Determination Of Malassezia Yeasts Enzyme Production By Apizym Assay
The activity of 19 different enzymes produced by Malassezia was tested using the API Zym assay . A total of 26 Malassezia isolates from SD groups were tested for: proteases , lipases , phosphatases , glycosidases . Results were expressed semi-quantitatively, ranging from no activity to maximum enzymatic activity.
Does Parkinsons Disease Cause Hives
Hives are raised welts that can be extremely itchy. They can appear red or pink in lighter skin tones, but this reddening may not be visible in darker skin tones.
Hives can be very small and separate, or they can form together to cover large areas of the body. They often occur in batches or clusters and may frequently change in appearance.
Hives are typically triggered by an allergic reaction. But they can also be caused by other irritants. Triggers can include:
- foods, such as eggs, nuts, or shellfish
- insect stings or bites
For the most part, doctors dont associate Parkinsons disease with hives. But there are some Parkinsons disease medications that can cause a rash in some people.
For example, according to one 2017 study , carbidopa and levodopa formulations are sometimes compounded with a yellow dye that can possibly cause a rash.
This is considered to be a very rare side effect. But if you experience allergic reactions after taking one of your medications, talk with your doctor or pharmacist about switching to another formulation.
Malassezia Over Proliferate In Aids
Over proliferation of normally well-tolerated microbes is frequently observed in immunodeficient patients. The very first symptoms of AIDS often involve the over proliferation of fungi, such as Candida in the mouth , Malassezia on the skin , or Pneumocystis in the lungs . Such fungi are normally present in healthy individuals , and are considered benign members of the human microbiome.
Latent microbes which are not considered part of the normal microbiome can also cause severe illness in AIDS patients. Toxoplasma gondii is a protist which colonizes the CNS of a large subset of the population for life . It rarely causes severe symptoms in immunocompetent individuals, but often causes life-threatening encephalitis in AIDS patients or during immunosuppression . Though much rarer today, Treponema pallidum also colonizes the CNS of infected individuals for life, typically without causing symptoms until old age . AIDS hastens neurosyphilis in previously asymptomatic Treponema pallidum carriers, placing young patients at an unusually high risk of this disease .
Recommended Reading: Does Exercise Slow The Progression Of Parkinson’s
Malassezia And Parkinson’s Disease
Beyond the strong association between PD and SD, and preliminary evidence of Malassezia‘s presence inside the CNS, three additional lines of evidence support a direct contribution of Malassezia in PD: many PD risk alleles affect lipid metabolism , Malassezia invasiveness and melanin production are both stimulated by L-DOPA , and low CD4+ T cell counts observed in PD might contribute to the over proliferation of microbes such as Malassezia.
The Role Of Cannabinoid Use In The Treatment Of Sd
Considering Malassezias implication in the pathogenesis of SD, mitigating fungal proliferation and localized inflammation is essential to treatment. Hence, topical antifungals are often used to reduce the proliferation of Malassezia while topical corticosteroids are used to minimize skin inflammation. Additional level A recommended treatments include lithium , which works by reducing the release of fatty acids in the skin, and tacrolimus . For severe recalcitrant SD, as seen in neurological disorders such as PD, only systemic antifungal therapies have been shown to have some efficacy . They are also known, however, to be hepatotoxic, and alternative therapies could be of benefit. Currently, both in vitro and in vivo reports support the potential use of cannabinoids in the treatment of inflammatory skin disorders although studies are few .
