Stage Five Of Parkinsons Disease
Stage five is the most advanced and is characterized by an inability to rise from a chair or get out of bed without help, they may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
Around-the-clock assistance is required at this stage to reduce the risk of falling and help the patient with all daily activities. At stage five, the patient may also experience hallucinations or delusions.
While the symptoms worsen over time, it is worth noting that some patients with PD never reach stage five. Also, the length of time to progress through the different stages varies from individual to individual. Not all the symptoms may occur in one individual either. For example, one person may have a tremor but balance remains intact. In addition, there are treatments available that can help at every stage of the disease. However, the earlier the diagnosis, and the earlier the stage at which the disease is diagnosed, the more effective the treatment is at alleviating symptoms.
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage
Parkinsons progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinsons about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinsons may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more off periods when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinsons symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinsons most often die because of an infection or another condition, usually caused by Parkinsons.
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
Also Check: What Are Early Warning Signs Of Parkinson’s Disease
Is Parkinsons Disease Inherited
Scientists have discovered gene mutations that are associated with Parkinsons disease.
There is some belief that some cases of early-onset Parkinsons disease disease starting before age 50 may be inherited. Scientists identified a gene mutation in people with Parkinsons disease whose brains contain Lewy bodies, which are clumps of the protein alpha-synuclein. Scientists are trying to understand the function of this protein and its relationship to genetic mutations that are sometimes seen in Parkinsons disease and in people with a type of dementia called Lewy body dementia.
Several other gene mutations have been found to play a role in Parkinsons disease. Mutations in these genes cause abnormal cell functioning, which affects the nerve cells ability to release dopamine and causes nerve cell death. Researchers are still trying to discover what causes these genes to mutate in order to understand how gene mutations influence the development of Parkinsons disease.
Scientists think that about 10% to 15% of persons with Parkinsons disease may have a genetic mutation that predisposes them to development of the disease. There are also environmental factors involved that are not fully understood.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Recommended Reading: What Are Early Warning Signs Of Parkinson’s Disease
How Long Can A Person Live With Stage 5 Parkinson
When patients reach stage five the final stage of Parkinson’s disease they will have severe posture issues in their back, neck, and hips. In end–stage of Parkinson’s disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
One may also ask, what do Parkinson’s patients usually die from? But the most common cause of death in those with Parkinson’s is pneumonia, because the disease impairs patients‘ ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
what happens in stage 5 Parkinson’s?
Stage Five of Parkinson’s Disease Stage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
How quickly can Parkinson’s progress?
While symptoms and disease progression are unique to each person, knowing the typical stages of Parkinson’s can help you cope with changes as they occur. Some people experience the changes over 20 years or more. Others find the disease progresses more quickly.
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinsons disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable reducing symptoms during on periods and no longer controlling symptoms during off periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they cant. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
Recommended Reading: How Long Do Parkinson’s Patients Live
What Is Palliative Care
Palliative care is defined by the World Health Organization as an approach that improves the quality of life of patients and their families, when they are facing challenges related to life-threatening conditions. Palliative care was first introduced for pain management and focused mainly on people with cancer, but its reach has broadened by now involving other chronic conditions that deteriorate physical and mental conditions. These include neurodegenerative conditions such as Parkinsons disease.
Various models for implementing palliative care exist, with adaptations in specific social, economic and cultural settings. As prevalence of neurodegenerative diseases increases in ageing populations, the need for palliative care services will continue to grow.
What Are The Non
Parkinson’s disease stages are defined by the severity of a patient’s motor symptoms and how much those symptoms impact one’s ability to function every day. But there are non-motor symptoms that are more likely to develop later in the disease, too, and a doctor may take those into consideration when assessing someone with the disorder.
For example, people with late-stage Parkinson’s disease might have difficulty chewing, eating, speaking, or swallowing , which is considered both a motor and non-motor symptom. Dysphagia in particular can lead to serious health problems like malnutrition, dehydration, and aspiration.
In the final stages of Parkinson’s disease, a person might develop cognitive changes, including slowness of memory or thinking, trouble planning and accomplishing tasks, and difficulty concentrating. Or they might notice changes in their bone health or vision.
But there’s no telling for sure if or when these symptoms will occur in any individual because Parkinson’s disease symptoms vary from person to person.
Recommended Reading: Does Sam Waterston Have Parkinson
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38 and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patients handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
Hospice Care For Late Stage Parkinsons
There are a number of reasons why choosing to have home health care services for Parkinson patients is one of the best options. Hospice care for late stage Parkinsons is extremely important.
- End of Life 40% of those who were in a long term care facility died alone without a family member being with them. Every person in the study listed who had in home health care and hospice had at least 1 significant family member or loved one with them at the time of their passing.
