor and the laboratory personnel that you are taking levodopa and carbidopa.
Levodopa and carbidopa can lose its effect completely over time or only at certain times during the day. Call your doctor if your Parkinson’s disease symptoms worsen or vary in severity.
As your condition improves and it is easier for you to move, be careful not to overdo physical activities. Increase your activity gradually to avoid falls and injuries.
Levodopa and carbidopa can cause false results in urine tests for sugar and ketones .
Do not let anyone else take your medication. Ask your pharmacist any questions you have about refilling your prescription
It is important for you to keep a written list of all of the prescription and nonprescription medicines you are taking, as well as any products such as vitamins, minerals, or other dietary supplements. You should bring this list with you each time you visit a doctor or if you are admitted to a hospital. It is also important information to carry with you in case of emergencies.
You May Like: Can You Be Tested For Parkinson’s
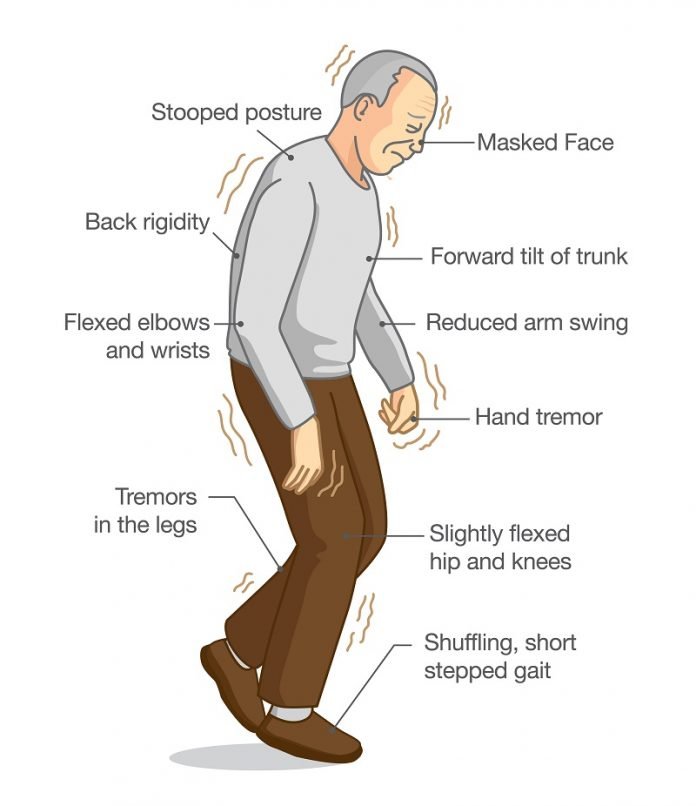
What Are The Symptoms
The best-known symptoms of Parkinson’s disease involve loss of muscle control. However, experts now know that muscle control-related issues aren’t the only possible symptoms of Parkinson’s disease.
Motor-related symptoms
Motor symptoms which means movement-related symptoms of Parkinsons disease include the following:
Additional motor symptoms can include:
- Blinking less often than usual. This is also a symptom of reduced control of facial muscles.
- Cramped or small handwriting. Known as micrographia, this happens because of muscle control problems.
- Drooling. Another symptom that happens because of loss of facial muscle control.
- Mask-like facial expression. Known as hypomimia, this means facial expressions change very little or not at all.
- Trouble swallowing . This happens with reduced throat muscle control. It increases the risk of problems like pneumonia or choking.
- Unusually soft speaking voice . This happens because of reduced muscle control in the throat and chest.
Non-motor symptoms
Several symptoms are possible that aren’t connected to movement and muscle control. In years past, experts believed non-motor symptoms were risk factors for this disease when seen before motor symptoms. However, theres a growing amount of evidence that these symptoms can appear in the earliest stages of the disease. That means these symptoms might be warning signs that start years or even decades before motor symptoms.