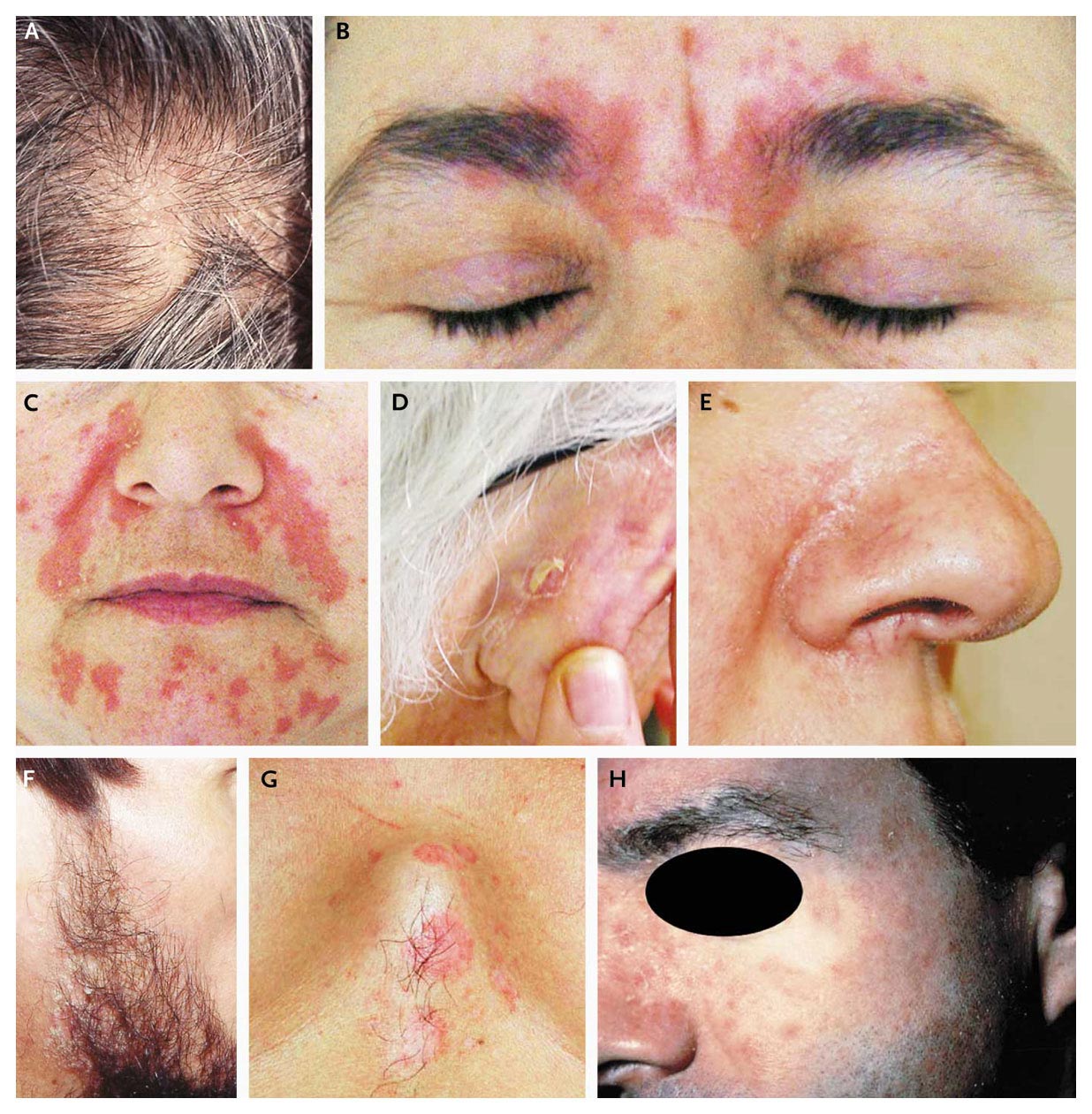
Lipid production by sebaceous glands is important in understanding the pathogenesis of SD. It has been shown that patients had more extensive skin desquamation than healthy individuals. Oleic acid has irritant and desquamative effects and is a byproduct of host lipid consumption by Malassezia . Sebum dysregulation appears to play an important role in the pathogenesis of SD. Studying the effects of cannabinoids on sebum production may aid in understanding the potential benefits of oral cannabinoids in SD treatment.
Fig. 1.
Also Check: Can Parkinson’s Symptoms Be Something Else
Additional Clues From Autonomic Nervous System Issues Seen In Aids
The connection between AIDS and seborrheic dermatitis has already been previously mentioned in this book, but lets review it once again in the context of the nervous system.
Out of all health conditions, HIV AIDS appears to have the strongest influence on the likelihood of the individual developing seborrheic dermatitis .
One way to look at this connection is that AIDS has a disastrous impact on immune function, allowing the most common suspect of seborrheic dermatitis, the malassezia yeast, to proliferate freely and wreak havoc on the skin surface. In this line of thought, the immune system and its ability to properly deal with malassezia yeasts are at the heart of the resulting skin symptoms.