- Satisfaction 83% of those who utilized hospice were satisfied to highly satisfied with their experience. They cited their satisfaction with the ability to handle the extreme grief and handling of the symptoms of the disease as two of the main reasons for being appreciative with the care received.
- Focus Hospice care for late stage Parkinsons focuses on comfort care, symptom care, grief counseling and acceptance. Maintaining a level of understanding and comfort for both the patient and their loved ones is a primary goal.
We can see the importance of a loved one remaining at home as they battle PD, especially as they move towards the final stages of the disease. Above & Beyond Home Health Care can be there for you with professional hospice care for late stage Parkinsons so you know that your loved one is provided for with the best care possible.
Cited Works:
End of Life Care for a Person with Parkinson Disease Dept. of Education
Recommended Reading: What Is The Life Expectancy Of Someone With Parkinson’s Disease
Managing The Terminal Phase
When the terminal phase can be anticipated by an acceleration in the patient’s global deterioration, a decision may have been taken with the patient and family not to treat further episodes of infection. A careful check for specific symptoms should be sought from the patient directly or from observing the patient for any signs of distress. Close family members will often recognise signs of unspoken distress. The views of experienced clinical staff may determine if the patient is frightened, in pain or has different nursing requirements.
For patients unable to swallow in the terminal stage, medication can be administered subcutaneously as needed or continuously using a syringe driver. Medication can be given, if necessary, to relieve specific symptoms as follows:
-
midazolam for fear or agitation
-
hyoscine butylbromide for drooling or chesty secretions
-
morphine for pain
If pain is present, a sufficient dose of morphine should be used to relieve it but without causing undesirable opioid side effects.
Bilateral Or Midline Involvement Without Impairment Of Balance
Months or years later similar symptoms and signs are noticed on the opposite side of the body, or other signs appear in midline what physicians call Axial signs. These may include: bilateral loss of facial expression decreased blinking speech abnormalities soft voice, monotony, fading volume after starting to speak loudly, slurring, stiffness of truncal muscles making the patient appear awkward and stiff or resulting in neck and back pain postural abnormalities causing stooping, generalized slowness in, but still capable of, carrying out all activities of daily living, sometimes an aggravation to those waiting for the patient to complete tasks.
Usually the diagnosis is easy at this Stage if it has been preceded by a clear cut tremor or other symptom on one side. But not all Parkinson’s patients have tremor or other definite signs of Stage I unilateral Parkinsonism. If Stage I was missed and the predominant symptoms at Stage II are only slowness and a lack of spontaneous movement, the diagnosis may still be in doubt. For example, even in Stage II, Parkinsonism may be interpreted as only advancing age.
You May Like: What Is The Life Expectancy Of Someone With Parkinson’s Disease
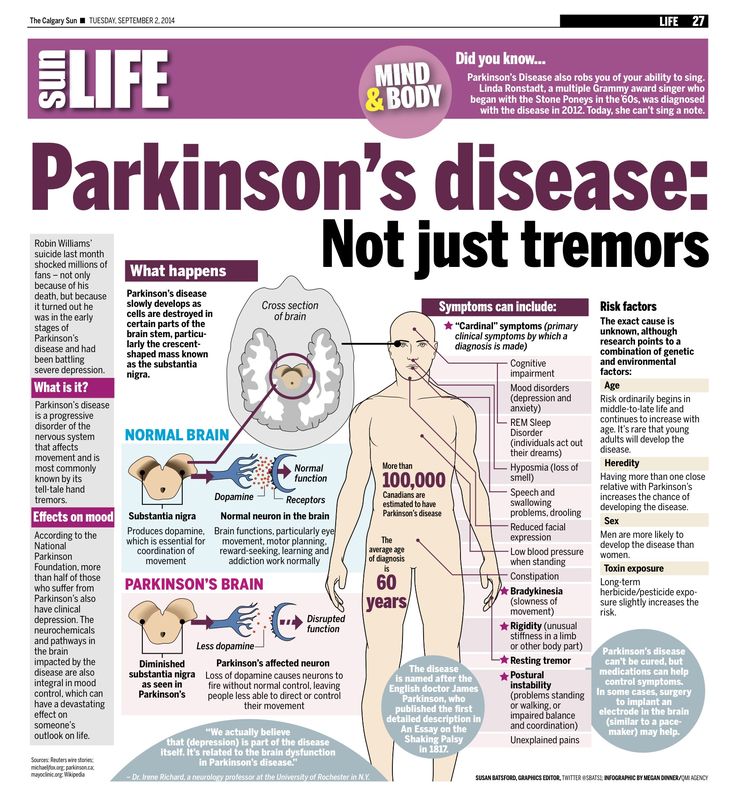
What Are The Causes Of Parkinsons Disease
Even with in-depth studies and research, the leading cause of Parkinsons disease is still unknown.