Non-motor symptoms include:
Stages of Parkinsons disease
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinsons. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Don’t Miss: How Long Can A Person Live With Stage 5 Parkinson
Myth #: Levodopa Is Toxic To Neurons And Contributes To Disease Progression
FACTS: The question of whether levodopa is toxic to neurons and accelerates disease progression has been studied in numerous ways over the past three decades, without conclusive evidence that it does so. In fact, levodopa has been shown to increase life expectancy in people with PD, which strongly argues that levodopa does not accelerate the disease. In addition, levodopa has been shown in clinical trials to improve quality of life for people with PD.
In summary, the effectiveness of levodopa is unparalleled for people with PD, and as such, it is important to understand the facts about the medication and not get confused or deterred by common myths that could keep you from benefitting from this treatment. Always talk to your doctor openly about any concerns or questions you have so together you can make an informed decision that best suits your personal situation.
Managing Medication Interactions And Side Effects
All prescribed medications can have potential side effects, including those used to treat Parkinsons. Some things you think are symptoms of Parkinsons may actually be side effects of medication. Some peoples side effects will have a big impact on their lives and have to be kept under control along with the symptoms.
Recommended Reading: Ot Interventions For Parkinson’s Disease
Symptomatic And Neuroprotective Therapy
Pharmacologic treatment of Parkinson disease can be divided into symptomatic and neuroprotective therapy. At this time, there is no proven neuroprotective or disease-modifying therapy.
Levodopa, coupled with carbidopa, a peripheral decarboxylase inhibitor , remains the gold standard of symptomatic treatment for Parkinson disease. Carbidopa inhibits the decarboxylation of levodopa to dopamine in the systemic circulation, allowing for greater levodopa distribution into the central nervous system. Levodopa provides the greatest antiparkinsonian benefit for motor signs and symptoms, with the fewest adverse effects in the short term however, its long-term use is associated with the development of motor fluctuations and dyskinesias. Once fluctuations and dyskinesias become problematic, they are difficult to resolve.
Monoamine oxidase -B inhibitors can be considered for initial treatment of early disease. These drugs provide mild symptomatic benefit, have excellent adverse effect profiles, and, according to a Cochrane review, have improved long-term outcomes in quality-of-life indicators by 20-25%.
Neuroprotective therapy aims to slow, block, or reverse disease progression such therapies are defined as those that slow underlying loss of dopamine neurons. Although no therapy has been proven to be neuroprotective, there remains interest in the long-term effects of MAO-B inhibitors. Other agents currently under investigation include creatine and isradipine.
Final Thoughts On Using Cbd Oil For Parkinsons

There is no cure for Parkinsons disease. Once diagnosed, patients can only slow their progression.
However, there are ways to manage its pesky symptoms. One of them is using CBD oil. If youre planning to try it out, remember to make an appointment with your doctor first. This is to make sure that you dont experience any side effects of potential drug interactions. In addition, your doctor can also give you professional advice on finding the right dose.
Although more research is needed to confirm the benefits of CBD oil for Parkinsons disease, the best product that may support official treatment is Royal CBD oil. Made from organic hemp and using supercritical CO2, this product is pure, safe, and available in a wide range of potencies to suit different CBD needs.
Do you know anyone who takes CBD oil to cope with the symptoms of Parkinsons disease? Does it help? Let us know in the comment section below!
Don’t Miss: What Is Shuffling Gait Parkinson’s Disease
Stay Safe With Your Medicines
Read all labels carefully.
- Tell all your health care providers about all the medicines and supplements you take.
- Know all the medicines and foods youâre allergic to.
- Review any side effects your medicines can cause. Most reactions will happen when you start taking something, but thatâs not always the case. Some reactions may be delayed or may happen when you add a drug to your treatment. Call your doctor right away about anything unusual.
- Use one pharmacy if possible. Try to fill all your prescriptions at the same location, so the pharmacist can watch for drugs that might interact with each other.
- You can use online tools to see if any of your medicines wonât work well together.