However, another way to look at this connection is to consider the impact of AIDS on the autonomic nervous system. And a quick review of the literature reveals the following:
- Autonomic nervous system dysfunction is common amongst individuals infected with HIV
- Damage of the autonomic nerve fiber is a hallmark of HIV and occurs early in the course of the infection
- A possible reason for HIV to promote sympathetic bias is to improve its survival rate by changing the balance of the TH-1/TH-2 immune response
Improving autonomic balance through cardiovascular exercise Interestingly, one of the most straightforward methods to reduce the impact of HIVs effect on the autonomic immune function is through improvement of cardiovascular fitness .
Natural Treatment For Seborrheic Dermatitis
Natural treatment for seborrheic dermatitis is safe and effective. There are many modalities that fall under the category of natural treatment for seborrheic dermatitis and in this article we will discuss all pros and cons. If youre suffering from seborrheic dermatitis, the symptoms can be very discomforting, and if your child is affected by it, it can be stressful for you as a parent. Its a very common condition, and the symptoms usually go away on its own. However, you can take certain measures to speed up the healing process. Many people dont feel comfortable using conventional and allopathic treatments, which often have a high risk of side effects. As a result, many people are resorting to a natural treatment for seborrheic dermatitis to deal with the condition.
You May Like: Good Exercises For Parkinsons Disease
Read Also: Does Parkinson’s Affect Your Legs
Parkinsons Disease And Excessive Sweating
Excessive sweating, also known as hyperhidrosis, is the most common sweating issue seen in people with Parkinsons disease. It involves intense episodes of sweating that can drench your clothes and bedding.
These episodes can significantly affect daily life and make it hard to get a good nights sleep.
Excessive sweating can also lead to heat rash, which can cause symptoms that resemble hives. Heat rash happens when sweat gets trapped beneath the skin.
Sweating And Parkinsons Medications
Excessive sweating may happen at any time, or it may be connected to your Parkinsons disease medications.
If you take carbidopa and levodopa , you may notice you experience periods of excessive sweating when your medication is wearing off or not working as effectively as it should.
Anticholinergics, a different type of Parkinsons medication, can sometimes contribute to a lack of sweating.
2017 study , people with Parkinsons disease may be at increased risk of melanoma. Melanoma is a type of cancer that begins in skin cells called melanocytes.
Researchers in the study above estimated that the risk of developing melanoma is two times higher in those with Parkinsons disease when compared to those who dont have a Parkinsons diagnosis.
Only about 1 percent of skin cancers are melanomas. But even though it is uncommon, even in people with Parkinsons disease, its a good idea to see a dermatologist for an annual skin check.
Other skin conditions that have been associated with Parkinsons disease include:
- Bullous pemphigoid. This autoimmune disorder can cause itching and cause bullae to form on the skin.
- Rosacea. This condition causes skin inflammation that results in symptoms including redness, swelling, pain, flushing, and pustules on the skin.
If you have concerns about your skin, consider discussing them with your doctor or dermatologist.
Recommended Reading: What Type Of Doctor Treats Parkinson’s
Treatment Of The Face
Involved areas of the face may be washed frequently with shampoos that are effective against seborrhea as detailed above. Alternatively, ketoconazole cream, 2 percent, may be applied once or twice daily to affected areas. Often, 1 percent hydrocortisone cream will be added once or twice daily to affected areas and will aid with resolution of erythema and itching. Sodium sulfacetamide, 10 percent lotion, is also an effective topical agent for seborrheic dermatitis.
Recommended Reading: Amino Acids And Parkinsons
Patients Demographic Data And Determination Of Sd Severity
Most SD patients were male and intensity of SD was dominantly in severe or moderate form . Taking into account SD categories, there was no statistically significant difference between SDP and SDN groups in terms of SD severity: mild moderate severe . However, when SD was measured by scale there was a significant difference between SDP and SDN patients .
Table 1 Demographics and description of SD
Recommended Reading: How Does Parkinson’s Disease Affect The Spinal Cord
Malassezia Are A Necessary Factor In Seborrheic Dermatitis
Malassezia‘s role in SD is now generally accepted . Given the right conditions, Malassezia over proliferate on the skin , resulting in SDthough specific mechanisms are still open to debate . Most SD cases respond well to topical fungicides which reduce Malassezia populations on affected patches of skin to levels tolerated by patients .