However, this disease is explained through the loss of nerve cells in the substantia nigra, a section of the brain where dopamine is produced. When this nerve cells damage goes up to 80%, symptoms of the disorder become more evident.
Dopamine is the hormone messenger that helps the brain and the nervous system to coordinate movements. When dopamine decreases, the message is not as clear, making it hard to control body movements such as walking and talking.
Only 10% to 15% of Parkinsons disease cases are attributed to genetics. Most of these cases are discovered at a later stage, making it hard to prevent them.
The other 85% to 90% can be because of an individuals surroundings. Environmental toxicants such as pesticides and herbicides can damage the cell and increase the risk of having Parkinsons disease, although only by a modest degree.
Some researchers also argue that this disorders main culprit is the mixture of both genetics and the environment. Despite the many theories surrounding this disease, the evidence of why it exists remains inconclusive.
Fully Developed Severely Disabling Disease The Patient Is Still Able To Walk And Stand Unassisted But Is Markedly Incapacitated
The patient is unable to lead an independent life because of the need for help with some activities of daily living. It is this inability to live alone which marks the transition from Stage III to Stage IV. No matter how difficult it is for him/her, if the patient still is able to live alone, his/her disease is at Stage III not Stage IV. The patient at Stage IV however, does remain able to stand and walk unassisted.
You May Like: Postural Instability In Parkinson’s Disease
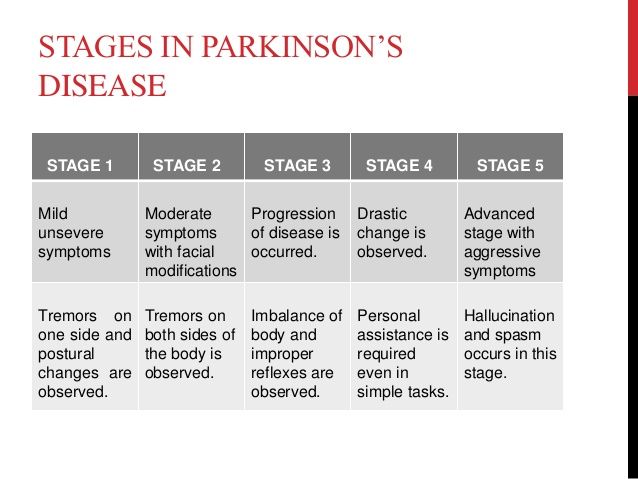
The Stages Of Parkinsons Disease
Stage One The Initial Stage: Symptoms are generally mild and may be easier to hide. Common symptoms include tremors, poor posture, balance issues, stooping of the back, and shaking of the limbs.
Stage Two Both Sides of the Body are Affected: The Parkinsons now affects both sides of the body, with increased symptoms that are more noticeable. Daily tasks become more difficult as symptoms now affect the entire body. It is harder to maintain your balance, walking becomes more difficult and tremors/shaking is more frequent.
Stage Three Increased symptoms & overall slowing down: By stage 3 the typical symptoms are more pronounced and the list of symptoms becomes more inclusive. One of the most noticeable changes is that movements and actions are much slower including facial expressions, speech, and motor skills. It is common to common to feel light headed, fainting, and experience hypo-tension .
Stage Five The Final Stage: During the final stages the person will require 24/7 one on one care and nursing skills. By stage 5, hospice care for late stage Parkinsons is a necessity and will help everyone involved with the acceptance of the final stage of the disease.Our trained hospice providers will guide you through these final stages. Our goal is to focus on the patient and the family unit as a whole.
Managing Care In Late Stages
, March 3, 2017
What to expect in the late stages of Parkinson’s disease and the challenges of caring with those difficulties and needs. Tips for helping someone overcome freezing, accomplishing activities of daily living as long as possible, managing medications and swallowing issues, and ways to minimize caregiver stress.
You May Like: Parkinson Disease Old Age Onset
Is Parkinsons Disease Fatal
Parkinsons disease itself doesnt cause death. However, symptoms related to Parkinsons can be fatal. For example, injuries that occur because of a fall or problems associated with dementia can be fatal.
Some people with Parkinsons experience difficulty swallowing. This can lead to aspiration pneumonia. This condition is caused when foods, or other foreign objects, are inhaled into the lungs.
What Are The Important Points Regarding Apomorphine At The End Of Life
Apomorphine is a dopamine agonist, which is given as a subcutaneous infusion either continuously or intermittently and also as single subcutaneous injections. An overview of studies into apomorphine use shows improvement in motor off periods and in dyskinesias.39
Apomorphine has side-effects similar to other dopaminergic medication but also notably nausea and vomiting. Ondansetron is not recommended for nausea in patients using apomorphine due to adverse effects.21
Subcutaneous apomorphine has been used at the end of life in a patient with advanced PD although with the recommendation that this is by a healthcare professional experienced in its use.40
Recommended Reading: Parkinsons And Genetics
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