You have the right and responsibility to know what medications your doctor prescribes. The more you know about them and how they work, the easier it will be for you to control your symptoms. You and your doctor can work together to create and change a medication plan. Make sure that you understand and share the same treatment goals. Talk about what you should expect from medications so that you can know if your treatment plan is working.
Show Sources
Keeping A Motor Diary
You can help your doctor understand how effective your medications are by keeping diary. Typically a motor diary, or wearing off diary, will include details such as:
- the times of day when you take your Parkinsons medication
- the times of day when you have good symptom control
- which symptoms re-emerge during the day and when
- what symptoms you experience at night
- any other complications you may experience, such as dyskinesia, and their relation to when you take your medication
- it can also be useful to note the timing of meals, drinks and snacks. Make a note of whether eating certain foods affects your symptom control protein, for example, can interfere with the absorption of some medications.
For a sample diary and information on keeping one see Keeping a diary.
Don’t Miss: Solutions For Parkinson’s Disease
Influence Of Sex On Nms: Onset Analysis
We compared mean values for NMS for the 3 cohorts categorized by sex of subject .
Prevalence of NMS at onset, categorized by sex. NMS mean scores were categorized by sex of participant or male ) for Parkinsons disease , SWEDD , and healthy controls . NMS scales analyzed are displayed A through Q indicating the score range in the title. Higher number indicates more dysfunction except for MoCA Cognition and USPIT Olfaction . Pairwise differences within the cohort were evaluated with independent-samples MannWhitney U test with Bonferroni correction for multiple comparisons. Differences between cohorts for each sex were evaluated using the independent-samples KruskalWallis test. Statistical differences within cohorts males) are indicated by an asterisk . Post hoc analyses signifying differences between the HC, PD, and SWEDD cohorts are indicated for females and males as a=HC versus PD, b=HC versus SWEDD, and c=PD versus SWEDD. p< 0.05.
Within the PD cohort, females reported significantly higher mean scores for overall autonomic dysfunction ), thermoregulatory dysfunction ), anxious mood ), and pain and other sensations ). Males reported a significantly higher degree of sexual dysfunction ), urinary dysfunction ), cognitive dysfunction and 1), and hyposmia ).
Within the SWEDD cohort, females reported significantly higher mean scores for gastrointestinal dysfunction and 1), anxious mood ), and pain and other sensations ).
What Is Levodopa + Carbidopa
Levodopa + carbidopa in combination is used to treat the symptoms of Parkinson’s disease, or Parkinson-like symptoms such as tremor, shakiness, stiffness, and difficulty moving. Levodopa changes into dopamine, a chemical in the brain that helps control movement. Carbidopa prevents levodopa changing to dopamine in the bloodstream. This means that more levodopa can enter the brain, and it helps to lessen some of the side effects such as nausea and vomiting . Levodopa becomes less effective over time. This is because it treats the symptoms of Parkinson’s but cannot stop the dopamine-producing cells from being lost. This means that as they are lost you will continue to get symptoms and need more frequent doses over time. Your brain cant become resistant to levodopa. People with Parkinsons will benefit from medications containing levodopa throughout their lifetime.
Don’t Miss: Is Parkinson’s Disease Infectious Or Noninfectious
How Do I Take Care Of Myself
If you have Parkinsons disease, the best thing you can do is follow the guidance of your healthcare provider on how to take care of yourself.
- Take your medication as prescribed. Taking your medications can make a huge difference in the symptoms of Parkinson’s disease. You should take your medications as prescribed and talk to your provider if you notice side effects or start to feel like your medications aren’t as effective.
- See your provider as recommended. Your healthcare provider will set up a schedule for you to see them. These visits are especially important to help with managing your conditions and finding the right medications and dosages.
- Dont ignore or avoid symptoms. Parkinsons disease can cause a wide range of symptoms, many of which are treatable by treating the condition or the symptoms themselves. Treatment can make a major difference in keeping symptoms from having worse effects.