SD occurs mainly in lipid-rich skin regions, especially the face, trunk and scalp . Malassezia are lipid-dependent fungi: they lack key lipid metabolism genes , and thus depend on host lipids for survival . Skin lipid production varies during our lifetime, with a peak in the first year of life, followed by a second peak in adolescence : production is depressed during the rest of childhood, which corresponds to the period of lowest SD risk . In adults, the risk of SD increases substantially with age . This is unexpected because skin lipid levels slowly decline with age , so Malassezia should have increasing difficulty securing lipids in the elderly.
When To See A Doctor
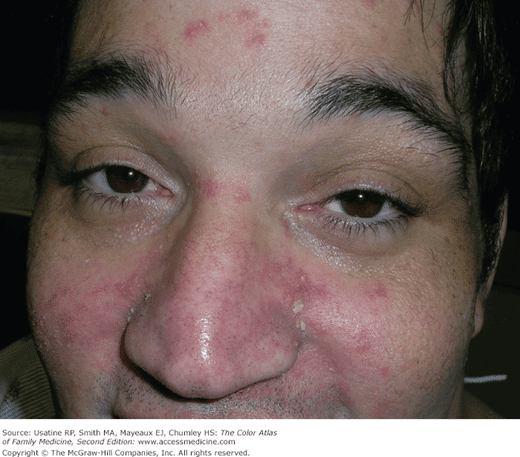
It is recommended to visit a doctor if you develop symptoms of eczema or dermatitis, especially if:
- The skin irritation is hampering your daily activities.
- You have constant pain.
- You have symptoms of a skin infection.
- Home remedies and self-care are unable to improve the infection.
- What can I do at home to help improve my condition?
- Am I allergic or sensitive to anything?
- What treatment do I need and how long will it take to work?
- How can I prevent the condition from flaring up?
- When and what symptoms did you first experience?
- Are you on any topical or oral medications?
- Have you identified any triggering factors?
- Does anyone else in your family has/had asthma or allergies?
Dont Miss: Beginning Signs Of Parkinsons
Recommended Reading: Does Parkinson’s Always Progress
Skin Issues Are Common Among Those With Parkinsons Disease
Most of us know or have known someone affected by Parkinsons Disease.
Each year, more than 60,000 people are diagnosed with Parkinsons, which is a progressive neurological condition.
In the United States, more than a million people live with Parkinsons disease. Statistics show men are more likely to develop it than women, and it usually occurs as we get into our 60s or 70s.
Some patients can experience slowness, tremors or balance problems. Others may experience decreased expressions in facial muscles, speaking softly, smaller handwriting than in the past, difficulty sleeping or constipation.
Not only does it affect the neurologic system, but it can affect the skin.
Various skin manifestations seen in Parkinsons disease are seborrheic dermatitis, dry skin, excess sweating and an increase in skin cancer development.
Changes in the skin are common symptoms of Parkinsons disease. Many patients with Parkinsons can develop oily or flaky skin, especially on the face and scalp. This is a common skin condition in the general population but more prevalent in patients with Parkinsons. It is referred to as seborrheic dermatitis.
For unknown reasons, seborrheic dermatitis is associated with an increased risk of Parkinsons disease. Patches of scaly, red skin, also referred to as dandruff, occurs primarily on the scalp and on the oily parts of the face such as the sides of the nose.
Also Check: What Causes Pain In Parkinsons Patients
Parkinsons Disease And Seborrheic Dermatitis
Those with Parkinsons disease are more likely to experience the skin condition known as seborrheic dermatitis.
Seborrheic dermatitis is a common form of eczema that typically affects your scalp. It can also appear in areas of your body that produce more oil, such as your face, chest, and back. Symptoms can include:
- dandruff in the hair, beard, mustache, or eyebrows
- skin that may appear greasy or shiny
- pimples that may cause scarring
Seborrheic dermatitis happens when the sebaceous glands in your skin produce too much oil. This can cause your skin to look greasy, red, and irritated. It often affects skin folds, such as the insides of the ears, the edges of the nose, and the eyelids.
Parkinsons disease symptoms result from dysfunction in the autonomic nervous system. This is the part of your nervous system that automatically controls functions like breathing and digestion.
People with Parkinsons disease may be at increased risk of seborrheic dermatitis because of a dysregulation in oil production. As many as 52 percent to 59 percent of people with Parkinsons disease may experience seborrheic dermatitis at some point.
Also Check: What Can Cause Parkinson’s
Suggestions To Alleviate Excessive Sweating
In some cases, episodes of profuse sweating take place as a medication dose is wearing off or during a period of dyskinesias. If the sweating episodes appear to be related to medication timing, then treatment may revolve around changing medication timing or dosages to reduce OFF time or dyskinesias.
In other cases, the episodes occur at random, or occur primarily during sleep. Basic lifestyle recommendations to aid in the management of excessive sweating include:
- wearing light, airy clothing
- taking cool or lukewarm showers
- drinking ample water
- using moisture wicking and cooling sheets, pajamas, clothing and socks. These products are made of materials that absorb more water and dry faster than standard fabrics and can be helpful for some people with excessive sweating
- avoiding sweat triggers including spicy foods, caffeine and alcohol
If these simple suggestions are not effective, and often they are not, additional strategies are available. The following are treatments recommended for those suffering from excessive sweating in the general population, and have not been tested specifically in people with PD. In addition, these treatments are generally focal and may not be as effective if sweating is widespread. Discuss these options with your physician:
Parkinsons Disease And The Skin
The concept of the skin as a factor in Parkinsons disease is not new, but several factors are just now coming together to force it onto the verge of clinical practice.
A precise diagnosis can be important from two perspectives. It can identify a condition which is treatable. It can also demarcate a contraindication, something that is not treatable. For example, many spa treatments can provoke an inflammatory reaction, so applying them to already inflamed skin is a recipe for disaster.
MICROBIOMES
Indeed, science is long overdue to give skin the credit it deserves, both in its true size and significance in human health. In terms of size, skin surface area is accepted to be only 2 meters squared basically a hide. However, a recent recalculation, expanding skin area to in excess of 25 meters squared, also boosts the developing role accorded to the skin microbiome.2
Human skin, with its large surface, harbors a wide variety of microbes, which include bacteria, fungi, viruses, archaea and skin mites. 2,4-9 Malassezia are a major component of the skin microbiome. They occur as skin commensals, but are also associated with various skin disorders and bloodstream infections.10
MALASSEZIA YEASTS
PREVALENCE
TREATMENTS
Anti-inflammatory agents in the form of topical steroids or topical calcineurin inhibitors can also be used in treatment, thus improving the patients well-being and quality of life.18
TESTING
You May Like: How Can You Help Someone With Parkinson Disease
Malassezia Are A Necessary Factor In Crohns Disease And Spondyloarthritides
Spondyloarthritides are a group chronic immune-mediated diseases mainly driven by alpha beta T cells recognizing intracellular peptides through HLA-B*27 presentation . Affected organs include the spine, joints, skin, eyes, gut, and prostate . Historically, isolated inflammation of the eyes, gut, and skinrespectively acute anterior uveitis, inflammatory bowel disease and psoriasiswere considered separate diseases unrelated to SpA. However, SpA, acute anterior uveitis, inflammatory bowel disease and psoriasis run together in families , and share many polymorphisms in genes controlling T cell activation , strongly suggesting that they are the same immunological pathology . In particular, the fact that HLA-B*27 increases the risk of each disease strongly suggests the same antigens are being targeted . Varied lines of evidence support the presence of an elusive necessary intracellular fungal infection in each affected organ, which is efficiently detected by HLA-B*27 and CARD9 . CARD9 is an essential signaling protein for fungal immunity: homozygous loss-of-function CARD9 mutations cause severe mycoses . CARD9 polymorphisms are associated with inflammatory bowel disease and SpA . Oral antifungal drugs are effective in psoriasis , psoriatic arthritis , and likely in Crohns disease as well .
Scales Formation On Oily Parts Of The Skin
There is formation of white or yellow scales on the oily parts of skin in patients with parkinsons disease. Although seborrheic dermatitis is a common skin issues in general population but is more frequently present in Parkinsons disease patients. There is formation of scaly patches, dandruff, and redness of skin mainly on the oily parts of the face like on the sides of the nose or on the scalp.
You May Like: Prayers For Parkinsons Disease
Recommended Reading: How Long Do You Live With Parkinson’s Disease
